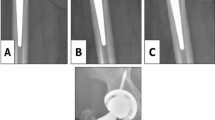
Abstract
Introduction
Comparison between fully hydroxyapatite (HA)-coated stems with differing geometry are lacking in the total hip arthroplasty (THA) literature. This study aimed to compare femoral canal fill, radiolucency formation, and 2-year implant survivorship between two commonly used, HA-coated stems.
Methods
All primary THAs performed with two fully HA-coated stems (Polar stem, Smith&Nephew, Memphis, TN and Corail stem, DePuy-Synthes, Warsaw, IN) with a minimum 2-year radiographic follow-up were identified. Radiographic measures of proximal femoral morphology based on the Dorr classification and femoral canal fill were analyzed. Radiolucent lines were identified by Gruen zone. Perioperative characteristics and 2-year survivorship were compared between stem types.
Results
A total of 233 patients were identified with 132 (56.7%) receiving the Polar stem (P) and 101 (43.3%) receiving the Corail stem (C). No differences were observed with respect to proximal femoral morphology. Femoral stem canal fill at the middle third of the stem was greater for P stem patients than for C stem patients (P stem; 0.80 ± 0.08 vs. C stem; 0.77 ± 0.08, p = 0.002), while femoral stem canal fill at the distal third of the stem and presence of subsidence were comparable between groups. A total of six and nine radiolucencies were observed in P stem and C stem patients, respectively. Revision rate at 2-year (P stem; 1.5% vs C stem; 0.0%, p = 0.51) and latest follow-up (P stem; 1.5% vs C stem; 1.0%, p = 0.72) did not differ between groups.
Conclusion
Greater canal fill at the middle third of the stem was observed for the P stem compared to the C stem, however, both stems demonstrated robust and comparable freedom from revision at 2-year and latest follow-up, with low incidences of radiolucent line formation. Mid-term clinical and radiographic outcomes for these commonly used, fully HA-coated stems remain equally promising in THA despite variations in canal fill.



Similar content being viewed by others
Data availability
Data is protected by our institutions IRB protocol but could be de-identifed and available on request.
References
Kremers HM, Larson DR, Crowson CS et al (2014) Prevalence of total hip and knee replacement in the United States. J Bone Jt Surg—Am 97(17):1386–1397. https://doi.org/10.2106/JBJS.N.01141
Singh JA, Yu S, Chen L, Cleveland JD (2019) Rates of total joint replacement in the United States: future projections to 2020–2040 using the national inpatient sample. J Rheumatol 46(9):1134–1140. https://doi.org/10.3899/jrheum.170990
Konan S, Abdel MP, Haddad FS (2019) Cemented versus uncemented hip implant fixation. Bone Joint Res 8(12):604–607. https://doi.org/10.1302/2046-3758.812.BJR-2019-0337
Yakkanti RR, Greif DN, Berge DJ Vanden, Robinson RP. Survival and performance of a dual tapered-wedge fully HA-coated press fit femoral stem. Arch Orthop Trauma Surg. Published online March 2022. https://doi.org/10.1007/s00402-022-04393-6
Ries C, Boese CK, Dietrich F, Miehlke W, Heisel C (2019) Femoral stem subsidence in cementless total hip arthroplasty: a retrospective single-centre study. Int Orthop 43(2):307–314. https://doi.org/10.1007/s00264-018-4020-x
Gkagkalis G, Goetti P, Mai S et al (2019) Cementless short-stem total hip arthroplasty in the elderly patient - is it a safe option?: a prospective multicentre observational study. BMC Geriatr 19(1):112. https://doi.org/10.1186/s12877-019-1123-1
Jacquot L, Bonnin MP, Machenaud A, Chouteau J, Saffarini M, Vidalain J-P (2018) Clinical and radiographic outcomes at 25–30 years of a hip stem fully coated with hydroxylapatite. J Arthroplasty 33(2):482–490. https://doi.org/10.1016/j.arth.2017.09.040
Karayiannis PN, Cassidy RS, Isaac G et al (2021) Risk factors for significant radiolucent line development in a fully coated hydroxyapatite stem. J Arthroplasty 36(11):3709–3715. https://doi.org/10.1016/j.arth.2021.07.001
Ishii S, Homma Y, Baba T, Ozaki Y, Matsumoto M, Kaneko K (2016) Does the canal fill ratio and femoral morphology of Asian females influence early radiographic outcomes of total hip arthroplasty with an uncemented proximally coated, tapered-wedge stem? J Arthroplasty 31(7):1524–1528. https://doi.org/10.1016/j.arth.2016.01.016
D’Ambrosio A, Peduzzi L, Roche O, Bothorel H, Saffarini M, Bonnomet F (2020) Influence of femoral morphology and canal fill ratio on early radiological and clinical outcomes of uncemented total hip arthroplasty using a fully coated stem. Bone Joint Res 9(4):182–191. https://doi.org/10.1302/2046-3758.94.BJR-2019-0149.R2
Rivière C, Grappiolo G, Engh CA et al (2018) Long-term bone remodelling around ‘legendary’ cementless femoral stems. EFORT Open Rev 3(2):45–57. https://doi.org/10.1302/2058-5241.3.170024
Louboutin L, Viste A, Desmarchelier R, Fessy M-H (2017) Long-term survivorship of the Corail™ standard stem. Orthop Traumatol Surg Res 103(7):987–992. https://doi.org/10.1016/j.otsr.2017.06.010
Lee PYF, Evans AR (2014) Early failure of the polarstem total hip arthroplasty—Can the australian NJR tell us the full story? J Arthroplasty 29(3):609–611. https://doi.org/10.1016/j.arth.2013.07.040
Kellam PJ, Frandsen JJ, Randall DJ, Blackburn BE, Peters CL, Pelt CE (2022) Neocortex formation in a tapered wedge stem is not indicative of complications or worse outcomes. J Arthroplasty 37(8):S895–S900. https://doi.org/10.1016/j.arth.2022.01.069
Delaunay C. Effect of hydroxyapatite coating on the radio-clinical results of a grit-blasted titanium alloy femoral taper. A case-control study of 198 cementless primary total hip arthroplasty with the AlloclassicTM system. Orthop Traumatol Surg Res. 2014;100(7):739–744. https://doi.org/10.1016/j.otsr.2014.07.010
McLaughlin JR, Lee KR. Cementless total hip replacement using second-generation components. J Bone Joint Surg Br. 2010;92-B(12):1636–1641. https://doi.org/10.1302/0301-620X.92B12.24582
Cho J-H, Garino JP, Choo S-K, Han K-Y, Kim J-H, Oh H-K (2010) Seven-year results of a tapered, titanium, hydroxyapatite-coated cementless femoral stem in primary total hip arthroplasty. Clin Orthop Surg 2(4):214. https://doi.org/10.4055/cios.2010.2.4.214
Tonino AJ, van der Wal BCH, Heyligers IC, Grimm B (2009) Bone remodeling and hydroxyapatite resorption in coated primary hip prostheses. Clin Orthop Relat Res 467(2):478–484. https://doi.org/10.1007/s11999-008-0559-y
Kaszuba S V., Cipparrone N, Gordon AC. The Actis and Corail Femoral Stems Provide for Similar Clinical and Radiographic Outcomes in Total Hip Arthroplasty. HSS J ®. 2020;16(S2):412–419. https://doi.org/10.1007/s11420-020-09792-2
Buttaro MA, Oñativia JI, Slullitel PA, et al. Metaphyseal debonding of the Corail collarless cementless stem. Bone Joint J. 2017;99-B(11):1435–1441. https://doi.org/10.1302/0301-620X.99B11.BJJ-2017-0431.R1
Noble PC, Gordon MJ, Weiss JM, Reddix RN, Conditt MA, Mathis KB (2005) Does total knee replacement restore normal knee function? Clin Orthop Relat Res 431(431):157–165. https://doi.org/10.1097/01.blo.0000150130.03519.fb
Yeung Y, Chiu KY, Yau WP, Tang WM, Cheung WY, Ng TP (2006) Assessment of the proximal femoral morphology using plain radiograph—Can it predict the bone quality? J Arthroplasty 21(4):508–513. https://doi.org/10.1016/j.arth.2005.04.037
Dorr LD, Faugere M-C, Mackel AM, Gruen TA, Bognar B, Malluche HH (1993) Structural and cellular assessment of bone quality of proximal femur. Bone 14(3):231–242. https://doi.org/10.1016/8756-3282(93)90146-2
Aydin N, Bezer M, Akgulle AH, Saygi B, Kocaoğlu B, Guven O (2009) Comparison of distal and proximal centralising devices in hip arthroplasty. Int Orthop 33(4):945–948. https://doi.org/10.1007/s00264-008-0610-3
Fottner A, Woiczinski M, Kistler M et al (2017) Influence of undersized cementless hip stems on primary stability and strain distribution. Arch Orthop Trauma Surg 137(10):1435–1441. https://doi.org/10.1007/s00402-017-2784-x
Engh CA, Massin P, Suthers KE (1990) Roentgenographic assessment of the biologic fixation of porous-surfaced femoral components. Clin Orthop Relat Res 257:107–128
Gruen TA, McNeice GM, Amstutz HC (1979) “Modes of failure” of cemented stem-type femoral components: a radiographic analysis of loosening. Clin Orthop Relat Res 141:17–27
Shrout PE, Fleiss JL (1979) Intraclass correlations: uses in assessing rater reliability. Psychol Bull 86(2):420–428. https://doi.org/10.1037//0033-2909.86.2.420
Rivera F, Leonardi F, Evangelista A, Pierannunzii L (2016) Risk of stem undersizing with direct anterior approach for total HIP arthroplasty. HIP Int 26(3):249–253. https://doi.org/10.5301/hipint.5000337
Janssen L, Wijnands KAP, Janssen D, Janssen MWHE, Morrenhof JW. Do Stem Design and Surgical Approach Influence Early Aseptic Loosening in Cementless THA? Clin Orthop Relat Res. 2018;476(6). https://journals.lww.com/clinorthop/Fulltext/2018/06000/Do_Stem_Design_and_Surgical_Approach_Influence.18.aspx
Mattesi L, Cheyrou-Lagrèze A, Odri G-A, Duhil A, Flurin L, Severyns M (2021) Does the surgical approach influence the canal fill of the proximal femur for hip arthroplasty? Arthroplast today 10:166–170. https://doi.org/10.1016/j.artd.2021.05.011
Vidalain J-P (2011) Twenty-year results of the cementless Corail stem. Int Orthop 35(2):189–194. https://doi.org/10.1007/s00264-010-1117-2
Jameson SS, Baker PN, Mason J, et al. Independent predictors of failure up to 7.5 years after 35 386 single-brand cementless total hip replacements. Bone Joint J. 2013;95-B(6):747–757. https://doi.org/10.1302/0301-620X.95B6.31378
Selvaratnam V, Shetty V, Sahni V (2015) Subsidence in collarless corail hip replacement. Open Orthop J 9(1):194–197. https://doi.org/10.2174/1874325001509010194
Callary SA, Campbell DG, Mercer GE, Nilsson KG, Field JR (2012) The 6-year migration characteristics of a hydroxyapatite-coated femoral stem. J Arthroplasty 27(7):1344-1348.e1. https://doi.org/10.1016/j.arth.2011.12.002
Thomas WC, Parvataneni HK, Vlasak RG, Gray CF (2020) Early polyethylene failure in a modern total hip prosthesis: a note of caution. J Arthroplasty 35(5):1297–1302. https://doi.org/10.1016/j.arth.2019.12.043
Skinner JA, Kroon PO, Todo S, Scott G. A femoral component with proximal HA coating. J Bone Joint Surg Br. 2003;85-B(3):366–370. https://doi.org/10.1302/0301-620X.85B3.13054
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript. No direct funding or support was received for this work.
Author information
Authors and Affiliations
Contributions
This study conceptualization and conception was made by MH. Methodology and study design was suggested and supervised by RS and YW. Material preparation, data collection and analysis were performed by IS, KL, EM, CSH, RME and NS. The first draft of the manuscript was written by IS, KL AND NS and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Dr. RS is a paid consultant for Smith&Nephew and InteliJoint and has stock options in Intelijoint and Gauss Surgical. Dr. MH is a paid consultant for Stryker and Exactech and receives research support from Exactech. Drs. IS, KL, EB, CSH, RME, YW and NS have not financial disclosures.
Ethical approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of NYU University (IRB i17- 01223).
Informed consent
Informed consent was waivered.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shichman, I., Lawrence, K.W., Berzolla, E. et al. Comparison of canal fill and radiolucent line formation between two fully coated, hydroxyapatite tapered stems: a 2-year follow-up after total hip arthroplasty. Arch Orthop Trauma Surg 143, 6945–6954 (2023). https://doi.org/10.1007/s00402-023-04944-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04944-5