Abstract
Objective
To determine whether statin therapy influences the efficacy of thrombin inhibitor bivalirudin or unfractionated heparin (UFH) during PCI.
Setting and patients
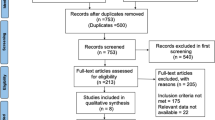
The post-hoc analysis of the ISAR-REACT 3 Trial included 4,570 patients: 3,106 patients were on statin therapy and 1,464 patients were not on statin therapy at the time of PCI procedure.
Main outcome measures
The primary outcome of this analysis was the 30-day composite of death, myocardial infarction, target vessel revascularization (TVR) or major bleeding.
Results
The primary outcome occurred in 7.9% patients (n = 246) in the statin group versus 9.8% (n = 143) in the non-statin group (P = 0.036). There was an interaction in univariate (P = 0.028) and multivariable (P = 0.026) analysis between pre-PCI statin therapy and the type of antithrombotic therapy regarding myocardial infarction. In the statin group, bivalirudin significantly reduced the incidence of major bleeding (2.6 vs. 4.3%, P = 0.013) with no significant difference in the incidence of myocardial infarction (4.9 vs. 5.2%; P = 0.73) compared with UFH. In the non-statin group, bivalirudin was inferior to UFH regarding the incidence of myocardial infarction (7.1 vs. 4.1%, P = 0.013), yet major bleeding remained lower among bivalirudin-treated patients (4.0 vs. 5.2%, P = 0.25).
Conclusion
This post-hoc analysis suggests the existence of an interaction between statin therapy before PCI and antithrombotic therapy during PCI. Patients receiving bivalirudin therapy at the time of PCI showed less periprocedural myocardial infarction when on pre-PCI statin therapy which has to be investigated in further studies.
Similar content being viewed by others
References
Ndrepepa G, Berger PB, Mehilli J, Seyfarth M, Neumann FJ, Schömig A, Kastrati A (2008) Periprocedural bleeding and 1-year outcome after percutaneous coronary interventions: appropriateness of including bleeding as a component of a quadruple end point. J Am Coll Cardiol 51:690–697
Lincoff AM, Bittl JA, Harrington RA et al (2003) Bivalirudin and provisional glycoprotein IIb/IIIa blockade compared with heparin and planned glycoprotein IIb/IIIa blockade during percutaneous coronary intervention: REPLACE-2 randomized trial. JAMA 289:853–863
Stone GW, White HD, Ohman EM, Bertrand ME, Lincoff AM, McLaurin BT, Cox DA, Pocock SJ, Ware JH, Feit F, Colombo A, Manoukian SV, Lansky AJ, Mehran R, Moses JW (2007) Bivalirudin in patients with acute coronary syndromes undergoing percutaneous coronary intervention: a subgroup analysis from the Acute Catheterization and Urgent Intervention Triage strategy (ACUITY) trial. Lancet 369:907–919
Stone GW, Witzenbichler B, Guagliumi G, Peruga JZ, Brodie BR, Dudek D, Kornowski R, Hartmann F, Gersh BJ, Pocock SJ, Dangas G, Wong SC, Kirtane AJ, Parise H, Mehran R (2008) Bivalirudin during primary PCI in acute myocardial infarction. N Engl J Med 358:2218–2230
Kastrati A, Neumann FJ, Mehilli J, Byrne RA, Iijima R, Büttner HJ, Khattab AA, Schulz S, Blankenship JC, Pache J, Minners J, Seyfarth M, Graf I, Skelding KA, Drischinger J, Richardt G, Berger PB, Schömig A (2008) ISAR-REACT 3 Trial investigators. Bivalirudin versus unfractionated heparin during percutaneous coronary intervention for angina pectoris. N Engl J Med 359:688–696
Stone GW, Ware JH, Bertrand ME, Lincoff AM, Moses JW, Ohman EM, White HD, Feit F, Colombo A, McLaurin BT, Cox DA, Manoukian SV, Fahy M, Clayton TC, Mehran R, Pocock SJ (2007) Antithrombotic strategies in patients with acute coronary syndromes undergoing early invasive management: one-year results from the ACUITY trial. JAMA 298:2497–2506
Ebrahimi R, Saleh J, Toggart E, Shah AP, Azmoon S, Babaei H, Lee J, Smith R, Movahed R, Rubin S (2008) Effect of preprocedural statin use on procedural myocardial infarction and major adverse cardiac adverse events in percutaneous coronary intervention: a meta-analysis. J Invasive Cardiol 20:292–295
Mood GR, Bavry AA, Roukoz H, Bhatt DL (2007) Meta-analysis of the role of statin therapy in reducing myocardial infarction following elective percutaneous coronary intervention. Am J Cardiol 100:919–923
Di Sciascio G, Patti G, Pasceri V, Gaspardone A, Colonna G, Montinaro A (2009) Efficacy of atorvastatin reload in patients on chronic statin therapy undergoing percutaneous coronary intervention: results of the ARMYDA-RECAPTURE (Atorvastatin for Reduction of Myocardial Damage During Angioplasty) Randomized Trial. J Am Coll Cardiol 54:558–565
Zhao JL, Yang YJ, Pei WD, Sun YH, Chen JL, Gao RL (2008) Effect of statin therapy on reperfusion arrhythmia in patients who underwent successful primary angioplasty. Clin Res Cardiol 97:147–151
Levine GN, Keaney JF Jr, Vita JA (1995) Cholesterol reduction in cardiovascular disease. Clinical benefits and possible mechanisms. N Engl J Med 332:512–521
Dangas G, Smith DA, Unger AH, Shao JH, Meraj P, Fier C, Cohen AM, Fallon JT, Badimon JJ, Ambrose JA (2000) Pravastatin: an antithrombotic effect independent of the cholesterol-lowering effect. Thromb Haemost 83:688–692
Wolfrum S, Grimm M, Heidbreder M, Dendorfer A, Katus HA, Liao JK, Richardt G (2003) Acute reduction of myocardial infarct size by a hydroxymethyl glutaryl coenzyme A reductase inhibitor is mediated by endothelial nitric oxide synthase. J Cardiovasc Pharmacol 41:474–480
Wolfrum S, Dendorfer A, Schutt M, Weidtmann B, Heep A, Tempel K, Klein HH, Dominiak P, Richardt G (2004) Simvastatin acutely reduces myocardial reperfusion injury in vivo by activating the phosphatidylinositide 3-kinase/Akt pathway. J Cardiovasc Pharmacol 44:348–355
van der Harst P, Böhm M, van Gilst WH, van Veldhuisen DJ (2008) The case for statin therapy in chronic heart failure. Clin Res Cardiol 97:139–146
Caron MF, McKendall GR (2003) Bivalirudin in percutaneous coronary intervention. Am J Health Syst Pharm 60:1841–1849
Ramana RK (2008) Lewis BE: percutaneous coronary intervention in patients with acute coronary syndrome: focus on bivalirudin. Vasc Health Risk Manag 4:493–505
Undas A, Brummel-Ziedins KE, Mann KG (2005) Statins and blood coagulation. Arterioscler Thromb Vasc Biol 25:287–294
Undas A, Celinska-Lowenhoff M, Brummel-Ziedins KE, Brozek J, Szczeklik A, Mann KG (2005) Simvastatin given for 3 days can inhibit thrombin generation and activation of factor V and enhance factor Va inactivation in hypercholesterolemic patients. Arterioscler Thromb Vasc Biol 25:1524–1525
Tousoulis D, Antoniades C, Bosinakou E, Kotsopoulou M, Tsioufis C, Tentolouris C, Trikas A, Pitsavos C, Stefanadis C (2005) Effects of atorvastatin on reactive hyperaemia and the thrombosis-fibrinolysis system in patients with heart failure. Heart 91:27–31
Avidan MS, Levy JH, van Aken H, Feneck RO, Latimer RD, Ott E, Martin E, Birnbaum DE, Bonfiglio LJ, Kajdasz DK, Despotis GJ (2005) Recombinant human antithrombin III restores heparin responsiveness and decreases activation of coagulation in heparin-resistant patients during cardiopulmonary bypass. J Thorac Cardiovasc Surg 130:107–113
Ridker PM, Danielson E, Fonseca FA, Genest J, Gotto AM Jr, Kastelein JJ, Koenig W, Libby P, Lorenzatti AJ, MacFadyen JG, Nordestgaard BG, Shepherd J, Willerson JT, Glynn RJ (2008) JUPITER Study Group. Rosuvastatin to prevent vascular events in men and women with elevated C-reactive protein. N Engl J Med 359:2195–2207
Iijima R, Ndrepepa G, Mehilli J, Byrne RA, Schulz S, Neumann FJ, Richardt G, Berger PB, Schömig A, Kastrati A (2009) Profile of bleeding and ischemic complications with bivalirudin and unfractionated heparin after percutaneous coronary intervention. Eur Heart J 30:290–296
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Khattab, A.A., Ndrepepa, G., Schulz, S. et al. Statin effect on thrombin inhibitor effectiveness during percutaneous coronary intervention: a post-hoc analysis from the ISAR-REACT 3 trial. Clin Res Cardiol 100, 579–585 (2011). https://doi.org/10.1007/s00392-011-0282-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-011-0282-7