Abstract
Introduction
Early results have indicated that the Bryan cervical total disc replacement (TDR) favorably compares to anterior cervical decompression and fusion, while it is associated with fewer complications and higher levels of satisfaction. In this study, we sought to prospectively report the midterm outcomes of the Bryan TDR.
Patients and methods
A total of 20 patients had performed their 4-year follow-up visit and had been assessed clinically and radiologically. Clinical outcomes (JOA, VAS, NDI, SF-36) and ROM measurements were investigated preoperatively and at 1 and 6 months, and 1, 2 and 4 years after operation. Complications were also investigated. Occurrences of heterotopic ossifications (HOs) and adjacent-level degeneration (ALD) radiographic changes were detected from 4-year follow-up X-rays.
Results
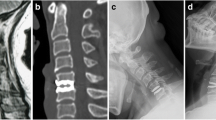
The mean JOA score, VAS score for arm and neck, NDI score and SF-36 score for PCS and MCS were reduced significantly at each postoperative time point when compared with the preoperative condition. The range of movement of the cervical spine, functional spinal unit, treated segment and the adjacent segment temporarily decreased at the early assessment, but all recovered to preoperative levels over a 6-month to 4-year time period. HO was evident in 6 of the 23 operated segments, which did not restrict the movement of the prosthesis. No obvious ALD was found on MRI. There were no cases of prosthesis migration, subsidence, loosening or wear.
Conclusion
The midterm outcomes demonstrated that the Bryan TDR maintains favorable clinical and radiological results, with preservation of movement and satisfactory clinical outcome. There were no serious complications or cases of prosthetic wear or failure. The long-term benefits are yet to be examined.





Similar content being viewed by others
References
Pitzen T (2012) Overview of surgical techniques and implants. Man Spine Surg 3:117–125
Brunon J (2009) Management of degenerative disease of the cervical spine. Pract Handb Neurosurg 7:1161–1176
Stieber JR, Brown K, Donald JD (2005) Anterior cervical decompression and fusion with plate fixation as an outpatient procedure. Spine J 5:503–507
Suen TK, Wong KH, Ho YF (2011) The outcomes of anterior spinal fusion for cervical compressive myelopathy: a retrospective review. J Orthop Trauma Rehabil 2:53–56
Ingrid Z, Roman W, Philipp M (2011) Artificial total disc replacement versus fusion for the cervical spine: a systematic review. Eur Spine J 20:177–184
Galbusera F, Bellini CM, Brayda-Bruno M (2008) Biomechanical studies on cervical total disc arthroplasty: a literature review. Clin Biomech 23:1095–1104
Sasso RC, Smucker JD, Hacker RJ (2007) Artificial disc versus fusion: a prospective, randomized study with 2-year follow-up on 99 patients. Spine 26:2933–2940
Wang QM, Cheng HB, Mao ZX (2011) Clinical and radiographic results after treatment of cervical degenerative disc disease with the Bryan disc prosthesis: a prospective study with 2-year follow-up. Acta Orthop Belg 77:809–815
Anderson PA, Rouleau JP (2004) Intervertebral disc arthroplasty. Spine 29:2779–2786
Baaj AA, Uribe JS, Vale FL (2009) History of cervical disc arthroplasty. Neurosurg Focus 3:10–16
Yang YC, Nie L, Cheng L (2009) Clinical and radiographic reports following cervical arthroplasty: a 24-month follow-up. Int Orthop 33:1037–1042
Nabhan A, Ishak B, Steudel WI (2011) Assessment of adjacent-segment mobility after cervical disc replacement versus fusion: RCT with 1 year’s results. Eur Spine J 6:934–941
Sasso RC, Best NM (2008) Cervical kinematics after fusion and Bryan disc arthroplasty. J Spinal Disord Tech 1:19–22
Shim CS, Lee SH, Park HJ et al (2006) Early clinical and radiologic outcomes of cervical arthroplasty with Bryan cervical disc prosthesis. J Spinal Disord Tech 7:465–470
Coric D, Finger F, Boltes P (2006) Prospective randomized controlled study of the Bryan cervical disc: early clinical results from a single investigational site. J Neurosurg Spine 4:31–35
Xu JX, Zhang YZ, Shen Y et al (2009) Effect of modified techniques in Bryan cervical disc arthroplasty. Spine 10:1012–1017
Kim SW, Shin JH, Arbatin JJ (2008) Effects of a cervical disc prosthesis on maintaining sagittal alignment of the functional spinal unit and overall sagittal balance of the cervical spine. Eur Spine J 17:20–29
McAfee PC, Cunningham BW, Devine J et al (2003) Classification of heterotopic ossification (HO) in artificial disk replacement. J Spinal Disord Tech 16:384–389
Sekhon LH, Sears W, Duggal N (2005) Cervical arthroplasty after previous surgery: results of treating 24 discs in 15 patients. J Neurosurg Spine 3:335–341
Sasso RC, Anderson PA, Riew KD (2011) Results of cervical arthroplasty compared with anterior discectomy and fusion: four-year clinical outcomes in a prospective, randomized controlled trial. J Bone Joint Surg Am 93:1684–1692
Chen J, Wang X, Bai WS (2012) Prevalence of heterotopic ossification after cervical total disc arthroplasty: a meta-analysis. Eur Spine J 21:674–680
Janssen M, Goldstein J, Murrey D (2007) Heterotopic ossification at the index level after Prodisc-C: what is the clinical significance? Spine J 7:48–49
Suchomel P (2010) Clinical results and development of heterotopic ossification in total cervical disc replacement during a 4-year follow-up. Eur Spine J 19:307–315
Quan GMY, Vital JM, Hansen S (2011) Eight-year clinical and radiological follow-up of the Bryan cervical disc arthroplasty. Spine 8:639–646
Shehab D, Elgazzar AH, Collier BD (2002) Heterotopic ossification. J Nucl Med 43:346–353
Conflict of interest
There is no perceived or otherwise conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
Zhenxiang Zhang and Beibei Gu are co-first authors.
Rights and permissions
About this article
Cite this article
Zhang, Z., Gu, B., Zhu, W. et al. Clinical and radiographic results of Bryan cervical total disc replacement: 4-year outcomes in a prospective study. Arch Orthop Trauma Surg 133, 1061–1066 (2013). https://doi.org/10.1007/s00402-013-1772-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-013-1772-z