Abstract
Aims
Longitudinal studies of the association between sex and adverse clinical outcomes in patients with chronic kidney disease (CKD) are scarce. We assessed whether major outcomes may differ by sex among CKD patients.
Methods
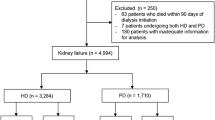
We analyzed a total of 1780 participants with non-dialysis CKD G1-5 from the KoreaN cohort study for Outcome in patients with Chronic Kidney Disease (KNOW-CKD). The primary outcome was a composite of non-fatal cardiovascular events or all-cause mortality. Secondary outcomes included fatal and non-fatal cardiovascular events, all-cause mortality, and a composite kidney outcome of ≥ 50% decline in estimated glomerular filtration rate from baseline or the onset of end-stage kidney disease.
Results
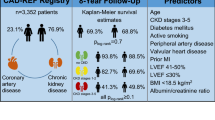
There were 1088 (61%) men and 692 (39%) women in the study cohort. The proportion of smokers was significantly higher in men (24% vs. 3%). During 8430 person-years of follow-up, 201 primary outcome events occurred: 144 (13%) in men and 57 (8%) in women, with corresponding incidence rates of 2.9 and 1.7 per 100 person-years, respectively. In multivariable Cox models, men were associated with a 1.58-fold (95% CI 1.06–2.35) higher risk of composite outcome. Propensity score matching analysis revealed similar findings (HR 1.81; 95% CI 1.14–2.91). Risk of all-cause mortality was significantly higher in men of the matched cohort. However, there was no difference in the risk of CKD progression. In the subgroup with coronary artery calcium (CAC) measurements, men had a higher likelihood of CAC progression.
Conclusions
In Korean CKD patients, men were more likely to experience adverse cardiovascular events and death than women.
Graphic abstract





Similar content being viewed by others
Availability of data and material
The data that support the findings of this study are available from the corresponding author (SHH) upon reasonable request.
References
GBD (2019) Demographic Collaborators (2020) Global age-sex-specific fertility, mortality, healthy life expectancy (HALE), and population estimates in 204 countries and territories, 1950–2019: a comprehensive demographic analysis for the global burden of disease study 2019. Lancet 396:1160–1203
Regitz-Zagrosek V, Kararigas G (2017) Mechanistic pathways of sex differences in cardiovascular disease. Physiol Rev 97:1–37
Metcalfe PD, Leslie JA, Campbell MT, Meldrum DR, Hile KL, Meldrum KK (2008) Testosterone exacerbates obstructive renal injury by stimulating TNF-alpha production and increasing proapoptotic and profibrotic signaling. Am J Physiol Endocrinol Metab 294:E435–E443
Mauvais-Jarvis F, Merz NB, Barnes PJ et al (2020) Sex and gender: modifiers of health, disease, and medicine. Lancet 396:565–582
Millett ERC, Peters SAE, Woodward M (2018) Sex differences in risk factors for myocardial infarction: cohort study of UK Biobank participants. BMJ 363:1–11
Huebschmann AG, Huxley RR, Kohrt WM, Zeitler P, Regensteiner JG, Reusch JEB (2019) Sex differences in the burden of type 2 diabetes and cardiovascular risk across the life course. Diabetologia 62:1761–1772
Garawi F, Devries K, Thorogood N, Uauy R (2014) Global differences between women and men in the prevalence of obesity: is there an association with gender inequality? Eur J Clin Nutr 68:1101–1106
Siegel RL, Miller KD, Jemal A (2017) Cancer statistics. CA Cancer J Clin 67:7–30
Vaccarezza M, Papa V, Milani D et al (2020) Sex/gender-specific imbalance in CVD: could physical activity help to improve clinical outcome targeting CVD molecular mechanisms in women? Int J Mol Sci 21:1–16
Nitsch D, Grams M, Sang Y et al (2013) Associations of estimated glomerular filtration rate and albuminuria with mortality and renal failure by sex: a meta-analysis. BMJ 346:1–14
Carrero JJ, Hecking M, Chesnaye NC, Jager KJ (2018) Sex and gender disparities in the epidemiology and outcomes of chronic kidney disease. Nat Rev Nephrol 14:151–164
Seppi T, Prajczer S, Dörler MM et al (2016) Sex differences in renal proximal tubular cell homeostasis. J Am Soc Nephrol 27:3051–3062
Kim C, Ricardo AC, Boyko EJ et al (2019) Sex hormones and measures of kidney function in the diabetes prevention program outcomes study. J Clin Endocrinol Metab 104:1171–1180
Elliot SJ, Karl M, Berho M et al (2003) Estrogen deficiency accelerates progression of glomerulosclerosis in susceptible mice. Am J Pathol 162:1441–1448
Doublier S, Lupia E, Catanuto P et al (2011) Testosterone and 17β-estradiol have opposite effects on podocyte apoptosis that precedes glomerulosclerosis in female estrogen receptor knockout mice. Kidney Int 79:404–413
Neugarten J, Acharya A, Silbiger SR (2000) Effect of gender on the progression of nondiabetic renal disease: a meta-analysis. J Am Soc Nephrol 11:319–329
Jafar TH, Schmid CH, Start PC et al (2003) The rate of progression of renal disease may not be slower in women compared with men: a patient-level meta-analysis. Nephrol Dial Transplant 18:2047–2053
Ricardo AC, Yang W, Sha D et al (2019) Sex-related disparities in CKD progression. J Am Soc Nephrol 30:137–146
Minutolo R, Gabbai FB, Chiodini P et al (2020) Sex differences in the progression of CKD among older patients: pooled analysis of 4 cohort studies. Am J Kidney Dis 75:30–38
Kidney Disease: Improving Global Outcomes (KDIGO) CKD-MBD Update Work Group (2017) KDIGO 2017 clinical practice guideline update for the diagnosis, evaluation, prevention, and treatment of chronic kidney disease-mineral and bone disorder (CKD-MBD). Kidney Int Suppl 7:1–59
Levey AS, Stevens LA, Schmid CH et al (2009) CKD-EPI (chronic kidney disease epidemiology collaboration): a new equation to estimate glomerular filtration rate. Ann Intern Med 150:604–612
Oh KH, Park SK, Park HC et al (2014) KNOW-CKD (KoreaN cohort study for outcome in patients with chronic kidney disease): design and methods. BMC Nephrol 15:80
Neves PO, Andrade J, Monção H (2017) Coronary artery calcium score: current status. Radiol Bras 50:182–189
Agatston AS, Janowitz WR, Hildner FJ, Zusmer NR, Viamonte M Jr, Detrano R (1990) Quantification of coronary artery calcium using ultrafast computed tomography. J Am Coll Cardiol 15:827–832
Chen J, Budoff MJ, Reilly MP et al (2017) Coronary artery calcification and risk of cardiovascular disease and death among patients with chronic kidney disease. JAMA Cardiol 2:635–643
Parikh NI, Hwang SJ, Larson MG, Meigs JB, Levy D, Fox CS (2006) Cardiovascular disease risk factors in chronic kidney disease. Arch Intern Med 166:1884–1891
Eriksen BO, Ingebretsen OC (2006) The progression of chronic kidney disease: a 10 year population-based study of the effects of gender and age. Kidney Int 69:375–382
Carrero JJ, de Jager DJ, Verduijn M et al (2011) Cardiovascular and noncardiovascular mortality among men and women starting dialysis. Clin J Am Soc Nephrol 6:1722–1730
Bild DE, Detrano R, Peterson D et al (2005) Ethnic differences in coronary calcification: the multi-ethnic study of atherosclerosis (MESA). Circulation 111:1313–1320
Schmermund A, Möhlenkamp S, Stang A et al (2002) Assessment of clinically silent atherosclerotic disease and established and novel risk factors for predicting myocardial infarction and cardiac death in health middle-aged subjects: rationale and design of the Heinz Nixdorf RECALL study. risk factors, evaluation of coronary calcium and lifestyle. Am Heart J 144:212–218
Vliegenthart R, Oudkerk M, Hofman A et al (2005) Coronary calcification improves cardiovascular risk prediction in the elderly. Circulation 112:572–577
Yano Y, O’Donnell CJ, Kuller L et al (2017) Association of coronary artery calcium score vs age with cardiovascular risk in older adults: an analysis of pooled population-base studies. JAMA Cardiol 2:986–894
Zhao M, Woodward M, Vaartjes I et al (2020) Sex differences in cardiovascular medication prescription in primary care: a systematic review and meta-analysis. J Am Heart Assoc 9:e014742
Tamargo J, Rosano G, Walther T et al (2017) Gender differences in the effects of cardiovascular drugs. Eur Heart J Cardiovasc Pharmacother 3:163–182
Miller JA, Anacta L, Cattran DC (1999) Impact of gender on the renal response to angiotensin II. Kidney Int 55:278–285
Ruggenenti P, Perna A, Zoccali C et al (2000) Chronic proteinuric nephropathies. II. Outcomes and response to treatment in a prospective cohort of 352 patients: differences between women and men in relation to the ACE gene polymorphism. J Am Soc Nephrol 11:88–96
Karp I, Chen SF, Pilote L (2007) Sex differences in the effectiveness of statins after myocardial infarction. CMAJ 176:333–338
Garg R, Yusuf S (1995) Overview of randomized trials of angiotensin-converting enzyme inhibitors on mortality and morbidity in patients with heart failure. Collaborative group on ACE inhibitor trials. JAMA 273:1450–1456
Kotecha D, Manzano L, Krum H et al (2016) Beta-blockers in heart failure collaborative group. Effect of age and sex on efficacy and tolerability of β blockers in patients with heart failure with reduced ejection fraction: individual patient data meta-analysis. BMJ 353:i18
Cholesterol Treatment Tiralists’ (CTT) Collaboration, Fulcher J, O’connel R, Voysey M, et al. (2015) Efficacy and safety of LDL-lowering therapy among men and women: meta-analysis of individual data from 174,000 participants in 27 randomised trials. Lancet 385:1397–1405
Jamal A, King BA, Neff LJ, Whitmill J, Dabb SD, Graffunder CM (2016) Current cigarette smoking among Adults—United States, 2005–2015. MMWR Morb Mortal Wkly Rep 65:1205–1211
Peters SAE, Huxley RR, Woodward M (2014) Do smoking habits differ between women and men in contemporary Western populations? Evidence from half a million people in the UK Biobank study. BMJ Open 4:1–8
Gunter R, Szeto E, Jeong SH, Suh S, Waters AJ (2020) Cigarette smoking in south korea: a narrative review. Korean J Fam Med 41:3–13
Mons U, Müezzinler A, Gellert C et al (2015) Impact of smoking and smoking cessation on cardiovascular events and mortality among older adults: meta-analysis of individual participant data from prospective cohort studies of the CHANCES consortium. BMJ 350:h1551
Coresh J, Byrd-Holt D, Astor BC et al (2005) Chronic kidney disease awareness, prevalence, and trends among U.S. adults, 1999 to 2000. J Am Soc Nephrol 16:180–188
Piccoli GB, Alrukhaimi M, Liu ZH, Zakharova E, Levin A (2018) What we do and do not know about women and kidney diseases; questions unanswered and answers unquestioned: reflection on World Kidney Day and International Women’s Day. BMC Nephrol 19:1–18
Xue JL, Eggers PW, Agodoa LY, Foley RN, Collins AJ (2007) Longitudinal study of racial and ethnic differences in developing end-stage renal disease among aged medicare beneficiaries. J Am Soc Nephrol 18:1299–1306
Kausz AT, Obrador GT, Arora P, Ruthazer R, Levey AS, Pereira BJ (2000) Late initiation of dialysis among women and ethnic minorities in the United States. J Am Soc Nephrol 11:2351–2357
Funding
This work was supported by the Research Program funded by the Korea Centers for Disease Control and Prevention (2011E3300300, 2012E3301100, 2013E3301600, 2013E3301601, 2013E3301602, 2016E3300200, and 2019E320101).
Author information
Authors and Affiliations
Contributions
C-YJ, GYH, and SHH contributed to the conception of the study. TIC, EWK, T-HY, JL, SWK, YKO, JYJ, K-HO, CA, and SHH contributed to data collection. C-YJ, GYH, HL, and SHH contributed to data analysis and interpretation. C-YJ and SHH drafted the manuscript. C-YJ, GYH, JTP, YSJ, HWK, HL, TIC, EWK, T-HY, S-WK, JL, SWK, YKO, JYJ, K-HO, CA, and SHH revised the manuscript for important intellectual content. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest with respect to this manuscript.
Ethical approval
The study was conducted in accordance with the principles of the Declaration of Helsinki, and approved by the institutional review boards of participating institutions.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jung, CY., Heo, G.Y., Park, J.T. et al. Sex disparities and adverse cardiovascular and kidney outcomes in patients with chronic kidney disease: results from the KNOW-CKD. Clin Res Cardiol 110, 1116–1127 (2021). https://doi.org/10.1007/s00392-021-01872-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-021-01872-5