Abstract
Aims
Troponin I (TNI) is an established marker for the diagnosis of acute coronary syndrome (ACS). The study evaluated if (induced) tachycardiac arrhyhthmias within the scope of the electrophysiological studies (EPS) led to elevation of TNI serum levels.
Method
TNI was measured in the serum of 28 patients before and after the EPS. The left ventricular ejection fraction (LV-EF) was investigated by two-dimensional echocardiography. Left ventricle hypertrophy (LVH) was measured according to the recommendations of the American Society of Echocardiography. All patients underwent coronary angiography prior to the EPS, and significant coronary heart disease was defined as stenosis > 50%. The EPS revealed supraventricular and ventricular tachycardias using the 18-step protocol with one, two, and three extrastimuli.
Results
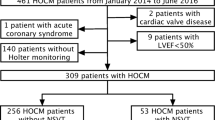
Indications for the EPS were syncope (n = 15), atrioventricular tachycardia (n = 4), non-sustained VT (n = 6), and sustained VT (n = 3). Coronary heart disease (CHD) was detected in 8 patients (1-vessel: n = 3; 2-vessel: n = 4; 3-vessel: n = 1), and 2 patients underwent percutaneous coronary intervention before EPS. Echocardiography revealed normal LV-EF in 18 patients and a reduction in the others (low n = 3, middle n = 5, high n = 2). Thirteen patients suffered from LVH. In 2 patients, external cardioversion was required during the EPS. TNI was elevated over 0.1 ng/ml (risk stratification cut-off for ACS) in 4 patients before and in 12 patients after EPS. There was no relationship between LV-EF, CHD, and the elevation of TNI after the EPS.
Conclusion
TNI can be elevated by (induced) tachycardias within the scope of electrophysiological studies without a relationship to LV-EF, LVH, and CHD.
Zusammenfassung
Ziel
Troponin I (TNI) ist ein etablierter Marker für die Diagnose eines akuten Koronarsyndroms (ACS). In der vorliegenden Studie wurde ermittelt, ob (induzierte) tachykarde Arrhythmien im Rahmen elektrophysiologischer Untersuchungen (EPU) zur Erhöhung des TNI-Serumspiegels führten.
Methode
TNI wurde im Serum von 28 Patienten vor und nach EPU bestimmt. Die linksventrikuläre Ejektionsfraktion (LV-EF) wurde mittels zweidimensionaler Echokardiographie gemessen. Eine linksventrikuläre Hypertrophie (LVH) wurde gemäß den Empfehlungen der American Society of Echocardiography ermittelt. Bei allen Patienten wurde eine Koronarangiographie vor der EPU durchgeführt, eine signifikante koronare Herzkrankheit (KHK) war als Stenose > 50% definiert. Bei der EPU wurde eine Stimulation mittels des 18-Schritt-Schemas mit einem, zwei und drei Extrastimuli durchgeführt.
Ergebnisse
Indikationen für EPU waren Synkope (n = 15), atrioventrikuläre Tachykardien (n = 4), nichtanhaltende VT (n = 6), und anhaltende VT (n = 3). Eine KHK wurde bei 8 Patienten festgestellt (1-Gefäß-Erkrankung: n = 3; 2-Gefäß-Erkr.: n = 4; 3-Gefäß-Erkr.: n = 1), und bei 2 Patienten erfolgte eine perkutane Koronarintervention vor EPU. Die Echokardiographie ergab eine normale LV-EF bei 18 Patienten und eine eingeschränkte LV-EF bei den übrigen (leightgradig: n = 3, mittelgradig: n = 5, hochgradig: n = 2). Eine LVH lag bei 13 Patienten vor. Bei 2 Patienten war eine externe Kardioversion während der EPU erforderlich. Bei 4 Patienten vor und bei 12 Patienten nach EPU war TNI über 0,1 ng/ml erhöht (Risikostratifizierungsgrenzwert für ACS). Es gab keinen Zusammenhang zwischen LV-EF, KHK und TNI-Erhöhung nach EPU.
Fazit
TNI kann durch (induzierte) Tachykardien im Rahmen einer EPU erhöht sein, ohne einen Zusammenhang mit LV-EF, LVH und KHK zu zeigen.
Similar content being viewed by others
References
Antman EM, Tanasijevic MJ, Thompson B et al (1996) Cardiac specific troponin I levels to predict the risk of mortality in patients with acute coronary syndromes. N Engl J Med 335:1342–1349
Galvani M, Ottani F, Ferrini D et al (1997) Prognostic influence of elevated values of cardiac troponin I in patients with unstable angina. Circulation 95:2053–2059
Lüscher MS, Thygesen K, Ravkilde J, Heickendorff L (1997) Applicability of cardiac troponin T and I for early risk stratification in unstable coronary disease. Circulation 96:2578–2585
Polanczyk CA, Lee TH, Cook EF et al (1998) Cardiac troponin I as a predictor of major cardiac events in emergency department patients with acute chest pain. J Am Coll Cardiol 32:8–14
Logeart D, Beyne P, Cusson C et al (2001) Evidence of cardiac myolysis in severe nonischenic heart failure and the potential role of incerased wall strain. Am Heart J 141:247–253
Nunes JP, Magalhaes D, Dias P, Faria DB (2001) Troponin I elevation after pericardiocentesis for cardiac tamponade: a role for myocardial strain? Int J Cardiol 81:277–278
Nunes JP, Macedo F (2000) An analytical triad for the diagnosis of pulmonary embolism. Cardiology 94:264
Bakshi TK, Choo MK, Edwards CC et al (2002) Causes of elevated troponin I with normal coronary angiogram. Intern J Med 32:520–525
Nunes JP, Silva JC, Maciel MJ (2004) Troponin I in atrial fibrillation with no coronary atherosclerosis. Acta Cardiol 59(3):345–346
Zellweger MJ, Schaer BA, Cron TA et al (2003) Elevated troponin levels in the absence of coronary artery disease after supraventricular tachycardia. Swiss Med Wkly 133:439–441
Morrow DA, Rifai N, Tanasijevic MJ et al (2000) Clinical efficacy of three assays for cardiac troponin I for risk stratification in acute coronary syndromes- a TIMI 11b substudy. Clin Chem 46(4):453–460
Erbel R, Krebs W, Henn G et al (1982) Comparison of single-plane and biplane volume determination two-dimensional echocardiography. 1. Asymmetric model hearts. Eur Heart J 3:469–480
Erbel R, Schweizer P, Lambertz H et al (1983) Echoventriculography – a simultaneous analysis of two-dimensional echocardiography and cineventriculography. Circulation 67:205–215
Voelker W (2004) Arbeitsgruppe Kardiovaskulärer Ultraschall der DGK. A structured report data set for documentation of echocardiographic studies – Update 2004. Z Kardiol 93(12):987–1004
Kennedy JW, Reichenbach DD, Baxley WA, Dodge HAT (1967) Left ventricular mass: a comparison of angiographic measurements with autopsy weight. Am J Cardiol 19:221–224
Dietz R, Rauch B (2003) Leitlinie zur Diagnose und Behandlung der koronaren Herzkrankheit der Deutschen Gesellschaft für Kardiologie-Herz- und Kreislaufforschung (DGK). Z Kardiol 92:501–521
Bonzel T, Erbel R, Hamm CW et al (2008) Perkutane Koronarinterventionen. Clin Res Cardiol 97:513–547
Hummel JD, Strickberger SA, Daoud E et al (1994) Results of programmed ventricular stimulation with four extrastimuli compared with one, two and three extrastimuli. Circulation 90:2827–2832
Morady F, Kadish A, Buitleir M de et al (1991) Prospective comparison of a conventional and an accelerated protocol of programmed ventricular stimulation in patients with coronary artery disease. Circulation 83:764–773
Wilkinson JM, Grand RJ (1978) Comparison of amino acid sequence of troponin I from different striated muscles. Nature 271:31–35
Adams JE 3rd, Schechtman KB, Landt Y et al (1994) Comparable detection of acute myocardial infarction by creatine kinase MB isoenzyme and cardiac troponin. J Clin Chem 40:1291–1295
Bleier J, Vorderwinkler KP, Falkensammer J et al (1998) Different intracellular compartmentations of cardiac troponins amd myosin heavy chains: a causal connection to their different early release after myocardial damage. Clin Chem 44:1912–1918
Katus HA, Remppis A, Neumann FJ et al (1991) Diagnostic efficiency of troponin T measurements in acute myocardial infarction. Circulation 83:902–12, ([see comment] 902–12. Comment in Circulation 1991; 83:1107–1109)
Mair J, Genser N, Morandell D et al (1996) Cardiac troponin I in the diagnosis of myocardial injury and infarction. Clin Chim Acta 245(1):19–38
Nunes JP (2001) Cardiac troponin I in systemic diseases. A possible role for myocardial strain. Rev Port Cardiol 20:785–788
Sobel BE, LeWinter MM (2000) Ingenuous interpretation of elevated blood levels of macromolecular markers of myocardial injury: a recipe for confusion. J Am Coll Cardiol 35:1355–1358, [review]
Feng J, Schaus BJ, Fallavollita JA et al (2001) Preload induces troponin I degradation independently of myocardial ischemia. Circulation 103:2035–2037
McDonough JL, Arrell DH, Eyk JE van (1999) Troponin I degradation and covalent complex formation accompanies myocardial ischemia/reperfusion injury. Circ Res 84:9–20
Rao SP, Miller S, Rosenbaum R, Lakier JB (1999) Cardiac troponin I and cardiac enzymes after electrophysiologic studies, ablations and defibrillator implantations. Am J Cardiol 84(4):470, A9
Goktekin O, Melek M, Gorenek B et al (2002) Cardiac troponin T and cardiac enzymes after external transthoracic cardioversion of ventricular arrhythmias in patients with coronary artery disease. Chest 122(6):2050–2054
Vikines K, Omvik P, Farstas M, Nordrehaug JE (2000) Cardiac biochemical markers after cardioversion of atrial fibrillation or atrial flutter. Am Heart J 140(4):690–696
Kosior DA, Opolski G, Tadeusiak W et al (2005) Serum troponin I and myoglobin after monophasic versus biphasic transthoracic shocks for cardioversion of persistent atrial fibrillation. Pacing Clin Electrophysiol 28(Suppl I):128–132
Conflict of interest
The corresponding author states that there are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bandorski, D., Bogossian, H., Lemke, B. et al. Do induced tachycardias within the scope of electrophysiological studies lead to elevated plasma troponin I levels?. Herzschr. Elektrophys. 22, 214–218 (2011). https://doi.org/10.1007/s00399-011-0151-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00399-011-0151-0