Abstract
Introduction
There is a paucity of information on the bone remodeling that occurs distal to the femoral stem following total hip arthroplasty as most previous studies have focused on proximal changes. In this study, we report the cortical thinning that occur distal to the femoral stem after primary total hip arthroplasty.
Methods
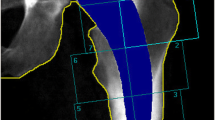
A retrospective review was performed at one institution over a 5-year period. 156 primary total hip arthroplasty procedures were included. The Cortical Thickness Index (CTI) was measured on both operative and non-operative hips at 1 cm, 3 cm and 5 cm below the prosthetic stem tip on anteroposterior radiographic images pre-operatively as well as at 6 months, 12 months and 24 months post-operatively. The difference in average CTI was measured using paired t-tests.
Results
There were statistically significant decreases in CTI distal to the femoral stem at 12 months and 24 months (-1.3% and -2.8%, respectively). Greater losses were seen in female patients, patients older than 75, and patients with BMI less than 35 at 6 months postoperative. There were no differences in CTI at any time point on the non-operative side.
Conclusion
The current study demonstrates that patients undergo bone loss as measured by CTI distal to the stem in the first 2 years following total hip arthroplasty. Comparison to the contralateral non-operative side confirms that this change is greater than expected for the natural aging process. A greater understanding of these changes will help optimize post-operative management and direct future innovations in implant design.


Similar content being viewed by others
References
Eskelinen A, Remes V, Helenius I, Pulkkinen P, Nevalainen J, Paavolainen P (2005) Total hip arthroplasty for primary osteoarthrosis in younger patients in the Finnish arthroplasty register. 4,661 primary replacements followed for 0–22 years. Acta Orthop 76:28–41. https://doi.org/10.1080/00016470510030292
Chen J-H, Liu C, You L, Simmons CA (2010) Boning up on Wolff’s Law: mechanical regulation of the cells that make and maintain bone. J Biomech 43:108–118. https://doi.org/10.1016/j.jbiomech.2009.09.016
Cabahug-Zuckerman P, Frikha-Benayed D, Majeska RJ, Tuthill A, Yakar S, Judex S, Schaffler MB (2016) Osteocyte apoptosis caused by hindlimb unloading is required to trigger osteocyte RANKL production and subsequent resorption of cortical and trabecular bone in mice femurs. J bone Miner Res 31:1356–1365. https://doi.org/10.1002/jbmr.2807
Cole EW, Moulton SG, Gobezie R, Romeo AA, Walker JB, Lederman E, Denard PJ (2020) Five-year radiographic evaluation of stress shielding with a press-fit standard length humeral stem. JSES Int 4:109–113. https://doi.org/10.1016/j.jses.2019.11.002
Yan SG, Chevalier Y, Liu F, Hua X, Schreiner A, Jansson V, Schmidutz F (2020) Metaphyseal anchoring short stem hip arthroplasty provides a more physiological load transfer: a comparative finite element analysis study. J Orthop Surg Res 15:498. https://doi.org/10.1186/s13018-020-02027-4
Abdel MP, Houdek MT, Watts CD, Lewallen DG, Berry DJ (2016) Epidemiology of periprosthetic femoral fractures in 5417 revision total hip arthroplasties. Bone Joint J 98:468–474. https://doi.org/10.1302/0301-620X.98B4.37203
Pavelka T, Salášek M, Weisová D (2017) Periprosthetic femoral fractures after total hip replacement: our results and treatment complications. Acta Chir Orthop Traumatol Cech 84:52–58
Cho YJ, Chun YS, Rhyu KH, Baek JH, Liang H (2016) Distal femoral cortical hypertrophy after hip arthroplasty using a cementless doubletapered femoral stem. J Orthop Surg 24:317–322. https://doi.org/10.1177/1602400309
Delsmann MM, Strahl A, Mühlenfeld M, Jandl NM, Beil FT, Ries C, Rolvien T (2021) High prevalence and undertreatment of osteoporosis in elderly patients undergoing total hip arthroplasty. Osteoporos Int 32:1661–1668. https://doi.org/10.1007/s00198-021-05881-y
Cruz E, Natera L, Mitjans M, Antón C, Cañete E, Cases E (2020) Is there a significant decrease in the femoral cortical bone around Furlong(®) stems after 18 years of follow-up? Eur J Orthop Surg Traumatol 30:117–122. https://doi.org/10.1007/s00590-019-02539-8
Nguyen BN, Hoshino H, Togawa D, Matsuyama Y (2018) Cortical thickness index of the proximal femur: a radiographic parameter for preliminary assessment of bone mineral density and osteoporosis status in the age 50 years and over population. Clin Orthop Surg 10:149–156. https://doi.org/10.4055/cios.2018.10.2.149
Baumgärtner R, Heeren N, Quast D, Babst R, Brunner A (2015) Is the cortical thickness index a valid parameter to assess bone mineral density in geriatric patients with hip fractures? Arch Orthop Trauma Surg 135:805–810. https://doi.org/10.1007/s00402-015-2202-1
Van Rietbergen B, Huiskes R, Weinans H, Sumner DR, Turner TM, Galante JO (1993) ESB research award 1992. the mechanism of bone remodeling and resorption around press-fitted THA stems. J Biomech 26:369–382. https://doi.org/10.1016/0021-9290(93)90001-u
Huiskes R (1990) The various stress patterns of press-fit, ingrown, and cemented femoral stems. Clin Orthop Relat Res. 261:27–38
Decking R, Puhl W, Simon U, Claes LE (2006) Changes in strain distribution of loaded proximal femora caused by different types of cementless femoral stems. Clin Biomech 21:495–501. https://doi.org/10.1016/j.clinbiomech.2005.12.011
Ritter MA, Fechtman RW (1988) Distal cortical hypertrophy following total hip arthroplasty. J Arthroplasty 3:117–121. https://doi.org/10.1016/s0883-5403(88)80076-7
Peitgen DS, Innmann MM, Merle C, Gotterbarm T, Moradi B, Streit MR (2018) Periprosthetic bone mineral density around uncemented titanium stems in the second and third decade after total hip arthroplasty: a DXA study after 12, 17 and 21 years. Calcif Tissue Int 103:372–379. https://doi.org/10.1007/s00223-018-0438-9
Knutsen AR, Lau N, Longjohn DB, Ebramzadeh E, Sangiorgio SN (2017) Periprosthetic femoral bone loss in total hip arthroplasty: systematic analysis of the effect of stem design. Hip Int 27:26–34. https://doi.org/10.5301/hipint.5000413
Streit MR, Innmann MM, Merle C, Bruckner T, Aldinger PR, Gotterbarm T (2013) Long-term (20- to 25-year) results of an uncemented tapered titanium femoral component and factors affecting survivorship. Clin Orthop Relat Res 471:3262–3269. https://doi.org/10.1007/s11999-013-3033-4
Kanto M, Fukunishi S, Fukui T, Nishio S, Fujihara Y, Okahisa S, Takeda Y, Yoshiya S, Tachibana T (2020) Radiological evaluation of the relationship between cortical hypertrophy and stress shielding after total hip arthroplasty using a cementless stem. Arthroplast Today 6:894–900. https://doi.org/10.1016/j.artd.2020.09.018
Katsimihas M, Katsimihas G, Lee MB, Learmonth ID (2006) Distal femoral cortical hypertrophy: predisposing factors and their effect on clinical outcome. Hip Int 16:18–22. https://doi.org/10.5301/hip.2008.967
Brodt S, Matziolis G, Buckwitz B, Zippelius T, Strube P, Roth A (2020) Long-term follow-up of bone remodelling after cementless hip arthroplasty using different stems. Sci Rep 10:10143. https://doi.org/10.1038/s41598-020-67189-x
Goto K, Furuya Y, Oda K, Minami R, Sano K, Sugimoto M, Matsuda S (2018) Long-term results of total hip arthroplasty using Charnley Elite-Plus stem and the effect of stem geometry on radiographic distal femoral cortical hypertrophy. J Orthop Sci 23:365–370. https://doi.org/10.1016/j.jos.2017.12.003
Iwase T, Morita D, Takemoto G (2020) The effects of patient characteristics and stem alignment on distal femoral cortical hypertrophy after cemented polished tapered stem implantation. Eur J Orthop Surg Traumatol 30:559–567. https://doi.org/10.1007/s00590-019-02605-1
Evans AL, Paggiosi MA, Eastell R, Walsh JS (2015) Bone density, microstructure and strength in obese and normal weight men and women in younger and older adulthood. J bone Miner Res 30:920–928. https://doi.org/10.1002/jbmr.2407
Prieto-Alhambra D, Premaor MO, FinaAvilés F, Hermosilla E, Martinez-Laguna D, Carbonell-Abella C, Nogués X, Compston JE, Díez-Pérez A (2012) The association between fracture and obesity is site-dependent: a population-based study in postmenopausal women. J bone Miner Res 27:294–300. https://doi.org/10.1002/jbmr.1466
Alswat KA (2017) Gender disparities in osteoporosis. J Clin Med Res. 9:382–387. https://doi.org/10.14740/jocmr2970w
Pitto RP, Mueller LA, Reilly K, Schmidt R, Munro J (2007) Quantitative computer-assisted osteodensitometry in total hip arthroplasty. Int Orthop 31:431–438. https://doi.org/10.1007/s00264-006-0257-x
Gausden EB, Beiene ZA, Blevins JL, Christ AB, Chalmers BP, Helfet DL, Sculco PK, Mayman DJ (2021) Periprosthetic femur fractures after total hip arthroplasty: does the mode of failure correlate with classification? J Arthroplasty 36:2597–2602. https://doi.org/10.1016/j.arth.2021.02.048
Marsland D, Mears SC (2012) A review of periprosthetic femoral fractures associated with total hip arthroplasty. Geriatr Orthop Surg Rehabil 3:107–120. https://doi.org/10.1177/2151458512462870
Deng J, Wang G, Li J, Wang S, Li M, Yin X, Zhang L, Tang P (2021) A systematic review and meta-analysis comparing arthroplasty and internal fixation in the treatment of elderly displaced femoral neck fractures. OTA Int 4:e087. https://doi.org/10.1097/OI9.0000000000000087
Ries C, Boese CK, Dietrich F, Miehlke W, Heisel C (2019) Femoral stem subsidence in cementless total hip arthroplasty: a retrospective single-centre study. Int Orthop 43:307–314. https://doi.org/10.1007/s00264-018-4020-x
Campbell D, Mercer G, Nilsson KG, Wells V, Field JR, Callary SA (2011) Early migration characteristics of a hydroxyapatite-coated femoral stem: an RSA study. Int Orthop 35:483–488. https://doi.org/10.1007/s00264-009-0913-z
Rattanaprichavej P, Laoruengthana A, Chotanaphuti T, Khuangsirikul S, Phreethanutt C, Pongpirul K (2019) Subsidence of hydroxyapatite-coated femoral stem in dorr type C proximal femoral morphology. J Arthroplasty 34:2011–2015. https://doi.org/10.1016/j.arth.2019.05.017
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have not published, posted, or submitted any other papers from this study. The authors have no disclosures or conflicts of interest.
Ethical approval
Ethical approval was granted by UAB Institutional Review Board for this study.
Informed consent
Informed consent was not required for this study per our institutions IRB.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Messner, M., Jacob, R., Hagewood, J. et al. Bone remodeling and cortical thinning distal to the femoral stem: a retrospective review. Arch Orthop Trauma Surg 143, 6461–6467 (2023). https://doi.org/10.1007/s00402-023-04860-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04860-8