Abstract
Introduction
While the incidence of reverse total shoulder arthroplasty (rTSA) is increasing constantly, newer implants with designs other than the classic Grammont geometry are gaining importance. More anatomic inclination angles and lateralization are supposed to have a positive impact on clinical results and complication rates. Presentation of midterm results therefore is important to support these assumptions. The aim of this study was to report the midterm clinical outcome of primary rTSA with an uncemented humeral short-stem prosthesis (USSP) with a humeral inclination angle of 145° and the analysis of different variables on the outcome.
Methods
This is a retrospective study of all patients with primary rTSA using an USSP and a combined humeral inclination angle of 145° (Ascend™ flex, Stryker) with a minimum clinical follow-up of 2 years. The implant combines a 132.5° inclination for the humeral stem with an additional 12.5° for the polyethylene inlay. Primary outcomes were patient-reported outcome measures: ASES score, simple shoulder test (SST) and subjective shoulder value (SSV). Secondary outcomes were complication and revision rates.
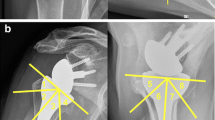
We analyzed different variables: preoperatively gender, age, indication for surgery and status of rotator cuff. Also, the glenoid morphology was classified according to Walch and a proximal humerus cortical bone thickness measurement (CBT avg) of 6 mm was used as a threshold for osteoporosis. Postoperatively, we analyzed different radiologic parameters: filling ratio, distalization and lateralization angles according to Boutsiadis.
Results
A total of 84 out of 99 (85%) patients with a mean FU of 46.7 months (range 24–80 months) could be included: 62 women and 22 men with a mean age of 74.7 years. Mean ASES score significantly increased from 47 preoperatively to 85.8 at the last follow-up (p = 0.001). The postoperative SST reached an average of 65.3 and the mean SSV was 83%. None of the variable parameters analyzed could be identified as a risk factor for a lower outcome defined as a SSV < 70. Three patients (3.6%) had a complication: one incomplete lower plexus lesion, one dislocation and one major hematoma. Surgical revision was needed in two cases (2.4%).
Conclusion
The midterm clinical outcome of primary reverse total shoulder arthroplasty (rTSA) with an uncemented humeral short stem and a humeral inclination angle of 145° showed good-to-excellent results with a low complication and revision rate independent from a wide range of pre- and postoperative variables. PROMs are comparable to those reported for anatomic TSA with a low complication rate, different to historical studies especially with the Grammont design.
Level of evidence
Treatment study, Level IV.



Similar content being viewed by others
References
Alentorn-Geli E, Samitier G, Torrens C et al (2015) Reverse shoulder arthroplasty. Part 2: Systematic review of reoperations, revisions, problems, and complications. Int J Shoulder Surg 9:60–67
Baulot E, Sirveaux F, Boileau P (2011) Grammont’s idea: the story of Paul Grammont’s functional surgery concept and the development of the reverse principle. Clin Orthop Relat Res 469:2425–2431
Bedeir YH, Gawish HM, Grawe BM (2020) Outcomes of Reverse Total Shoulder Arthroplasty in Patients 60 Years of Age or Younger: A Systematic Review. J Hand Surg Am 45:254 e251–254 e258
Bercik MJ, Kruse K 2nd, Yalizis M et al (2016) A modification to the Walch classification of the glenoid in primary glenohumeral osteoarthritis using three-dimensional imaging. J Shoulder Elbow Surg 25:1601–1606
Berliner JL, Regalado-Magdos A, Ma CB et al (2015) Biomechanics of reverse total shoulder arthroplasty. J Shoulder Elbow Surg 24:150–160
Boileau P, Morin-Salvo N, Gauci MO et al (2017) Angled BIO-RSA (bony-increased offset-reverse shoulder arthroplasty): a solution for the management of glenoid bone loss and erosion. J Shoulder Elbow Surg 26:2133–2142
Boutsiadis A, Lenoir H, Denard PJ et al (2018) The lateralization and distalization shoulder angles are important determinants of clinical outcomes in reverse shoulder arthroplasty. J Shoulder Elbow Surg 27:1226–1234
Brewley EE Jr, Christmas KN, Gorman RA 2nd et al (2020) Defining the younger patient: age as a predictive factor for outcomes in shoulder arthroplasty. J Shoulder Elbow Surg 29:S1–S8
Carducci MP, Zimmer ZR, Jawa A (2019) Predictors of unsatisfactory patient outcomes in primary reverse total shoulder arthroplasty. J Shoulder Elbow Surg 28:2113–2120
Coscia AC, Matar RN, Espinal EE et al (2021) Does preoperative diagnosis impact patient outcomes following reverse total shoulder arthroplasty? A systematic review. J Shoulder Elbow Surg 30:1458–1470
Cronin KJ, Magnuson JA, Murphy ML et al (2021) Responsiveness of patient-reported outcomes in shoulder arthroplasty: what are we actually measuring? J Shoulder Elbow Surg 30:1174–1180
Denard PJ, Noyes MP, Walker JB et al (2018) Radiographic changes differ between two different short press-fit humeral stem designs in total shoulder arthroplasty. J Shoulder Elbow Surg 27:217–223
Dimock R, Fathi Elabd M, Imam M et al (2021) Bony increased-offset reverse shoulder arthroplasty: A meta-analysis of the available evidence. Shoulder Elbow 13:18–27
Drager J, Polce EM, Fu M et al. (2021) Patients Undergoing Anatomic Total Shoulder Arthroplasty Achieve Clinically Significant Outcomes Faster than those Undergoing Reverse Shoulder Arthroplasty. J Shoulder Elbow Surg
Eichinger JK, Galvin JW (2015) Management of complications after total shoulder arthroplasty. Curr Rev Musculoskelet Med 8:83–91
Ek ET, Neukom L, Catanzaro S et al (2013) Reverse total shoulder arthroplasty for massive irreparable rotator cuff tears in patients younger than 65 years old: results after five to fifteen years. J Shoulder Elbow Surg 22:1199–1208
Erickson BJ, Frank RM, Harris JD et al (2015) The influence of humeral head inclination in reverse total shoulder arthroplasty: a systematic review. J Shoulder Elbow Surg 24:988–993
Ferle M, Pastor MF, Hagenah J et al (2019) Effect of the humeral neck-shaft angle and glenosphere lateralization on stability of reverse shoulder arthroplasty: a cadaveric study. J Shoulder Elbow Surg 28:966–973
Friedman RJ, Hawthorne KB, Genez BM (1992) The use of computerized tomography in the measurement of glenoid version. J Bone Joint Surg Am 74:1032–1037
Godeneche A, Garret J, Barth J et al (2019) Comparison of revision rates and radiographic observations of long and short, uncoated and coated humeral stem designs in total shoulder arthroplasty. EFORT Open Rev 4:70–76
Goldberg SS, Baranek ES, Korbel KC et al. (2021) Anatomic total shoulder arthroplasty using a stem-free ellipsoid humeral implant in patients of all ages. J Shoulder Elbow Surg
Goutallier D, Postel JM, Bernageau J et al. (1994) Fatty muscle degeneration in cuff ruptures. Pre- and postoperative evaluation by CT scan. Clin Orthop Relat Res:78–83
Greiner S, Schmidt C, Herrmann S et al (2015) Clinical performance of lateralized versus non-lateralized reverse shoulder arthroplasty: a prospective randomized study. J Shoulder Elbow Surg 24:1397–1404
Greiner SH, Back DA, Herrmann S et al (2010) Degenerative changes of the deltoid muscle have impact on clinical outcome after reversed total shoulder arthroplasty. Arch Orthop Trauma Surg 130:177–183
Jensen AR, Tangtiphaiboontana J, Marigi E et al. (2021) Anatomic total shoulder arthroplasty for primary glenohumeral osteoarthritis is associated with excellent outcomes and low revision rates in the elderly. J Shoulder Elbow Surg
Kazley JM, Cole KP, Desai KJ et al (2019) Prostheses for reverse total shoulder arthroplasty. Expert Rev Med Devices 16:107–118
Lenarz C, Shishani Y, Mccrum C et al (2011) Is reverse shoulder arthroplasty appropriate for the treatment of fractures in the older patient? Early observations. Clin Orthop Relat Res 469:3324–3331
Lung TS, Cruickshank D, Grant HJ et al (2019) Factors contributing to glenoid baseplate micromotion in reverse shoulder arthroplasty: a biomechanical study. J Shoulder Elbow Surg 28:648–653
Mather J, Macdermid JC, Faber KJ et al (2013) Proximal humerus cortical bone thickness correlates with bone mineral density and can clinically rule out osteoporosis. J Shoulder Elbow Surg 22:732–738
Mizuno N, Denard PJ, Raiss P et al (2013) Reverse total shoulder arthroplasty for primary glenohumeral osteoarthritis in patients with a biconcave glenoid. J Bone Joint Surg Am 95:1297–1304
Morwood MP, Johnston PS, Garrigues GE (2017) Proximal ingrowth coating decreases risk of loosening following uncemented shoulder arthroplasty using mini-stem humeral components and lesser tuberosity osteotomy. J Shoulder Elbow Surg 26:1246–1252
Nunes B, Linhares D, Costa F et al. (2020) Lateralized versus nonlateralized glenospheres in reverse shoulder arthroplasty: a systematic review with meta-analysis. J Shoulder Elbow Surg
P. Habermeyer SL, M. Loew, P. Magosch, F. Martetschläger, M. Tauber (2017) Schulterchirurgie. Urban & Fischer
Patte D (1990) Classification of rotator cuff lesions. Clin Orthop Relat Res:81–86
Phadnis J, Huang T, Watts A et al. (2016) Cemented or cementless humeral fixation in reverse total shoulder arthroplasty? a systematic review. Bone Joint J 98-B:65–74
Raiss P, Schnetzke M, Wittmann T et al (2019) Postoperative radiographic findings of an uncemented convertible short stem for anatomic and reverse shoulder arthroplasty. J Shoulder Elbow Surg 28:715–723
Samitier G, Alentorn-Geli E, Torrens C et al (2015) Reverse shoulder arthroplasty. Part 1: Systematic review of clinical and functional outcomes. Int J Shoulder Surg 9:24–31
Schnetzke M, Coda S, Raiss P et al (2016) Radiologic bone adaptations on a cementless short-stem shoulder prosthesis. J Shoulder Elbow Surg 25:650–657
Schnetzke M, Preis A, Coda S et al (2017) Anatomical and reverse shoulder replacement with a convertible, uncemented short-stem shoulder prosthesis: first clinical and radiological results. Arch Orthop Trauma Surg 137:679–684
Sershon RA, Van Thiel GS, Lin EC et al (2014) Clinical outcomes of reverse total shoulder arthroplasty in patients aged younger than 60 years. J Shoulder Elbow Surg 23:395–400
Shah SS, Gaal BT, Roche AM et al (2020) The modern reverse shoulder arthroplasty and an updated systematic review for each complication: part I. JSES Int 4:929–943
Shah SS, Roche AM, Sullivan SW et al (2021) The modern reverse shoulder arthroplasty and an updated systematic review for each complication: part II. JSES Int 5:121–137
Thomazeau H, Rolland Y, Lucas C et al (1996) Atrophy of the supraspinatus belly. Assessment by MRI in 55 patients with rotator cuff pathology. Acta Orthop Scand 67:264–268
Walch G, Badet R, Boulahia A et al (1999) Morphologic study of the glenoid in primary glenohumeral osteoarthritis. J Arthroplasty 14:756–760
Werner BC, Chang B, Nguyen JT et al (2016) What change in AmerAican shoulder and elbow surgeons score represents a clinically important change after shoulder arthroplasty? Clin Orthop Relat Res 474:2672–2681
Werner BS, Chaoui J, Walch G (2017) The influence of humeral neck shaft angle and glenoid lateralization on range of motion in reverse shoulder arthroplasty. J Shoulder Elbow Surg 26:1726–1731
Werner BS, Jacquot A, Mole D et al (2016) Is radiographic measurement of acromiohumeral distance on anteroposterior view after reverse shoulder arthroplasty reliable? J Shoulder Elbow Surg 25:e276-280
Zanetti M, Gerber C, Hodler J (1998) Quantitative assessment of the muscles of the rotator cuff with magnetic resonance imaging. Invest Radiol 33:163–170
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest regarding this manuscript. Independent from the submitted manuscript, received royalties/payments of all authors are listed: Payments for presentations from Waldemar Link, Zimmer Biomet, Heraeus, Ceramtec.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Approval by the local Ethical Committee of the “Ärztekammer Hamburg” with the case number PV7236 from 16.03.2020.
Informed consent:
All patients included had informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Linke, P., Linke, C., Neumann, J. et al. Midterm clinical outcome of uncemented short-stem reversed shoulder arthroplasty. Arch Orthop Trauma Surg 143, 3025–3036 (2023). https://doi.org/10.1007/s00402-022-04510-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-022-04510-5