Abstract
Background
Sudden cardiac death (SCD) is one of the main causes of cardiovascular mortality and accounts for 15–20% of deaths worldwide. The current stratification strategy using depressed left ventricular ejection fraction is insufficient to stratify the risk of SCD, especially in the general population. In recent years, there has been increasing evidence showing the antiarrhythmic properties of magnesium. In this systematic review, the authors aim to determine circulating magnesium as a potential risk stratification tool for SCD.
Methods
This systematic review was based on Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) and was conducted in July 2021 with sources from Google Scholar, PubMed, Science Direct, EBSCO Medline, and ProQuest.
Results
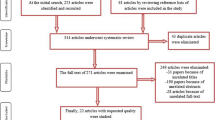
A total of six studies were included in this review. Three studies conducted in the general population consistently showed lower risk of SCD in populations with high circulating magnesium. There was no association between circulating magnesium level and risk of SCD in intensive cardiac care unit (ICCU) patients, whilst the results were conflicting in congestive heart failure (CHF) patients.
Conclusion
High circulating magnesium might have the potential to be utilized as a risk stratification tool for SCD, especially in the general population. However, further study is needed to support this evidence.
Zusammenfassung
Hintergrund
Der plötzliche Herztod („sudden cardiac death“ [SCD]) ist eine der Hauptursachen für die kardiovaskuläre Mortalität und verantwortlich für 15–20 % der Todesfälle weltweit. Die derzeitige Stratifizierungsstrategie unter Verwendung einer reduzierten linksventrikulären Ejektionsfraktion reicht nicht aus, um das SCD-Risiko adäquat zu stratifizieren, besonders nicht in der Allgemeinbevölkerung. In den letzten Jahren wurden zunehmend Hinweise auf die antiarrhythmischen Eigenschaften von Magnesium gefunden. In der vorliegenden systematischen Übersicht untersuchen wir, ob zirkulierendes Magnesium ein potenzieller Parameter zur SCD-Risikostratifizierung ist.
Methoden
Diese systematische Übersicht basiert auf den Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) und wurde im Juli 2021 mit Quellen von Google Scholar, PubMed, Science Direct, EBSCO MEDLINE und ProQuest durchgeführt.
Ergebnisse
Insgesamt wurden 6 Studien in diese Übersichtsarbeit eingeschlossen. Drei in der Allgemeinbevölkerung durchgeführte Studien zeigten durchweg ein geringeres SCD-Risiko in Populationen mit hohem zirkulierendem Magnesium. Es gab keinen Zusammenhang zwischen dem Spiegel von zirkulierendem Magnesium und dem SCD-Risiko bei Patienten auf kardiologischen Intensivstationen. Die Ergebnisse bei Patienten mit Herzinsuffizienz („congestive heart failure“ [CHF]) waren widersprüchlich.
Schlussfolgerung
Ein hoher Spiegel von zirkulierendem Magnesium könnte ein potenzieller Parameter zur SCD-Risikostratifizierung sein, insbesondere in der Allgemeinbevölkerung. Es sind jedoch weitere Studien erforderlich, um dies zu belegen.

Similar content being viewed by others
References
Mozaffarian D, Benjamin E, Go A, Arnett D, Blaha M, Cushman M et al (2015) Heart disease and stroke statistics—2015 update. Circulation. https://doi.org/10.1161/cir.0000000000000152
Hayashi M, Shimizu W, Albert C (2015) The spectrum of epidemiology underlying sudden cardiac death. Circ Res 116(12):1887–1906. https://doi.org/10.1161/circresaha.116.304521
Wong C, Brown A, Lau D, Chugh S, Albert C, Kalman J et al (2019) Epidemiology of sudden cardiac death: global and regional perspectives. Heart Lung Circ 28(1):6–14. https://doi.org/10.1016/j.hlc.2018.08.026
Adabag AS, Luepker RV, Roger VL, Gersh BJ (2010) Sudden cardiac death: epidemiology and risk factors. Nat Rev Cardiol 7(4):216–225. https://doi.org/10.1038/nrcardio.2010.3
Huikuri H (2011) Prediction and prevention of sudden cardiac arrest. CMAJ 183(15):1692–1693. https://doi.org/10.1503/cmaj.111245
Fishman G, Chugh S, DiMarco J, Albert C, Anderson M, Bonow R et al (2010) Sudden cardiac death prediction and prevention. Circulation 122(22):2335–2348. https://doi.org/10.1161/CIRCULATIONAHA.110.976092
Fiorentini D, Cappadone C, Farruggia G, Prata C (2021) Magnesium: biochemistry, nutrition, detection, and social impact of diseases linked to its deficiency. Nutrients 13(4):1136. https://doi.org/10.3390/nu13041136
Jahnen-Dechent W, Ketteler M (2012) Magnesium basics. Clin Kidney J 5(1):i3–i14. https://doi.org/10.1093/ndtplus/sfr163
DiNicolantonio J, Liu J, O’Keefe J (2018) Magnesium for the prevention and treatment of cardiovascular disease. Open Heart 5(2):e775. https://doi.org/10.1136/openhrt-2018-000775
Tangvoraphonkchai K, Davenport A (2018) Magnesium and cardiovascular disease. Adv Chronic Kidney Dis 25(3):251–260. https://doi.org/10.1053/j.ackd.2018.02.010
National Heart, Lung, and Blood Institute (2021) Quality assessment tool for observational cohort and cross-sectional studies. https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools. Accessed 20 Nov 2021
National Heart, Lung, and Blood Institute (2021) Quality assessment of case-control studies. https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools. Accessed 20 Nov 2021
Chiuve SE, Korngold EC, Januzzi JL Jr, Gantzer ML, Albert CM (2011) Plasma and dietary magnesium and risk of sudden cardiac death in women. Am J Clin Nutr 93:253–260. https://doi.org/10.3945/ajcn.110.00225
Kieboom B, Niemeijer M, Leening M, van den Berg M, Franco O, Deckers J et al (2016) Serum magnesium and the risk of death from coronary heart disease and sudden cardiac death. J Am Heart Assoc. https://doi.org/10.1161/jaha.115.002707
Peacock J, Ohira T, Post W, Sotoodehnia N, Rosamond W, Folsom A (2010) Serum magnesium and risk of sudden cardiac death in the atherosclerosis risk in communities (ARIC) study. Am Heart J 160(3):464–470. https://doi.org/10.1016/j.ahj.2010.06.012
Naksuk N, Hu T, Krittanawong C, Thongprayoon C, Sharma S, Park J et al (2017) Association of serum magnesium on mortality in patients admitted to the intensive cardiac care unit. Am J Med 130(2):229.e5–229.e13. https://doi.org/10.1016/j.amjmed.2016.08.033
Eichhorn E, Tandon P, Dibianco R, Timmis G, Fenster P, Shannon J et al (1993) Clinical and prognostic significance of serum magnesium concentration in patients with severe chronic congestive heart failure: the promise study. J Am Coll Cardiol 21(3):634–640. https://doi.org/10.1016/0735-1097(93)90095-i
Madsen B, Rasmussen V, Hansen J (1997) Predictors of sudden death and death from pump failure in congestive heart failure are different. Analysis of 24 h Holter monitoring, clinical variables, blood chemistry, exercise test and radionuclide angiography. Int J Cardiol 58(2):151–162. https://doi.org/10.1016/s0167-5273(96)02853-7
Goldberger J, Cain M, Hohnloser S, Kadish A, Knight B, Lauer M et al (2008) American heart association/American college of cardiology foundation/heart rhythm society scientific statement on noninvasive risk stratification techniques for identifying patients at risk for sudden cardiac death: a scientific statement from the American heart association council on clinical cardiology committee on electrocardiography and arrhythmias and council on epidemiology and prevention. Circulation 118(14):1497–1518
Goldberger JJ, Buxton AE, Cain M, Costantini O, Exner DV, Knight BP et al (2011) Risk stratification for arrhythmic sudden cardiac death: identifying the roadblocks. Circulation 123(21):2423–2430
Chakraborti S, Chakraborti T, Mandal M, Mandal A, Das S, Ghosh S (2002) Protective role of magnesium in cardiovascular diseases: a review. Mol Cell Biochem 238(1):163–179. https://doi.org/10.1023/a:1019998702946
Fazekas T, Scherlag BJ, Vos M, Wellens HJ, Lazzara R (1993) Magnesium and the heart: antiarrhythmic therapy with magnesium. Clin Cardiol 16(11):768–774. https://doi.org/10.1002/clc.4960161105
Williamson M, Snyder L (2011) Wallach’s interpretation of diagnostic tests. Wolters Kluwer/Lippincott Williams & Wilkins Health, Philadelphia
Fiset C, Kargacin ME, Kondo CS, Lester WM, Duff HJ (1996) Hypomagnesemia: characterization of a model of sudden cardiac death. J Am Coll Cardiol 27(7):1771–1776. https://doi.org/10.1016/0735-1097(96)00089-7
Cannon LA, Heiselman DE, Dougherty JM, Jones J (1987) Magnesium levels in cardiac arrest victims: relationship between magnesium levels and successful resuscitation. Ann Emerg Med 16(11):1195–1199. https://doi.org/10.1016/s0196-0644(87)80222-6
Zhang X, Del Gobbo L, Hruby A, Rosanoff A, He K, Dai Q et al (2016) The circulating concentration and 24‑h urine excretion of magnesium dose- and time-dependently respond to oral magnesium supplementation in a meta-analysis of randomized controlled trials. J Nutr 146(3):595–602. https://doi.org/10.3945/jn.115.223453
Li J, Hovey K, Andrews C, Quddus A, Allison M, Van Horn L et al (2020) Association of dietary magnesium intake with fatal coronary heart disease and sudden cardiac death. J Womens Health (Larchmt) 29(1):7–12. https://doi.org/10.1089/jwh.2019.777
Haigney M, Silver B, Tanglao E, Silverman H, Hill J, Shapiro E et al (1995) Noninvasive measurement of tissue magnesium and correlation with cardiac levels. Circulation 92(8):2190–2197. https://doi.org/10.1161/01.cir.92.8.2190
Ralston M, Murnane M, Kelley R, Altschuld R, Unverferth D, Leier C (1989) Magnesium content of serum, circulating mononuclear cells, skeletal muscle, and myocardium in congestive heart failure. Circulation 80(3):573–580. https://doi.org/10.1161/01.cir.80.3.573
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
E. Davis, B.C. Fernando, L.F.J. Jusni, K.R. Hendryan, R. Kuatama, and D.A. Ridjab declare that they have no competing interests.
For this article no studies with human participants or animals were performed by any of the authors. All studies mentioned were in accordance with the ethical standards indicated in each case.
Additional information

Scan QR code & read article online
Rights and permissions
About this article
Cite this article
Davis, E., Fernando, B.C., Jusni, L.F.J. et al. Circulating magnesium as a potential risk stratification tool for sudden cardiac death: a systematic review. Herzschr Elektrophys 34, 153–160 (2023). https://doi.org/10.1007/s00399-023-00941-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00399-023-00941-8
Keywords
- Normomagnesemia
- Sudden cardiac death
- Stratification strategy
- Left ventricular ejection fraction
- Mortality