Abstract
Purpose
We determined the association of total sugar intake with body weight and fat mass in children on an energy-equivalent basis and potential changes in the association from 2 to 8 years of age.
Methods
Data were available from the Childhood Obesity Project Trial initiated in 2002. Sugar intake was measured by 3-day weighed food protocols at 2, 3, 4, 5, 6, and 8 years of age. Body mass index (BMI) and fat mass index (FMI) were available at the same time points. To investigate the association of sugar intake with anthropometrics over time, linear mixed models were applied. Odds ratios for having a high BMI or FMI (above one standard deviation) were estimated by logistic random-effects models. To control for total energy intake, the residual method was chosen and models were additionally adjusted for total energy intake.
Results
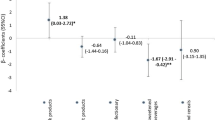
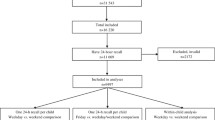
Data were available for 809 children with in total 2846 observations. In an isocaloric model, an increase of 100 kcal from sugar per day was significantly associated with lower zBMI (− 0.033; 95% CI −0.061, − 0.005) and zFMI (− 0.050; 95% CI − 0.089, − 0.011). In addition, a 100 kcal higher sugar intake was related to lower odds of having a high zBMI (OR 0.743; 95% CI 0.611, 0.903).
Conclusion
This study provides no indication that increased total sugar intake positively affects BMI on an energy-equivalent basis. Whether the negative association of sugar is due to physiological effects or points more to macronutrient preferences or a reporting bias (lower sugar intake) in children with higher BMI can be debated.
Clinical trial registry
ClinicalTrials.gov Identifier: NCT00338689; Registered: June 19, 2006. URL: http://clinicaltrials.gov/ct2/show/NCT00338689?term=NCT00338689&rank=1.
Similar content being viewed by others
Abbreviations
- BMI:
-
Body mass index
- CHOP:
-
Childhood Obesity Project
- EI:
-
Energy intake
- FMI:
-
Fat mass index
- OR:
-
Odds ratio
- WHO:
-
World Health Organization
References
UNICEF-WHO-The World Bank. Joint child malnutrition estimates. http://apps.who.int/gho/data/node.main.ngest?lang=en. Accessed 21 Oct 2019
World Health Organization (2014) Global status report on noncommunicable diseases 2014 (No. WHO/NMH/NVI/15.1). World Health Organization. Available from: https://apps.who.int/iris/bitstream/handle/10665/148114/9789241564854_eng.pdf. Accessed 21 Oct 2019
van Stralen MM, te Velde SJ, van Nassau F, Brug J, Grammatikaki E, Maes L, De Bourdeaudhuij I, Verbestel V, Galcheva S, Iotova V, Koletzko BV, von Kries R, Bayer O, Kulaga Z, Serra-Majem L, Sanchez-Villegas A, Ribas-Barba L, Manios Y, Chinapaw MJ (2012) Weight status of European preschool children and associations with family demographics and energy balance-related behaviours: a pooled analysis of six European studies. Obes Rev 13(Suppl 1):29–41. https://doi.org/10.1111/j.1467-789X.2011.00959.x
Organization WH (2015) Guideline: sugars intake for adults and children. World Health Organization,
Bray GA, Popkin BM (2014) Dietary sugar and body weight: have we reached a crisis in the epidemic of obesity and diabetes?: health be damned! Pour on the sugar. Diabetes Care 37(4):950–956. https://doi.org/10.2337/dc13-2085
Perrar I, Schmitting S, Della Corte KW, Buyken AE, Alexy U (2019) Age and time trends in sugar intake among children and adolescents: results from the DONALD study. Eur J Nutr. https://doi.org/10.1007/s00394-019-01965-y
Malik VS, Schulze MB, Hu FB (2006) Intake of sugar-sweetened beverages and weight gain: a systematic review1–3. Am J Clin Nutr 84(2):274–288. https://doi.org/10.1093/ajcn/84.1.274
van Baak MA, Astrup A (2009) Consumption of sugars and body weight. Obes Rev 10(Suppl 1):9–23. https://doi.org/10.1111/j.1467-789X.2008.00561.x
Ludwig DS, Ebbeling CB (2018) The carbohydrate-insulin model of obesity: beyond “calories in, calories Out”. JAMA Intern Med 178(8):1098–1103. https://doi.org/10.1001/jamainternmed.2018.2933
Rippe JM, Angelopoulos TJ (2016) Sugars, obesity, and cardiovascular disease: results from recent randomized control trials. Eur J Nutr 55(2):45–53. https://doi.org/10.1007/s00394-016-1257-2
Public Health England (2015) SACN Carbohydrates and Health Report [Online]. Available from: http://publichealthwell.ie/node/887648. Accessed 21 Oct 2019
Te Morenga L, Mallard S, Mann J (2013) Dietary sugars and body weight: systematic review and meta-analyses of randomised controlled trials and cohort studies. Bmj 346:e7492. https://doi.org/10.1136/bmj.e7492
European Childhood Obesity Trial Study G (2009) Lower protein in infant formula is associated with lower weight up to age 2 years: a randomized clinical trial. Am J Clin Nutr 89(6):1836–1845. https://doi.org/10.3945/ajcn.2008.27091
Verwied-Jorky S, Schiess S, Luque V, Grote V, Scaglioni S, Vecchi F, Martin F, Stolarczyk A, Koletzko B, Project ftECO (2011) Methodology for longitudinal assessment of nutrient intake and dietary habits in early childhood in a transnational multicenter study. J Pediatr Gastroenterol Nutr 52(1):96–102. https://doi.org/10.1097/mpg.0b013e3181f28d33
Pawellek I, Grote V, Theurich M, Closa-Monasterolo R, Stolarczyk A, Verduci E, Xhonneux A, Koletzko B (2017) Factors associated with sugar intake and sugar sources in European children from 1 to 8 years of age. Eur J Clin Nutr 71(1):25–32. https://doi.org/10.1038/ejcn.2016.206
de Onis M, Onyango AW, Van den Broeck J, Chumlea WC, Martorell R (2004) Measurement and standardization protocols for anthropometry used in the construction of a new international growth reference. Food Nutr Bull 25(1 Suppl):S27–36. https://doi.org/10.1177/15648265040251s104
de Onis M, Onyango AW, Borghi E, Siyam A, Nishida C, Siekmann J (2007) Development of a WHO growth reference for school-aged children and adolescents. Bull World Health Organ 85(9):660–667
Slaughter MH, Lohman TG, Boileau RA, Horswill CA, Stillman RJ, Van Loan MD, Bemben DA (1988) Skinfold equations for estimation of body fatness in children and youth. Hum Biol 60(5):709–723
Totzauer M, Luque V, Escribano J, Closa-Monasterolo R, Verduci E, ReDionigi A, Hoyos J, Langhendries JP, Gruszfeld D, Socha P, Koletzko B, Grote V (2018) Effect of lower versus higher protein content in infant formula through the first year on body composition from 1 to 6 years: follow-up of a randomized clinical trial. Obes (Silver Spring Md) 26(7):1203–1210. https://doi.org/10.1002/oby.22203
UNESCO United Nations Educational, Scientific and Cultural Organization (2003) International standard classification of education, ISCED 1997. Advances in cross-national comparison: a European working book for demographic and socio-economic variables, pp 195–220. Available from: http://uis.unesco.org/sites/default/files/documents/international-standard-classification-of-education-1997-en_0.pdf. Accessed 21 Oct 2019
Schwarzfischer P, Weber M, Gruszfeld D, Socha P, Luque V, Escribano J, Xhonneux A, Verduci E, Mariani B, Koletzko B, Grote V (2017) BMI and recommended levels of physical activity in school children. BMC Pub Health 17(1):595. https://doi.org/10.1186/s12889-017-4492-4
Gomes D, Luque V, Xhonneux A, Verduci E, Socha P, Koletzko B, Berger U, Grote V (2018) A simple method for identification of misreporting of energy intake from infancy to school age: results from a longitudinal study. Clin Nutr 37(3):1053–1060. https://doi.org/10.1016/j.clnu.2017.05.003
Williams CL, Strobino BA (2008) Childhood diet, overweight, and CVD risk factors: the Healthy Start project. Prev Cardiol 11(1):11–20
Herbst A, Diethelm K, Cheng G, Alexy U, Icks A, Buyken AE (2011) Direction of associations between added sugar intake in early childhood and body mass index at age 7 years may depend on intake levels. J Nutr 141(7):1348–1354. https://doi.org/10.3945/jn.110.137000
Janssen I, Katzmarzyk PT, Boyce WF, Vereecken C, Mulvihill C, Roberts C, Currie C, Pickett W (2005) Comparison of overweight and obesity prevalence in school-aged youth from 34 countries and their relationships with physical activity and dietary patterns. Obes Rev 6(2):123–132. https://doi.org/10.1111/j.1467-789x.2005.00176.x
O’Neil CE, Fulgoni VL, Nicklas TA (2011) Association of candy consumption with body weight measures, other health risk factors for cardiovascular disease, and diet quality in US children and adolescents: NHANES 1999–2004. Food Nutr Res. https://doi.org/10.3402/fnr.v3455i3400.5794
Voortman T, Braun KV, Kiefte-de Jong JC, Jaddoe VW, Franco OH, van den Hooven EH (2016) Protein intake in early childhood and body composition at the age of 6 years: the Generation R Study. Int J Obes (Lond) 40(6):1018–1025. https://doi.org/10.1038/ijo.2016.29
Pimpin L, Jebb S, Johnson L, Wardle J, Ambrosini GL (2016) Dietary protein intake is associated with body mass index and weight up to 5 y of age in a prospective cohort of twins. Am J Clin Nutr 103(2):389–397. https://doi.org/10.3945/ajcn.115.118612
Maillard G, Charles MA, Lafay L, Thibult N, Vray M, Borys JM, Basdevant A, Eschwege E, Romon M (2000) Macronutrient energy intake and adiposity in non obese prepubertal children aged 5–11 years (the Fleurbaix Laventie Ville Sante Study). Int J Obes Relat Metab Disord 24(12):1608–1617
Rolland-Cachera MF, Akrout M, Peneau S (2016) Nutrient intakes in early life and risk of obesity. Int J Environ Res Public Health. https://doi.org/10.3390/ijerph13060564
Astrup A, Raben A (2000) Sugar as a slimming agent? Br J Nutr 84(5):585–586
Collins CE, Watson J, Burrows T (2010) Measuring dietary intake in children and adolescents in the context of overweight and obesity. Int J Obes (Lond) 34(7):1103–1115. https://doi.org/10.1038/ijo.2009.241
Graffe MIM, Pala V, De Henauw S, Eiben G, Hadjigeorgiou C, Iacoviello L, Intemann T, Jilani H, Molnar D, Russo P, Veidebaum T, Moreno LA (2019) Dietary sources of free sugars in the diet of European children: the IDEFICS Study. Eur J Nutr. https://doi.org/10.1007/s00394-019-01957-y
Sluik D, van Lee L, Engelen AI, Feskens EJM (2016) Total, free, and added sugar consumption and adherence to guidelines: the Dutch National Food Consumption Survey 2007–2010. Nutrients 8(2):70–70. https://doi.org/10.3390/nu8020070
Lin PY, Lin FY, Chen TC, Chen WL, Doong JY, Shikanai S, Sarukura N, Yamamoto S (2016) Relationship between sugar intake and obesity among school-age children in Kaohsiung, Taiwan. J Nutr Sci Vitaminol (Tokyo) 62(5):310–316. https://doi.org/10.3177/jnsv.62.310
Butte NF, Cai G, Cole SA, Wilson TA, Fisher JO, Zakeri IF, Ellis KJ, Comuzzie AG (2007) Metabolic and behavioral predictors of weight gain in Hispanic children: the Viva la Familia Study. Am J Clin Nutr 85(6):1478–1485. https://doi.org/10.1093/ajcn/85.6.1478
Berkey CS, Rockett HR, Field AE, Gillman MW, Colditz GA (2004) Sugar-added beverages and adolescent weight change. Obes Res 12(5):778–788. https://doi.org/10.1038/oby.2004.94
Rodríguez LA, Madsen KA, Cotterman C, Lustig RH (2016) Added sugar intake and metabolic syndrome in US adolescents: cross-sectional analysis of the National Health and Nutrition Examination Survey 2005–2012. Public Health Nutr 19(13):2424–2434. https://doi.org/10.1017/S1368980016000057
Ludwig DS, Peterson KE, Gortmaker SL (2001) Relation between consumption of sugar-sweetened drinks and childhood obesity: a prospective, observational analysis. Lancet. https://doi.org/10.1016/S0140-6736(00)04041-1
Wang J, Shang L, Light K, O’Loughlin J, Paradis G, Gray-Donald K (2015) Associations between added sugar (solid vs. liquid) intakes, diet quality, and adiposity indicators in Canadian children. Appl Physiol Nutr Metab 40(8):835–841. https://doi.org/10.1139/apnm-2014-0447
Hendricks K, Briefel R, Novak T, Ziegler P (2006) Maternal and child characteristics associated with infant and toddler feeding practices. J Am Diet Assoc 106(1):135–148. https://doi.org/10.1016/j.jada.2005.09.035
Acknowledgements
We thank the participating families and all project partners for their enthusiastic support of the project. Furthermore, thanks to the European Childhood Obesity Trial Study Group, who designed and conducted the study, entered the data, and participated in the data analysis.
Funding
The studies reported herein have been carried out with partial financial support from the Commission of the European Community, specifically the RTD Program “Quality of Life and Management of Living Resources” within the Fifth Framework Program (Research Grants No. QLRT-2001-00389 and QLK1-CT-200230582) and the Sixth Framework Program (Contract No. 007036), the European Union (EU) Seventh Framework Program (FP7/2007-2013), project EarlyNutrition (Grant Agreement No. 289346), the EU H2020 project PHC-2014-DynaHealth (Grant No. 633595), and the European Research Council Advanced Grant ERC-2012-AdG (No. 322605) META-GROWTH. This manuscript does not necessarily reflect the views of the Commission and in no way anticipates the future policy in this area. No funding bodies had any role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
NA analyzed the data, drafted and finalized the manuscript. DG, KG, JE, NF, DR, JH, EV, AR, BK, and VG conducted the study and entered data at study sites and critically reviewed the manuscript. BK designed the research and critically reviewed the manuscript. VG designed the research, participated in the data analysis, and critically reviewed the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Aumueller, N., Gruszfeld, D., Gradowska, K. et al. Associations of sugar intake with anthropometrics in children from ages 2 until 8 years in the EU Childhood Obesity Project. Eur J Nutr 59, 2593–2601 (2020). https://doi.org/10.1007/s00394-019-02107-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-019-02107-0