Abstract
Purpose
Arthroscopic microfracture (AM) of osteochondral lesions of the talus is used to induce intrinsic refilling of the defect and reduce pain. The aim of this retrospective study was to investigate the clinical state after AM and the MRI outcome.
Methods
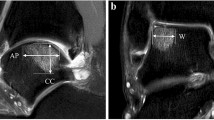
A total of 22 patients [10 women, 12 men, 31 years old (mean, 13–68 range)] treated for osteochondral lesions of the talus by AM were examined 2 years (median) postoperatively and pre- and postoperative MRI results compared. Swelling/effusion, articular constriction, joint pain, and range of motion restriction were documented. Clinical state was evaluated using the AOFAS hindfoot score. MRI was used to assess the size of the defect, presence of bone marrow edema, cysts and effusion, thickness of repair tissue, and integrity of the cartilage.
Results
In all but six cases, the defect was located at the medial shoulder of the talus. The postoperative AOFAS score at follow-up was 87.5 points (median 36–100 points range). Seven patients were free of pain, 11 had “mild, occasional” pain, 1 “moderate daily”, and 3 “severe, almost always present” pain (AOFAS). The defect volume was significantly reduced from 377 mm3 preoperatively (median, interquartile distance: 417 mm3) to 249 mm3 postoperatively (median, IQD: 336 mm3, p = 0.019, Wilcoxon). In 7 cases, the defect was completely filled, in 11 partially and in 4 only slightly.
Conclusion
After AM of osteochondral lesions of the talus, 18 of 22 patients had no or mild, occasional pain at 2 years follow-up. On MRI, the lesion volume had been reduced and filling with repair tissue was found.



Similar content being viewed by others
References
McGahan PJ, Pinney SJ (2010) Current concept review: osteochondral lesions of the talus. Foot Ankle Int 31(1):90–101. doi:10.3113/FAI.2010.0090
Kappis M (1922) Weitere Beiträge zur traumatisch-mechanischen Entstehung der spontanen Knorpelablösung (sogen. osteochondritis dissecans). Dtsch Z Chir 171:13–29
Berndt AL, Harty M (1959) Transchondral fractures (osteochondritis dissecans) of the talus. J Bone Joint Surg Am 41(A):988–1020
Bruns J, Behrens P (1998) Osteochondrosis dissecans. Ätiologische und pathophysiologische Aspekte. Arthroskopie 11:166–176
Steinhagen J, Niggemeyer O, Bruns J (2001) Etiology and pathogenesis of osteochondrosis dissecans tali. Orthopade 30(1):20–27
Stroud CC, Marks RM (2000) Imaging of osteochondral lesions of the talus. Foot Ankle Clin 5(1):119–133
van Bergen CJ, de Leeuw PA, van Dijk CN (2008) Treatment of osteochondral defects of the talus. Rev Chir Orthop Reparatrice Appar Mot 94(8):398–408. doi:10.1016/j.rco.2008.09.003
Loomer R, Fisher C, Lloyd-Smith R, Sisler J, Cooney T (1993) Osteochondral lesions of the talus. Am J Sports Med 21(1):13–19
Meftah M, Katchis SD, Scharf SC, Mintz DN, Klein DA, Weiner LS (2011) SPECT/CT in the management of osteochondral lesions of the talus. Foot Ankle Int 32(3):233–238. doi:10.3113/FAI.2011.0233
Ferkel RD, Zanotti RM, Komenda GA, Sgaglione NA, Cheng MS, Applegate GR, Dopirak RM (2008) Arthroscopic treatment of chronic osteochondral lesions of the talus: long-term results. Am J Sports Med 36(9):1750–1762. doi:10.1177/0363546508316773
Schuman L, Struijs PA, van Dijk CN (2002) Arthroscopic treatment for osteochondral defects of the talus. Results at follow-up at 2 to 11 years. J Bone Joint Surg Br 84(3):364–368
Steadman JR, Rodkey WG, Singleton SB, Briggs KK (1997) Microfracture technique for full-thickness chondral defects: technique and clinical results. Oper Techn Orthop 7:300–304
Niemeyer P, Salzmann G, Schmal H, Mayr H, Sudkamp NP (2011) Autologous chondrocyte implantation for the treatment of chondral and osteochondral defects of the talus: a meta-analysis of available evidence. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-011-1729-0
Giannini S, Battaglia M, Buda R, Cavallo M, Ruffilli A, Vannini F (2009) Surgical treatment of osteochondral lesions of the talus by open-field autologous chondrocyte implantation: a 10 year follow-up clinical and magnetic resonance imaging T2-mapping evaluation. Am J Sports Med 37(1):112S–118S. doi:10.1177/0363546509349928
Wiewiorski M, Leumann A, Buettner O, Pagenstert G, Horisberger M, Valderrabano V (2011) Autologous matrix-induced chondrogenesis aided reconstruction of a large focal osteochondral lesion of the talus. Arch Orthop Trauma Surg 131(3):293–296. doi:10.1007/s00402-010-1048-9
Baltzer AW, Arnold JP (2005) Bone-cartilage transplantation from the ipsilateral knee for chondral lesions of the talus. Arthroscopy 21(2):159–166. doi:10.1016/j.arthro.2004.10.021
Gobbi A, Francisco RA, Lubowitz JH, Allegra F, Canata G (2006) Osteochondral lesions of the talus: randomized controlled trial comparing chondroplasty, microfracture, and osteochondral autograft transplantation. Arthroscopy 22(10):1085–1092. doi:10.1016/j.arthro.2006.05.016
Becher C, Thermann H (2005) Results of microfracture in the treatment of articular cartilage defects of the talus. Foot Ankle Int 26(8):583–589. doi:894977
Becher C, Driessen A, Thermann H (2008) Microfracture technique for the treatment of articular cartilage lesions of the talus. Orthopade 37(3):196, 198–203. doi:10.1007/s00132-008-1213-9
Lee KB, Bai LB, Chung JY, Seon JK (2010) Arthroscopic microfracture for osteochondral lesions of the talus. Knee Surg Sports Traumatol Arthrosc 18(2):247–253. doi:10.1007/s00167-009-0914-x
Chuckpaiwong B, Berkson EM, Theodore GH (2008) Microfracture for osteochondral lesions of the ankle: outcome analysis and outcome predictors of 105 cases. Arthroscopy 24(1):106–112. doi:10.1016/j.arthro.2007.07.022
Doral MN, Bilge O, Batmaz G, Donmez G, Turhan E, Demirel M, Atay OA, Uzumcugil A, Atesok K, Kaya D (2011) Treatment of osteochondral lesions of the talus with microfracture technique and postoperative hyaluronan injection. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-011-1856-7
Becher C, Driessen A, Hess T, Longo UG, Maffulli N, Thermann H (2010) Microfracture for chondral defects of the talus: maintenance of early results at midterm follow-up. Knee Surg Sports Traumatol Arthrosc 18(5):656–663. doi:10.1007/s00167-009-1036-1
Marlovits S, Striessnig G, Resinger CT, Aldrian SM, Vecsei V, Imhof H, Trattnig S (2004) Definition of pertinent parameters for the evaluation of articular cartilage repair tissue with high-resolution magnetic resonance imaging. Eur J Radiol 52(3):310–319. doi:10.1016/j.ejrad.2004.03.014
Potter HG, Foo LF (2006) Magnetic resonance imaging of articular cartilage: trauma, degeneration, and repair. Am J Sports Med 34(4):661–677. doi:10.1177/0363546505281938
Schneider T, Fink B, Jerosch J, Assheuer J, Ruther W (1998) The value of magnetic resonance imaging as postoperative control after arthroscopic treatment of osteochondritis dissecans. Arch Orthop Trauma Surg 117(4–5):235–239
Apprich S, Trattnig S, Welsch GH, Noebauer-Huhmann IM, Sokolwski M, Hirschfeld C, Stelzeneder D, Domayer S (2012) Assessment of articular cartilage repair tissue after matrix-associated autologous chondrocyte transplantation or the microfracture technique in the ankle joint using diffusion-weighted imaging at 3 Tesla. Osteoarthr Cartil. doi:10.1016/j.joca.2012.03.008
Domayer SE, Apprich S, Stelzeneder D, Hirschfeld C, Sokolowski M, Kronnerwetter C, Chiari C, Windhager R, Trattnig S (2012) Cartilage repair of the ankle: first results of T2 mapping at 7.0 T after microfracture and matrix associated autologous cartilage transplantation. Osteoarthr Cartil. doi:10.1016/j.joca.2012.04.015
Kreuz PC, Steinwachs MR, Erggelet C, Krause SJ, Konrad G, Uhl M, Sudkamp N (2006) Results after microfracture of full-thickness chondral defects in different compartments in the knee. Osteoarthr Cartil 14(11):1119–1125. doi:10.1016/j.joca.2006.05.003
Mithoefer K, Williams RJ, 3rd, Warren RF, Potter HG, Spock CR, Jones EC, Wickiewicz TL, Marx RG (2005) The microfracture technique for the treatment of articular cartilage lesions in the knee. A prospective cohort study. J Bone Joint Surg Am 87(9):1911–1920. doi:10.2106/JBJS.D.02846
Cuttica DJ, Shockley JA, Hyer CF, Berlet GC (2011) Correlation of MRI edema and clinical outcomes following microfracture of osteochondral lesions of the talus. Foot Ankle Spec 4(5):274–279. doi:10.1177/1938640011411082
Guo QW, Hu YL, Jiao C, Yu CL, Ao YF (2010) Arthroscopic treatment for osteochondral lesions of the talus: analysis of outcome predictors. Chin Med J (Engl) 123(3):296–300
Giannini S, Vannini F (2004) Operative treatment of osteochondral lesions of the talar dome: current concepts review. Foot Ankle Int 25(3):168–175. doi:594999
Lahm A, Erggelet C, Steinwachs M, Reichelt A (2000) Arthroscopic management of osteochondral lesions of the talus: results of drilling and usefulness of magnetic resonance imaging before and after treatment. Arthroscopy 16(3):299–304. doi:S0749806300535968
Ettl V, Kenn W, Radke S, Kirschner S, Goerttler-Krauspe I, Vispo-Seara JL (2001) The role of MRI in therapy and follow-up after surgical treatment of osteochondrosis dissecans of the talus. Z Orthop Ihre Grenzgeb 139(2):157–162. doi:10.1055/s-2001-15049
Jurgensen I, Bachmann G, Schleicher I, Haas H (2002) Arthroscopic versus conservative treatment of osteochondritis dissecans of the knee: value of magnetic resonance imaging in therapy planning and follow-up. Arthroscopy 18(4):378–386. doi:S0749806302445021
Higashiyama I, Kumai T, Takakura Y, Tamail S (2000) Follow-up study of MRI for osteochondral lesion of the talus. Foot Ankle Int 21(2):127–133
Acknowledgement
The authors would like to thank Sherryl Sundell for English grammar revision.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kuni, B., Schmitt, H., Chloridis, D. et al. Clinical and MRI results after microfracture of osteochondral lesions of the talus. Arch Orthop Trauma Surg 132, 1765–1771 (2012). https://doi.org/10.1007/s00402-012-1595-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-012-1595-3