Abstract
Introduction
At our hospital, an unusually high proportion of patients and families opted for conservative management of hip fractures. This study aimed to compare the mortality rates of patients with hip fractures treated conservatively to that of operatively managed patients in a dedicated hip fracture unit.
Materials and methods
Retrospective analysis was done for patients who were treated for hip fractures between January 2015 and October 2017 in a Hip Fracture Unit at a tertiary hospital. Patients were managed non-operatively or surgically after discussion with the multi-disciplinary team.
Results
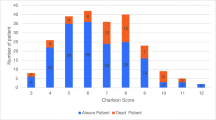
233 patients were treated conservatively and 781 underwent operative management for hip fractures. Patients managed non-operatively had a higher inpatient, 30-day and 1-year mortality rates. Inpatient mortality was 6.01% for conservatively managed compared to 0% for operative management. 30-day mortality for conservatively managed patients was 8.58% as compared to 0% for operatively managed patients, and 1-year mortality was 33.05% as opposed to 8.96%. There was an association seen with the type of management of hip fractures and that of inpatient death (p = 0.000), death in 30 days (p = 0.000) and death in 1 year (p = 0.000). The type of management was a predictive factor in 1-year mortality (p = 0.000). The average number of co-morbidities in conservatively managed patients was 5.2 compared to surgically managed patients of 4.0. Conservatively managed hip patients had a higher prevalence of stroke, chronic kidney disease and ischemic heart disease. Complications during hospital stay were comparable for both groups. The mean length of hospital stay was similar for both groups.
Conclusion
Surgical intervention for hip fractures is associated with lower inpatient, 30-day and 1-year mortality rates. However, patient co-morbidities and pre-morbid conditions should also be considered.
Level of evidence
IV.


Similar content being viewed by others
References
Haentjens P, Magaziner J, Colo ́n-Emeric CS, Vanderschueren D, Milisen K, Velkeniers B, Boonen S. (2010) Meta-analysis: excess mortality after hip fracture among older women and men. Ann Intern Med 152(6):380–390
Dahl E (1980) Mortality and life expectancy after hip fractures. Acta Orthop Scand 51:163–170
Ions GK, Stevens J (1987) Prediction of survival in patients with femoral neck fractures. J Bone Joint Surg 69-B:384–387
Riska EB (1970) Factors influencing the primary mortality in the treatment of hip fractures. Injury 2:107–115
Shafton G, Herbsman H, Pavlides C (1967) Selective conservatism in hip fractures. Surgery 61:524–527
Williams N, Hardy BM, Tarrant S et al (2013) Changes in hip fracture incidence, mortality and length of stay over the last decade in an Australian major trauma centre. Arch Osteoporos 8:150
Chia PH, Gualano L, Seevanayagam S, Weinberg L (2013) Outcomes following fractured neck of femur in an Australian metropolitan teaching hospital. Bone Joint Res 2:162–168
Beals RK (1972) Survival following hip fracture: long follow up of 607 patients. J Chronic Dis 25:235–244
Database NHF (2013) National hip fracture database national report 2013. Royal College of Physicians, London
Wood DJ, Ions GK, Quinby JM et al (1992) Factors which influence mortality after subcapital hip fracture. J Bone Joint Surg 74-B:199–202
Handoll HHG, Parker MJ (2008) Conservative versus operative treatment for hip fractures in adults. Cochrane Database Syst Rev 3:CD000337
Gdalevich M, Cohen D, Yosef D, Tauber C (2004) Morbidity and mortality after hip fracture: the impact of operative delay. Arch Orthop Trauma Surg 124(5):334–340
McGuire KJ, Bernstein J, Polsky D, Silber JH (2004) The 2004 Marshall Urist Award: delays until surgery after hip fracture increases mortality. Clin Orthop Relat Res 428:294–301
Bottle A, Aylin P (2006) Mortality associated with delay in operation after hip fracture: observational study. BMJ 332(7547):947–951
Weller I, Wai EK, Jaglal S, Kreder HJ (2005) The effect of hospital type and surgical delay on mortality after surgery for hip fracture. J Bone Joint Surg Br 87(3):361–366
Sheehan KJ, Sobolev B, Guy P (2017) Mortality by timing of hip fracture surgery: factors and relationships at play. J Bone Joint Surg Am 99(20):e106
Moulton LS, Green NL, Sudahar T, Makwana NK, Whittaker JP (2015) Outcome after conservatively managed intracapsular fractures of the femoral neck. Ann R Coll Surg Eng 97(4):279–282
Gregory JJ, Kostakopoulou K, Cool WP, Ford DJ (2010) One-year outcome for elderly patients with displaced intracapsular fractures of the femoral neck managed non-operatively. Injury 41(12):1273–1276
Holmberg S, Conradi P, Kalen R, Thorgren KG (1986) Mortality after cervical hip fracture. 3002 patients followed for 6 years. Acta Orthop Scand 57:8–11
Jensen JS, Tondevold E (1979) Mortality after hip fractures. Acta Orthop Scand 50:161–167
Levi N (1996) Early mortality after cervical hip fractures. Injury 8:565–567
White BL, Fisher WD, Laurin CA (1980s) Rate of mortality for elderly patients after fracture of the hip in the 1980s. J Bone Joint Surg [Am] 69:1335–1340
Acknowledgements
Ng Hui Min, for data collection. Dr Stephen Allen, for his assistance. DSRB approval has been obtained: 2015/00661. IRB approval has been obtained (Ref: 2015/00661)
Funding
The research study received no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that there is no conflict of interests to declare.
Human and animal participants rights
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tan, C., Park, D.H., Chen, Y. et al. Mortality rates for hip fracture patients managed surgically and conservatively in a dedicated unit in Singapore. Arch Orthop Trauma Surg 142, 99–104 (2022). https://doi.org/10.1007/s00402-020-03605-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-020-03605-1