Abstract
Introduction
Bone fractures in older adults involve hospitalization and surgical intervention, aspects that have been related to loss of autonomy and independence. Several variables have been studied as moderators of how these patients recover. However, the implications of cognitive plasticity for functional recovery have not been studied to date.
Objective
The present study analyzes the relationship between cognitive plasticity—defined as the capacity for learning or improved performance under conditions of training or performance optimization—and functional recovery in older adults hospitalized following a bone fracture.
Patients and methods
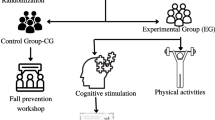
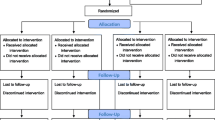
The study comprised 165 older adults who underwent surgery for bone fractures at a hospital in southern Spain. Participants were evaluated at different time points thereafter, with instruments that measure activities of daily life (ADL), namely the Barthel Index (BI) and the Lawton Index, as well as with a learning potential (cognitive plasticity) assessment test (Auditory Verbal Learning Test of Learning Potential, AVLT-LP).
Results
Results show that most of the participants have improved their level of independence 3 months after the intervention. However, some patients continue to have medium to high levels of dependency and this dependency is related to cognitive plasticity.
Conclusion
The results of this study reveal the importance of the cognitive plasticity variable for evaluating older adults hospitalized for a fracture. They indicate a possible benefit to be obtained by implementing programs that reduce the degree of long-term dependency or decrease the likelihood of it arising.
Zusammenfassung
Einführung
Knochenbrüche bei älteren Menschen bedeuten einen Krankenhausaufenthalt und chirurgische Intervention. Das sind Faktoren, die mit dem Verlust der Autonomie und der Unabhängigkeit in Zusammenhang stehen. Bisher wurden verschiedene Variablen als Einflussfaktoren auf die Heilung untersucht. Bisher nicht untersucht wurden Auswirkungen der kognitiven Plastizität auf die funktionelle Genesung.
Ziel
Die vorliegende Studie analysiert die Beziehung zwischen kognitiver Plastizität, definiert als Lernfähigkeit oder als Leistungssteigerung bei Training- oder Leistungsoptimierung, und funktioneller Genesung bei älteren Menschen im Krankenhaus nach Knochenfraktur.
Patienten und Methoden
In diese Studie wurden 165 ältere Patienten mit Knochenbrüchen eingeschlossen, die sich in einem Krankenhaus in Südspanien einer Operation unterzogen. Anschließend wurden zu verschiedenen Zeitpunkten tägliche Aktivitäten (ADL) mit dem Barthel-Index und dem Lawton-Index gemessen und ein Test zur Beurteilung der kognitiven Plastizität (Auditory Verbal Learning Test of Learning Potential, AVLT-LP) durchgeführt.
Ergebnisse
Die Ergebnisse zeigen, dass 3 Monate nach dem Eingriff eine Verbesserung der Unabhängigkeit bei den meisten Teilnehmern eintrat. Bei einigen jedoch bestand auch nach dieser Zeit weiterhin eine mittlere bis hohe Abhängigkeit, was im Zusammenhang mit der kognitiven Plastizität der Teilnehmer zu werten ist.
Schlussfolgerung
Die Ergebnisse dieser Studie zeigen die Bedeutung der Variable kognitive Plastizität für die Bewertung älterer Menschen, die mit einem Knochenbruch im Krankenhaus sind. Des Weiteren deuten sie auf einen möglichen Nutzen von Programmen hin, die den Grad einer langfristigen Abhängigkeit bzw. die Wahrscheinlichkeit, dass diese entsteht, verringern.

Similar content being viewed by others
References
Davies K, Collerton J, Jagger C et al (2010) Engaging the oldest old in research: lessons from the Newcastle 85 + study. BMC Geriatr 10:64. doi:10.1186/1471-2318-10-64
Gwozdz W, Sousa-Poza A (2010) Ageing, health and life satisfaction of the oldest old: an analysis for Germany. Soc Indic Res 97:397–417. doi:10.1007/s11205-009-9508-8
Singer T, Lindenberger U, Baltes PB (2003) Plasticity of memory for new learning in very old age: a story of major loss? Psychol Aging 18:306–317
Beaupre L, Cinats J, Jones C et al (2007) Does functional recovery in elderly hip fracture patients differ between patients admitted from long-term care and the community? J Gerontol 62A:1127
Castro C, García MT (2008) Cuidados en el paciente traumatológico. In: Guillen Llera F, Perez del Molino Martin J, Petidier Torregrossa R (eds) Síndromes y cuidados en el paciente geriátrico, 2ª edn. Elservier Masson, Barcelona, pp 385–396
Abianza P, Navarro JL, Romero L et al (2007) Upper extremity function an independent predictor of adverse events in hospitalized elderly. Gerontology 1:267–273
Luis PA, León RM, Domínguez PM (2007) Upper extremity function, an independent predictor of adverse events in hospitalized elderly. Gerontology 53:267–273
Delgado E, Suarez FN, Miniana JC (2009) Variables asociadas al deterioro funcional al alta y al los tres meses, en ancianos hospitalizados por insuficiencia cardiaca. Rev Esp Geriatr Gerontol 2:66–72
Feng L, Scherer S, Tan B et al (2010) Comorbid cognitive impairment and depression is a significant predictor of poor outcomes in hip fracture rehabilitation. Int Psychogeriatr 22:246
McGuire LC, Ford ES, Ajani UA (2006) The impact of cognitive functioning on mortality and the development of functional disability in older adults with diabetes: the second longitudinal study on aging. BMC Geriatr 1:1–7
Canga A, Narvaiza M (2006) Intervención de enfermería para disminuir las complicaciones derivadas de la hospitalización en los ancianos. Gerokomos 17:24–31
Vidan MT (1991) Inestabilidad y caídas. In: Ribera Casado JM, Cruz Jentoft yAJ (eds) Geriatria, 1ª edn. IDEPSA, Madrid, pp 75–81
Wakefield BJ, Holman JE (2007) Functional trajectories associated with hospitalization in older adults. West J Nurs Res 29:161–173
French FH, Torgerson DJ, Porter RW (1995) Cost analysis of fracture of the neck of femur. Age Ageing 24:185–189
Saénz MP, Gonzalez-Montalvo JI, Alarcon T, Madruga F (2006) Optimización del tratamiento médico en pacientes geriátricos con fractura de cadera. Influencia del equipo consultor geriátrico. Rev Esp Geriatr Gerontol 41:85–89
Jacelon CS (2004) Older adults and autonomy in acute care: increasing patients’ independence and control during hospitalization. J Gerontol Nurs 30:29–36
Covinsky KE, Pal Mer RM (2003) Loss of independence in activities of daily living in older adults hospitalized with medical illnesses: increased vulnerability with age. J Am Geriatr Soc 51:451–458
Varela L, Chavez H, Herrera A et al (2004) Valoración geriátrica integral en adultos mayores hospitalizados a nivel nacional. Diagnóstico 43:57–63
Gutiérrez J, Domínguez V, Solano JJ (1999) Deterioro funcional secundario a la hospitalización por enfermedad aguda en el anciano. Análisis de la incidencia y de los factores asociados. Rev Clin Esp 1:418–423
Feldt K, Finch M (2002) Older adults with hip fractures: treatment of pain following hospitalization. J Gerontol Nurs 28:27–35
Macias Montero MC, Guerrero Diaz MT, Hernandez Jimenez V (2008) Valoración Mental. In: Guillen Llera F, Perez del Molino Martín J, Petidier Torregrossa yR (eds) Sindromes y cuidados del paciente Geriatrico, 2ª edn. Elservier-Masson, Barcelona, pp 245–260
Calero-García MJ, Ortega AR, Navarro E et al (2012) Impact of admissions for bone fractures on the dependency ratio of adults over 65 years of age in southern Spain. Arch Gerontol Geriatr 55:305–309
Arenas L, Yaffe K, Covinsky K, Chren MM (2003) Cognitive screening predicts magnitude of functional recovery from admission to 3 months after discharge in hospitalized elders. J Gerontol 58A:37
Pedone C, Ercolani S, Catani M, Maggio D (2005) Elderly patients with cognitive impairment have a high risk for functional decline during hospitalization: the GIFA study. J Gerontol 60A:1576
Inouye SK (1994) The dilemma of delirium: clinical and research controversies regardimg diagnosis and evaluation of delirium in hospitalized elderly medical patients. Am J Med 97:278–288
Resnick B, Orwig D, Hawkes W et al (2007) The relation ship between psychosocial state and exercise behavior of older women 2 months after hip fracture. Rehabil Nurs 32:139–149
Gruber-Baldini A, Zimmerman S, Morrison R et al (2003) Cognitive impairment in hip fracture patients: timing of detection and longitudinal follow-up. J Am Geriatr Soc 51:1227–1236
Resnick B, Orwig D, Inguito P, Xi BB (2007) The baltimore hip studies projects: prevention of fracture through intervention. Symposium. Gerontological Society of America. Gerontologist 47:203
Stern P, y Cartensen L (2000) In: Stern P, Cartensen L (eds) The aging mind: opportunites in cognitive research, 1st edn. National Academy Press, Washington
Baltes M, Kuhl KP, Sowarka D, Gutzman H (1995) Potential of cognitive plasticity as a diagnostic instrument: a cross-validation and extension. Psychol Aging 10:167–172
Baltes M, Raykov T (1996) Prospective validity of cognitive plasticity in the diagnosis of mental status: a structural equation model. Neuropsychology 10:549–556
Calero MD, Navarro E (2004) Relationship between plasticity, mild cognitive impairment and cognitive decline. Arch Clin Neuropsychol 19:653–660
Raykov T, Baltes M, Neher K, Sowarka D (2002) A comparative study of two psychometric approaches to detect risk status for dementia. Gerontology 48:185–193
Calero MD, Navarro E (2007) Cognitive plasticity as a modulating variable on the effects of memory training in elderly persons. Arch Clin Neuropsychol 22:63–72
Calero MD, Navarro E, Muñoz-Manzano L (2007) Influence of level of activity on cognitive performance and cognitive plasticity in elderly persons. Arch Gerontol Geriatr 45:307–318
Vance D, Crowe M (2006) A proposed model of neuroplasticity and cognitive reserve in older adults. Act Adapt Aging 30:61–79
Calero MD, Navarro E (2011) Differences in cognitive performance, level of dependency and quality of life (QoL), related to age and cognitive status in a sample of Spanish old adults under and over 80 years of age. Arch Gerontol Geriatr 53:292–297
Navarro E, Calero MD, Lopez A et al (2008) Nivel de dependencia en la vida diaria y plasticidad cognitiva en la vejez. Escritos De Psicología 2:74–84
Folstein MF, Folstein SE, McHugh PR (1975) “Mini Mental state”. A practical method for the cognitive state of patiens for the clinician. J Psychiatr Res 12:189–198
Baztán JJ, Pérez J, Alarcón T et al (1993) Índice de Barthel: Instrumento válido para la valoración funcional de pacientes con enfermedad cerebrovascular. Rev Esp Geriatr Gerontol 28:32–40
Fernández de Larrinoa P, Martin M, Bulbena A (2001) Medición clínica de la demencia. Una guía de recursos. Into de Investigaciones Psiquiátricas, Bilbao
Lawton M, Brody P (1969). Assessment of older people: self-maintaining and instrumental activities daily living. Gerontologist 9:179–186
Cid J, Damián J (1997) Valoración de la discapacidad física: El índice de Barthel. 71:127–137
Sager MA, Rudberg MA, Jalaluddin M et al (1996) Hospital admission risk profile (HARP): identifying older patients at riks for functional decline following acute medical illness and hospitalization. J Am Geriatr Soc:251–257
Wiedl KH, Wienöbst J, Schöttke H (1999) Estimation rehabilitation potential in schizophrenic subjects. In: Böker F, Brenner HD, Genner yR (eds) Rehabilitation of cognitive disorders in schizophrenic patients. Huber, Bern
Wiedl KH, Schöttke H, Calero MD (2001) Dynamic assessment of cognitive rehabilitation potential in schizophrenic persons and in old people with and without dementia. Int J Psychol Assess 17:112–119
Rey A (1958) L’examen Clinique en Psychologia Press Universitaire de France. Paris
Calero MD, Navarro E (2006) La plasticidad cognitiva en la vejez. Técnicas de Evaluación e intervención. Octaedro, Barcelona
Fernández-Ballesteros R, Zamarrón MD, Tárraga LL (2005) Learning potential: a new method for assessing cognitive impairment. Int Psychogeriatr 17:119–128
Navarro E, Calero MD (2009) Estimation of cognitive plasticity in old adults using dynamic assessment techniques. J Cogn Educ Psychol 8:38–51
Wiedl KH, Schöttke H, Calero MD (2001) Dynamic assessment of cognitive rehabilitation potential in schizophrenic persons and in old people with and without dementia. Int J Psychol Assess 17:112–119
Fernández-Ballesteros R, Zamarrón MD, Tárraga L et al (2003) Cognitive plasticity in healthy, mild cognitive impairment subjects and Alzheimer’s disease patients: a research Project in Spain. Eur Psychol 8:148–159
Watzke S, Brieger P, y Wiedl K (2009) Prediction of vocational rehabilitation outcome in schizophrenia: incremental prognostic validity of learning potential beyond basic cognitive performance. J Cogn Educ Psychol 8:52–62
Fernández-Ballesteros R, Botella J, Zamarrón MD et al (2012) Cognitive plasticity in normal and pathological aging. Clin Interv Aging 7:15–25
Calero MD, Y Navarro E (2004) Relation between plasticity, mild cognitive impairment and cognitive decline. Arch Clin Neuropsychol 19:623–660
Compliance with ethical guidelines
Conflict of interest. M.J. Calero-García, M.D. Calero, E. Navarro and A.R.Ortega state that there are no conflicts of interest. All studies on humans described in the present manuscript were carried out with the approval of the responsible ethics committee and in accordance with national law and the Helsinki Declaration of 1975 (in its current, revised form). Informed consent was obtained from all patients included in studies.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Calero-García, M., Calero, M., Navarro, E. et al. Cognitive plasticity as a moderator of functional dependency in elderly patients hospitalized for bone fractures. Z Gerontol Geriat 48, 22–28 (2015). https://doi.org/10.1007/s00391-014-0610-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00391-014-0610-4
Keywords
- Gerontology
- Bartel Index
- Quality of life
- Activities of daily life
- Instrumental activities of daily life