Abstract
Introduction
Anticipation of patient-specific component sizes prior to total knee arthroplasty (TKA) is essential to avoid excessive cost associated with additional surgical trays and morbidity associated with imperfect sizing. Current methods of size prediction, including templating, are inconsistent and time-consuming. Machine learning (ML) algorithms may allow for accurate TKA component size prediction with the ability to make predictions in real-time.
Methods
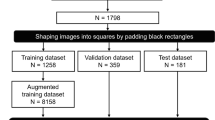
Consecutive patients receiving primary TKA between 2012 and 2020 from two large tertiary academic and six community hospitals were identified. The primary outcomes were the final femoral and tibial component sizes extracted from automated inventory systems. Five ML algorithms were trained with routinely corrected demographic variables (age, height, weight, body mass index, and sex) using 80% of the study population and internally validated on an independent set of the remaining 20% of patients. Algorithm performance was evaluated through accuracy, mean absolute error (MAE), and root mean-squared error (RMSE).
Results
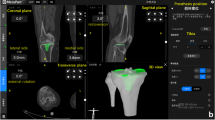
A total of 17,283 patients that received one of 9 TKA implants from independent manufacturers were included. The SGB model accuracy for predicting ± 4-mm of the true femoral anteroposterior diameter was 83.6% and for ± 1 size of the true femoral component size was 95.0%. The SGB model accuracy for predicting ± 4-mm of the true tibial medial/lateral diameter was 83.0% and for ± 1 size of the true tibial component size was 97.8%. Patient sex was the most influential feature in terms of informing the SGB model predictions for both femoral and tibial component sizing. A TKA implant sizing application was subsequently created.
Conclusion
Novel machine learning algorithms demonstrated good to excellent performance for predicting TKA component size. Patient sex appears to contribute an important role in predicting TKA size. A web-based real-time prediction application was created capable of integrating patient specific data to predict TKA size, which will require external validation prior to clinical use.






Similar content being viewed by others
References
Tang A, Yeroushalmi D, Zak S, Lygrisse K, Schwarzkopf R, Meftah M (2020) The effect of implant size difference on patient outcomes and failure after bilateral simultaneous total knee arthroplasty. J Orthop 22:282–287
Berend ME, Ritter MA, Hyldahl HC, Meding JB, Redelman R (2008) Implant migration and failure in total knee arthroplasty is related to body mass index and tibial component size. J Arthroplasty 23(6 Suppl 1):104–109
Chau R, Gulati A, Pandit H, Beard DJ, Price AJ, Dodd CA, Gill HS, Murray DW (2009) Tibial component overhang following unicompartmental knee replacement–does it matter? Knee 16(5):310–313
Marmor S, Renault E, Valluy J, Saffarini M (2019) Over-voluming predicted by pre-operative planning in 24% of total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 27(5):1544–1551
Gonzalez MH, Mekhail AO (2004) The failed total knee arthroplasty: evaluation and etiology. J Am Acad Orthop Surg 12(6):436–446
Trickett RW, Hodgson P, Forster MC, Robertson A (2009) The reliability and accuracy of digital templating in total knee replacement. J Bone Joint Surg Br 91(7):903–906
Boese CK, Wilhelm S, Haneder S, Lechler P, Eysel P, Bredow J (2019) Influence of calibration on digital templating of hip arthroplasty. Int Orthop 43(8):1799–1805
Sloan M, Premkumar A, Sheth NP (2018) Projected volume of primary total joint arthroplasty in the U.S., 2014 to 2030. J Bone Joint Surg Am 100(17):1455–1460
Polce EM, Kunze KN, Paul K, Levine BR (2021) Machine learning predicts femoral and tibial implant size mismatch for total knee arthroplasty. Arthroplast Today 8:268–277.e2. https://doi.org/10.1016/j.artd.2021.01.006
Bozic KJ, Kamath AF, Ong K, Lau E, Kurtz S, Chan V, Vail TP, Rubash H, Berry DJ (2015) Comparative epidemiology of revision arthroplasty: failed THA poses greater clinical and economic burdens than failed TKA. Clin Orthop Relat Res 473(6):2131–2138
Sershon RA, Courtney PM, Rosenthal BD, Sporer SM, Levine BR (2017) Can demographic variables accurately predict component sizing in primary total knee arthroplasty? J Arthroplasty 32(10):3004–3008
Sershon RA, Li J, Calkins TE, Courtney PM, Nam D, Gerlinger TL, Sporer SM, Levine BR (2019) Prospective validation of a demographically based primary total knee arthroplasty size calculator. J Arthroplasty 34(7):1369–1373
Bhowmik-Stoker M, Scholl L, Khlopas A, Sultan AA, Sodhi N, Moskal JT, Mont MA, Teeny SM (2018) Accurately predicting total knee component size without preoperative radiographs. Surg Technol Int 33:337–342
Collins GS, Reitsma JB, Altman DG, Moons KG (2015) Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. BMJ 350:g7594
Luo W, Phung D, Tran T, Gupta S, Rana S, Karmakar C, Shilton A, Yearwood J, Dimitrova N, Ho TB, Venkatesh S, Berk M (2016) Guidelines for developing and reporting machine learning predictive models in biomedical research: a multidisciplinary view. J Med Internet Res 18(12):323
Kunze KN, Polce EM, Nwachukwu BU, Chahla J, Nho SJ (2021) Development and internal validation of supervised machine learning algorithms for predicting clinically significant functional improvement in a mixed population of primary hip arthroscopy. Arthroscopy 37(5):1488–1497. https://doi.org/10.1016/j.arthro.2021.01.005
Kunze KN, Polce EM, Rasio J, Nho SJ (2020) Machine learning algorithms predict clinically significant improvements in satisfaction after hip arthroscopy. Arthroscopy 37(4):1143–1151. https://doi.org/10.1016/j.arthro.2020.11.027
Kunze KN, Burnett RA, Lee EK, Rasio JP, Nho SJ (2020) Development of machine learning algorithms to predict being lost to follow-up after hip arthroscopy for femoroacetabular impingement syndrome. Arthrosc Sports Med Rehabil 2(5):e591–e598
Polce EM, Kunze KN, Fu MC, Garrigues GE, Forsythe B, Nicholson GP, Cole BJ, Verma NN (2020) Development of supervised machine learning algorithms for prediction of satisfaction at 2 years following total shoulder arthroplasty. J Shoulder Elbow Surg 30(6):e290–e299. https://doi.org/10.1016/j.jse.2020.09.007
Kunze KN, Polce EM, Sadauskas AJ, Levine BR (2020) Development of machine learning algorithms to predict patient dissatisfaction after primary total knee arthroplasty. J Arthroplasty 35(11):3117–3122
Kunze KN, Karhade AV, Sadauskas AJ, Schwab JH, Levine BR (2020) Development of machine learning algorithms to predict clinically meaningful improvement for the patient-reported health state after total hip arthroplasty. J Arthroplasty 35(8):2119–2123
Kunze KN, Karhade AV, Sadauskas AJ, Schwab JH, Levine BR (2020) Development of machine learning algorithms to predict clinically meaningful improvement for the patient-reported health state after total hip arthroplasty. J Arthroplasty 35(8):2119–2123. https://doi.org/10.1016/j.arth.2020.03.019
Breiman L (2001) Random forests. Mach Learn 45(1):5–32
Hastie T, Tibshirani R, Friedman J (2009) The elements of statistical learning: data mining, inference, and prediction. Springer
Friedman JH (2002) Stochastic gradient boosting. Comput Stat Data Anal 38(4):367–378
Friedman JH (2001) Greedy function approximation: a gradient boosting machine. Ann Stat 29(5):1189–1232
Friedman J, Hastie T, Tibshirani R (2010) Regularization paths for generalized linear models via coordinate descent. J Stat Softw 33(1):1–22
Ribeiro MT, Singh S, Guestrin C (2016) "Why Should I Trust You?": explaining the predictions of any classifier. In: Proceedings of the 22nd SIGKDD international conference on knowledge discovery and data mining, pp 1135–1144
Miller AG, Purtill JJ (2012) Accuracy of digital templating in total knee arthroplasty. Am J Orthop (Belle Mead NJ) 41(11):510–512
Levine B, Fabi D, Deirmengian C (2010) Digital templating in primary total hip and knee arthroplasty. Orthopedics 33(11):797
Wongsak S, Kawinwonggowit V, Mulpruck P, Channoom T, Woratanarat P (2009) Accuracy of knee implants sizing predicted by digital images. J Med Assoc Thai 92(Suppl 6):S85-90
Jung WH, Seo JG, Kim DH, Balabadra S, Mandot U, Kumar D (2020) Optimal rotational positioning of tibial component in total knee arthroplasty: determined by linker surgical technique using a high definition CT. Arch Orthop Trauma Surg 140(3):401–408
Klasan A, Twiggs JG, Fritsch BA, Miles BP, Heyse TJ, Solomon M, Parker DA (2020) Correlation of tibial component size and rotation with outcomes after total knee arthroplasty. Arch Orthop Trauma Surg 140(11):1819–1824
Zahn RK, Graef F, Conrad JL, Renner L, Perka C, Hommel H (2020) Accuracy of tibial positioning in the frontal plane: a prospective study comparing conventional and innovative techniques in total knee arthroplasty. Arch Orthop Trauma Surg 140(6):793–800
Marino D, Patel J, Popovich JM Jr, Cochran J (2020) Patient demographics and anthropometric measurements predict tibial and femoral component sizing in total knee arthroplasty. Arthroplast Today 6(4):860–865
Wallace SJ, Murphy MP, Schiffman CJ, Hopkinson WJ, Brown NM (2020) Demographic data is more predictive of component size than digital radiographic templating in total knee arthroplasty. Knee Surg Relat Res 32(1):63
Funding
No funding was obtained for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
KNK, AP, EMP: no conflicts of interest. PMC: is a paid consultant for Depuy, Hip Innovation Technology, Zimmer; has stock or stock options in Parvizi Surgical Innovation; and is a Board Member or has a Committee Appointment at AAHKS. BRL: is a paid consultant for Link Orthopaedics, Merete, Exactech; receives research support from Zimmer, Artelon; receives royalties, financial or material support from Human Kinetics, Elsevier and SLACK Inc.; and is a Board Member or has a Committee Appointment at AAHKS, MAOA and the AAOS.
Ethical approval
This study was exempt from ethical approval.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kunze, K.N., Polce, E.M., Patel, A. et al. Validation and performance of a machine-learning derived prediction guide for total knee arthroplasty component sizing. Arch Orthop Trauma Surg 141, 2235–2244 (2021). https://doi.org/10.1007/s00402-021-04041-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-021-04041-5