Abstract
Introduction
The aim of this study was to examine if robotic-assisted total knee arthroplasty (RATKA) is cost- and time-effective in terms of implant stock and perioperative parameters, as optimizing perioperative efficiency may contribute to value-based care.
Materials and methods
Four hundred thirty-two consecutive patients who received primary total knee arthroplasties (TKAs) from May 2017 to March 2020 in a regional hospital were included in this study. Operating room time (OR time), surgical time, number of trays, insert thickness, and length of stay (LOS) were assessed and compared for a cohort group with navigation-assisted procedures to a group with robotic-assisted procedures (MAKO, Stryker, USA). Prediction of implant size was assessed for the robotic-assisted group. The Mann–Whitney U test was used for comparisons between groups when the normality assumption was not met. Categorical variables were assessed using the Fisher’s exact test. p < 0.05 was considered statistically significant.
Results
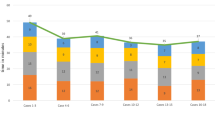
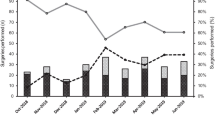
In the RATKA group, we noticed a significant mean reduction of 11 min in total OR time (p < 0.001), the use of thinner insert (p < 0.001), and a shorter mean length of stay of 1 day (p < 0.001). Compared to the navigation group, surgical time was not significantly longer, nor clinically relevant (0.238). In 76.9% of the robotic-assisted cases, the estimated implant size was equal to the final size and in all other cases, the preoperative implant size was oversized.
Conclusion
The introduction of the MAKO robotic-assisted total knee arthroplasty resulted in a gain in operating room time, a thinner and more predictable insert thickness, a shorter length of stay in hospital, and less instrumentation compared to navigation-assisted procedures.
Level of evidence
Level III, Retrospective cohort study.


Similar content being viewed by others
Data availability
All data are anonymous available in a computer database.
Abbreviations
- ASA:
-
American Society of Anesthesiologists
- BMI:
-
Body mass index
- CPM:
-
Continuous passive motion
- IRB:
-
Institutional review board
- LMWH:
-
Low-molecular-weight heparins
- LOS:
-
Length of stay
- OR:
-
Operation room
- RATKA:
-
Robotic-assisted total knee arthroplasty
- SD:
-
Standard deviation
- THA:
-
Total hip arthroplasty
- TKA:
-
Total Knee Arthroplasty
- UKA:
-
Unicompartmental knee arthroplasty
References
Naziri Q, Burekhovich SA, Mixa PJ et al (2019) The trends in robotic-assisted knee arthroplasty: a statewide database study. J Orthop 16:298–301. https://doi.org/10.1016/j.jor.2019.04.020
Lang JE, Mannava S, Floyd AJ et al (2011) Robotic systems in orthopaedic surgery. J. Bone Jt. Surg. Ser. B 93:1296–1299
Jacofsky DJ, Allen M (2016) Robotics in arthroplasty: a comprehensive review. J Arthroplasty 31:2353–2363
Lonner JH (2009) Indications for unicompartmental knee arthroplasty and rationale for robotic arm-assisted technology. Am J Orthop (Belle Mead NJ) 38:3–6
Lonner JH, Moretti VM (2016) The evolution of image-free robotic assistance in unicompartmental knee arthroplasty. Am J Orthop (Belle Mead NJ) 45:249–254
Lonner JH, Fillingham YA (2018) Pros and cons: a balanced view of robotics in knee arthroplasty. J Arthroplasty 33:2007–2013. https://doi.org/10.1016/j.arth.2018.03.056
Pierce J, Needham K, Adams C et al (2020) Robotic arm-assisted knee surgery: an economic analysis. Am J Manag Care 26:205–210. https://doi.org/10.37765/AJMC.2020.43763
Cotter EJ, Wang J, Illgen RL (2020) Comparative cost analysis of robotic-assisted and jig-based manual primary total knee arthroplasty. J Knee Surg. https://doi.org/10.1055/S-0040-1713895
Sousa PL, Sculco PK, Mayman DJ et al (2020) Robots in the operating room during hip and knee arthroplasty. Curr Rev Musculoskelet Med 13:309. https://doi.org/10.1007/S12178-020-09625-Z
Sodhi N, Khlopas A, Piuzzi NS et al (2018) The learning curve associated with robotic total knee arthroplasty. J Knee Surg 31:17–21. https://doi.org/10.1055/S-0037-1608809/ID/JR17SEP0024SSA-15
Marchand KB, Ehiorobo J, Mathew KK et al (2020) Learning curve of robotic-assisted total knee arthroplasty for a high-volume surgeon. J Knee Surg. https://doi.org/10.1055/S-0040-1715126/ID/JR190398OA-25
Kayani B, Konan S, Huq SS et al (2019) Robotic-arm assisted total knee arthroplasty has a learning curve of seven cases for integration into the surgical workflow but no learning curve effect for accuracy of implant positioning. Knee Surgery, Sport Traumatol Arthrosc 27:1132. https://doi.org/10.1007/S00167-018-5138-5
Deckey DG, Rosenow CS, Verhey JT et al (2021) Robotic-assisted total knee arthroplasty improves accuracy and precision compared to conventional techniques. Bone Joint J 103:74–80. https://doi.org/10.1302/0301-620X.103B6.BJJ-2020-2003.R1
Mulier JP, De Boeck L, Meulders M et al (2015) Factors determining the smooth flow and the non-operative time in a one-induction room to one-operating room setting. J Eval Clin Pract 21:205–214. https://doi.org/10.1111/JEP.12288
Sires JD, Craik JD, Wilson CJ (2019) Accuracy of bone resection in MAKO total knee robotic-assisted surgery. J Knee Surg. https://doi.org/10.1055/s-0039-1700570
Marchand KB, Salem HS, Mathew KK et al (2021) The accuracy of computed tomography-based, three-dimensional implant planning in robotic-assisted total knee arthroplasty. J Knee Surg. https://doi.org/10.1055/S-0041-1729548
Zhang J, Ndou WS, Ng N et al (2021) Robotic-arm assisted total knee arthroplasty is associated with improved accuracy and patient reported outcomes: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/S00167-021-06464-4
Archer A, Salem HS, Coppolecchia A, Mont MA (2021) Lengths of stay and discharge dispositions after total knee arthroplasty: a comparison of robotic-assisted and manual techniques. J Knee Surg. https://doi.org/10.1055/S-0041-1735280
Tompkins GS, Sypher KS, Li HF et al (2021) Robotic vs manual total knee arthroplasty in high volume surgeons: a comparison of cost and quality metrics. J Arthroplasty. https://doi.org/10.1016/J.ARTH.2021.12.018
Abdelfadeel W, Houston N, Star A et al (2020) CT planning studies for robotic total knee arthroplasty. Bone Joint J 102:79–84. https://doi.org/10.1302/0301-620X.102B6.BJJ-2019-1498.R1
Koolmees D, Bernstein DN, Makhni EC (2021) Time-driven activity-based costing provides a lower and more accurate assessment of costs in the field of orthopaedic surgery compared with traditional accounting methods. Arthroscopy 37:1620–1627. https://doi.org/10.1016/J.ARTHRO.2020.11.028
Fang CJ, Mazzocco JC, Sun DC et al (2022) Total knee arthroplasty hospital costs by time-driven activity-based costing: robotic vs conventional. Arthroplast Today 13:43. https://doi.org/10.1016/J.ARTD.2021.11.008
Maritan G, Franceschi G, Nardacchione R et al (2022) Similar survivorship at the 5-year follow-up comparing robotic-assisted and conventional lateral unicompartmental knee arthroplasty. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/S00167-022-07218-6
Mont MA, Cool C, Gregory D et al (2021) Health care utilization and payer cost analysis of robotic arm assisted total knee arthroplasty at 30, 60, and 90 days. J Knee Surg 34:328–337. https://doi.org/10.1055/S-0039-1695741/ID/JR190145OA-23
Cool CL, Jacofsky DJ, Seeger KA et al (2019) A 90-day episode-of-care cost analysis of robotic-arm assisted total knee arthroplasty. J Comp Eff Res 8:327–336. https://doi.org/10.2217/CER-2018-0136/ASSET/IMAGES/LARGE/FIGURE1.JPEG
Funding
No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
GL has a financial conflict of interest with Stryker, he received speaker and consultancy fee.
Institutional review board ethical approval was awarded prior to study initiation. This article was primary edited by L. Loomans.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Loomans, L., Leirs, G. & Vandenneucker, H. Operating room efficiency after the implementation of MAKO robotic-assisted total knee arthroplasty. Arch Orthop Trauma Surg 143, 5501–5506 (2023). https://doi.org/10.1007/s00402-023-04834-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-023-04834-w