Abstract
Purpose
Available evidence on the relation between vitamin D status and Hashimoto’s thyroiditis (HT) remains inconsistent. We conducted a meta-analysis of serum 25-hydoxyvitamin [25(OH)D] concentrations in HT, and examined how the strength of this relationship varies as a function of several moderating factors.
Methods
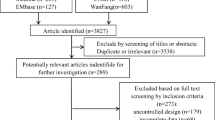
Twenty-six observational, case–control studies, published before Feb 20, 2018, were located using Google Scholar, PubMed, Web of Science, SCOPUS, LILACS and SCIELO. Study quality was assessed and random-effects models were used, along with univariate mixed-effect meta-regression, for all analyses.
Results
The 25 studies (2695 cases, 2263 controls) confirmed lower serum 25(OH)D concentrations in HT compared to healthy controls, with Cohen’s d − 0.62 (95% CI − 0.89, − 0.34; P = 1.5 × 10−5) and substantial heterogeneity between studies. HT showed an odds ratio (OR) of 3.21 (1.94–5.3; P = 5.7 × 10−6) for 25(OH)D deficiency (cut-off 20 ng/mL) against healthy controls. A corrected Cohen’s d of − 0.43 [(− 0.76, − 0.09), P = 0.013] was obtained by trim-and-fill adjustment for publication bias. The association was consistent across Asian and European studies, pediatric and adult population, high- and moderate-quality studies. Near-equatorial latitudes (< 35° N/S, P = 3.4 × 10−4) and moderate-income economy (gross national income (GNI) 1000 < US$ < 12,000, P = 0.012) were associated with more discrepant 25(OH)D concentrations between the groups. Higher latitude (P = 0.0047), and higher mean body mass index (P = 0.006, 10 studies) were associated with smaller Cohen’s d by univariate meta-regression, with evidence of nonlinear moderation by GNI (P = 3.5 × 10−6), and mean serum thyrotropin in affected individuals (P = 0.017, 21 studies).
Conclusion
The present work shows a significant association between circulating 25(OH)D and HT, partly resolves mixed findings by identifying the empirical moderators contributing to overall heterogeneity, and highlights HT patient groups and the conditions under which the association is strongest.


Similar content being viewed by others
References
Pearce EN, Farwell AP, Braverman LE (2003) Thyroiditis. N Engl J Med 348(26):2646–2655
Booth DR, Ding N, Parnell GP, Shahijanian F, Coulter S, Schibeci SD, Atkins AR, Stewart GJ, Evans RM, Downes M, Liddle C (2016) Cistromic and genetic evidence that the vitamin D receptor mediates susceptibility to latitude-dependent autoimmune diseases. Genes Immun 17(4):213–219. https://doi.org/10.1038/gene.2016.12
Zeitelhofer M, Adzemovic MZ, Gomez-Cabrero D, Bergman P, Hochmeister S, N’diaye M, Paulson A, Ruhrmann S, Almgren M, Tegnér JN, Ekström TJ, Guerreiro-Cacais AO, Jagodic M (2017) Functional genomics analysis of vitamin D effects on CD4 + T cells in vivo in experimental autoimmune encephalomyelitis. Proc Natl Acad Sci USA 114(9):E1678–E1687. https://doi.org/10.1073/pnas.1615783114
Dankers W, Colin EM, van Hamburg JP, Lubberts E (2017) Vitamin D in Autoimmunity: molecular Mechanisms and Therapeutic Potential. Front Immunol 7:697. https://doi.org/10.3389/fimmu.2016.00697
Kim D (2017) The role of vitamin D in thyroid diseases. Int J Mol Sci 18(9):E1949. https://doi.org/10.3390/ijms18091949
Nettore IC, Albano L, Ungaro P, Colao A, Macchia PE (2017) Sunshine vitamin and thyroid. Rev Endocr Metab Disord 18(3):347–354. https://doi.org/10.1007/s11154-017-9406-3
Hu S, Rayman MP (2017) Multiple nutritional factors and the risk of Hashimoto’s thyroiditis. Thyroid 27(5):597–610. https://doi.org/10.1089/thy.2016.0635
Wang J, Lv S, Chen G, Gao C, He J, Zhong H, Xu Y (2015) Meta-analysis of the association between vitamin D and autoimmune thyroid disease. Nutrients 7(4):2485–2498. https://doi.org/10.3390/nu7042485
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:135. https://doi.org/10.1186/1471-2288-14-135
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P (2018) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. The Ottawa Hospital Research Institute. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 22 Feb 2018
Wacker M, Holick MF (2013) Sunlight and vitamin D: a global perspective for health. Dermatoendocrinol 5(1):51–108. https://doi.org/10.4161/derm.24494
Grant WB, Bhattoa HP, Pludowski P (2017) Determinants of vitamin D deficiency from sun exposure: a global perspective. In: Feldman D, Pike JW, Bouillon R, Giovannucci E, Goltzman D, Hewison M (eds) Vitamin D: Volume 2: health, disease and therapeutics, 4th edn. Academic Press, London, pp 79–86
Akaike H (1981) Likelihood of a model and information criteria. J Econom 16:3–14
Tamer G, Arik S, Tamer I, Coksert D (2011) Relative vitamin D insufficiency in Hashimoto’s thyroiditis. Thyroid 21(8):891–896. https://doi.org/10.1089/thy.2009.0200
Kivity S, Agmon-Levin N, Zisappl M, Shapira Y, Nagy EV, Dankó K, Szekanecz Z, Langevitz P, Shoenfeld Y (2011) Vitamin D and autoimmune thyroid diseases. Cell Mol Immunol 8(3):243–247. https://doi.org/10.1038/cmi.2010.73
Camurdan OM, Döğer E, Bideci A, Celik N, Cinaz P (2012) Vitamin D status in children with Hashimoto thyroiditis. J Pediatr Endocrinol Metab 25(5–6):467–470
Dellal F, Niyazoglu M, Ademoglu E, Gorar S, Candan Z, Bekdemir H, Uc ZA, Senes M, Ozderya A, Aral Y (2013) Evaluation of Serum trace elements and vitamin levels in Hashimoto’s thyroiditis: single centre experience from Turkey. Open J Endocr Metab Dis 3(4):236–240. https://doi.org/10.4236/ojemd.2013.34031
Bozkurt NC, Karbek B, Ucan B, Sahin M, Cakal E, Ozbek M, Delibasi T (2013) The association between severity of vitamin D deficiency and Hashimoto’s thyroiditis. Endocr Pract 19(3):479–484. https://doi.org/10.4158/EP12376.OR
Mansournia N, Mansournia MA, Saeedi S, Dehghan J (2014) The association between serum 25OHD levels and hypothyroid Hashimoto’s thyroiditis. J Endocrinol Invest 37(5):473–476. https://doi.org/10.1007/s40618-014-0064-y
Botelho I (2014) Prevalence of Vitamin D insufficiency in patients with Hashimoto’s thyroiditis and its relationship with thyroid autoimmunity. Master’s thesis, Faculdade de Ciências Médicas, Universidade Estadual de Campinas Campinas, SP (Brasil). http://repositorio.unicamp.br/handle/REPOSIP/308788. Accessed 23 Sept 2018
Unal AD, Tarcin O, Parildar H, Cigerli O, Eroglu H, Demirag NG (2014) Vitamin D deficiency is related to thyroid antibodies in autoimmune thyroiditis. Cent Eur J Immunol 39(4):493–497. https://doi.org/10.5114/ceji.2014.47735
Ma J, Wu D, Li C, Fan C, Chao N, Liu J, Li Y, Wang R, Miao W, Guan H, Shan Z, Teng W (2015) Lower serum 25-hydroxyvitamin D level is associated with 3 types of autoimmune thyroid diseases. Medicine (Baltimore) 94(39):e1639. https://doi.org/10.1097/MD.0000000000001639
Lizis-Kolus K (2014) Ocena wpływu niedoboru witaminy D na przebieg choroby Hashimoto u chorych w województwie świętokrzyskim. Dissertation, Collegium Medicum, Wydział Lekarski, Uniwersytet Jagielloński, Kraków (Poland). http://dl.cm-uj.krakow.pl:8080/dlibra/docmetadata?id=4036. Accessed 23 Sept 2018
Maciejewski A, Wójcicka M, Roszak M, Losy J, Łącka K (2015) Assessment of vitamin D level in autoimmune thyroiditis patients and a control group in the Polish population. Adv Clin Exp Med 24(5):801–806. https://doi.org/10.17219/acem/29183
Evliyaoğlu O, Acar M, Özcabı B, Erginöz E, Bucak F, Ercan O, Kucur M (2015) Vitamin D deficiency and Hashimoto’s thyroiditis in children and adolescents: a critical vitamin D level for this Association? J Clin Res Pediatr Endocrinol 7(2):128–133. https://doi.org/10.4274/jcrpe.2011
Şıklar Z, Karataş D, Doğu F, Hacıhamdioğlu B, İkincioğulları A, Berberoğlu M (2016) Regulatory T cells and vitamin D status in children with chronic autoimmune thyroiditis. J Clin Res Pediatr Endocrinol 8(3):276–281. https://doi.org/10.4274/jcrpe.2766
Yasmeh J, Farpour F, Rizzo V, Kheradnam S, Sachmechi I (2016) Hashimoto thyroiditis not associated with vitamin D deficiency. Endocr Pract 22(7):809–813. https://doi.org/10.4158/EP15934.OR
Prasad I, Kumari R, Saran A (2016) Vitamin D evaluation in autoimmune thyroid diseases. Int J Contemp Med Res 3(12):3415–3418
Guleryuz B, Akin F, Ata MT, Dalyanoglu MM, Turgut S (2016) Vitamin-D receptor (VDR) gene polymorphisms (TaqI, FokI) in Turkish patients with Hashimoto’s thyroiditis: relationship to the levels of Vit-D and cytokines. Endocr Metab Immune Disord Drug Targets 16(2):131–139. https://doi.org/10.2174/1871530316666160728092613
Sönmezgöz E, Ozer S, Yilmaz R, Önder Y, Bütün I, Bilge S (2016) Hypovitaminosis D in children with Hashimoto’s thyroiditis. Rev Med Chil 144(5):611–616. https://doi.org/10.4067/S0034-98872016000500009
Metwalley KA, Farghaly HS, Sherief T, Hussein A (2016) Vitamin D status in children and adolescents with autoimmune thyroiditis. J Endocrinol Invest 39(7):793–797. https://doi.org/10.1007/s40618-016-0432-x
Kim D (2016) Low vitamin D status is associated with hypothyroid Hashimoto’s thyroiditis. Hormones (Athens) 15(3):385–393. https://doi.org/10.14310/horm.2002.1681
Priya R, Kalra P, Vashuda KC (2016) Autoimmune hypothyroidism and vitamin D levels. J Med Sci Clin Res 4(2):9453–9457. https://doi.org/10.18535/jmscr/v4i02.57
Giovinazzo S, Vicchio TM, Certo R, Alibrandi A, Palmieri O, Campennì A, Cannavò S, Trimarchi F, Ruggeri RM (2017) Vitamin D receptor gene polymorphisms/haplotypes and serum 25(OH)D(3) levels in Hashimoto’s thyroiditis. Endocrine 55(2):599–606. https://doi.org/10.1007/s12020-016-0942-5
Ke W, Sun T, Zhang Y, He L, Wu Q, Liu J, Zha B (2017) 25-hydroxyvitamin D serum level in Hashimoto’s thyroiditis, but not Graves’ disease is relatively deficient. Endocr J 64(6):581–587. https://doi.org/10.1507/endocrj.EJ16-0547
Nalbant A, Gokosmanoglu F, Cinemre H, Varim C, Kaya T, Ergenc H (2017) The relation between serum vitamin D levels and Hashimoto thyroiditis in women. Kuwait Med J 49:223–226
Yavuzer H, Işık S, Cengiz M, Bolayırlı IM, Döventaş A, Erdinçler DS (2017) The relationship between vitamin D levels and receptor activator of nuclear factor ligand in Hashimoto’s thyroiditis. Med Bull Haseki 55:261–268
Rezaee H, Najafipour F, Ranjdoust F, Sadra V, Hamishekar H, Najafipour M, Zareizadeh J, Janipour M (2017) Evaluation of serum vitamin D levels in patients with Hashimoto’s thyroiditis. Int J Adv Biotechnol Res 8:890–895
Perga S, Martire S, Montarolo F, Giordani I, Spadaro M, Bono G, Corvisieri S, Messuti I, Panzica G, Orlandi F, Bertolotto A (2018) The footprints of poly-autoimmunity: evidence for common biological factors involved in multiple sclerosis and Hashimoto’s thyroiditis. Front Immunol 9:311. https://doi.org/10.3389/fimmu.2018.00311
Viechtbauer W, Cheung MW (2010) Outlier and influence diagnostics for meta-analysis. Res Synth Methods 1(2):112–125. https://doi.org/10.1002/jrsm.11
Pilz S, März W, Cashman KD, Kiely ME, Whiting SJ, Holick MF et al (2018) Rationale and plan for vitamin D food fortification: a review and guidance paper. Front Endocrinol (Lausanne) 9:373. https://doi.org/10.3389/fendo.2018.00373
Jeffery LE, Raza K, Hewison M (2016) Vitamin D in rheumatoid arthritis-towards clinical application. Nat Rev Rheumatol 12(4):201–210. https://doi.org/10.1038/nrrheum.2015.140
Edwards MH, Cole ZA, Harvey NC, Cooper C (2014) The global epidemiology of vitamin D status. J Aging Res Clin Pract 3(3):148–158
Kimlin MG, Lucas RM, Harrison SL, van der Mei I, Armstrong BK, Whiteman DC, Kricker A, Nowak M, Brodie AM, Sun J (2014) The contributions of solar ultraviolet radiation exposure and other determinants to serum 25-hydroxyvitamin D concentrations in Australian adults: the AusD Study. Am J Epidemiol 179(7):864–874. https://doi.org/10.1093/aje/kwt446
Nimitphong H, Holick MF (2013) Vitamin D status and sun exposure in southeast Asia. Dermatoendocrinol 5(1):34–37. https://doi.org/10.4161/derm.24054
Jungert A, Spinneker A, Nagel A, Neuhäuser-Berthold M (2014) Dietary intake and main food sources of vitamin D as a function of age, sex, vitamin D status, body composition, and income in an elderly German cohort. Food Nutr Res 58:23632. https://doi.org/10.3402/fnr.v58.23632
Rabenberg M, Scheidt-Nave C, Busch MA, Rieckmann N, Hintzpeter B, Mensink GB (2015) Vitamin D status among adults in Germany–results from the German Health Interview and Examination Survey for Adults (DEGS1). BMC Public Health 15:641. https://doi.org/10.1186/s12889-015-2016-7
Moore CE, Radcliffe JD, Liu Y (2014) Vitamin D intakes of adults differ by income, gender and race/ethnicity in the U.S.A., 2007 to 2010. Public Health Nutr 17(4):756–763. https://doi.org/10.1017/S1368980013002929
Arabi A, El Rassi R, El-Hajj Fuleihan G (2010) Hypovitaminosis D in developing countries-prevalence, risk factors and outcomes. Nat Rev Endocrinol 6(10):550–561. https://doi.org/10.1038/nrendo.2010.146
Novaković R, Cavelaars A, Geelen A, Nikolić M, Altaba II, Viñas BR, Ngo J, Golsorkhi M, Medina MW, Brzozowska A, Szczecinska A, de Cock D, Vansant G, Renkema M, Majem LS, Moreno LA, Glibetić M, Gurinović M, van’t Veer P, de Groot LC (2014) Socio-economic determinants of micronutrient intake and status in Europe: a systematic review. Public Health Nutr 17(5):1031–1045. https://doi.org/10.1017/S1368980013001341
Moore CE, Radcliffe JD, Liu Y (2014) Vitamin D intakes of children differ by race/ethnicity, sex, age, and income in the United States, 2007 to 2010. Nutr Res 34(6):499–506. https://doi.org/10.1016/j.nutres.2014.06.002
Voortman T, van den Hooven EH, Heijboer AC, Hofman A, Jaddoe VW, Franco OH (2015) Vitamin D deficiency in school-age children is associated with sociodemographic and lifestyle factors. J Nutr 145(4):791–798. https://doi.org/10.3945/jn.114.208280
Darmon N, Drewnowski A (2008) Does social class predict diet quality? Am J Clin Nutr 87(5):1107–1117
Chaudhary A, Gustafson D, Mathys A (2018) Multi-indicator sustainability assessment of global food systems. Nat Commun 9(1):848. https://doi.org/10.1038/s41467-018-03308-7
Cashman KD, Sheehy T, O’Neill CM (2018) Is vitamin D deficiency a public health concern for low middle income countries? A systematic literature review. Eur J Nutr 58(1):433–453. https://doi.org/10.1007/s00394-018-1607-3
Sørensen TH, Olsen KR, Vedsted P (2009) Association between general practice referral rates and patients’ socioeconomic status and access to specialized health care a population-based nationwide study. Health Policy 92(2–3):180–186. https://doi.org/10.1016/j.healthpol.2009.03.011
Hansen RP, Olesen F, Sørensen HT, Sokolowski I, Søndergaard J (2008) Socioeconomic patient characteristics predict delay in cancer diagnosis: a Danish cohort study. BMC Health Serv Res 8:49. https://doi.org/10.1186/1472-6963-8-49
Beedasy J (2010) Rural designations and geographic access to tertiary healthcare in Idaho. Online J Rural Res Policy 5(2):1–21. https://doi.org/10.4148/ojrrp.v5i2.191
Hauch A, Al-Qurayshi Z, Friedlander P, Kandil E (2014) Association of socioeconomic status, race, and ethnicity with outcomes of patients undergoing thyroid surgery. JAMA Otolaryngol Head Neck Surg 140(12):1173–1183. https://doi.org/10.1001/jamaoto.2014.1745
Taylor PN, Iqbal A, Minassian C, Sayers A, Draman MS, Greenwood R, Hamilton W, Okosieme O, Panicker V, Thomas SL, Dayan C (2014) Falling threshold for treatment of borderline elevated thyrotropin levels-balancing benefits and risks: evidence from a large community-based study. JAMA Intern Med 174(1):32–39. https://doi.org/10.1001/jamainternmed.2013.11312
Mammen JS, McGready J, Oxman R, Chia CW, Ladenson PW, Simonsick EM (2015) Thyroid hormone therapy and risk of thyrotoxicosis in community-resident older adults: findings from the Baltimore longitudinal study of aging. Thyroid 25(9):979–986. https://doi.org/10.1089/thy.2015.0180
Somwaru LL, Arnold AM, Cappola AR (2011) Predictors of thyroid hormone initiation in older adults: results from the cardiovascular health study. J Gerontol A Biol Sci Med Sci 66(7):809–814. https://doi.org/10.1093/gerona/glr063
Olmos RD, Figueiredo RC, Aquino EM, Lotufo PA, Bensenor IM (2015) Gender, race and socioeconomic influence on diagnosis and treatment of thyroid disorders in the Brazilian Longitudinal Study of Adult Health (ELSA-Brasil). Braz J Med Biol Res 48(8):751–758. https://doi.org/10.1590/1414-431X20154445
Thvilum M, Brandt F, Brix TH, Hegedüs L (2014) Hypothyroidism is a predictor of disability pension and loss of labor market income: a Danish register-based study. J Clin Endocrinol Metab 99(9):3129–3135. https://doi.org/10.1210/jc.2014-1407
Ott J, Promberger R, Kober F, Neuhold N, Tea M, Huber JC, Hermann M (2011) Hashimoto’s thyroiditis affects symptom load and quality of life unrelated to hypothyroidism: a prospective case-control study in women undergoing thyroidectomy for benign goiter. Thyroid 21(2):161–167. https://doi.org/10.1089/thy.2010.0191
Rhee CM, Chen Y, You AS, Brunelli SM, Kovesdy CP, Budoff MJ, Brent GA, Kalantar-Zadeh K, Nguyen DV (2017) Thyroid status, quality of life, and mental health in patients on hemodialysis. Clin J Am Soc Nephrol 12(8):1274–1283. https://doi.org/10.2215/CJN.13211216
Samuels MH (2014) Psychiatric and cognitive manifestations of hypothyroidism. Curr Opin Endocrinol Diabetes Obes 21(5):377–383. https://doi.org/10.1097/MED.0000000000000089
Vigário Pdos S, Vaisman F, Coeli CM, Ward L, Graf H, Carvalho G, Júnior RM, Vaisman M (2013) Inadequate levothyroxine replacement for primary hypothyroidism is associated with poor health-related quality of life-a Brazilian multicentre study. Endocrine 44(2):434–440. https://doi.org/10.1007/s12020-013-9886-1
Lillevang-Johansen M, Abrahamsen B, Jørgensen HL, Brix TH, Hegedüs L (2018) Over- and under-treatment of hypothyroidism is associated with excess mortality: a register-based cohort study. Thyroid 28(5):566–574. https://doi.org/10.1089/thy.2017.0517
Thvilum M, Brandt F, Almind D, Christensen K, Brix TH, Hegedüs L (2013) Type and extent of somatic morbidity before and after the diagnosis of hypothyroidism. A nationwide register study. PLoS ONE 8(9):e75789. https://doi.org/10.1371/journal.pone.0075789
Feller M, Snel M, Moutzouri E, Bauer DC, de Montmollin M, Aujesky D, Ford I, Gussekloo J, Kearney PM, Mooijaart S, Quinn T, Stott D, Westendorp R, Rodondi N, Dekkers OM (2018) Association of thyroid hormone therapy with quality of life and thyroid-related symptoms in patients with subclinical hypothyroidism: a systematic review and meta-analysis. JAMA 320(13):1349–1359. https://doi.org/10.1001/jama.2018.13770
Klaver EI, van Loon HC, Stienstra R, Links TP, Keers JC, Kema IP, Kobold AC, van der Klauw MM, Wolffenbuttel BH (2013) Thyroid hormone status and health-related quality of life in the LifeLines Cohort Study. Thyroid 23(9):1066–1073. https://doi.org/10.1089/thy.2013.0017
Ovesen L, Andersen R, Jakobsen J (2003) Geographical differences in vitamin D status, with particular reference to European countries. Proc Nutr Soc 62(4):813–821
Johnson LK, Hofsø D, Aasheim ET, Tanbo T, Holven KB, Andersen LF, Røislien J, Hjelmesæth J (2012) Impact of gender on vitamin D deficiency in morbidly obese patients: a cross-sectional study. Eur J Clin Nutr 66(1):83–90. https://doi.org/10.1038/ejcn.2011.140
Poomthavorn P, Saowan S, Mahachoklertwattana P, Chailurkit L, Khlairit P (2012) Vitamin D status and glucose homeostasis in obese children and adolescents living in the tropics. Int J Obes (Lond) 36(4):491–495. https://doi.org/10.1038/ijo.2011.260
Saneei P, Salehi-Abargouei A, Esmaillzadeh A (2013) Serum 25-hydroxy vitamin D levels in relation to body mass index: a systematic review and meta-analysis. Obes Rev 14(5):393–404. https://doi.org/10.1111/obr.12016
Ahern T, Khattak A, O’Malley E, Dunlevy C, Kilbane M, Woods C, McKenna MJ, O’Shea D (2014) Association between vitamin D status and physical function in the severely obese. J Clin Endocrinol Metab 99(7):E1327–E1331. https://doi.org/10.1210/jc.2014-1704
Pourshahidi LK (2015) Vitamin D and obesity: current perspectives and future directions. Proc Nutr Soc 74(2):115–124. https://doi.org/10.1017/S0029665114001578
Knudsen N, Laurberg P, Rasmussen LB, Bülow I, Perrild H, Ovesen L, Jørgensen T (2005) Small differences in thyroid function may be important for body mass index and the occurrence of obesity in the population. J Clin Endocrinol Metab 90(7):4019–4024
Bhaskaran K, Dos-Santos-Silva I, Leon DA, Douglas IJ, Smeeth L (2018) Association of BMI with overall and cause-specific mortality: a population-based cohort study of 3·6 million adults in the UK. Lancet Diabetes Endocrinol 6(12):944–953. https://doi.org/10.1016/S2213-8587(18)30288-2
Wang S, Wu Y, Zuo Z, Zhao Y, Wang K (2018) The effect of vitamin D supplementation on thyroid autoantibody levels in the treatment of autoimmune thyroiditis: a systematic review and a meta-analysis. Endocrine 59(3):499–505. https://doi.org/10.1007/s12020-018-1532-5
Major JM, Graubard BI, Dodd KW, Iwan A, Alexander BH, Linet MS, Freedman DM (2013) Variability and reproducibility of circulating vitamin D in a nationwide U.S. population. J Clin Endocrinol Metab 98(1):97–104. https://doi.org/10.1210/jc.2012-2643
Gail MH, Wu J, Wang M, Yaun SS, Cook NR, Eliassen AH, McCullough ML, Yu K, Zeleniuch-Jacquotte A, Smith-Warner SA, Ziegler RG, Carroll RJ (2016) Calibration and seasonal adjustment for matched case-control studies of vitamin D and cancer. Stat Med 35(13):2133–2148. https://doi.org/10.1002/sim.6856
Jiang X, O’Reilly PF, Aschard H, Hsu YH, Richards JB, Dupuis J et al (2018) Genome-wide association study in 79,366 European-ancestry individuals informs the genetic architecture of 25-hydroxyvitamin D levels. Nat Commun 9(1):260. https://doi.org/10.1038/s41467-017-02662-2
Black LJ, Seamans KM, Cashman KD, Kiely M (2012) An updated systematic review and meta-analysis of the efficacy of vitamin D food fortification. J Nutr 142(6):1102–1108. https://doi.org/10.3945/jn.112.158014
Enko D, Fridrich L, Rezanka E, Stolba R, Ernst J, Wendler I, Fabian D, Hauptlorenz S, Halwachs-Baumann G (2014) 25-hydroxy-vitamin D status: limitations in comparison and clinical interpretation of serum-levels across different assay methods. Clin Lab 60(9):1541–1550
Lips P, Chapuy MC, Dawson-Hughes B, Pols HA, Holick MF (1999) An international comparison of serum 25-hydroxyvitamin D measurements. Osteoporos Int 9(5):394–397
Jones G (2015) Interpreting vitamin D assay results: proceed with caution. Clin J Am Soc Nephrol 10(2):331–334. https://doi.org/10.2215/CJN.05490614
Black LJ, Anderson D, Clarke MW, Ponsonby AL, Lucas RM, Autoimmune Investigator Group (2015) Analytical bias in the measurement of serum 25-hydroxyvitamin D concentrations impairs assessment of vitamin D status in clinical and research settings. PLoS ONE 10(8):e0135478. https://doi.org/10.1371/journal.pone.0135478
Acknowledgements
This work was supported by Josip Juraj Strossmayer University of Osijek (Grant No. VIF2016MEFOS-37).
Author information
Authors and Affiliations
Contributions
MS designed the research, analyzed the data, and performed the statistical analysis; MS and ST conducted the research and interpreted the results. Both authors provided critical revisions of the systematic review and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Štefanić, M., Tokić, S. Serum 25-hydoxyvitamin D concentrations in relation to Hashimoto’s thyroiditis: a systematic review, meta-analysis and meta-regression of observational studies. Eur J Nutr 59, 859–872 (2020). https://doi.org/10.1007/s00394-019-01991-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-019-01991-w