Abstract
Purpose
This study examined the association of free sugar (FS) intake with obesity measures and blood pressure (BP) among a nationally representative sample of Australian adults.
Methods
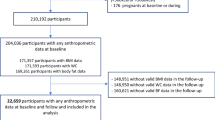
Data from adults (weighted n = 5136) who completed 2 × 24-h recalls and had complete data for BP, waist circumference (WC), waist-to-height ratio (WHtR), and body mass index (BMI) were analyzed. Associations between percentage energy of FS from all food sources (%EFStotal), beverages only (%EFSbeverages), and non-beverages sources only (%EFSnon-beverages) and obesity measures and BP were examined using linear and non-linear regressions. Logistic regression was used to calculate the odds ratios (OR) of being classified as overweight and/or obese, having increased cardiometabolic risks, and elevated BP per 5% point increase in %EFStotal, %EFSbeverages, and %EFSnon-beverages. All regression analyses were adjusted for known socio-economic and lifestyle confounders.
Results
%EFSbeverage was positively associated with BMI, WC, and WHtR (all p < 0.05), while %EFSnon-beverage was inversely associated with these outcomes. Increases in odds of having an undesirable WC/WHtR were found with increasing %EFSbeverages (OR per 5% point increase in %EFSbeverages: 1.19 for WC; 1.23 for WHtR, both p < 0.001). %EFStotal and %EFSnon-beverages were weakly and negatively associated with diastolic BP. A 5% point increase in %EFStotal and %EFSnon-beverage was associated with a 10–25% reduction in odds of having elevated BP.
Conclusions
Our results suggested that only a higher FS intake from beverages may be associated with obesity, and higher FS intake was associated with reduced odds of having elevated BP.
Similar content being viewed by others
References
World Health Organization (2015) Guideline: sugars intake for adults and children. World Health Organization, Geneva
Cobiac L, Record S, Leppard P, Syrette J, Flight I (2003) Sugars in the Australian diet: results from the 1995 National Nutrition Survey. Nutr Diet 60(3):152–173
Louie JCY, Moshtaghian H, Rangan AM, Flood VM, Gill TP (2016) Intake and sources of added sugars among Australian children and adolescents. Eur J Nutr 55(8):2347–2355. https://doi.org/10.1007/s00394-015-1041-8
Lei L, Rangan AM, Flood VM, Louie JCY (2016) Dietary intake and food sources of added sugar in the Australian population. Br J Nutr 115(5):868–877
Luger M, Lafontan M, Bes-Rastrollo M et al (2018) Sugar-sweetened beverages and weight gain in children and adults: a systematic review from 2013 to 2015 and a comparison with previous studies. Obes Facts 10(6):674–693. https://doi.org/10.1159/000484566
Te Morenga L, Mallard S, Mann J (2013) Dietary sugars and body weight: systematic review and meta-analyses of randomised controlled trials and cohort studies. BMJ 346:e7492. https://doi.org/10.1136/bmj.e7492
Te Morenga LA, Howatson AJ, Jones RM, Mann J (2014) Dietary sugars and cardiometabolic risk: systematic review and meta-analyses of randomized controlled trials of the effects on blood pressure and lipids. Am J Clin Nutr 100(1):65–79. https://doi.org/10.3945/ajcn.113.081521
Jayalath VH, de Souza RJ, Ha V et al (2015) Sugar-sweetened beverage consumption and incident hypertension: a systematic review and meta-analysis of prospective cohorts. Am J Clin Nutr 102(4):914–921. https://doi.org/10.3945/ajcn.115.107243
Chen L, Appel LJ, Loria C et al (2009) Reduction in consumption of sugar-sweetened beverages is associated with weight loss: the PREMIER trial. Am J Clin Nutr 89(5):1299–1306
DiMeglio DP, Mattes RD (2000) Liquid versus solid carbohydrate: effects on food intake and body weight. Int J Obes 24(6):794–800
Australian Bureau of Statistics (2014) Australian Health Survey, 2011–13. ABS, Canberra
Australian Bureau of Statistics (2014) Australian health survey: users’ guide, 2011–13. Australian Bureau of Statistics, Canberra
Commonwealth Government of Australia (2016) Census and statistics act 1905. Federal Register of Legislation, Canberra
Bliss R (2004) Researchers produce innovation in dietary recall. Agric Res 52(6):10–12
Australian Bureau of Statistics (2013) Australian Health Survey: Users’ Guide, 2011–2013. http://www.abs.gov.au/ausstats/abs@.nsf/Lookup/74D87E30B3539C53CA257BBB0014BB36?opendocument. Accessed 2 Jun 2015
Food Standards Australia New Zealand (2014) AUTNUT 2011–13 food composition database
Louie JCY, Lei L, Rangan AM (2016) Reliability of a systematic methodology to estimate added sugars content of foods when applied to a recent Australian food composition database. J Food Comp Anal 46:36–42. https://doi.org/10.1016/j.jfca.2015.11.002
Louie JC, Moshtaghian H, Boylan S et al (2015) A systematic methodology to estimate added sugar content of foods. Eur J Clin Nutr 69(2):154–161. https://doi.org/10.1038/ejcn.2014.256
Australian Buread of Statistics (2013) 4363.0.55.001 - Australian Health Survey: Users’ Guide, 2011–2013—BODY MASS AND PHYSICAL MEASUREMENTS. Australia Bureau of Statistics. http://www.abs.gov.au/ausstats/abs@.nsf/Lookup/9C2B28A7F682FD6FCA257B8D00229E9B?opendocument. Accessed 19 Jul 2018
Cole TJ, Bellizzi MC, Flegal KM, Dietz WH (2000) Establishing a standard definition for child overweight and obesity worldwide: international survey. BMJ 320(7244):1240
Cole TJ, Flegal KM, Nicholls D, Jackson AA (2007) Body mass index cut offs to define thinness in children and adolescents: international survey. BMJ 335(7612):194
World Health Organisation (2006) BMI classification. WHO, Geneva
Ashwell M, Gunn P, Gibson S (2012) Waist-to-height ratio is a better screening tool than waist circumference and BMI for adult cardiometabolic risk factors: systematic review and meta-analysis. Obes Rev 13(3):275–286
World Health Organization (2000) Obesity: preventing and managing the global epidemic, vol 894. World Health Organization, Geneva
Stergiou G, Palatini P, Asmar R et al (2018) Blood pressure measurement and hypertension diagnosis in the 2017 US guidelines: first things first. Hypertension 71(6):963–965. https://doi.org/10.1161/hypertensionaha.118.10853
Australian Government Department of Health (2015) ASGC remoteness areas. Australian Government Department of Health, Australia
Harttig U, Haubrock J, Knuppel S, Boeing H (2011) The MSM program: web-based statistics package for estimating usual dietary intake using the multiple source method. Eur J Clin Nutr 65(Suppl 1):S87–S91. https://doi.org/10.1038/ejcn.2011.92
Mok A, Ahmad R, Rangan A, Louie JCY (2018) Intake of free sugars and micronutrient dilution in Australian adults. Am J Clin Nutr 107(1):94–104. https://doi.org/10.1093/ajcn/nqx008
Goldberg G, Black A, Jebb S et al (1991) Critical evaluation of energy intake data using fundamental principles of energy physiology: 1. Derivation of cut-off limits to identify under-recording. Eur J Clin Nutr 45(12):569–581
Louie JCY, Buyken AE, Heyer K, Flood VM (2011) Dietary glycaemic index and glycaemic load among Australian children and adolescents. Br J Nutr 106(08):1273–1282. https://doi.org/10.1017/S0007114511001577
Tornaritis MJ, Philippou E, Hadjigeorgiou C et al (2014) A study of the dietary intake of Cypriot children and adolescents aged 6–18 years and the association of mother’s educational status and children’s weight status on adherence to nutritional recommendations. BMC Public Health 14:13. https://doi.org/10.1186/1471-2458-14-13
Ferrari P, Slimani N, Ciampi A et al (2002) Evaluation of under- and overreporting of energy intake in the 24-hour diet recalls in the European Prospective Investigation into Cancer and Nutrition (EPIC). Public Health Nutr 5(6B):1329–1345. https://doi.org/10.1079/PHN2002409
Wong THT, Louie JCY (2018) The direct and indirect associations of usual free sugar intake on BMI z-scores of Australian children and adolescents. Eur J Clin Nutr 72(7):1058–1060. https://doi.org/10.1038/s41430-018-0124-z
Pan A, Hu FB (2011) Effects of carbohydrates on satiety: differences between liquid and solid food. Curr Opin Clin Nutr Metab Care 14(4):385–390
Zheng M, Allman-Farinelli M, Heitmann BL et al (2015) Liquid versus solid energy intake in relation to body composition among Australian children. J Hum Nutr Diet 28(s2):70–79. https://doi.org/10.1111/jhn.12223 doi
Haber G, Heaton K, Murphy D, Burroughs L (1977) Depletion and disruption of dietary fibre: effects on satiety, plasma-glucose, and serum-insulin. Lancet 310(8040):679–682
Teff KL, Devine J, Engelman K (1995) Sweet taste: effect on cephalic phase insulin release in men. Physiol Behav 57(6):1089–1095
Malik AH, Akram Y, Shetty S, Malik SS, Njike VY (2014) Impact of sugar-sweetened beverages on blood pressure. Am J Cardiol 113(9):1574–1580
Probst YC, Dengate A, Jacobs J, Louie JC, Dunford EK (2017) The major types of added sugars and non-nutritive sweeteners in a sample of Australian packaged foods. Public Health Nutr 20(18):3228–3233. https://doi.org/10.1017/S136898001700218X
He FJ, MacGregor GA (2014) Salt intake, sugar-sweetened soft drink consumption, and blood pressure. Am J Cardiol 114(3):499
Santos JA, Webster J, Land M-A et al (2017) Dietary salt intake in the Australian population. Public Health Nutr 20(11):1887–1894. https://doi.org/10.1017/S1368980017000799
Burki TK (2016) Sugar tax in the UK. Lancet Oncol 17(5):e182. https://doi.org/10.1016/S1470-2045(16)30021-3
Vecino-Ortiz AI, Arroyo-Ariza D (2018) A tax on sugar sweetened beverages in Colombia: estimating the impact on overweight and obesity prevalence across socio economic levels. Soc Sci Med 209:111–116. https://doi.org/10.1016/j.socscimed.2018.05.043
Nakamura R, Mirelman AJ, Cuadrado C et al (2018) Evaluating the 2014 sugar-sweetened beverage tax in Chile: an observational study in urban areas. PLoS Med 15(7):e1002596. https://doi.org/10.1371/journal.pmed.1002596
Long MW, Gortmaker SL, Ward ZJ et al (2015) Cost effectiveness of a sugar-sweetened beverage excise tax in the US. Am J Prev Med 49(1):112–123. https://doi.org/10.1016/j.amepre.2015.03.004
Australian Bureau of Statistics (2015) Consumption of sweetened beverages. Australian Bureau of Statistics, Canberra
Malik VS, Pan A, Willett WC, Hu FB (2013) Sugar-sweetened beverages and weight gain in children and adults: a systematic review and meta-analysis. Am J Clin Nutr 98(4):1084–1102
de Ruyter JC, Olthof MR, Seidell JC, Katan MB (2012) A trial of sugar-free or sugar-sweetened beverages and body weight in children. New Eng J Med 367(15):1397–1406
National Cancer Institute (2015) Dietary assessment primer. Summary tables: recommendations on potential approaches to dietary assessment for different research objectives requiring group-level estimates. http://dietassessmentprimer.cancer.gov/approach/table.html. Accessed 21 May 2015
Subar AF, Freedman LS, Tooze JA et al (2015) Addressing current criticism regarding the value of self-report dietary data. J Nutr 145(12):2639–2645. https://doi.org/10.3945/jn.115.219634
Tasevska N (2015) Urinary sugars—a biomarker of total sugars intake. Nutrients 7(7):5255
Liu SV, Moore LB, Halliday TM et al (2018) Short-term changes in added sugar consumption by adolescents reflected in the carbon isotope ratio of fingerstick blood. Nutr Health 24(4):251–259. https://doi.org/10.1177/0260106018799522
Beasley JM, Jung M, Tasevska N et al (2016) Biomarker-predicted sugars intake compared with self-reported measures in US Hispanics/Latinos: results from the HCHS/SOL SOLNAS study. Public Health Nutr 19(18):3256–3264. https://doi.org/10.1017/S1368980016001580
Campbell R, Tasevska N, Jackson KG et al (2017) Association between urinary biomarkers of total sugars intake and measures of obesity in a cross-sectional study. PLoS One 12(7):e0179508. https://doi.org/10.1371/journal.pone.0179508
Tasevska N, Pettinger M, Kipnis V et al (2018) Associations of biomarker-calibrated intake of total sugars with the risk of Type 2 diabetes and cardiovascular disease in the Women’s Health Initiative Observational study. Am J Epidemiol 187(10):2126–2135. https://doi.org/10.1093/aje/kwy115
Acknowledgements
We would like to acknowledge that the original data of 2011-12 National Nutrition and Physical Activity Survey were collected by the Australian Bureau of Statistics. The authors declare that those who carried out the original analysis and collection of data bear no responsibility for further analysis and interpretation.
Author information
Authors and Affiliations
Contributions
The authors’ responsibilities were as follows—JCYL and AR: jointly designed, supervised, and guided the study. RA: coded foods in the AUSNUT2012-13 database as beverages and non-beverages. RA, JCYL, and AM: involved in calculating usual intake of nutrients. RA and JCYL: analyzed the data. RA: wrote the first draft of the manuscript. AM, RA, JCYL, and AR: interpretation of data, contributed to the discussion, and critically reviewed the final manuscript. JCYL had primary responsibility for the final content.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare they have no conflicts of interest. No specific funding was received from any agency in the public, commercial, or not-for-profit sectors.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ahmad, R., Mok, A., Rangan, A.M. et al. Association of free sugar intake with blood pressure and obesity measures in Australian adults. Eur J Nutr 59, 651–659 (2020). https://doi.org/10.1007/s00394-019-01932-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-019-01932-7