Abstract
Purpose
We aimed to investigate the relationship between overall nutritional status and cancer mortality.
Methods
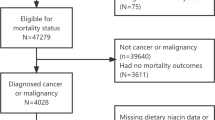
A total of 12 262 US adults from six consecutive surveys of the National Health and Nutrition Examination Survey (NHANES 2003–2014) were analyzed. The overall health nutritional biomarkers index (HNBI) score, capturing characteristics of 17 biomarkers was developed to assess the overall nutritional status. The lower the HNBI score, the healthier nutritional status would be. Hazard ratio (HR) and 95% confidence intervals (95% CIs) were calculated by Cox proportional hazards regression models to evaluate the association between the HNBI score and cancer mortality.
Results
The lower overall HNBI score was associated with decreased risk of cancer mortality, compared with participants in the 4th quartile of overall HNBI score, the HR (95% CIs) for participants in the 1st quartiles was 0.54 (0.33–0.89) (P-trend = 0.019). Healthier lifestyle habits and not obesity interacted with HNBI score, compared with participants with higher HNBI score and smoking currently/not exercising regularly/obesity, participants with lower HNBI score and not smoking currently/exercising regularly/not obesity were associated with lower risk of cancer mortality, the HR (95% CIs) were 0.43 (0.26–0.73), 0.57 (0.33–0.97), and 0.62 (0.47–0.97), respectively. These significant associations remained among participants who were followed-up more than 2 years.
Conclusion
Our findings suggested that healthier overall nutritional status was associated with lower risk of cancer mortality among US adults. Not smoking, exercise regularly and not obesity interacted with overall nutritional status. Adherence to better overall nutritional status, lifestyle habits and optimal weight would prevent premature death from cancer.

Similar content being viewed by others
Availability of data and materials
Data described in the manuscript, code book, and analytic code will be made publicly and freely available without restriction at https://www.cdc.gov/nchs/nhanes/.
References
Global health estimates 2016: deaths by cause, age, sex, by country and by region, 2000–2016. Geneva, World Health Organization; 2018
Mayne ST, Playdon MC, Rock CL (2016) Diet, nutrition, and cancer: past, present and future. Nat Rev Clin Oncol 13(8):504–515. https://doi.org/10.1038/nrclinonc.2016.24
Collaborators USBoD, Mokdad AH, Ballestros K, Echko M, Glenn S, Olsen HE, Mullany E, Lee A, Khan AR, Ahmadi A, Ferrari AJ, Kasaeian A, Werdecker A, Carter A, Zipkin B, Sartorius B, Serdar B, Sykes BL, Troeger C, Fitzmaurice C, Rehm CD, Santomauro D, Kim D, Colombara D, Schwebel DC, Tsoi D, Kolte D, Nsoesie E, Nichols E, Oren E, Charlson FJ, Patton GC, Roth GA, Hosgood HD, Whiteford HA, Kyu H, Erskine HE, Huang H, Martopullo I, Singh JA, Nachega JB, Sanabria JR, Abbas K, Ong K, Tabb K, Krohn KJ, Cornaby L, Degenhardt L, Moses M, Farvid M, Griswold M, Criqui M, Bell M, Nguyen M, Wallin M, Mirarefin M, Qorbani M, Younis M, Fullman N, Liu P, Briant P, Gona P, Havmoller R, Leung R, Kimokoti R, Bazargan-Hejazi S, Hay SI, Yadgir S, Biryukov S, Vollset SE, Alam T, Frank T, Farid T, Miller T, Vos T, Barnighausen T, Gebrehiwot TT, Yano Y, Al-Aly Z, Mehari A, Handal A, Kandel A, Anderson B, Biroscak B, Mozaffarian D, Dorsey ER, Ding EL, Park EK, Wagner G, Hu G, Chen H, Sunshine JE, Khubchandani J, Leasher J, Leung J, Salomon J, Unutzer J, Cahill L, Cooper L, Horino M, Brauer M, Breitborde N, Hotez P, Topor-Madry R, Soneji S, Stranges S, James S, Amrock S, Jayaraman S, Patel T, Akinyemiju T, Skirbekk V, Kinfu Y, Bhutta Z, Jonas JB, Murray CJL (2018) The State of US Health, 1990–2016: burden of diseases, injuries, and risk factors among US States. JAMA. 319(14):1444–1472. https://doi.org/10.1001/jama.2018.0158
Zhang FF, Cudhea F, Shan Z, Michaud DS, Imamura F, Eom H, Ruan M, Rehm CD, Liu J, Du M, Kim D, Lizewski L, Wilde P, Mozaffarian D (2019) Preventable Cancer Burden Associated with poor diet in the United States. JNCI Cancer Spectr 3(2):pkz034. https://doi.org/10.1093/jncics/pkz034
Islami F, Goding Sauer A, Miller KD, Siegel RL, Fedewa SA, Jacobs EJ, McCullough ML, Patel AV, Ma J, Soerjomataram I, Flanders WD, Brawley OW, Gapstur SM, Jemal A (2018) Proportion and number of cancer cases and deaths attributable to potentially modifiable risk factors in the United States. CA Cancer J Clin 68(1):31–54. https://doi.org/10.3322/caac.21440
Akbaraly TN, Ferrie JE, Berr C, Brunner EJ, Head J, Marmot MG, Singh-Manoux A, Ritchie K, Shipley MJ, Kivimaki M (2011) Alternative Healthy Eating Index and mortality over 18 y of follow-up: results from the Whitehall II cohort. Am J Clin Nutr 94(1):247–253. https://doi.org/10.3945/ajcn.111.013128
Reedy J, Krebs-Smith SM, Miller PE, Liese AD, Kahle LL, Park Y, Subar AF (2014) Higher diet quality is associated with decreased risk of all-cause, cardiovascular disease, and cancer mortality among older adults. J Nutr 144(6):881–889. https://doi.org/10.3945/jn.113.189407
Lassale C, Gunter MJ, Romaguera D, Peelen LM, Van der Schouw YT, Beulens JW, Freisling H, Muller DC, Ferrari P, Huybrechts I, Fagherazzi G, Boutron-Ruault MC, Affret A, Overvad K, Dahm CC, Olsen A, Roswall N, Tsilidis KK, Katzke VA, Kuhn T, Buijsse B, Quiros JR, Sanchez-Cantalejo E, Etxezarreta N, Huerta JM, Barricarte A, Bonet C, Khaw KT, Key TJ, Trichopoulou A, Bamia C, Lagiou P, Palli D, Agnoli C, Tumino R, Fasanelli F, Panico S, Bueno-de-Mesquita HB, Boer JM, Sonestedt E, Nilsson LM, Renstrom F, Weiderpass E, Skeie G, Lund E, Moons KG, Riboli E, Tzoulaki I (2016) Diet quality scores and prediction of all-cause, cardiovascular and cancer mortality in a pan-European Cohort Study. PLoS One 11(7):e0159025. https://doi.org/10.1371/journal.pone.0159025
Mursu J, Steffen LM, Meyer KA, Duprez D, Jacobs DR Jr (2013) Diet quality indexes and mortality in postmenopausal women: the Iowa Women’s Health Study. Am J Clin Nutr 98(2):444–453. https://doi.org/10.3945/ajcn.112.055681
Park YM, Fung TT, Steck SE, Zhang J, Hazlett LJ, Han K, Lee SH, Merchant AT (2016) Diet quality and mortality risk in metabolically obese normal-weight adults. Mayo Clin Proc 91(10):1372–1383. https://doi.org/10.1016/j.mayocp.2016.06.022
Vargas AJ, Neuhouser ML, George SM, Thomson CA, Ho GY, Rohan TE, Kato I, Nassir R, Hou L, Manson JE (2016) Diet quality and colorectal cancer risk in the Women’s Health Initiative Observational Study. Am J Epidemiol 184(1):23–32. https://doi.org/10.1093/aje/kwv304
Cuenca-Garcia M, Artero EG, Sui X, Lee DC, Hebert JR, Blair SN (2014) Dietary indices, cardiovascular risk factors and mortality in middle-aged adults: findings from the Aerobics Center Longitudinal Study. Ann Epidemiol 24(4):297-303 e292. https://doi.org/10.1016/j.annepidem.2014.01.007
Izano MA, Fung TT, Chiuve SS, Hu FB, Holmes MD (2013) Are diet quality scores after breast cancer diagnosis associated with improved breast cancer survival? Nutr Cancer 65(6):820–826. https://doi.org/10.1080/01635581.2013.804939
Elmadfa I, Meyer AL (2014) Developing suitable methods of nutritional status assessment: a continuous challenge. Adv Nutr 5(5):590S-598S. https://doi.org/10.3945/an.113.005330
Potischman N (2003) Biologic and methodologic issues for nutritional biomarkers. J Nutr 133(Suppl 3):875S-880S. https://doi.org/10.1093/jn/133.3.875S
Freedman DM, Looker AC, Abnet CC, Linet MS, Graubard BI (2010) Serum 25-hydroxyvitamin D and cancer mortality in the NHANES III study (1988–2006). Cancer Res 70(21):8587–8597. https://doi.org/10.1158/0008-5472.CAN-10-1420
Rossi E, Hung J, Beilby JP, Knuiman MW, Divitini ML, Bartholomew H (2006) Folate levels and cancer morbidity and mortality: prospective cohort study from Busselton. Western Australia Ann Epidemiol 16(3):206–212. https://doi.org/10.1016/j.annepidem.2005.03.010
Peng Y, Dong B, Wang Z (2016) Serum folate concentrations and all-cause, cardiovascular disease and cancer mortality: a cohort study based on 1999–2010 National Health and Nutrition Examination Survey (NHANES). Int J Cardiol 219:136–142. https://doi.org/10.1016/j.ijcard.2016.06.024
Katzke VA, Sookthai D, Johnson T, Kuhn T, Kaaks R (2017) Blood lipids and lipoproteins in relation to incidence and mortality risks for CVD and cancer in the prospective EPIC-Heidelberg cohort. BMC Med 15(1):218. https://doi.org/10.1186/s12916-017-0976-4
Cheung MR (2013) Blood lead concentration correlates with all cause, all cancer and lung cancer mortality in adults: a population based study. Asian Pac J Cancer Prev 14(5):3105–3108. https://doi.org/10.7314/apjcp.2013.14.5.3105
Gupta D, Lis CG (2010) Pretreatment serum albumin as a predictor of cancer survival: a systematic review of the epidemiological literature. Nutr J 9:69. https://doi.org/10.1186/1475-2891-9-69
Wang M, Xu Y, Pan S, Zhang J, Zhong A, Song H, Ling W (2011) Long-term heavy metal pollution and mortality in a Chinese population: an ecologic study. Biol Trace Elem Res 142(3):362–379. https://doi.org/10.1007/s12011-010-8802-2
Yang Q, Bostick RM, Friedman JM, Flanders WD (2009) Serum folate and cancer mortality among U.S. adults: findings from the Third National Health and Nutritional Examination Survey linked mortality file. Cancer Epidemiol Biomarkers Prev. 18(5):1439–1447. https://doi.org/10.1158/1055-9965.EPI-08-0908
Khaw KT, Luben R, Wareham N (2014) Serum 25-hydroxyvitamin D, mortality, and incident cardiovascular disease, respiratory disease, cancers, and fractures: a 13-y prospective population study. Am J Clin Nutr 100(5):1361–1370. https://doi.org/10.3945/ajcn.114.086413
Sritara P, Patoomanunt P, Woodward M, Narksawat K, Tulyadachanon S, Ratanachaiwong W, Sritara C, Barzi F, Yamwong S, Tanomsup S (2007) Associations between serum lipids and causes of mortality in a cohort of 3499 urban Thais: Tthe Electricity Generating Authority of Thailand (EGAT) study. Angiology 58(6):757–763. https://doi.org/10.1177/0003319707304042
Schober SE, Mirel LB, Graubard BI, Brody DJ, Flegal KM (2006) Blood lead levels and death from all causes, cardiovascular disease, and cancer: results from the NHANES III mortality study. Environ Health Perspect 114(10):1538–1541. https://doi.org/10.1289/ehp.9123
Schwingshackl L, Bogensberger B, Hoffmann G (2018) Diet quality as assessed by the healthy eating index, alternate healthy eating index, dietary approaches to stop hypertension score, and health outcomes: an updated systematic review and meta-analysis of cohort studies. J Acad Nutr Diet 118(1):74–100. https://doi.org/10.1016/j.jand.2017.08.024
Chen TC, Parker JD, Clark J, Shin HC, Rammon JR, Burt VL (2018) National Health and Nutrition Examination Survey: estimation procedures, 2011–2014. Vital Health Stat 2(177):1–26
Pfeiffer CM, Hughes JP, Lacher DA, Bailey RL, Berry RJ, Zhang M, Yetley EA, Rader JI, Sempos CT, Johnson CL (2012) Estimation of trends in serum and RBC folate in the US population from pre- to postfortification using assay-adjusted data from the NHANES 1988–2010. J Nutr 142(5):886–893. https://doi.org/10.3945/jn.111.156919
Schleicher RL, Sternberg MR, Lacher DA, Sempos CT, Looker AC, Durazo-Arvizu RA, Yetley EA, Chaudhary-Webb M, Maw KL, Pfeiffer CM, Johnson C (2016) A Method-bridging Study for Serum 25-hydroxyvitamin D to standardize historical radioimmunoassay data to liquid chromatography-tandem mass spectrometry. Natl Health Stat Rep 93:1–16
Wilson PW, Abbott RD, Garrison RJ, Castelli WP (1981) Estimation of very-low-density lipoprotein cholesterol from data on triglyceride concentration in plasma. Clin Chem 27(12):2008–2010
Patterson RE, Haines PS, Popkin BM (1994) Diet quality index: capturing a multidimensional behavior. J Am Diet Assoc 94(1):57–64. https://doi.org/10.1016/0002-8223(94)92042-7
Neuhouser ML, Patterson RE, King IB, Horner NK, Lampe JW (2003) Selected nutritional biomarkers predict diet quality. Public Health Nutr 6(7):703–709. https://doi.org/10.1079/phn2003486
The Linkage of National Center for Health Statistics Survey Data to the National Death Index–2015 Linked Mortality File (LMF): Methodology Overview and Analytic Considerations. Accessed Apr 11, 2019.
January CT, Wann LS, Calkins H, Chen LY, Cigarroa JE, Cleveland JC Jr, Ellinor PT, Ezekowitz MD, Field ME, Furie KL, Heidenreich PA, Murray KT, Shea JB, Tracy CM, Yancy CW (2019) 2019 AHA/ACC/HRS Focused Update of the 2014 AHA/ACC/HRS Guideline for the Management of patients with atrial fibrillation: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society in Collaboration With the Society of Thoracic Surgeons. Circulation 140(2):e125–e151. https://doi.org/10.1161/CIR.0000000000000665
Reedy J, Lerman JL, Krebs-Smith SM, Kirkpatrick SI, Pannucci TE, Wilson MM, Subar AF, Kahle LL, Tooze JA (2018) Evaluation of the Healthy Eating Index-2015. J Acad Nutr Diet 118(9):1622–1633. https://doi.org/10.1016/j.jand.2018.05.019
Plan and operation of the Third National Health and Nutrition Examination Survey, 1988–94. Series 1: programs and collection procedures (1994). Vital Health Stat 1 (32): 1–407
Knol MJ, VanderWeele TJ, Groenwold RH, Klungel OH, Rovers MM, Grobbee DE (2011) Estimating measures of interaction on an additive scale for preventive exposures. Eur J Epidemiol 26(6):433–438. https://doi.org/10.1007/s10654-011-9554-9
Hosmer DW, Lemeshow S (1992) Confidence interval estimation of interaction. Epidemiology 3(5):452–456. https://doi.org/10.1097/00001648-199209000-00012
Monteiro CA, Cannon G, Levy RB, Moubarac JC, Louzada ML, Rauber F, Khandpur N, Cediel G, Neri D, Martinez-Steele E, Baraldi LG, Jaime PC (2019) Ultra-processed foods: what they are and how to identify them. Public Health Nutr 22(5):936–941. https://doi.org/10.1017/S1368980018003762
Rohrmann S, Braun J, Bopp M, Faeh D, Swiss National C (2013) Inverse association between circulating vitamin D and mortality–dependent on sex and cause of death? Nutr Metab Cardiovasc Dis 23(10):960–966. https://doi.org/10.1016/j.numecd.2013.05.005
Elizabeth L, Machado P, Zinocker M, Baker P, Lawrence M (2020) Ultra-processed foods and health outcomes: a narrative review. Nutrients 12(7):1955. https://doi.org/10.3390/nu12071955
Zhao M, Veeranki SP, Li S, Steffen LM, Xi B (2019) Beneficial associations of low and large doses of leisure time physical activity with all-cause, cardiovascular disease and cancer mortality: a national cohort study of 88,140 US adults. Br J Sports Med 53(22):1405–1411. https://doi.org/10.1136/bjsports-2018-099254
O’Donovan G, Lee IM, Hamer M, Stamatakis E (2017) Association of “Weekend Warrior” and Other Leisure time physical activity patterns with risks for all-cause, cardiovascular disease, and cancer mortality. JAMA Intern Med 177(3):335–342. https://doi.org/10.1001/jamainternmed.2016.8014
Zhang M, An Q, Yeh F, Zhang Y, Howard BV, Lee ET, Zhao J (2015) Smoking-attributable mortality in American Indians: findings from the Strong Heart Study. Eur J Epidemiol 30(7):553–561. https://doi.org/10.1007/s10654-015-0031-8
Bhaskaran K, Dos-Santos-Silva I, Leon DA, Douglas IJ, Smeeth L (2018) Association of BMI with overall and cause-specific mortality: a population-based cohort study of 36 million adults in the UK. Lancet Diabetes Endocrinol 6(12):944–953. https://doi.org/10.1016/S2213-8587(18)30288-2
Bawaked RA, Gomez SF, Homs C, Casas Esteve R, Cardenas G, Fito M, Schroder H (2018) Association of eating behaviors, lifestyle, and maternal education with adherence to the Mediterranean diet in Spanish children. Appetite 130:279–285. https://doi.org/10.1016/j.appet.2018.08.024
Zurita-Ortega F, San Roman-Mata S, Chacon-Cuberos R, Castro-Sanchez M, Muros JJ (2018) Adherence to the Mediterranean diet is associated with physical activity, self-concept and sociodemographic factors in university student. Nutrients 10(8):966. https://doi.org/10.3390/nu10080966
Larson NI, Story M, Perry CL, Neumark-Sztainer D, Hannan PJ (2007) Are diet and physical activity patterns related to cigarette smoking in adolescents? Findings from Project EAT. Prev Chronic Dis 4(3):A51
Jamal A, Homa DM, O’Connor E, Babb SD, Caraballo RS, Singh T, Hu SS, King BA (2015) Current cigarette smoking among adults-United States, 2005–2014. MMWR Morb Mortal Wkly Rep 64(44):1233–1240. https://doi.org/10.15585/mmwr.mm6444a2
Piercy KL, Troiano RP, Ballard RM, Carlson SA, Fulton JE, Galuska DA, George SM, Olson RD (2018) The physical activity guidelines for Americans. JAMA 320(19):2020–2028. https://doi.org/10.1001/jama.2018.14854
Ogden CL, Fryar CD, Hales CM, Carroll MD, Aoki Y, Freedman DS (2018) Differences in obesity prevalence by demographics and Urbanization in US children and adolescents, 2013–2016. JAMA 319(23):2410–2418. https://doi.org/10.1001/jama.2018.5158
Rhodes DG, Murayi T, Clemens JC, Baer DJ, Sebastian RS, Moshfegh AJ (2013) The USDA Automated Multiple-Pass Method accurately assesses population sodium intakes. Am J Clin Nutr 97(5):958–964. https://doi.org/10.3945/ajcn.112.044982
Acknowledgements
We thank the investigators, the staff, and the participants of the National Health and Nutrition Examination Survey for their valuable contribution.
Funding
This study was supported by the National Natural Science Foundation of China (Grant numbers: 82073536 and 81573134).
Author information
Authors and Affiliations
Contributions
WJW, DDZ, FZZ and XYW were involved in the conception and design of the study. All authors contributed to the interpretation and critical revision of manuscript. The statistical analyses were conducted by WJW and XYW.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest regarding the publication of this article.
Ethical approval
The NHANES protocol was approved by the National Center for Health Statistics Research Ethics Review Board, and all participants provided informed consent.
Consent to participate
All participants gave their informed consent prior to their inclusion in the study.
Consent for publication
Not applicable.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wu, X., Wang, W., Zhang, D. et al. Nutritional status, lifestyle habits and cancer mortality: a population-based prospective cohort study. Eur J Nutr 61, 1343–1352 (2022). https://doi.org/10.1007/s00394-021-02739-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-021-02739-1