Abstract
Background
Cardiac magnetic resonance (CMR) provides information on morpho-functional abnormalities and myocardial tissue characterisation. Appropriate indications for CMR in athletes are uncertain.
Objective
To analyse the CMR performed at our Institute to evaluate variables associated with pathologic findings in a large cohort of athletes presenting with different clinical conditions.
Methods
All the CMR performed at our Institute in athletes aged > 14 years were recruited. CMR indications were investigated. CMR was categorised as “positive” or “negative” based on the presence of morphological and/or functional abnormalities and/or the presence of late gadolinium enhancement (excluding the right ventricular insertion point), fat infiltration, or oedema. Variables associated with “positive” CMR were explored.
Results
A total of 503 CMR were included in the analysis. “Negative” and “positive” CMR were 61% and 39%, respectively. Uncommon ventricular arrhythmias (VAs) were the most frequent indications for CMR, but the proportion of positive results was low (37%), and only polymorphic ventricular patterns were associated with positive CMR (p = 0.006). T-wave inversion at 12-lead ECG, particularly on lateral and inferolateral leads, was associated with positive CMR in 34% of athletes (p = 0.05). Echocardiography abnormalities resulted in a large proportion (58%) of positive CMR, mostly cardiomyopathies.
Conclusion
CMR is more efficient in identifying a pathologic cardiac substrate in athletes in case of VAs (i.e., polymorphic beats), abnormal ECG repolarisation (negative T-waves in inferolateral leads), and borderline echocardiographic findings (LV hypertrophy, mildly depressed LV function). On the other hand, CMR is associated with a large proportion of negative results. Therefore, a careful clinical selection is needed to indicate CMR in athletes appropriately.
Graphical Abstract
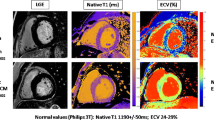
Clinical indications for CMR and positive CMR findings.
The left panel shows clinical indications for CMR in our athletic cohort and the percentage of negative CMRs. In contrast, the right one shows the percentages of positive CMR findings with some examples. The white arrows in the right panel show an ARVD with a dilated right ventricle and multiple aneurysms of its free wall. The red arrows show the distribution of LGE in the left ventricle. The red panel below shows indications associated with positive CMR findings. ARVD, arrhythmogenic right ventricular disease; BAV, bicuspid aortic valve; CMP, cardiomyopathies; CMR, cardiac magnetic resonance; DCM, dilated cardiomyopathy; ECG, electrocardiogram; Echo, echocardiogram; FHx, family history; HCM, hypertrophic cardiomyopathy; LAD, left axis deviation; LBBB, left bundle branch block; LGE, late gadolinium enhancement; LV, left ventricle; LVH, left ventricular hypertrophy; LVNC, left ventricular non-compaction; MVP, mitral valve prolapse; RV, right ventricle; SVAs, supraventricular arrhythmias; VAs, ventricular arrhythmias; VHD, valvular heart diseases; TWI, T-wave inversion.

Similar content being viewed by others
Data availability
The data underlying this article will be shared on reasonable request to the corresponding author.
References
Maestrini V, Torlasco C, Hughes R, Moon JC (2020) Cardiovascular magnetic resonance and sport cardiology: a growing role in clinical dilemmas. J Cardiovasc Transl Res 13:296–305. https://doi.org/10.1007/s12265-020-10022-7
Pelliccia A, Maron BJ (1995) Preparticipation cardiovascular evaluation of the competitive athlete: perspectives from the 30-year Italian experience. Am J Cardiol 75:827–829. https://doi.org/10.1016/S0002-9149(99)80421-4
Pelliccia A, Adami PE, Quattrini F et al (2017) Are Olympic athletes free from cardiovascular diseases? Systematic investigation in 2352 participants from Athens 2004 to Sochi 2014. Br J Sports Med 51:238–243. https://doi.org/10.1136/BJSPORTS-2016-096961
Pelliccia A, Sharma S, Gati S et al (2021) 2020 ESC Guidelines on sports cardiology and exercise in patients with cardiovascular disease. Eur Heart J 42:17–96. https://doi.org/10.1093/eurheartj/ehaa605
Ljungqvist A, Jenoure PJ, Engebretsen L et al (2009) The International Olympic Committee (IOC) consensus statement on periodic health evaluation of elite athletes, March 2009. Clin J Sport Med 19:347–365. https://doi.org/10.1097/JSM.0B013E3181B7332C
Mancia G, Fagard R, Narkiewicz K et al (2013) 2013 ESH/ESC guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). Eur Heart J 34:2159–2219. https://doi.org/10.1093/EURHEARTJ/EHT151
Drezner JA, Sharma S, Baggish A et al (2017) International criteria for electrocardiographic interpretation in athletes: consensus statement. Br J Sports Med 51:704–731. https://doi.org/10.1136/BJSPORTS-2016-097331
Caselli S, Vaquer Sequì A, Lemme E et al (2017) Prevalence and management of systemic hypertension in athletes. Am J Cardiol 119:1616–1622. https://doi.org/10.1016/J.AMJCARD.2017.02.011
Myers J, Arena R, Franklin B et al (2009) Recommendations for clinical exercise laboratories: a scientific statement from the American Heart Association. Circulation 119:3144–3161. https://doi.org/10.1161/CIRCULATIONAHA.109.192520
Corrado D, Drezner JA, D’Ascenzi F, Zorzi A (2020) How to evaluate premature ventricular beats in the athlete: critical review and proposal of a diagnostic algorithm. Br J Sports Med 54:1142–1148. https://doi.org/10.1136/BJSPORTS-2018-100529
Pelliccia A, Caselli S, Sharma S et al (2018) European Association of Preventive Cardiology (EAPC) and European Association of Cardiovascular Imaging (EACVI) joint position statement: recommendations for the indication and interpretation of cardiovascular imaging in the evaluation of the athlete’s heart. Eur Heart J 39:1949–1969. https://doi.org/10.1093/EURHEARTJ/EHX532
Lang RM, Badano LP, Mor-Avi V et al (2015) Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur Heart J Cardiovasc Imaging 16:233–271. https://doi.org/10.1093/EHJCI/JEV014
Kramer CM, Barkhausen J, Bucciarelli-Ducci C, et al (2020) Standardized cardiovascular magnetic resonance imaging (CMR) protocols: 2020 update. J Cardiovasc Magn Reson 22. https://doi.org/10.1186/S12968-020-00607-1
Leiner T, Bogaert J, Friedrich MG, et al (2020) SCMR Position Paper (2020) on clinical indications for cardiovascular magnetic resonance. J Cardiovasc Magn Reson 22:76. https://doi.org/10.1186/s12968-020-00682-4
Messroghli DR, Moon JC, Ferreira VM, et al (2017) Clinical recommendations for cardiovascular magnetic resonance mapping of T1, T2, T2* and extracellular volume: a consensus statement by the Society for Cardiovascular Magnetic Resonance (SCMR) endorsed by the European Association for Cardiovascular Imaging (EACVI). J Cardiovasc Magn Reson 19. https://doi.org/10.1186/S12968-017-0389-8
Maceira AM, Monmeneu JV, López MP, et al (2023) Reference ventricular dimensions and function parameters by cardiovascular magnetic resonance in highly trained Caucasian athletes. J Cardiovasc Magn Reson 25. https://doi.org/10.1186/s12968-023-00910-7
D’Ascenzi F, Pelliccia A, Solari M et al (2017) Normative reference values of right heart in competitive athletes: a systematic review and meta-analysis. J Am Soc Echocardiogr 30:845-858.e2. https://doi.org/10.1016/j.echo.2017.06.013
Zorzi A, Marra MP, Rigato I, et al (2016) Nonischemic left ventricular scar as a substrate of life-threatening ventricular arrhythmias and sudden cardiac death in competitive athletes. Circ Arrhythm Electrophysiol 9. https://doi.org/10.1161/CIRCEP.116.004229
Crescenzi C, Zorzi A, Vessella T et al (2021) Predictors of left ventricular scar using cardiac magnetic resonance in athletes with apparently idiopathic ventricular arrhythmias. J Am Heart Assoc 10:1–14. https://doi.org/10.1161/JAHA.120.018206
Pelliccia A, Maron BJ, Culasso F et al (1996) Athlete’s heart in women. Echocardiographic characterization of highly trained elite female athletes. JAMA 276:211–215. https://doi.org/10.1001/JAMA.276.3.211
D’Ascenzi F, Biella F, Lemme E, et al (2020) Female athlete’s heart: sex effects on electrical and structural remodeling. Circ Cardiovasc Imaging 1–13. https://doi.org/10.1161/CIRCIMAGING.120.011587
Pelliccia A, Borrazzo C, Maestrini V et al (2022) Determinants of LV mass in athletes: the impact of sport, constitutional traits and cardiovascular risk factors. Eur J Appl Physiol. https://doi.org/10.1007/S00421-022-05098-9
Author information
Authors and Affiliations
Contributions
V.M. and A.P.: conception and design of the work, data acquisition, analysis, writing, reviewing and final approval of the manuscript; S.M, M.P., C.B., S.P., D.F., L.I.B., E.L., G.D.G, R.M., M.R.S. and G.G.: data acquisition, analysis and interpretation of data for the work, writing, reviewing, and final approval of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
Institutional Review Board approval was obtained.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Conflict of interests
The authors declare no competing interests.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Maestrini, V., Penza, M., Monosilio, S. et al. The role of cardiac magnetic resonance in sports cardiology: results from a large cohort of athletes. Clin Res Cardiol 113, 781–789 (2024). https://doi.org/10.1007/s00392-024-02447-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-024-02447-w