Abstract
Introduction
Previous reports using cadaveric knees and musculoskeletal computer simulation have shown that kinematically aligned (KA) total knee arthroplasty (TKA) provides more natural and physiological tibiofemoral kinematic patterns than mechanically aligned (MA) TKA. These reports suggested that the modification of joint line obliquity improve the knee kinematics. This study aimed to determine whether joint line obliquity change the intraoperative tibiofemoral kinematics in TKA candidates with knee osteoarthritis.
Methods
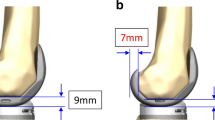
Thirty consecutive knees with varus osteoarthritis that underwent TKA using a navigation system were evaluated. Two types of trial components were prepared: (1) MA TKA model: component trial in which articulating surface was parallel to the bone cut surface (2) KA TKA model: the femoral component trial, which mimicked the KA TKA method of Dossett et al. was designed 3° valgus and 3° internal rotation to the femoral bone cut surface, and the tibial component trial was designed 3° varus to the tibial bone cut surface. These two trials were set on the same knees during the operation, and the tibiofemoral rotational kinematics and varus–valgus laxity were measured from 0° to 120° of knee flexion using a navigation system.
Results
The joint gap was 20 ± 2 mm and 3° ± 1° varus in extension and 20 ± 2 mm and 3° ± 1°varus in flexion. The differences in femoral component rotation between KA TKA and MA TKA were not statistically significant for any knee flexion angle. The differences in varus–valgus laxity between KA TKA and MA TKA were also not statistically significant for any knee flexion angle.
Conclusion
Although the degree of joint line obliquity varies widely in various KA TKA methods, this study, which mimicked the method of Dossett et al. showed that the modification of joint line obliquity did not change the tibiofemoral kinematics and stability of the knee joint in TKA candidates with knee osteoarthritis.




Similar content being viewed by others
References
Cip J, Obwegeser F, Benesch T, Bach C, Ruckenstuhl P, Martin A (2018) Twelve-year follow-up of navigated computer-assisted versus conventional total knee arthroplasty a prospective randomized comparative trial. J Arthroplasty. 33(5):1404–1411
Schiavone Panni A, Falez F, D’Apolito R, Corona K, Perisano C, Vasso M (2017) Long-term follow-up of a non-randomised prospective cohort of one hundred and ninety two total knee arthroplasties using the NexGen implant. Int Orthop. 41(6):1155–1162
Bourne RB, Chesworth B, Davis A, Mahomed N, Charron K (2010) Comparing patient outcomes after THA and TKA: is there a difference? Clin Orthop Relat Res. 468(2):542–546
Bourne RB, Chesworth BM, Davis AM, Mahomed NN, Charron KD (2010) Patient satisfaction after total knee arthroplasty: who is satisfied and who is not? Clin Orthop Relat Res. 468(1):57–63
Mooney LT, Smith A, Sloan K, Clark GW (2016) The effect of the native kinematics of the knee on the outcome following total knee arthroplasty. Bone Joint J. 98B(11):1471–1478
Dennis DA, Komistek RD, Mahfouz MR (2003) In vivo fluoroscopic analysis of fixed-bearing total knee replacements. Clin Orthop Relat Res. 410:114–130
Howell SM, Howell SJ, Kuznik KT, Cohen J, Hull ML (2013) Does a kinematically aligned total knee arthroplasty restore function without failure regardless of alignment category? Clin Orthop Relat Res. 471(3):1000–1007
Howell SM, Papadopoulos S, Kuznik KT, Hull ML (2013) Accurate alignment and high function after kinematically aligned TKA performed with generic instruments. Knee Surg Sports Traumatol Arthrosc. 21(10):2271–2280
Lustig S, Sappey-Marinier E, Fary C, Servien E, Parratte S, Batailler C (2021) Personalized alignment in total knee arthroplasty: current concepts. SICOT J. 7:19
Dossett HG, Estrada NA, Swartz GJ, LeFevre GW, Kwasman BG (2014) A randomised controlled trial of kinematically and mechanically aligned total knee replacements: two-year clinical results. Bone Joint J. 96B(7):907–913
Maderbacher G, Keshmiri A, Krieg B, Greimel F, Grifka J, Baier C (2019) Kinematic component alignment in total knee arthroplasty leads to better restoration of natural tibiofemoral kinematics compared to mechanic alignment. Knee Surg Sports Traumatol Arthrosc. 27(5):1427–1433
Ishikawa M, Kuriyama S, Ito H, Furu M, Nakamura S, Matsuda S (2015) Kinematic alignment produces near-normal knee motion but increases contact stress after total knee arthroplasty: a case study on a single implant design. Knee. 22(3):206–212
Nakamura S, Tian Y, Tanaka Y et al (2017) The effects of kinematically aligned total knee arthroplasty on stress at the medial tibia: a case study for varus knee. Bone Joint Res. 6(1):43–51
Ishida K, Shibanuma N, Matsumoto T et al (2015) Factors affecting intraoperative kinematic patterns and flexion angles in navigated total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. 23(6):1741–1747
Tsubosaka M, Ishida K, Kodato K et al (2021) Mid-flexion stability in the anteroposterior plane is achieved with a medial congruent insert in cruciate-retaining total knee arthroplasty for varus osteoarthritis. Knee Surg Sports Traumatol Arthrosc. 29(2):467–473
Hino K, Ishimaru M, Iseki Y, Watanabe S, Onishi Y, Miura H (2013) Mid-flexion laxity is greater after posterior-stabilised total knee replacement than with cruciate-retaining procedures: a computer navigation study. Bone Joint J. 95B(4):493–497
Hino K, Kutsuna T, Watamori K et al (2018) Bi-cruciate substituting total knee arthroplasty provides varus-valgus stability throughout the midflexion range. Knee. 25(5):897–902
Koo TK, Li MY (2016) A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med. 15(2):155–63
Komistek RD, Dennis DA, Mahfouz M (2003) In vivo fluoroscopic analysis of the normal human knee. Clin Orthop Relat Res. 410:69–81
Nishio Y, Onodera T, Kasahara Y, Takahashi D, Iwasaki N, Majima T (2014) Intraoperative medial pivot affects deep knee flexion angle and patient-reported outcomes after total knee arthroplasty. J Arthroplasty. 29(4):702–706
Kettelkamp DB, Johnson RJ, Smidt GL, Chao EY, Walker M (1970) An electrogoniometric study of knee motion in normal gait. J Bone Joint Surg Am. 52(4):775–790
Laubenthal KN, Smidt GL, Kettelkamp DB (1972) A quantitative analysis of knee motion during activities of daily living. Phys Ther. 52(1):34–43
Schroer WC, Berend KR, Lombardi AV et al (2013) Why are total knees failing today? Etiology of total knee revision in 2010 and 2011. J Arthroplasty. 28(8 Suppl):116–119
Dennis DA, Komistek RD, Mahfouz MR, Haas BD, Stiehl JB (2003) Multicenter determination of in vivo kinematics after total knee arthroplasty. Clin Orthop Relat Res. 416:37–57
Funding
There was no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
There was no conflict of interest.
Ethical approval
This study was approved by the institutional review boards of our hospitals (approval number: 4405).
Informed consent
All patients provided written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Minoda, Y., Sugama, R., Ohta, Y. et al. The modification of bone cut angle and joint line obliquity did not change the tibiofemoral kinematics and stability of knee joint after total knee arthroplasty. Arch Orthop Trauma Surg 143, 6345–6351 (2023). https://doi.org/10.1007/s00402-023-04899-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04899-7