Abstract
Introduction
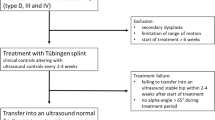
Early diagnosis and treatment of hip dysplasia are widely accepted as major factors for beneficial outcome. However, modalities for reduction and retention as well as for imaging are currently under clinical investigation. Local and general risk factors, e.g., breech presentation and the family’s desire to avoid in-hospital treatment are major concerns in the decision-making process and consultation. For treatment of unstable hips in newborns the treatment with the Tübingen splint has proven good results in recent studies. However, mid- and long-term outcome studies are missing. We report on clinical results and X-ray parameter of initially unstable hips after treatment with the Tübingen splint at two time points: 12–24 and 24–48 months of age.
Materials and Methods
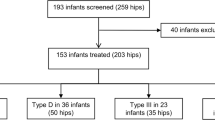
Included were newborns with 83 unstable hips (type D, III, IV according to Graf) which were successfully treated with the Tübingen splint—used as reduction splint 24 h per day/7 days per week—until type I hips were documented by ultrasound examination. Measurments are based on routine pelvic X-ray control at the age of 12–24 and 24–48 months. The acetabular angle was determined and according to the Tönnis-Classification evaluated into: normal findings (< 1 s), slightly dysplastic findings (1–2 s) and severely dysplastic findings (> 2 s). Children with secondary hip dysplasia were not included in this series.
Results
In 2nd year of life, 45 hips (54.2%; initial hip type D: 47.4%, III: 63.2%, IV: 42.9%) of the formerly unstable hips show normal X-ray findings. Although final ultrasound showed normal findings, at this time point 28 hips (33.7%; initial hip type D: 34.2%, III: 31.6%, IV: 42.9%) were slightly dysplastic and 10 (12.0%%; initial hip type D: 18.4%, III: 5.3%, IV: 14.3%) still severely dysplastic. At the age of 24–48 months, the percentage of radiologic normal hips had increased to 61 hips (73.5%; initial hip type D: 68.4%, III: 81.6%, IV: 57.1%), the number of slightly (19 hips) and severely dysplastic (3 hips) hips had decreased 22.9% (initial hip type D: 28.9%, III: 15.8%, IV: 28.6%) respectively 3.6% (initial hip type D: 2.6%, III: 2.6%, IV: 14.3%). At this time no operative intervention was neccessary.
Conclusions
Our mid-term data show on the one hand a good development of unstable hips after successful treatment with the Tübingen splint. On the other hand despite successful therapy and normal ultrasound findings at the end of treatment further imaging by X-ray are mandatory to close follow-up and to detect those which might need surgical correction of residual dysplasia.









Similar content being viewed by others
References
Farr S, Grill F, Müller D (2008) When is the optimal time for hip ultrasound screening?. Orthopade 37(6):532 (534–6, 538–540)
Grill F, Müller D (1997) Results of hip ultrasonographic screening in Austria. Orthopade 26(1):25–32
Graf R (2017) Hip sonography: background; technique and common mistakes; results; debate and politics; challenges. Hip Int J Clin Exp Res Hip Pathol Ther 27(3):215–219
Katthagen BD, Mittelmeier H, Becker D (1988) Incidence and start of inpatient treatment of pediatric hip dislocations in West Germany. Z Orthop Ihre Grenzgeb 126(5):475–483
Bernau A (1990) The Tübingen hip flexion splint in the treatment of hip dysplasia. Z Orthop Ihre Grenzgeb 128(4):432–435
Fettweis E (1968) Sit-crouch-position-plaster in hip joint dysplasies. Arch Orthop Unfallchir 63(1):38–51
Pavlik A (1957) Method of functional therapy with strap braces as a principle of conservative therapy of congenital dislocation of the hip in infants. Z Orthop Ihre Grenzgeb 89(3):341–352
Bensahel H, Csukonyi Z, Huguenin P (1988) Vascular disorders of the proximal femur following treatment of congenital hip dislocation. Arch Orthop Trauma Surg Arch Orthopadische Unf-Chir 107(6):372–376
van der Sluijs JA, De Gier L, Verbeke JI, Witbreuk MMEH., Pruys JEH, van Royen BJ (2009) Prolonged treatment with the Pavlik harness in infants with developmental dysplasia of the hip. J Bone Joint Surg Br 91(8):1090–1093
Walton MJ, Isaacson Z, McMillan D, Hawkes R, Atherton WG (2010) The success of management with the Pavlik harness for developmental dysplasia of the hip using a United Kingdom screening programme and ultrasound-guided supervision. J Bone Joint Surg Br 92(7):1013–1016
Seidl T, Lohmaier J, Hölker T, Funk J, Placzek R, Trouillier HH (2012) Reduction of unstable and dislocated hips applying the Tübingen hip flexion splint? Orthopade 41(3):195–199
Kubo H, Pilge H, Weimann-Stahlschmidt K, Stefanovska K, Westhoff B, Krauspe R (2017) Use of the Tübingen splint for the initial management of severely dysplastic and unstable hips in newborns with DDH: an alternative to Fettweis plaster and Pavlik harness. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-017-2827-3
Lehmann HP, Hinton R, Morello P, Santoli J (2000) Developmental dysplasia of the hip practice guideline: technical report. Committee on quality improvement, and subcommittee on developmental dysplasia of the hip. Pediatrics 105(4):E57
Starr V, Ha BY (2014) Imaging update on developmental dysplasia of the hip with the role of MRI. AJR Am J Roentgenol 203(6):1324–1335
Schrading S, Schulze A (2016) Preoperative diagnostic imaging and planning. Orthopade 45(8):644–652
Tönnis D (1997) Röntgenuntersuchung und arthrographie des Hüftgelenks im Kleinkindesalter. Orthopade 26(1):49–58
Sochart DH, Paton RW (1996) Role of ultrasound assessment and harness treatment in the management of developmental dysplasia of the hip. Ann R Coll Surg Engl 78(6):505–508
Allington NJ (2015) Successful Pavlik Harness Treatment for Developmental Dysplasia of the Hip and Normal X-Ray at the Age of 2 Years: Is a Longer Follow-up Necessary? J Pediatr Orthop 37(5):328–331
Bian Z, Guo Y, Tian W (2009) Treatment of developmental dysplasia of the hip in children: results of closed reduction and immobilization in hip spica cast. Zhonghua Wai Ke Za Zhi 47(13):1017–1019
Kotlarsky P, Haber R, Bialik V, Eidelman M (2015) Developmental dysplasia of the hip: What has changed in the last 20 years? World J Orthop 6(11):886–901
Sarkissian EJ, Sankar WN, Zhu X, Wu CH, Flynn JM (2015) Radiographic follow-up of DDH in infants: are X-rays necessary after a normalized ultrasound? J Pediatr Orthop 35(6):551–555
Alexiev VA, Harcke HT, Kumar SJ (2006) Residual dysplasia after successful Pavlik harness treatment: early ultrasound predictors. J Pediatr Orthop 26(1):16–23
Tucci JJ, Kumar SJ, Guille JT, Rubbo ER (1991) Late acetabular dysplasia following early successful Pavlik harness treatment of congenital dislocation of the hip. J Pediatr Orthop 11(4):502–505
Miao M, Cai H, Hu L, Wang Z (2017) Retrospective observational study comparing the international hip dysplasia institute classification with the Tonnis classification of developmental dysplasia of the hip. Medicine (Baltimore) 96(3):e5902
Modaressi K, Erschbamer M, Exner GU (2011) Dysplasia of the hip in adolescent patients successfully treated for developmental dysplasia of the hip. J Child Orthop 5(4):261–266
Cashman JP, Round J, Taylor G, Clarke NMP (2002) The natural history of developmental dysplasia of the hip after early supervised treatment in the Pavlik harness. A prospective, longitudinal follow-up. J Bone Jt Surg Br 84(3):418–425
Dornacher D, Cakir B, Reichel H, Nelitz M (2010) Early radiological outcome of ultrasound monitoring in infants with developmental dysplasia of the hips. J Pediatr Orthop Part B 19(1):27–31
Demirhan M, Dikici F, Eralp L, Onen M, Göksan B (2002) A treatment algorithm for developmental dysplasia of the hip for infants 0 to 18 months of age and its prospective results. Acta Orthop Traumatol Turc 36(1):42–51
Funding
No funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All Authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards (Ethics committee vote of the University of Dusseldorf, study no. 4949).
Rights and permissions
About this article
Cite this article
Kubo, H., Pilge, H., Nepp, K. et al. Development of unstable hips after treatment with the Tübingen splint: mid-term follow-up of 83 hip joints. Arch Orthop Trauma Surg 138, 629–634 (2018). https://doi.org/10.1007/s00402-018-2882-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-018-2882-4