Abstract
Introduction
Arthrofibrosis remains a common cause of patient dissatisfaction and reoperation after total knee arthroplasty (TKA). Losartan is an angiotensin receptor blocker (ARB) with inhibitory effects on transforming growth factor beta, previously implicated in tissue repair induced fibrosis, and has been studied to prevent stiffness following hip arthroscopy. This study aimed to evaluate pre- and postoperative range of motion (ROM) and the incidence of manipulation under anesthesia (MUA) following primary TKA in patients taking Losartan preoperatively for hypertension.
Materials and methods
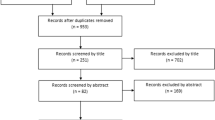
A retrospective review of 170 patients from 2012 to 2020 who underwent a primary, elective TKA and were prescribed Losartan at least three months prior to surgery. All patients who were prescribed Losartan and had a preoperative and postoperative ROM in their chart were included and were matched to a control group of patients who underwent TKA and had no Losartan prescription. ROM, MUA, readmissions, reoperations, and revisions were assessed using chi-square and independent sample t tests.
Results
Seventy-nine patients met the inclusion criteria. Preoperative ROM was similar between patients on Losartan and the control group (103.59° ± 16.14° vs. 104.59° ± 21.59°, respectively; p = 0.745). Postoperative ROM and ΔROM were greater for patients prescribed Losartan (114.29° ± 12.32° vs. 112.76° ± 11.65°; p = 0.429 and 10.57° ± 14.95° vs. 8.17° ± 21.68°; p = 0.422), though this difference did not reach statistical significance. There was no difference in readmission, rate of manipulation for stiffness, or all-cause revision rates.
Conclusion
In this study, we found that the use of Losartan did not significantly improve postoperative ROM, reduce MUA or decrease revision rates. Further prospective studies using Losartan are required to elucidate the potential effects on ROM and incidence of arthrofibrosis requiring MUA.
Level III evidence
Retrospective cohort study.

Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, J.C.R, upon reasonable request.
References
Rutherford RW, Jennings JM, Levy DL et al (2018) Revision total knee arthroplasty for arthrofibrosis. J Arthroplasty. https://doi.org/10.1016/j.arth.2018.03.037
Schroer WC, Berend KR, Lombardi AV et al (2013) Why are total knees failing today? Etiology of total knee revision in 2010 and 2011. J Arthroplasty. https://doi.org/10.1016/j.arth.2013.04.056
Mayr HO, Weig TG, Plitz W (2004) Arthrofibrosis following ACL reconstruction—reasons and outcome. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-004-0718-x
Stephenson JJ, Quimbo RA, Gu T (2010) Knee-attributable medical costs and risk of re-surgery among patients utilizing non-surgical treatment options for knee arthrofibrosis in a managed care population. Curr Med Res Opin. https://doi.org/10.1185/03007991003676479
Lam LO, Swift S, Shakespeare D (2003) Fixed flexion deformity and flexion after knee arthroplasty. What happens in the first 12 months after surgery and can a poor outcome be predicted? Knee. https://doi.org/10.1016/S0968-0160(02)00102-3
Abdul N, Dixon D, Walker A et al (2015) Fibrosis is a common outcome following total knee arthroplasty. Sci Rep. https://doi.org/10.1038/srep16469
Lee S, Sakurai T, Ohsako M et al (2010) Tissue stiffness induced by prolonged immobilization of the rat knee joint and relevance of AGEs (pentosidine). Connect Tissue Res. https://doi.org/10.3109/03008201003686941
Kalson NS, Borthwick LA, Mann DA, Deehan DJ (2016) International consensus on the definition and classification of fibrosis of the knee joint. Bone Jt J. https://doi.org/10.1302/0301-620X.98B10.37957
Kim KK, Sheppard D, Chapman HA (2018) TGF-β1 signaling and tissue fibrosis. Cold Spring Harb Perspect Biol. https://doi.org/10.1101/cshperspect.a022293
Meng XM, Nikolic-Paterson DJ, Lan HY (2016) TGF-β: the master regulator of fibrosis. Nat Rev Nephrol 12(6):325–338. https://doi.org/10.1038/nrneph.2016.48
Lim DS, Lutucuta S, Bachireddy P et al (2001) Angiotensin II blockade reverses myocardial fibrosis in a transgenic mouse model of human hypertrophic cardiomyopathy. Circulation. https://doi.org/10.1161/01.CIR.103.6.789
Otsuka M, Takahashi H, Shiratori M et al (2004) Reduction of bleomycin induced lung fibrosis by candesartan cilexetil, an angiotensin II type 1 receptor antagonist. Thorax. https://doi.org/10.1136/thx.2003.000893
Paizis G, Gilbert RE, Cooper ME et al (2001) Effect of angiotensin II type 1 receptor blockade on experimental hepatic fibrogenesis. J Hepatol. https://doi.org/10.1016/S0168-8278(01)00146-5
Suga SI, Mazzali M, Ray PE et al (2002) Angiotensin ii type 1 receptor blockade ameliorates tubulointerstitial injury induced by chronic potassium deficiency. Kidney Int. https://doi.org/10.1046/j.1523-1755.2002.00208.x
Colebatch AN, Hart DJ, Zhai G et al (2009) Effective measurement of knee alignment using AP knee radiographs. Knee. https://doi.org/10.1016/j.knee.2008.07.007
Kane LT, Fang T, Galetta MS et al (2019) Propensity score matching: a statistical method. Clin Spine Surg. https://doi.org/10.1097/BSD.0000000000000932
Caliendo M, Kopeinig S (2008) Some practical guidance for the implementation of propensity score matching. J Econ Surv. https://doi.org/10.1111/j.1467-6419.2007.00527.x
Austin PC (2009) Some methods of propensity-score matching had superior performance to others: results of an empirical investigation and monte carlo simulations. Biometr J. https://doi.org/10.1002/bimj.200810488
Burks TN, Cohn RD (2011) Role of TGF-β signaling in inherited and acquired myopathies. Skeletal Muscle 1(1):19. https://doi.org/10.1186/2044-5040-1-19
Mann CJ, Perdiguero E, Kharraz Y et al (2011) Aberrant repair and fibrosis development in skeletal muscle. Skeletal Muscle 1(1):21. https://doi.org/10.1186/2044-5040-1-21
Serrano AL, Mann CJ, Vidal B et al (2011) Cellular and molecular mechanisms regulating fibrosis in skeletal muscle repair and disease. Curr Top Dev Biol 96:167–201. https://doi.org/10.1016/B978-0-12-385940-2.00007-3
Serrano AL, Muñoz-Cánoves P (2010) Regulation and dysregulation of fibrosis in skeletal muscle. Exp Cell Res 316:3050–3058. https://doi.org/10.1016/J.YEXCR.2010.05.035
Bedair HS, Karthikeyan T, Quintero A et al (2008) Angiotensin II receptor blockade administered after injury improves muscle regeneration and decreases fibrosis in normal skeletal muscle. Am J Sports Med. https://doi.org/10.1177/0363546508315470
Kobayashi T, Uehara K, Ota S et al (2013) The timing of administration of a clinically relevant dose of losartan influences the healing process after contusion induced muscle injury. J Appl Physiol. https://doi.org/10.1152/japplphysiol.00140.2011
Garg K, Corona BT, Walters TJ (2014) Losartan administration reduces fibrosis but hinders functional recovery after volumetric muscle loss injury. J Appl Physiol. https://doi.org/10.1152/japplphysiol.00689.2014
Kobayashi M, Ota S, Terada S et al (2016) The combined use of losartan and muscle-derived stem cells significantly improves the functional recovery of muscle in a young mouse model of contusion injuries. Am J Sports Med. https://doi.org/10.1177/0363546516656823
Langston JR, Ramsey DC, Skoglund K, Schabel K (2020) Angiotensin II blockade had no effect on range of motion after total knee arthroplasty: a retrospective review. J Orthop Surg Res. https://doi.org/10.1186/s13018-020-1555-5
Hernandez NM, Cunningham DJ, Kabirian N et al (2021) Angiotensin receptor blockers were not associated with decreased arthrofibrosis after total knee arthroplasty. Orthopedics. https://doi.org/10.3928/01477447-20201216-09
Mohammed R, Syed S, Ahmed N (2009) Manipulation under anaesthesia for stiffness following knee arthroplasty. Ann R Coll Surg Engl. https://doi.org/10.1308/003588409X359321
Kim GK, Mortazavi SMJ, Parvizi J, Purtill JJ (2012) Revision for stiffness following TKA: a predictable procedure? Knee. https://doi.org/10.1016/j.knee.2011.06.016
Lizaur A, Marco L, Cebrian R (1997) Preoperative factors influencing the range of movement after total knee arthroplasty for severe osteoarthritis. J Bone Jt Surg Br. https://doi.org/10.1302/0301-620x.79b4.0790626
Gadinsky NE, Ehrhardt JK, Urband C, Westrich GH (2011) Effect of body mass index on range of motion and manipulation after total knee arthroplasty. J Arthroplasty. https://doi.org/10.1016/j.arth.2010.12.004
Funding
No funding was provided for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
JA, KAL, VS and BF have nothing to disclose. RS reports being a board or committee member for AAOS and AAHKS, being part of the editorial or governing board for Arthroplasty Today and JOA, having stock and stock options in Gauss surgical and PSI, being a paid consultant and having stock or stock options in Intelijoint, and being a paid consultant and receiving IP royalties and research support from Smith and Nephew. JR reports being a board or committee member for NYSSO.
Ethical approval
Our Institutional Review Board (IRB) approved the present study.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Arraut, J., Lygrisse, K.A., Singh, V. et al. The effect of losartan on range of motion and rates of manipulation in total knee arthroplasty: a retrospective matched cohort study. Arch Orthop Trauma Surg 143, 4043–4048 (2023). https://doi.org/10.1007/s00402-022-04696-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04696-8