Abstract
Background
In different circumstances such as infant malnutrition, old age or chronic disease, decline of muscular strength, particularly anaerobic power, is shown. In this context, our laboratory, has demonstrated a decrease in anaerobic glycolytic power in pre-pubertal Bolivian children living at low and high altitude and suffering from marginal protein malnutrition.
Aim of the study
To bring molecular support to the relationship between protein malnutrition and anaerobic glycolytic metabolism, we studied the impact of prolonged protein malnutrition on lactate metabolism in different muscles of growing rats. Lactate dehydrogenase (LDH), monocarboxylate transporters (MCT1, MCT4) and membrane protein CD147 were chosen as specific markers of anaerobic glycolytic metabolism.
Methods
Two groups of 10 weaning male rats were fed for 10 weeks either ad libitum with a well-balanced diet containing 18% protein or an isocaloric-diet containing 8% protein. LDH activity and mRNA amounts of LDH isoforms, MCT, CD147 were measured.
Results
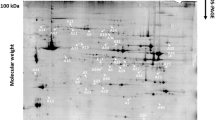
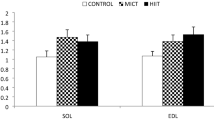
Protein deprivation during rat growth induced a decrease of LDH specific activity in skeletal muscles (mean value of −41%), accompanied by isoform distribution modifications in soleus, but not in glycolytic muscles (extensor digitorum longus (EDL) or plantaris). A reduction in mRNA amounts encoding the LDH A and B subunits was observed in EDL. A decrease in LDH B mRNA amounts was monitored in plantaris, whereas no modification in both LDH isoform mRNA quantities was observed in soleus. MCT1 mRNA quantities were decreased in EDL but MCT4 mRNA quantities remained stable. CD147 mRNA amounts were unchanged except for EDL with a 42% increase.
Conclusions
The global decreases of LDH activity, LDH and MCT gene expressions in growing rat skeletal muscles support the observed alterations of lactate metabolism associated with lowered muscular anaerobic performances in protein malnutrition.



Similar content being viewed by others
Abbreviations
- CTRL::
-
Control
- EDL::
-
Extensor digitorum longus
- L32::
-
Ribosomal L32 protein
- LDH::
-
Lactate dehydrogenase
- MALN::
-
Malnourished
- MCT1::
-
Monocarboxylate transporter 1
- MCT4::
-
Monocarboxylate transporter 4
- REx::
-
Relative expression
References
Ardawi MS, Majzoub MF, Masoud IM, Newsholme EA (1989) Enzymic and metabolic adaptations in the gastrocnemius, plantaris and soleus muscles of hypocaloric rats. Biochem J 261:219–225
Barclay CJ, Loiselle DS (1992) Dependence of muscle fatigue on stimulation protocol: effect of hypocaloric diet. J Appl Physiol 72:2278–2284
Raju NV (1974) Effect of early malnutrition on muscle function and metabolism in rats. Life Sci 15:949–960
Russell DM, Atwood HL, Whittaker JS, Itakura T, Walker PM, Mickle DA, Jeejeebhoy KN (1984) The effect of fasting and hypocaloric diets on the functional and metabolic characteristics of rat gastrocnemius muscle. Clin Sci (Lond) 67:185–194
Oldfors A, Sourander P (1986) Nutritional rehabilitation of skeletal muscle in protein-deprived young rats. J Neurol Sci 75:173–179
Taskar K, Tulpule PG (1964) Influence of protein and calorie deficiencies in the rat on the energy-transfer reactions of the striated muscle. Biochem J 92:391–398
Lago ES, Teodosio NR, Araujo CR, Azevedo MC, Pessoa DC, Campos FA, Zucas SM, Flores H (1993) Rat models of protein and protein-energy malnutrition. Int J Vitam Nutr Res 63:52–56
Penney D, Anderson D, Dongas J (1976) Effects of early severe malnutrition on heart and skeletal muscle lactate dehydrogenase. J Nutr 106: 1235–1240
Nishio ML, Jeejeebhoy KN (1992) Effect of malnutrition on aerobic and anaerobic performance of fast- and slow-twitch muscles of rats. J Parenter Enteral Nutr 16:219–225
Bar-Or O (1986) Pathophysiological factors which limit the exercise capacity of the sick child. Med Sci Sports Exerc 18:276–282
Chopra JS (1991) Neurological consequences of protein and protein-calorie undernutrition. Crit Rev Neurobiol 6:99–117
Gupta RK, Mittal RD, Agarwal KN, Agarwal DK (1994) Muscular sufficiency, serum protein, enzymes and bioenergetic studies (31-phosphorus magnetic resonance spectroscopy) in chronic malnutrition. Acta Paediatr 83:327–331
Blonc S, Fellmann N, Bedu M, Falgairette G, De Jonge R, Obert P, Beaune B, Spielvogel H, Tellez W, Quintela A, San Miguel JL, Coudert J (1996) Effect of altitude and socioeconomic status on VO2max and anaerobic power in prepubertal Bolivian girls. J Appl Physiol 80:2002–2008
Obert P, Bedu M, Fellmann N, Falgairette G, Beaune B, Quintela A, Van Praagh E, Spielvogel H, Kemper H, Post B, et al. (1993) Effect of chronic hypoxia and socioeconomic status on VO2max and anaerobic power of Bolivian boys. J Appl Physiol 74:888–896
Kayser B, Narici M, Milesi S, Grassi B, Cerretelli P (1993) Body composition and maximum alactic anaerobic performance during a one month stay at high altitude. Int J Sports Med 14:244–247
Hanning RM, Blimkie CJ, Bar-Or O, Lands LC, Moss LA, Wilson WM (1993) Relationships among nutritional status and skeletal and respiratory muscle function in cystic fibrosis: does early dietary supplementation make a difference? Am J Clin Nutr 57:580–587
Klijn PH, Terheggen-Lagro SW, Van Der Ent CK, Van Der Net J, Kimpen JL , Helders PJ (2003) Anaerobic exercise in pediatric cystic fibrosis. Pediatr Pulmonol 36:223–229
Laaban JP (2000) Nutrition and chronic respiratory failure. Ann Med Interne (Paris) 151:542–548
McParland C, Resch EF, Krishnan B, Wang Y, Cujec B, Gallagher CG (1995) Inspiratory muscle weakness in chronic heart failure: role of nutrition and electrolyte status and systemic myopathy. Am J Respir Crit Care Med 151:1101–1107
Leberer E, Pette D (1984) Lactate dehydrogenase isozymes in type I, IIA and IIB fibres of rabbit skeletal muscles. Histochemistry 80:295–298
Halestrap AP, Price NT (1999) The proton-linked monocarboxylate transporter (MCT) family: structure, function and regulation. Biochem J 343:281–299
Brooks G.A (2000) Intra and extra-cellular lactate shuttles. Med Sci Sports Exerc 32:790–799
Fishbein WN, Merezhinskaya N, Foellmer JW (2002) Relative distribution of three major lactate transporters in frozen human tissues and their localization in unfixed skeletal muscle. Muscle Nerve 26:101–112
Bonen A (2001) The expression of lactate transporters (MCT1 and MCT4) in heart and muscle. Eur J Appl Physiol 86:6–11
Manning Fox JE, Meredith D, Halestrap AP (2000) Characterisation of human monocarboxylate transporter 4 substantiates its role in lactic acid efflux from skeletal muscle. J Physiol 529:285–293
Kirk P, Wilson MC, Heddle C, Brown MH, Barclay AN, Halestrap AP (2000) CD147 is tightly associated with lactate transporters MCT1 and MCT4 and facilitates their cell surface expression. EMBO J 19:3896–3904
Rossignol F, Solares M, Balanza E, Coudert J, Clottes E (2003). Expression of lactate dehydrogenase A and B genes in different tissues of rats adapted to chronic hypobaric hypoxia. J Cell Biochem 89:67–79
Thellin O, Zorzi W, Lakaye B, De Borman B, Coumans B, Hennen G, Grisar T, Igout A, Heinen E (1999) Housekeeping genes as internal standards: use and limits. J Biotechnol 75:291–295
Fiorotto ML, Davis TA (1997) Food intake alters muscle protein gain with little effect on Na(+)-K(+)-ATPase and myosin isoforms in suckled rats. Am J Physiol 272:R1461–R1471
Chauhan S, Nayak NC, Ramalingaswami V (1965) The heart and skeletal muscle in experimental protein malnutrition in rhesus monkeys. J Pathol Bacteriol 90:301–319
Oldfors A, Mair WG, Sourander P (1983) Muscle changes in protein-deprived young rats. A morphometrical, histochemical and ultrasound study. J Neurol Sci 59:291–302
Nascimento OJ, Madi K, Guedes e Silva JB, Soares Filho PJ, Hahn MD, Couto B, Freitas MR (1990) Striated muscle in protein malnutrition: an experimental study in albino rats. Arq Neuropsiquiatr 48:395–402
Montgomery RD (1962) Changes in the basal metabolic rate of the malnourished infant and their relation to body composition. J Clin Invest 41:1653–1663
Kumari R, Rao YN, Talukdar B, Agarwal S, Puri RK (1993) Serum enzyme abnormalities in protein energy malnutrition. Indian Pediatr 30:469–473
Goldspink DF, Cox VM, Smith SK, Eaves LA, Osbaldeston NJ, Lee DM, Mantle D (1995) Muscle growth in response to mechanical stimuli. Am J Physiol 268:E288–E297
Semsarian C, Sutrave P, Richmond DR, Graham RM (1999) Insulin-like growth factor (IGF-I) induces myotube hypertrophy associated with an increase in anaerobic glycolysis in a clonal skeletal-muscle cell model. Biochem J 339:443–451
Takahashi S, Kajikawa M, Umezawa T, Takahashi S, Kato H, Miura Y, Nam TJ, Noguchi T, Naito H (1990) Effect of dietary proteins on the plasma immunoreactive insulin-like growth factor-1/somatomedin C concentration in the rat. Br J Nutr 63:521–534
Noguchi T (2000) Protein nutrition and insulin-like growth factor system. Br J Nutr 84:S241–S244
Oster MH, Fielder PJ, Levin N, Cronin MJ (1995) Adaptation of the growth hormone and insulin-like growth factor-I axis to chronic and severe calorie or protein malnutrition. J Clin Invest 95:2258–2265
Lewis MI, Li H, Huang ZS, Biring MS, Cercek B, Fournier M (2003) Influence of varying degrees of malnutrition on IGF-I expression in the rat diaphragm. J Appl Physiol 95:555–562
Beaune B, Blonc S, Fellmann N, Bedu M, Coudert J (1997) Serum insulin-like growth factor I and physical performance in prepubertal Bolivian girls of a high and low socio-economic status. Eur J Appl Physiol Occup Physiol 76:98–102
Marieze VL, Briand M, Badaoui S, Dadet MH, Briand Y (1994) Expression of lactic dehydrogenase isoenzymes in rabbit muscle during development. Int J Biochem 26:491–495
Dubouchaud H, Butterfield GE, Wolfel EE, Bergman BC, Brooks GA (2000) Endurance training, expression, and physiology of LDH, MCT1, and MCT4 in human skeletal muscle. Am J Physiol Endocrinol Metab 278:E571–E579
McClelland GB, Khanna S, Gonzalez GF, Butz CE, Brooks GA (2003) Peroxisomal membrane monocarboxylate transporters: evidence for a redox shuttle system? Biochem Biophys Res Commun 304:130–135
Gladden LB (2004) Lactate metabolism: a new paradigm for the third millennium. J Physiol 558:5–30
Finnemann SC, Marmorstein AD, Neill JM, Rodriguez-Boulan E (1997) Identification of the retinal pigment epithelium protein RET-PE2 as CE-9/OX-47, a member of the immunoglobulin superfamily. Invest Ophthalmol Vis Sci 38:2366–2374
Lambert K, Py G, Eydoux N, Matecki S, Ramonatxo M, Prefaut C, Mercier J (2003) Effect of food restriction on lactate sarcolemmal transport. Metabolism 52:322–327
Filippatos GS, Anker SD, Kremastinos DT (2005) Pathophysiology of peripheral muscle wasting in cardiac cachexia. Curr Opin Clin Nutr Metab Care 8:249–254
Bonnefoy M, Constans T, Ferry M (2000) Influence of nutrition and physical activity on muscle in the very elderly. Presse Med 29:2177–2182
Pasini E, Aquilani R, Gheorghiade M, Dioguardi FS (2003) Malnutrition, muscle wasting and cachexia in chronic heart failure: the nutritional approach. Ital Heart J 4:232–235
Acknowledgments
The authors would like to thank Pamela Houston for careful reading of the manuscript. This work was supported by a grant from the Ministère Français de la Recherche et de la Technologie.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by a grant from the Ministère Français de la Recherche et de la Technologie.
Rights and permissions
About this article
Cite this article
Jouaville, L.F., Fellmann, N., Coudert, J. et al. Skeletal muscle expression of LDH and monocarboxylate transporters in growing rats submitted to protein malnutrition. Eur J Nutr 45, 355–362 (2006). https://doi.org/10.1007/s00394-006-0606-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00394-006-0606-y