Abstract
Purpose
To test the effect of three diets in their ability to sustain weight loss and improve type 2 diabetes (T2D) and cardiovascular disease (CVD) risk markers after 18-month intervention.
Methods
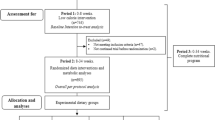
Following a ≥8 % weight loss, 131 healthy, overweight/obese (BMI ± SD 31.5 ± 2.6 kg/m2) men (n = 55) and women (n = 76) aged 28.2 ± 4.8 years were randomized to either 1. Moderate fat (40 E%) with 20 E% MUFA and low in glycemic index (GI) (MUFA, n = 54), 2. Low fat (25 E%) and medium in GI (LF, n = 51) or 3. Control (35 E% fat) and high in GI (CTR, n = 26) all with similar protein content, and all provided ad libitum. First 6-month intervention with 100 % food provision (previously reported) following 12 months of moderately intensive intervention with 20 % food provision now reported.
Results
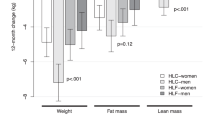
Attrition rate was higher in MUFA (63 %) than in LF (37 %, P = 0.019) and CTR (42 %, P = 0.09) group. Weight regain in completers was not different between groups (mean ± SEM), MUFA 7.1 ± 2.1 % versus LF 5.6 ± 1.3 % versus CTR 7.2 ± 1.5 %, nor was body fat regain, MUFA 4.8 ± 1.0 % versus LF 4.7 ± 0.8 % versus CTR 5.7 ± 0.6 %. The MUFA group reduced LDL/HDL ratio by −0.47 ± 0.09 compared with −0.23 ± 0.11 in LF (P < 0.05) and 0.06 ± 0.14 (P < 0.005) in CTR groups.
Conclusions
Weight regain or body composition did not differ between diets over 18 months. No effects on risk markers for T2D or CVD were found, with the exception of an improvement in the LDL/HDL ratio by the MUFA diet compared to the CTR diet. The LF diet was generally more satisfactory and the MUFA diet seemed more difficult to follow.


Similar content being viewed by others
References
Anderson JW, Konz EC, Frederich RC, Wood CL (2001) Long-term weight-loss maintenance: a meta-analysis of US studies. Am J Clin Nutr 74:579–584
Douketis JD, Macie C, Thabane L, Williamson DF (2005) Systematic review of long-term weight loss studies in obese adults: clinical significance and applicability to clinical practice. Int J Obes (Lond) 29:1153–1167
Nordic Council oM (2005) Nordic nutrition recommendations 2004. Integrating nutrition and physical activity, Copenhagen
Johnston B, Kanters S, Bandayrel K, Wu P, Naji F, Siemieniuk R, Ball GDC, Busse J, Thorlund K, Guyatt G, Jansen J, Mills E (2014) Comparison of weight loss among named diet programs in overweight and obese adults: a meta-analysis. JAMA J Am Med Assoc 312:923–933
Hu T, Bazzano LA (2014) The low-carbohydrate diet and cardiovascular risk factors: evidence from epidemiologic studies. NMCD Nutr Metab Cardiovasc Dis 24:337–343
Hu T, Mills K, Yao L, Demanelis K, Eloustaz M, Yancy W, Kelly T, He J, Bazzano L (2012) Effects of low-carbohydrate diets versus low-fat diets on metabolic risk factors: a meta-analysis of randomized controlled clinical trials. Am J Epidemiol 176(Suppl 7):S44–S54
Estruch R, Ros E, Salas Salvadó J, Covas M, Corella D, Arós F, Gómez Gracia E, Ruiz Gutiérrez V, Fiol M, Lapetra J, Lamuela Raventos R, Serra Majem L, Pintó X, Basora J, Muñoz M, Sorlí J, Martínez J, Martínez González M (2013) Primary prevention of cardiovascular disease with a Mediterranean diet. N Engl J Med 368:1279–1290
Nordmann A, Suter Zimmermann K, Bucher H, Shai I, Tuttle K, Estruch R, Briel M (2011) Meta-analysis comparing Mediterranean to low-fat diets for modification of cardiovascular risk factors. Am J Med 124(841–51):e2
Due A, Larsen TM, Hermansen K, Stender S, Holst JJ, Toubro S, Martinussen T, Astrup A (2008) Comparison of the effects on insulin resistance and glucose tolerance of 6-mo high-monounsaturated-fat, low-fat, and control diets. Am J Clin Nutr 87:855–862
Due A, Larsen TM, Mu H, Hermansen K, Stender S, Astrup A (2008) Comparison of 3 ad libitum diets for weight-loss maintenance, risk of cardiovascular disease, and diabetes: a 6-mo randomized, controlled trial. Am J Clin Nutr 88:1232–1241
Skov AR, Toubro S, Raben A, Astrup A (1997) A method to achieve control of dietary macronutrient composition in ad libitum diets consumed by free-living subjects. Eur J Clin Nutr 51:667–672
Gadbury GL, Coffey CS, Allison DB (2003) Modern statistical methods for handling missing repeated measurements in obesity trial data: beyond LOCF. Obes Rev 4:175–184
Estruch R, Martinez-Gonzalez MA, Corella D, Salas-Salvado J, Ruiz-Gutierrez V, Covas MI, Fiol M, Gomez-Gracia E, Lopez-Sabater MC, Vinyoles E, Aros F, Conde M, Lahoz C, Lapetra J, Saez G, Ros E (2006) Effects of a Mediterranean-style diet on cardiovascular risk factors: a randomized trial. Ann Intern Med 145:1–11
Fernandez de la Puebla RA, Fuentes F, Perez-Martinez P, Sanchez E, Paniagua JA, Lopez-Miranda J, Perez-Jimenez F (2003) A reduction in dietary saturated fat decreases body fat content in overweight, hypercholesterolemic males. Nutr Metab Cardiovasc Dis 13:273–277
McLaughlin T, Carter S, Lamendola C, Abbasi F, Schaaf P, Basina M, Reaven G (2007) Clinical efficacy of two hypocaloric diets that vary in overweight patients with type 2 diabetes: comparison of moderate fat versus carbohydrate reductions. Diabetes Care 30:1877–1879
Michalsen A, Lehmann N, Pithan C, Knoblauch NT, Moebus S, Kannenberg F, Binder L, Budde T, Dobos GJ (2006) Mediterranean diet has no effect on markers of inflammation and metabolic risk factors in patients with coronary artery disease. Eur J Clin Nutr 60:478–485
Paniagua JA, Gallego DL, Romero I, Vidal-Puig A, Latre JM, Sanchez E, Perez-Martinez P, Lopez-Miranda J, Perez-Jimenez F (2007) Monounsaturated fat-rich diet prevents central body fat distribution and decreases postprandial adiponectin expression induced by a carbohydrate-rich diet in insulin-resistant subjects. Diabetes Care 30:1717–1723
Pelkman CL, Fishell VK, Maddox DH, Pearson TA, Mauger DT, Kris-Etherton PM (2004) Effects of moderate-fat (from monounsaturated fat) and low-fat weight-loss diets on the serum lipid profile in overweight and obese men and women. Am J Clin Nutr 79:204–212
Petersen M, Taylor MA, Saris WH, Verdich C, Toubro S, Macdonald I, Rossner S, Stich V, Guy-Grand B, Langin D, Martinez JA, Pedersen O, Holst C, Sorensen TI, Astrup A (2006) Randomized, multi-center trial of two hypo-energetic diets in obese subjects: high- versus low-fat content. Int J Obes (Lond) 30:552–560
Vincent-Baudry S, Defoort C, Gerber M, Bernard MC, Verger P, Helal O, Portugal H, Planells R, Grolier P, Miot-Carlin MJ, Vague P, Lairon D (2005) The Medi-RIVAGE study: reduction of cardiovascular disease risk factors after a 3-mo intervention with a Mediterranean-type diet or a low-fat diet. Am J Clin Nutr 82:964–971
Azadbakht L, Mirmiran P, Esmaillzadeh A, Azizi F (2007) Better dietary adherence and weight maintenance achieved by a long-term moderate-fat diet. Br J Nutr 97:399–404
McManus K, Antinoro L, Sacks F (2001) A randomized controlled trial of a moderate-fat, low-energy diet compared with a low fat, low-energy diet for weight loss in overweight adults. Int J Obes Relat Metab Disord 25:1503–1511
Shai I, Schwarzfuchs D, Henkin Y, Shahar DR, Witkow S, Greenberg I, Golan R, Fraser D, Bolotin A, Vardi H, Tangi-Rozental O, Zuk-Ramot R, Sarusi B, Brickner D, Schwartz Z, Sheiner E, Marko R, Katorza E, Thiery J, Fiedler GM, Bluher M, Stumvoll M, Stampfer MJ (2008) Weight loss with a low-carbohydrate, Mediterranean, or low-fat diet. N Engl J Med 359:229–241
Bray GA, Popkin BM (1998) Dietary fat intake does affect obesity! Am J Clin Nutr 68:1157–1173
Michel de Lorgeril M, Salen P, Martin JL, Monjaud I, Delaye J, Mamelle N (1999) Mediterranean diet, traditional risk factors, and the rate of cardiovascular complications after myocardial infarction: final report of the Lyon Diet Heart Study. Circulation 99:779–785
Trichopoulou A, Bamia C, Trichopoulos D (2005) Mediterranean diet and survival among patients with coronary heart disease in Greece. Arch Intern Med 165:929–935
Knoops KT, de Groot LC, Kromhout D, Perrin AE, Moreiras-Varela O, Menotti A, van Staveren WA (2004) Mediterranean diet, lifestyle factors, and 10-year mortality in elderly European men and women: the HALE project. JAMA 292:1433–1439
Serra-Majem L, Roman B, Estruch R (2006) Scientific evidence of interventions using the Mediterranean diet: a systematic review. Nutr Rev 64:S27–S47
Esposito K, Marfella R, Ciotola M, Di PC, Giugliano F, Giugliano G, D’Armiento M, D’Andrea F, Giugliano D (2004) Effect of a mediterranean-style diet on endothelial dysfunction and markers of vascular inflammation in the metabolic syndrome: a randomized trial. JAMA 292:1440–1446
Esposito K, Pontillo A, Di Palo C, Giugliano G, Masella M, Marfella R, Giugliano D (2003) Effect of weight loss and lifestyle changes on vascular inflammatory markers in obese women: a randomized trial. JAMA 289:1799–1804
Esposito K, Maiorino MI, Ciotola M, Di PC, Scognamiglio P, Gicchino M, Petrizzo M, Saccomanno F, Beneduce F, Ceriello A, Giugliano D (2009) Effects of a Mediterranean-style diet on the need for antihyperglycemic drug therapy in patients with newly diagnosed type 2 diabetes: a randomized trial. Ann Intern Med 151:306–314
Tuttle K, Shuler L, Packard D, Milton J, Daratha K, Bibus D, Short R (2008) Comparison of low-fat versus Mediterranean-style dietary intervention after first myocardial infarction (from The Heart Institute of Spokane Diet Intervention and Evaluation Trial). Am J Cardiol 101:1523–1530
Culberson A, Kafai MR, Ganji V (2009) Glycemic load is associated with HDL cholesterol but not with the other components and prevalence of metabolic syndrome in the third National Health and Nutrition Examination Survey, 1988–1994. Int Arch Med 2:3
Liu S, Manson JE, Stampfer MJ, Holmes MD, Hu FB, Hankinson SE, Willett WC (2001) Dietary glycemic load assessed by food-frequency questionnaire in relation to plasma high-density-lipoprotein cholesterol and fasting plasma triacylglycerols in postmenopausal women. Am J Clin Nutr 73:560–566
Augustin LS, Kendall CW, Jenkins DJ, Willett WC, Astrup A, Barclay AW, Bjorck I, Brand-Miller JC, Brighenti F, Buyken AE, Ceriello A, La Vecchia C, Livesey G, Liu S, Riccardi G, Rizkalla SW, Sievenpiper JL, Trichopoulou A, Wolever TM, Baer-Sinnott S, Poli A (2015) Glycemic index, glycemic load and glycemic response: an International Scientific Consensus Summit from the International Carbohydrate Quality Consortium (ICQC). Nutr Metab Cardiovasc Dis 25:795–815
Ford ES, Liu S (2001) Glycemic index and serum high-density lipoprotein cholesterol concentration among us adults. Arch Intern Med 161:572–576
Frost G, Leeds AA, Dore CJ, Madeiros S, Brading S, Dornhorst A (1999) Glycaemic index as a determinant of serum HDL-cholesterol concentration. Lancet 353:1045–1048
Jenkins DJ, Kendall CW, McKeown-Eyssen G, Josse RG, Silverberg J, Booth GL, Vidgen E, Josse AR, Nguyen TH, Corrigan S, Banach MS, Ares S, Mitchell S, Emam A, Augustin LS, Parker TL, Leiter LA (2008) Effect of a low-glycemic index or a high-cereal fiber diet on type 2 diabetes: a randomized trial. JAMA 300:2742–2753
Bos MB, de Vries JH, Feskens EJ, van Dijk SJ, Hoelen DW, Siebelink E, Heijligenberg R, de Groot LC (2010) Effect of a high monounsaturated fatty acids diet and a Mediterranean diet on serum lipids and insulin sensitivity in adults with mild abdominal obesity. Nutr Metab Cardiovasc Dis 20:591–598
Rivellese AA, Maffettone A, Vessby B, Uusitupa M, Hermansen K, Berglund L, Louheranta A, Meyer BJ, Riccardi G (2003) Effects of dietary saturated, monounsaturated and n-3 fatty acids on fasting lipoproteins, LDL size and post-prandial lipid metabolism in healthy subjects. Atherosclerosis 167:149–158
Thomsen C, Rasmussen O, Lousen T, Holst JJ, Fenselau S, Schrezenmeir J, Hermansen K (1999) Differential effects of saturated and monounsaturated fatty acids on postprandial lipemia and incretin responses in healthy subjects. Am J Clin Nutr 69:1135–1143
Franz MJ, Bantle JP, Beebe CA, Brunzell JD, Chiasson JL, Garg A, Holzmeister LA, Hoogwerf B, Mayer-Davis E, Mooradian AD, Purnell JQ, Wheeler M (2002) Evidence-based nutrition principles and recommendations for the treatment and prevention of diabetes and related complications. Diabetes Care 25:148–198
Nielsen A, Korzen S, Holm L (2008) Inverting the food pyramid? Social and cultural acceptability of Walter Willett’s dietary recommendations among people with weight concerns. Appetite 51:178–186
Dansinger ML, Gleason JA, Griffith JL, Selker HP, Schaefer EJ (2005) Comparison of the Atkins, Ornish, Weight Watchers, and Zone diets for weight loss and heart disease risk reduction: a randomized trial. JAMA 293:43–53
Acknowledgments
The authors wish to thank the project staff of the Department of Human Nutrition. Special thanks to Professor Walter Willett, Department of Epidemiology and Nutrition, Harvard School of Public Health, Boston, Massachusetts, USA, and David Ludwig MD, PhD, Department of Medicine, Children’s Hospital, Boston, Massachusetts, USA, for participating in the design of the project and Miguel Padilla, PhD, Department of Biostatistics, University of Alabama at Birmingham, USA, for the ITT analysis.
Funding
This research was supported by foundations, associations, and research councils (e.g. H.A. Foundation, The Danish Heart Association, The Danish Diabetes Association, Centre for Advanced Food Research, The state Research Councils, The Danish Pork Council foundations). Effort for David B Allison was supported by P3ODK056336. Most of the foods in the supermarket (80 %) and the low-calorie diets were sponsored by the food industry. No sponsor participated in the analysis or interpretation of the data, manuscript preparation, review, or approval, or the decision to publish.
Author contribution
Due had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis. Astrup, Larsen, Toubro, and Due are involved in study concept and design. Due and Larsen are involved in acquisition of data. Due, Larsen, Mu, Hermansen, Stender, Toubro, Allison, and Astrup analysed and interpreted the data. Due drafted the manuscript. Due, Larsen, Mu, Hermansen, Stender, Toubro, Allison, and Astrup contributed to the critical revision of the manuscript for important intellectual content. Due and Allison are involved in statistical analysis. Astrup, Larsen and Due obtained funding. Due, Larsen, Mu, Hermansen, Stender, and Astrup provided administrative, technical, or material support. Astrup supervised the study. All listed authors have contributed significantly to the manuscript and given their consent for publication. None of the listed authors have conflicting interests that might affect the outcome of this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Due, A., Larsen, T.M., Mu, H. et al. The effect of three different ad libitum diets for weight loss maintenance: a randomized 18-month trial. Eur J Nutr 56, 727–738 (2017). https://doi.org/10.1007/s00394-015-1116-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-015-1116-6