Abstract
Background
It is unclear whether there is a difference in the incidence of postoperative fever (POF) between hip, knee and shoulder arthroplasty. The influence of a trauma setting has not been investigated.
Methods
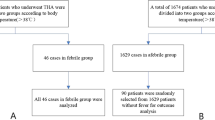
A retrospective review was performed on 675 joint replacement surgeries (hip, knee, shoulder arthroplasty) in an elective or trauma setting over a 2 year period (2016–2018). Patient demographics and perioperative/postoperative parameters were investigated. The fever curve was characterized. The results and costs of any fever-related diagnostic workup were reviewed.
Results
A total of 89 patients (13.2%) experienced a POF ≥ 38.0 °C, only 21 patients (3.1%) a POF ≥ 38.5 °C (of the latter: 4.6% of hip arthroplasties, 0.6% of knee arthroplasties, 0% of shoulder arthroplasties). There was a significantly greater risk (OR 3.88) for POF ≥ 38.5 °C in trauma total hip arthroplasty (THA) compared to elective THA (10.6 vs. 3.0%; p < 0.01). Differences in POF rate between the various joint areas were statistically insignificant when comparing only elective and trauma cases with each other, even though there was a trend for higher rates in hip surgery. Patients experiencing POF ≥ 38.5 °C were more often males (p < 0.01) and had an increased intraoperative blood loss (p = 0.03) and longer hospital stay (p < 0.01). There was only 1/89 POF patients developing an early periprosthetic joint infection. The cost of a positive fever workup (3/27 patients, 11.1%) leading to a new diagnosis and treatment was 2045 US$.
Conclusion
POF ≥ 38.5 °C was more frequent in traumatic THA compared to elective THA. A trend of difference between POF rates between the different joint areas was statistically insignificant after separating elective and traumatic cases. The risk of developing an early periprosthetic joint infection was not increased in POF. A fever-related diagnostic workup was rarely helpful in the absence of clinical symptoms.



Similar content being viewed by others
References
Dimitriou D, Helmy N, Hasler J, Flury A, Finsterwald M, Antoniadis A (2019) The role of total hip arthroplasty through the direct anterior approach in femoral neck fracture and factors affecting the outcome. J Arthroplasty 34:82–87. https://doi.org/10.1016/j.arth.2018.08.037
Dimitriou D, Antoniadis A, Flury A, Liebhauser M, Helmy N (2018) Total hip arthroplasty improves the quality-adjusted life years in patients who exceeded the estimated life expectancy. J Arthroplasty 33:3484–3489. https://doi.org/10.1016/j.arth.2018.07.005
Ashley B, Spiegel DA, Cahill P, Talwar D, Baldwin KD (2017) Post-operative fever in orthopaedic surgery: how effective is the ‘fever workup?’ J Orthop Surg 25:1–9. https://doi.org/10.1177/2309499017727953
Andres BM, Taub DD, Gurkan I, Wenz JE (2003) Postoperative fever after total knee arthroplasty: the role of cytokines. Clin Orthop Relat Res. https://doi.org/10.1097/01.blo.0000093914.26658.55
Saltzman BM, Mayo BC, Bohl DD, Frank RM, Cole BJ, Verma NN et al (2017) Evaluation of fever in the immediate post-operative period following shoulder arthroplasty. Bone Jt J 99B:1515–1519. https://doi.org/10.1302/0301-620X.99B11.BJJ-2017-0469.R1
Summersell PC, Turnbull A, Long G, Diwan A, Macdessi S, Cooke PJ et al (2003) Temperature trends in total hip arthroplasty: a retrospective study. J Arthroplasty. https://doi.org/10.1016/S0883-5403(03)00015-9
Bindelglass DF, Pellegrino J (2007) The role of blood cultures in the acute evaluation of postoperative fever in arthroplasty patients. J Arthroplasty 22:701–702. https://doi.org/10.1016/j.arth.2006.09.007
Anderson JT, Osland JD (2009) Blood cultures for evaluation of fever after total joint arthroplasty. Am J Orthop (Belle Mead NJ) 38:134–136
Yoo JH, Restrepo C, Chen AF, Parvizi J (2017) Routine workup of postoperative pyrexia following total joint arthroplasty is only necessary in select circumstances. J Arthroplasty 32:520–525. https://doi.org/10.1016/j.arth.2016.09.025
Ward DT, Hansen EN, Takemoto SK, Bozic KJ (2010) Cost and effectiveness of postoperative fever diagnostic evaluation in total joint arthroplasty patients. J Arthroplasty 25:43–48. https://doi.org/10.1016/j.arth.2010.03.016
Yoo JH, Kim KT, Kim TY, Hwang JH, Chang JD (2017) Postoperative fever after hemiarthroplasty in elderly patients over 70 years of age with displaced femoral neck fracture: necessity of routine workup? Injury 48:441–446. https://doi.org/10.1016/j.injury.2016.12.013
Khan N, Troelsen A, Husted H (2015) Prevention of post-operative anaemia in hip and knee arthroplasty – a systematic review. Dan Med J 62:A5170
Petretta R, McConkey M, Slobogean GP, Handel J, Broekhuyse HM (2013) Incidence, risk factors, and diagnostic evaluation of postoperative fever in an orthopaedic trauma population. J Orthop Trauma 27:558–562. https://doi.org/10.1097/BOT.0b013e31828af4df
Sivakumar B, Vijaysegaran P, Ottley M, Crawford R, Coulter C (2012) Blood cultures for evaluation of early postoperative fever after femoral neck fracture surgery. J Orthop Surg (Hong Kong) 20:336–340. https://doi.org/10.1177/230949901202000314
Karam JA, Zmistowski B, Restrepo C, Hozack WJ, Parvizi J (2014) Fewer postoperative fevers: an unexpected benefit of multimodal pain management? Clin Orthop Relat Res 472:1489–1495. https://doi.org/10.1007/s11999-014-3555-4
Jules-Elysee KM, Wilfred SE, Memtsoudis SG, Kim DH, YaDeau JT, Urban MK et al (2012) Steroid modulation of cytokine release and desmosine levels in bilateral total knee replacement. J Bone Jt Surgery-American. https://doi.org/10.2106/jbjs.k.00995
Tan TL, Shohat N, Rondon AJ, Foltz C, Goswami K, Ryan SP et al (2019) Perioperative antibiotic prophylaxis in total joint arthroplasty: a single dose is as effective as multiple doses. J Bone Jt Surg - Am. https://doi.org/10.2106/JBJS.18.00336
Ishii Y, Noguchi H, Takeda M, Sato J, Takayama S, Toyabe SI (2014) Characteristics and significance of fever during 4 weeks after primary total knee arthroplasty. Arch Orthop Trauma Surg 134:707–712. https://doi.org/10.1007/s00402-014-1949-0
Shetty V, Kasture S (2013) Is immediate postoperative fever related to drop in haemoglobin? A comparative study in simultaneous bilateral total knee arthroplasty patients. Eur J Orthop Surg Traumatol 23:345–347. https://doi.org/10.1007/s00590-012-0969-0
Kennedy JG, Rodgers WB, Zurakowski D, Sullivan R, Griffin D, Beardsley W et al (1997) Pyrexia after total knee replacement. A cause for concern? Am J Orthop (Belle Mead NJ) 26:549–52
Tai TW, Chang CW, Lin CJ, Lai KA, Yang CY (2009) Elevated temperature trends after total knee arthroplasty. Orthopedics 32:886. https://doi.org/10.3928/01477447-20091020-05
Xu N, Xu T, Tan X, Xu L, Ye M, Pan Y et al (2021) Fluid homeostasis may predict the prognosis of non-infectious fever after total knee arthroplasty within 7-day: a retrospective cohort study. Front Surg 8:1–7. https://doi.org/10.3389/fsurg.2021.690803
Vijaysegaran P, Coulter SA, Coulter C, Crawford RW (2012) Blood cultures for assessment of postoperative fever in arthroplasty patients. J Arthroplasty 27:375–377. https://doi.org/10.1016/j.arth.2011.05.025
Funding
This research did not receive any specific grant from funding agencies in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis was performed largely by SR with the support of AF and TT. The first draft of the manuscript was written by SR and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
Naeder Helmy receives royalties from Medacta International (Switzerland) and he is a medical advisor of Medacta International (Switzerland), Bayer AG, and Mathys (Switzerland). These affiliations are NOT relevant to the content of this research article, though. The other authors have no competing interests to declare that are relevant to the content of this article.
Ethical approval
This retrospective chart review study involving human participants was in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The local Human Investigation Committee (IRB) approved this study.
Informed consent
Informed consent was obtained from all individual participants included in the study. Patients signed informed consent regarding publishing their data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Radzanowski, S., Flury, A., Tondelli, T. et al. Postoperative fever: differences between elective vs. traumatic hip, knee and shoulder arthroplasty. Arch Orthop Trauma Surg 143, 4077–4084 (2023). https://doi.org/10.1007/s00402-022-04716-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04716-7