Abstract
Background
Experimental evidence has revealed that phosphodiesterase five inhibitors (PDE5is) increase epithelial barrier function and suppress intestinal carcinogenesis. Few epidemiological studies have investigated the role of PDE5i in increasing the risk of colorectal cancer (CRC); however, these studies have proffered varying conclusions. We therefore aimed to perform a comprehensive review and meta-analysis to investigate whether PDE5i use is associated with the incidence of CRC.
Methods
Databases, namely, PubMed, Scopus, Embase, and Web of Science, were used for literature search. Observational studies (published until January 31, 2021) that assessed the association of PDE5i use with CRC incidence were considered. Pooled relative risk (RR) estimates and corresponding 95% confidence intervals (CIs) were calculated using the DerSimonian-Laird random-effects model.
Results
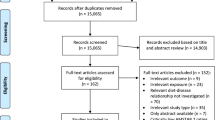
We identified four retrospective studies that involved 965,044 participants and 3,518 CRC cases detected during a mean follow-up of 12.7 years. Pooled results indicated a significantly reduced CRC risk among all PDE5i users (RR, 0.85; 95% CI, 0.76–0.95; P = 0.004, I2 = 63%). Moreover, continuous use of PDE5i was associated with a significantly reduced risk of CRC (RR, 0.63; 95% CI, 0.59–0.68; P < 0.001, I2 = 0.0%). However, the type of PDE5i exhibited no association with the risk of CRC (RR, 1.00; 95% CI, 0.98–1.02; I2 = 84.7%).
Conclusion
Our findings suggest that continuous use of PDE5i was associated with a significantly reduced risk of CRC development. Future studies with a longitudinal design and adequate control of confounding factors are required to clarify whether a longer duration of PDE5i use alters the risk of CRC.





Similar content being viewed by others
Data availability
The data underlying this article will be shared on reasonable request to the corresponding author.
References
Peak TC, Richman A, Gur S, Yafi FA, Hellstrom WJG (2016) The role of PDE5 inhibitors and the NO/cGMP pathway in cancer. Sex Med Rev 4(1):74–84. https://doi.org/10.1016/j.sxmr.2015.10.004
Bian K, Murad F. sGC-cGMP signaling: target for anticancer therapy. Adv Fetal Neonatal Physiol 2014;5–13
Aoun F, Slaoui A, Walid AHO et al (2018) Association between phosphodiesterase type 5 inhibitors and prostate cancer: a systematic review. Prog Urol 28(12):560–566. https://doi.org/10.1016/j.purol.2018.07.004
Wu Y, Qu X, Wang Y et al (2019) Effect of phosphodiesterase type 5 inhibitors on prostate cancer risk and biochemical recurrence after prostate cancer treatment: A systematic review and meta-analysis. Andrologia 51(2):e13198. https://doi.org/10.1111/and.13198
Loeb S, Ventimiglia E, Salonia A, Folkvaljon Y, Stattin P (2017) Meta-analysis of the association between phosphodiesterase inhibitors (PDE5Is) and risk of melanoma. J Natl Cancer Inst 109(8). https://doi.org/10.1093/jnci/djx086
Loeb S, Folkvaljon Y, Lambe M et al (2015) Use of Phosphodiesterase type 5 inhibitors for erectile dysfunction and risk of malignant melanoma. JAMA 313(24):2449–2455. https://doi.org/10.1001/jama.2015.6604
Lin S, Wang J, Wang L et al (2017) Phosphodiesterase-5 inhibition suppresses colonic inflammation-induced tumorigenesis via blocking the recruitment of MDSC. Am J Cancer Res 7(1):41–52
Zhu B, Vemavarapu L, Thompson WJ, Strada SJ (2005) Suppression of cyclic GMP-specific phosphodiesterase 5 promotes apoptosis and inhibits growth in HT29 cells. J Cell Biochem 94(2):336–350. https://doi.org/10.1002/jcb.20286
Mei X-L, Yang Y, Zhang Y-J et al (2015) Sildenafil inhibits the growth of human colorectal cancer in vitro and in vivo. Am J Cancer Res 5(11):3311–3324
Islam BN, Sharman SK, Hou Y et al (2017) Sildenafil suppresses inflammation-driven colorectal cancer in mice. Cancer Prev Res (Phila) 10(7):377–388. https://doi.org/10.1158/1940-6207.Capr-17-0015
Sutton SS, Magagnoli J, Cummings TH, Hardin JW (2020) The association between phosphodiesterase-5 inhibitors and colorectal cancer in a national cohort of patients. Clin Transl Gastroenterol 11(6):e00173. https://doi.org/10.14309/ctg.0000000000000173
Cea Soriano L, García Rodríguez LA (2020) No association between use of phosphodiesterase 5 inhibitors and colorectal cancer in men with erectile dysfunction. Pharmacoepidemiol Drug Saf 29(5):605–608. https://doi.org/10.1002/pds.5000
Cronin KA, Lake AJ, Scott S et al (2018) Annual report to the nation on the status of cancer, part I: national cancer statistics. Cancer 124(13):2785–2800
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ 339:b2535. https://doi.org/10.1136/bmj.b2535
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D, Moher D, Becker BJ, Sipe TA, Thacker SB (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of Observational Studies in Epidemiology (MOOSE) group. JAMA 283(15):2008–2012
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605
Higgins JP, Thompson SG (2002) Quantifying heterogeneity in a meta-analysis. Statistics Med 21:1539–1558
Huang W, Sundquist J, Sundquist K, Ji J (2019 Sep) Use of phosphodiesterase 5 inhibitors is associated with lower risk of colorectal cancer in men with benign colorectal neoplasms. Gastroenterology 157(3):672-681.e4. https://doi.org/10.1053/j.gastro.2019.05.012
Matthews A, Langan SM, Douglas IJ, Smeeth L, Bhaskaran K (2016) Phosphodiesterase type 5 inhibitors and risk of malignant melanoma: matched cohort study using primary care data from the UK clinical practice research datalink. PLoS Med 13(6):e1002037. https://doi.org/10.1371/journal.pmed.1002037
Tinsley HN, Gary BD, Thaiparambil J, Li N, Lu W, Li Y, Maxuitenko YY, Keeton AB, Piazza GA (2010) Colon tumor cell growth–inhibitory activity of sulindac sulfide and other nonsteroidal anti-inflammatory drugs is associated with phosphodiesterase 5 inhibition. Cancer Prev Res 3(10):1303–1313
Mei XL, Yang Y, Zhang YJ, Li Y, Zhao JM, Qiu JG, Zhang WJ, Jiang QW, Xue YQ, Zheng DW, Chen Y (2015) Sildenafil inhibits the growth of human colorectal cancer in vitro and in vivo. Am J Cancer Res 5(11):3311
Cruz-Burgos M, Losada-Garcia A, Cruz-Hernández CD, Cortés-Ramírez SA, Camacho-Arroyo I, Gonzalez-Covarrubias V, Morales-Pacheco M, Trujillo-Bornios SI, Rodríguez-Dorantes M (2021) New approaches in oncology for repositioning drugs: the case of PDE5 inhibitor sildenafil. Front Oncol 11:208
Author information
Authors and Affiliations
Contributions
Principal investigators of the study: ASB. Data collection and analysis: ASB and KVS. Literature review: ASB, KVS, and WT. Writing: ASB and WT. Manuscript revision: ASB, KVS, and WT. All authors read and approved the final paper.
Corresponding author
Ethics declarations
Ethics approval
No ethical approval will be needed because data were acquired from previously published studies.
Informed consent
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bhagavathula, A.S., Tesfaye, W. & Vidyasagar, K. Phosphodiesterase type 5 inhibitors use and risk of colorectal cancer: a systematic review and meta-analysis. Int J Colorectal Dis 36, 2577–2584 (2021). https://doi.org/10.1007/s00384-021-04022-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-021-04022-5