Abstract
Introduction
Osteochondral lesion of the talus (OCT) frequently accompanies chronic lateral ankle instability (CLAI). However, it remains unclear whether concomitant OCT and CLAI should be treated surgically at the same time. The purpose was to evaluate the clinical outcome of simultaneous surgery involving stabilization of CLAI and retrograde drilling for only subchondral bone lesion of the talus.
Study design
The study was a case series; level of evidence, 4.
Materials and methods
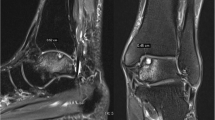
Between January 2006 and February 2010, 16 feet of 16 patients (5 men, 11 women; mean age 25 years; age range 14–49 years) with CLAI accompanied by only subchondral bone lesion of talus underwent surgical repair or reconstruction of the anterior talofibular ligament and retrograde drilling. Subchondral bone lesion of talus was diagnosed by preoperative magnetic resonance imaging (MRI) and intraoperative arthroscopic investigation. Clinical outcome was measured using the American Orthopedic Foot and Ankle Society Ankle-Hindfoot Scale (AOFAS) and a visual analog scale (VAS). Improvement in lesion area was evaluated by assessing the change between preoperative and postoperative MRI findings.
Results
Preoperative to postoperative changes in all patients were as follows: mean AOFAS score improved from 73.4 points (range 62–87) to 91.2 points (range 85–100) (p < 0.001); mean VAS score improved from 55.0 points (range 40–80) to 6.5 points (range 0–20) (p < 0.001); and mean lesion area improved from 33.9 mm2 (range 14.2–59.6) to 11.8 mm2 (range 4.3–22.1) (p < 0.001).
Conclusions
Simultaneous surgery involving lateral ankle stabilization and retrograde drilling under arthroscopic and fluoroscopic guidance is a promising method for treating CLAI accompanied by only subchondral bone lesion of talus.





Similar content being viewed by others
References
Maffulli N, Ferran NA (2008) Management of acute and chronic ankle instability. J Am Acad Orthop Surg 16:608–615
Takao M, Oae K, Uchio Y, Ochi M, Yamamoto H (2005) Anatomical reconstruction of the lateral ligaments of the ankle with a gracilis tendon. A new technique using an interference fit anchoring system. Am J Sports Med 33:814–823
Eyring EJ, Guthrie WD (1986) A surgical approach to the problem of severe lateral instability at the ankle. Clin Orthop Relat Res 206:185–191
Karlsson J, Bergsten T, Lansinger O, Peterson L (1988) Reconstruction of the lateral ligaments of the ankle for chronic lateral instability. J Bone Joint Surg Am 70:581–588
Rechtine GR, McCarroll JR, Webster DA (1982) Reconstruction for chronic lateral instability of the ankle: a review of 28 surgical patients. Orthopaedics 5:44–50
Sammarco GJ, DiRaimondo CV (1988) Surgical treatment of lateral ankle instability syndrome. Am J Sports Med 16:501–511
Taga I, Shino K, Inoue M, Nakata K, Maeda A (1993) Articular cartilage lesions in ankles with lateral ligament injury: an arthroscopic study. Am J Sports Med 21:120–127
DiGiovanni BF, Frage CJ, Cohen BE, Shereff MJ (2000) Associated injuries found in chronic lateral ankle instability. Foot Ankle Int 21:809–815
Hintermann B, Boss A, Schäfer D (2002) Arthroscopic findings in patients with chronic ankle instability. Am J Sports Med 30:402–409
Komenda AG, Ferkel RD (1999) Arthroscopic findings associated with the unstable ankle. Foot Ankle Int 20:708–713
Okuda R, Kinoshita M, Morikawa J, Yasuda T, Abe M (2005) Arthroscopic findings in chronic lateral ankle instability: do focal chondral lesions influence the results of ligament reconstruction? Am J Sports Med 33:35–42
Takao M, Uchio Y, Naito K, Fukazawa I, Ochi M (2005) Arthroscopic assessment for intra-articular disorders in residual ankle disability after sprain. Am J Sports Med 33:686–692
Choi WJ, Lee JW, Han SH, Kim BS, Lee SK (2008) Chronic lateral ankle instability: the effect of intra-articular lesions on clinical outcome. Am J Sports Med 36:2167–2172
Gregush RV, Ferkel RD (2010) Treatment of the unstable ankle with an osteochondral lesion: results and long-term follow-up. Am J Sports Med 38:782–790
Nelson DW, DiPaola J, Colville M, Schmidgall J (1990) Osteochondritis dissecans of the talus and knee: prospective comparison of MR and arthroscopic classification. J Comput Assist Tomogr 14:804–808
Karlsson J, Lansinger O (1992) Lateral instability of the ankle joint. Clin Orthop Relat Res 276:253–261
Cox JS, Hewes TF (1979) “Normal” talar tilt angle. Clin Orthop Relat Res 140:37–41
Grace DL (1984) Lateral ankle ligament injuries. Inversion and anterior stress radiography. Clin Orthop Relat Res 183:153–159
Pritsch M, Horoshovski H, Farine I (1986) Arthroscopic treatment of osteochondral lesions of the talus. J Bone Joint Surg Am 85:989–993
Takao M, Ochi M, Naito K, Uchio Y, Kono T, Oae K (2003) Arthroscopic drilling for chondral, subchondral, and combined chondral–subchondral lesions of the talar dome. Arthroscopy 19:524–530
Kitaoka HB, Alexander IJ, Adelaar RS, Nunley JA, Myerson MS, Sanders M (1994) Clinical rating systems for the ankle-hindfoot, midfoot, hallux, and lesser toes. Foot Ankle Int 15:349–353
Choi WJ, Park KK, Kim BS, Lee JW (2009) Osteochondral lesion of the talus: is there a critical defect size for poor outcome? Am J Sports Med 37:1974–1980
Takao M, Uchio Y, Kakimaru H, Kumahashi N, Ochi M (2004) Arthroscopic drilling with debridement of remaining cartilage for osteochondral lesions of the talar dome in unstable ankles. Am J Sports Med 32:332–336
Easley ME, Latt LD, Santangelo JR, Merian-Genast M, Nunley JA 2nd (2010) Osteochondral lesions of the talus. J Am Acad Orthop Surg 18:616–630
O’Loughlin PF, Heyworth BE, Kennedy JG (2010) Current concepts in the diagnosis and treatment of osteochondral lesions of the ankle. Am J Sports Med 38:392–404
Lee CK, Mercurio C (1981) Operative treatment of osteochondritis dissecans in situ by retrograde drilling and cancellous bone graft: a preliminary report. Clin Orthop Relat Res 158:129–136
Anders S, Lechler P, Rackl W, Grifka J, Schaumburger J (2012) Fluoroscopy-guided retrograde core drilling and cancellous bone grafting in osteochondral defects of the talus. Int Orthop 36:1635–1640
Geerling J, Zech S, Kendoff D, Citak M, O’Loughlin PF, Hüfner T, Krettek C, Richter M (2009) Initial outcomes of 3-dimensional imaging-based computer-assisted retrograde drilling of talar osteochondral lesions. Am J Sports Med 37:1351–1357
Kono M, Takao M, Naito K, Uchio Y, Ochi M (2006) Retrograde drilling for osteochondral lesions of the talar dome. Am J Sports Med 34:1450–1456
Taranow WS, Bisignani GA, Towers JD, Conti SF (1999) Retrograde drilling of osteochondral lesions of the medial talar dome. Foot Ankle Int 20:474–480
Gras F, Marintschev I, Müller M, Klos K, Lindner R, Mückley T, Hofmann GO (2010) Arthroscopic-controlled navigation for retrograde drilling of osteochondral lesions of the talus. Foot Ankle Int 31:897–904
Hoffmann M, Petersen JP, Schröder M, Spiro AS, Kammal M, Rueger JM, Ruecker AH (2012) Retrograde drilling of talar osteochondritis dissecans lesions: a feasibility and accuracy analysis of a novel electromagnetic navigation method versus a standard fluoroscopic method. Arthroscopy 28:1547–1554
Kennedy JG, Suero EM, O’Loughlin PF, Brief A, Bohne WH (2008) Clinical tips: retrograde drilling of talar osteochondral defects. Foot Ankle Int 29:616–619
O’Loughlin PF, Kendoff D, Pearle AD, Kennedy JG (2009) Arthroscopic-assisted fluoroscopic navigation for retrograde drilling of a talar osteochondral lesion. Foot Ankle Int 30:70–73
Seebauer CJ, Bail HJ, Wichlas F, Jung T, Papanikolaou IS, van der Voort I, Rump JC, Schilling R, Winkelmann A, Walther T, Chopra SS, Teichgräber UK (2009) Osteochondral lesions of the talus: retrograde drilling with high-field-strength MR guidance. Radiology 252:857–864
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yasui, Y., Takao, M., Miyamoto, W. et al. Simultaneous surgery for chronic lateral ankle instability accompanied by only subchondral bone lesion of talus. Arch Orthop Trauma Surg 134, 821–827 (2014). https://doi.org/10.1007/s00402-014-1969-9
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-014-1969-9