Abstract
Purpose
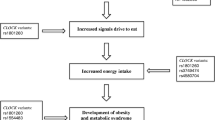
A common variant of the melatonin receptor 1B (MTNR1B) gene has been related to increased signaling of melatonin, a hormone previously associated with body fatness mainly through effects on energy metabolism. We examined whether the MTNR1B variant affects changes of body fatness and composition in response to a dietary weight loss intervention.
Methods
The MTNR1B rs10830963 variant was genotyped for 722 overweight and obese individuals, who were randomly assigned to one of four diets varying in macronutrient composition. Anthropometric and body composition measurements (DXA scan) were collected at baseline and at 6 and 24 months of follow-up.
Results
Statistically significant interactions were observed between the MTNR1B genotype and low-/high-fat diet on changes in weight, body mass index (BMI), waist circumference (WC) and total body fat (p interaction = 0.01, 0.02, 0.002 and 0.04, respectively), at 6 months of dietary intervention. In the low-fat diet group, increasing number of the sleep disruption-related G allele was significantly associated with a decrease in weight (p = 0.004), BMI (p = 0.005) and WC (p = 0.001). In the high-fat diet group, carrying the G allele was positively associated with changes in body fat (p = 0.03). At 2 years, the associations remained statistically significant for changes in body weight (p = 0.02), BMI (p = 0.02) and WC (p = 0.048) in the low-fat diet group, although the gene–diet interaction became less significant.
Conclusions
The results suggest that carriers of the G allele of the MTNR1B rs10830963 may have a greater improvement in body adiposity and fat distribution when eating a low-fat diet.


Similar content being viewed by others
References
Laermans J, Depoortere I (2016) Chronobesity: role of the circadian system in the obesity epidemic. Obes Rev 17:108–125. https://doi.org/10.1111/obr.12351
Garaulet M, Ordovás JM, Madrid JA (2010) The chronobiology, etiology and pathophysiology of obesity. Int J Obes (Lond) 34:1667–1683. https://doi.org/10.1038/ijo.2010.118
Qian J, Scheer FAJL. (2016) Circadian system and glucose metabolism: implications for physiology and disease. Trends Endocrinol Metab 27:282–293. https://doi.org/10.1016/j.tem.2016.03.005
Scott EM (2015) Circadian clocks, obesity and cardiometabolic function. Diabetes Obes Metab 17:84–89. https://doi.org/10.1111/dom.12518
Cipolla-Neto J, Amaral FG, Afeche SC et al (2014) Melatonin, energy metabolism, and obesity: a review. J Pineal Res 56:371–381. https://doi.org/10.1111/jpi.12137
Dubocovich ML, Delagrange P, Krause DN et al (2010) Nomenclature, classification, and pharmacology of G protein-coupled melatonin receptors. Pharmocological Rev 62:343–380. https://doi.org/10.1124/pr.110.002832.343
Gamble KL, Berry R, Frank SJ, Young ME (2014) Circadian clock control of endocrine factors. Nat Rev Endocrinol 10:466–475. https://doi.org/10.1038/nrendo.2014.78
Prokopenko I, Langenberg C, Florez JC et al (2009) Variants in MTNR1B influence fasting glucose levels. Nat Genet 41:77–81. https://doi.org/10.1038/ng.290
Manning AK, Hivert M-F, Scott RA et al (2012) A genome-wide approach accounting for body mass index identifies genetic variants influencing fasting glycemic traits and insulin resistance. Nat Genet 44:659–669. https://doi.org/10.1038/ng.2274
Gaulton KJ, Ferreira T, Lee Y et al (2015) Genetic fine mapping and genomic annotation defines causal mechanisms at type 2 diabetes susceptibility loci. Nat Genet 47:1415–1425. https://doi.org/10.1038/ng.3437
Tuomi T, Nagorny CLF, Singh P et al (2016) Increased melatonin signaling is a risk factor for type 2 diabetes. Cell Metab 23:1067–1077. https://doi.org/10.1016/j.cmet.2016.04.009
Stancáková A, Kuulasmaa T, Paananen J et al (2009) Association of 18 confirmed susceptibility loci for type 2 diabetes with indices of insulin release, proinsulin conversion, and insulin sensitivity in 5,327 nondiabetic Finnish men. Diabetes 58:2129–2136
Kong X, Zhang X, Xing X et al (2015) The association of type 2 diabetes loci identified in genome-wide association studies with metabolic syndrome and its components in a Chinese population with type 2 diabetes. PLoS One 10:1–21. https://doi.org/10.1371/journal.pone.0143607
Grotenfelt NE, Wasenius NS, Rönö K et al (2016) Interaction between rs10830963 polymorphism in MTNR1B and lifestyle intervention on occurrence of gestational diabetes. Diabetologia 59:1655–1658. https://doi.org/10.1007/s00125-016-3989-1
Goni L, Cuervo M, Milagro FI, Martínez JA (2014) Gene-gene interplay and gene–diet interactions involving the MTNR1B rs10830963 variant with body weight loss. J Nutrigenet Nutrigenomics 7:232–242. https://doi.org/10.1159/000380951
Szewczyk-Golec K, Woźniak A, Reiter RJ (2015) Inter-relationships of the chronobiotic, melatonin, with leptin and adiponectin: implications for obesity. J Pineal Res 59:277–291. https://doi.org/10.1111/jpi.12257
Barrenetxe J, Delagrange P, Martínez JA (2004) Physiological and metabolic functions of melatonin. J Physiol Biochem 60:61–72
Sacks FM, Bray GA, Carey VJ et al (2009) Comparison of weight-loss diets with different compositions of fat, protein, and carbohydrates. N Engl J Med 360:859–873. https://doi.org/10.1056/NEJMoa1208410
Mirzaei K, Xu M, Qi Q et al (2014) Variants in glucose- and circadian rhythm-related genes affect the response of energy expenditure to weight-loss diets: the POUNDS LOST Trial. Am J Clin Nutr 99:392–399. https://doi.org/10.3945/ajcn.113.072066
De Souza RJ, Bray GA, Carey VJ et al (2012) Effects of 4 weight-loss diets differing in fat, protein, and carbohydrate on fat mass, lean mass, visceral adipose tissue, and hepatic fat: results from the POUNDS LOST trial. Am J Clin Nutr 95:614–625. https://doi.org/10.3945/ajcn.111.026328
Summa KC, Turek FW (2014) Chronobiology and obesity: interactions between circadian rhythms and energy regulation. Adv Nutr 5:312S–312S9S. https://doi.org/10.3945/an.113.005132
Turek FW, Joshu C, Kohsaka A et al (2005) Obesity and metabolic syndrome in circadian clock mutant mice. Science 308:1043–1045. https://doi.org/10.1126/science.1108750
Kumar Jha P, Challet E, Kalsbeek A (2015) Circadian rhythms in glucose and lipid metabolism in nocturnal and diurnal mammals. Mol Cell Endocrinol 418:74–88. https://doi.org/10.1016/j.mce.2015.01.024
Wolden-Hanson T, Mitton DR, McCants RL et al (2000) Daily melatonin administration to middle-aged male rats suppresses body weight, intraabdominal adiposity, and plasma leptin and insulin independent of food intake and total body fat. Endocrinology 141:487–497. https://doi.org/10.1210/en.141.2.487
Lane JM, Chang AM, Bjonnes AC et al (2016) Impact of common diabetes risk variant in MTNR1B on sleep, circadian, and melatonin physiology. Diabetes 65:1741–1751. https://doi.org/10.2337/db15-0999
Oosterman JE, Kalsbeek A, la Fleur SE, Belsham DD (2015) Impact of nutrients on circadian rhythmicity. Am J Physiol Regul Integr Comp Physiol 308:R337–R350. https://doi.org/10.1152/ajpregu.00322.2014
Yanagihara H, Ando H, Hayashi Y et al (2006) High-fat feeding exerts minimal effects on rhythmic mRNA expression of clock genes in mouse peripheral tissues. Chronobiol Int 23:905–914. https://doi.org/10.1080/07420520600827103
Hsieh M-C, Yang S-C, Tseng H-L et al (2010) Abnormal expressions of circadian-clock and circadian clock-controlled genes in the livers and kidneys of long-term, high-fat-diet-treated mice. Int J Obes (Lond) 34:227–239. https://doi.org/10.1038/ijo.2009.228
Cano P, Jiménez-Ortega V, Larrad Á et al (2008) Effect of a high-fat diet on 24-h pattern of circulating levels of prolactin, luteinizing hormone, testosterone, corticosterone, thyroid-stimulating hormone and glucose, and pineal melatonin content, in rats. Endocrine 33:118–125. https://doi.org/10.1007/s12020-008-9066-x
Cano P, Cardinali DP, Rios-Lugo MJ et al (2009) Effect of a high-fat diet on 24-hour pattern of circulating adipocytokines in rats. Obes (Silver Spring) 17:1866–1871. https://doi.org/10.1038/oby.2009.200
Cardinali DP, Cano P, Jiménez-Ortega V, Esquifino AI (2011) Melatonin and the metabolic syndrome: physiopathologic and therapeutical implications. Neuroendocrinology 93:133–142. https://doi.org/10.1159/000324699
Zalatan F, Krause JA, Blask DE (2001) Inhibition of isoproterenol-induced lipolysis in rat inguinal adipocytes in vitro by physiological melatonin via a receptor-mediated mechanism. Endocrinology 142:3783–3790. https://doi.org/10.1210/en.142.9.3783
Staiger H, Machicao F, Schäfer SA et al (2008) Polymorphisms within the novel type 2 diabetes risk locus MTNR1B determine β-cell function. PLoS One 3:e3962. https://doi.org/10.1371/journal.pone.0003962
Foster GD, Wyatt HR, Hill JO et al (2003) A randomized trial of a low-carbohydrate diet for obesity. N Engl J Med 348:2082–2090. https://doi.org/10.1056/NEJMoa022207
Dansinger ML, Gleason JA, Griffith JL et al (2005) Comparison of the Atkins, Ornish, Weight Watchers, and Zone Diets for weight loss and heart disease risk reduction: a randomized trial. J Am Med Assoc 293:43–53. https://doi.org/10.1097/00008483-200505000-00012
Shai I, Schwarzfuchs D, Henkin Y et al (2008) Weight loss with a low-carbohydrate, Mediterranean, or low-fat diet. N Engl J Med 359:229–241. https://doi.org/10.1056/NEJMoa1208410
Acknowledgements
The authors thank all participants of the study for their dedication and contribution to the research. The study is supported by grants from the National Heart, Lung, and Blood Institute (HL-071981, HL-034594, HL-126024), the National Institute of Diabetes and Digestive and Kidney Diseases (DK-091718, DK-100383, DK-078616), the Boston Obesity Nutrition Research Center (DK-46200), and United States–Israel Binational Science Foundation Grant 2011036. LG is a recipient of a pre-doctoral and a mobility grant from the Spanish Ministry of Education, Culture and Sport. YH is a recipient of a Grant-in-Aid for Scientific Research from the Japan Society for the Promotion of Science. LQ was a recipient of the American Heart Association Scientist Development Award (0730094N).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical standards
All procedures of the present study were in accordance with the ethical standards laid down in the 1964 Helsinki declaration and its later amendments. The study was approved by the human subjects committee at each institution and by a data and safety monitoring board appointed by the National Heart, Lung and Blood Institute.
Informed consent
All participants provided written informed consent.
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Goni, L., Sun, D., Heianza, Y. et al. A circadian rhythm-related MTNR1B genetic variant modulates the effect of weight-loss diets on changes in adiposity and body composition: the POUNDS Lost trial. Eur J Nutr 58, 1381–1389 (2019). https://doi.org/10.1007/s00394-018-1660-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-018-1660-y