Abstract
Purpose
To assess patient outcomes following reverse shoulder arthroplasty in patients with complex proximal humerus fracture and the clinical implications of greater tuberosity malunions.
Methods
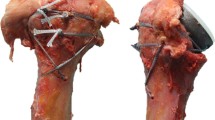
This prospective study included 56 patients who underwent RSA (DELTA XTEND™, DePuy Synthes, Warsaw, IN, USA) to treat proximal humerus fractures. We used a standardized suture technique to reattach the tuberosities. Demographic, comorbidity, and radiological parameters were collected. Assessments at 2-year follow-up (n = 49) are given as follows: range of motion (ROM), pain level, Constant Murley scores (CS), subjective shoulder value (SSV), and tuberosity healing.
Results
Anatomic tuberosity healing was achieved in 31 (55%) patients (group 1), 14 (25%) had a malunion (group 2), and complete migration occurred in 11 (20%) (group 3). No statistically significant differences between groups 1 and 2 were detected: CS (p = 0.53), SSV (p = 0.07), ROM (forward flexion (FF) p = 0.19, internal rotation (IR) p = 0.34, and external rotation (ER) p = 0.76). Group 3 had poorer outcomes (median [IQR]) than group 1: CS (59 [50–71]) vs. 72 [65–78]), FF (120 [100–150]) vs. 150 [125–160] and ER (− 20 [− 20 to 10] vs. 30 [20–45], respectively. Three complications (group 1) occurred: one-stage revision after low-grade infection, haematoma due to early rivaroxaban intake, and open reduction and internal fixation for acromion insufficiency fracture. No patients showed signs of stem or glenoid loosening after 2 years.
Conclusion
Cases with complete superior migration experienced poorer clinical outcomes than those with anatomic healing. Despite a relatively high malunion rate, the outcomes were not significantly worse in these patients compared to anatomically healed GT cases.


Similar content being viewed by others
References
Kruithof RN, Formijne Jonkers HA, van der Ven DJC, van Olden GDJ, Timmers TK (2017) Functional and quality of life outcome after non-operatively managed proximal humeral fractures. J Orthop Traumatol 18(4):423–430. https://doi.org/10.1007/s10195-017-0468-5
Bufquin T, Hersan A, Hubert L, Massin P (2007) Reverse shoulder arthroplasty for the treatment of three- and four-part fractures of the proximal humerus in the elderly: a prospective review of 43 cases with a short-term follow-up. J Bone Jt Surg [Br] 89(4):516–520. https://doi.org/10.1302/0301-620X.89B4.18435
Cazeneuve JF, Cristofari DJ (2009) Delta III reverse shoulder arthroplasty: radiological outcome for acute complex fractures of the proximal humerus in elderly patients. Orthop Traumatol Surg Res 95(5):325–329. https://doi.org/10.1016/j.otsr.2009.03.018
Gallinet D, Clappaz P, Garbuio P, Tropet Y, Obert L (2009) Three or four parts complex proximal humerus fractures: hemiarthroplasty versus reverse prosthesis: a comparative study of 40 cases. Orthop Traumatol Surg Res 95(1):48–55. https://doi.org/10.1016/j.otsr.2008.09.002
Klein M, Juschka M, Hinkenjann B, Scherger B, Ostermann PA (2008) Treatment of comminuted fractures of the proximal humerus in elderly patients with the Delta III reverse shoulder prosthesis. J Orthop Trauma 22(10):698–704. https://doi.org/10.1097/BOT.0b013e31818afe40
Reitman RD, Kerzhner E (2011) Reverse shoulder arthoplasty as treatment for comminuted proximal humeral fractures in elderly patients. Am J Orthop 40(9):458–461
Valenti P, Zampeli F, Ciais G, Kany J, Katz D (2020) The initial treatment of complex proximal humerus fracture affects the outcome of revision with reverse shoulder arthroplasty. Int Orthop 44(7):1331–1340. https://doi.org/10.1007/s00264-020-04612-y
Wall B, Walch G (2007) Reverse shoulder arthroplasty for the treatment of proximal humeral fractures. Hand Clin 23(4):425–430. https://doi.org/10.1016/j.hcl.2007.08.002. (v–vi)
Savin DD, Zamfirova I, Iannotti J, Goldberg BA, Youderian AR (2016) Survey study suggests that reverse total shoulder arthroplasty is becoming the treatment of choice for four-part fractures of the humeral head in the elderly. Int Orthop 40(9):1919–1925. https://doi.org/10.1007/s00264-016-3227-y
Boileau P, Watkinson DJ, Hatzidakis AM, Balg F (2005) Grammont reverse prosthesis: design, rationale, and biomechanics. J Shoulder Elbow Surg 14(1 Suppl S):147S-161S. https://doi.org/10.1016/j.jse.2004.10.006
Lenarz C, Shishani Y, McCrum C, Nowinski RJ, Edwards TB, Gobezie R (2011) Is reverse shoulder arthroplasty appropriate for the treatment of fractures in the older patient? Early observations. Clin Orthop Relat Res 469(12):3324–3331. https://doi.org/10.1007/s11999-011-2055-z
Levy JC, Badman B (2011) Reverse shoulder prosthesis for acute four-part fracture: tuberosity fixation using a horseshoe graft. J Orthop Trauma 25(5):318–324. https://doi.org/10.1097/BOT.0b013e3181f22088
Zumstein MA, Pinedo M, Old J, Boileau P (2011) Problems, complications, reoperations, and revisions in reverse total shoulder arthroplasty: a systematic review. J Shoulder Elbow Surg 20(1):146–157. https://doi.org/10.1016/j.jse.2010.08.001
Boileau P, Krishnan SG, Tinsi L, Walch G, Coste JS, Mole D (2002) Tuberosity malposition and migration: reasons for poor outcomes after hemiarthroplasty for displaced fractures of the proximal humerus. J Shoulder Elbow Surg 11(5):401–412
Boileau P, Alta TD, Decroocq L, Sirveaux F, Clavert P, Favard L, Chelli M (2019) Reverse shoulder arthroplasty for acute fractures in the elderly: is it worth reattaching the tuberosities? J Shoulder Elbow Surg 28(3):437–444. https://doi.org/10.1016/j.jse.2018.08.025
Chun YM, Kim DS, Lee DH, Shin SJ (2017) Reverse shoulder arthroplasty for four-part proximal humerus fracture in elderly patients: can a healed tuberosity improve the functional outcomes? J Shoulder Elbow Surg 26(7):1216–1221. https://doi.org/10.1016/j.jse.2016.11.034
Garofalo R, Flanagin B, Castagna A, Lo EY, Krishnan SG (2015) Reverse shoulder arthroplasty for proximal humerus fracture using a dedicated stem: radiological outcomes at a minimum 2 years of follow-up-case series. J Orthop Surg Res 10:129. https://doi.org/10.1186/s13018-015-0261-1
Grubhofer F, Wieser K, Meyer DC, Catanzaro S, Beeler S, Riede U, Gerber C (2016) Reverse total shoulder arthroplasty for acute head-splitting, 3- and 4-part fractures of the proximal humerus in the elderly. J Shoulder Elbow Surg 25(10):1690–1698. https://doi.org/10.1016/j.jse.2016.02.024
Wright JO, Ho A, Kalma J, Koueiter D, Esterle J, Marcantonio D, Wiater JM, Wiater B (2019) Uncemented reverse total shoulder arthroplasty as initial treatment for comminuted proximal humerus fractures. J Orthop Trauma 33(7):e263–e269. https://doi.org/10.1097/BOT.0000000000001465
Torrens C, Alentorn-Geli E, Mingo F, Gamba C, Santana F (2018) Reverse shoulder arthroplasty for the treatment of acute complex proximal humeral fractures: influence of greater tuberosity healing on the functional outcomes. J Orthop Surg (Hong Kong) 26(1):2309499018760132. https://doi.org/10.1177/2309499018760132
Neer CS 2nd (1970) Displaced proximal humeral fractures. I. Classification and evaluation. J Bone Jt Surg [Am] 52(6):1077–1089
Spross C, Meester J, Mazzucchelli RA, Puskas GJ, Zdravkovic V, Jost B (2019) Evidence-based algorithm to treat patients with proximal humerus fractures—a prospective study with early clinical and overall performance results. J Shoulder Elbow Surg 28(6):1022–1032. https://doi.org/10.1016/j.jse.2019.02.015
Constant CR, Murley AH (1987) A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res 214:160–164
Fuchs B, Jost B, Gerber C (2000) Posterior-inferior capsular shift for the treatment of recurrent, voluntary posterior subluxation of the shoulder. J Bone Jt Surg [Am] 82(1):16–25. https://doi.org/10.2106/00004623-200001000-00003
Gilbart MK, Gerber C (2007) Comparison of the subjective shoulder value and the Constant score. J Shoulder Elbow Surg 16(6):717–721. https://doi.org/10.1016/j.jse.2007.02.123
Levigne C, Boileau P, Favard L, Garaud P, Mole D, Sirveaux F, Walch G (2008) Scapular notching in reverse shoulder arthroplasty. J Shoulder Elbow Surg 17(6):925–935. https://doi.org/10.1016/j.jse.2008.02.010
Sirveaux F, Favard L, Oudet D, Huquet D, Walch G, Mole D (2004) Grammont inverted total shoulder arthroplasty in the treatment of glenohumeral osteoarthritis with massive rupture of the cuff. Results of a multicentre study of 80 shoulders. J Bone Jt Surg [Br] 86(3):388–395. https://doi.org/10.1302/0301-620x.86b3.14024
Sperling JW, Cofield RH, O’Driscoll SW, Torchia ME, Rowland CM (2000) Radiographic assessment of ingrowth total shoulder arthroplasty. J Shoulder Elbow Surg 9(6):507–513. https://doi.org/10.1067/mse.2000.109384
Jain NP, Mannan SS, Dharmarajan R, Rangan A (2019) Tuberosity healing after reverse shoulder arthroplasty for complex proximal humeral fractures in elderly patients-does it improve outcomes? A systematic review and meta-analysis. J Shoulder Elbow Surg 28(3):e78–e91. https://doi.org/10.1016/j.jse.2018.09.006
Cuff DJ, Pupello DR (2013) Comparison of hemiarthroplasty and reverse shoulder arthroplasty for the treatment of proximal humeral fractures in elderly patients. J Bone Jt Surg [Am] 95(22):2050–2055. https://doi.org/10.2106/JBJS.L.01637
Gallinet D, Adam A, Gasse N, Rochet S, Obert L (2013) Improvement in shoulder rotation in complex shoulder fractures treated by reverse shoulder arthroplasty. J Shoulder Elbow Surg 22(1):38–44. https://doi.org/10.1016/j.jse.2012.03.011
Sebastia-Forcada E, Cebrian-Gomez R, Lizaur-Utrilla A, Gil-Guillen V (2014) Reverse shoulder arthroplasty versus hemiarthroplasty for acute proximal humeral fractures. A blinded, randomized, controlled, prospective study. J Shoulder Elbow Surg 23(10):1419–1426. https://doi.org/10.1016/j.jse.2014.06.035
Hess F, Bohnert L, Jaberg L, Welter J, Pape HC, Sireus A (2020) Tuberosity union in patients with proximal humerus fractures treated with reverse shoulder arthroplasty: a technical note and exploratory analysis. Int Orthop 44(12):2711–2717. https://doi.org/10.1007/s00264-020-04831-3
Cazeneuve JF, Cristofari DJ (2010) The reverse shoulder prosthesis in the treatment of fractures of the proximal humerus in the elderly. J Bone Jt Surg [Br] 92(4):535–539. https://doi.org/10.1302/0301-620X.92B4.22450
Frankle MA, Ondrovic LE, Markee BA, Harris ML, Lee WE 3rd (2002) Stability of tuberosity reattachment in proximal humeral hemiarthroplasty. J Shoulder Elbow Surg 11(5):413–420. https://doi.org/10.1067/mse.2002.126098
Krishnan SG, Reineck JR, Bennion PD, Feher L, Burkhead WZ Jr (2011) Shoulder arthroplasty for fracture: does a fracture-specific stem make a difference? Clin Orthop Relat Res 469(12):3317–3323. https://doi.org/10.1007/s11999-011-1919-6
Li F, Zhu Y, Lu Y, Liu X, Wu G, Jiang C (2014) Hemiarthroplasty for the treatment of complex proximal humeral fractures: does a trabecular metal prosthesis make a difference? A prospective, comparative study with a minimum 3-year follow-up. J Shoulder Elbow Surg 23(10):1437–1443. https://doi.org/10.1016/j.jse.2014.04.017
Funding
No grants or other financial support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of Eastern Switzerland (EKOS 2019-00414).
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fischer, J., Welter, J., Horn, N. et al. Is malunion of the greater tuberosity after reverse shoulder arthroplasty in patients with complex proximal humerus fracture associated with worse clinical outcomes? A prospective cohort study. Arch Orthop Trauma Surg 143, 6527–6533 (2023). https://doi.org/10.1007/s00402-023-04951-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04951-6