Abstract
Objectives
To evaluate comparative outcomes of laparoscopic mesh rectopexy (LMR) and laparoscopic posterior sutured rectopexy (LPSR) in patients with rectal prolapse.
Methods
We conducted a systematic search of electronic databases and bibliographic reference lists with application of a combination of free text and controlled vocabulary search adapted to thesaurus headings, search operators, and limits. Recurrence, Cleveland Clinic Incontinence Score (CCIS), Cleveland Clinic Constipation Score (CCCS), surgical site infections, procedure time, and length of hospital stay were the evaluated outcome measures.
Results
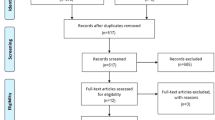
We identified 5 comparative studies reporting a total of 307 patients evaluating outcomes of LMR (n=160) or LPSR (n=147) in patients with rectal prolapse. LMR was associated with significantly lower recurrence rate (OR: 0.28, P=0.009) but longer procedure time (MD: 23.93, P<0.0001) compared to LPSR. However, there was no significant difference in CCIS (MD: −1.02, P=0.50), CCCS (MD: −1.54, P=0.47), surgical site infection (OR: 1.48, P=0.71), and length of hospital stay (MD: −1.54, P=0.47) between two groups. No mesh erosion was reported in any of the included studies at maximum follow-up point. Sub-group analyses with respect to ventral mesh rectopexy, posterior mesh rectopexy, randomised studies, and adult patients were consistent with the main analysis.
Conclusions
LMR seems to be associated with lower recurrence but longer procedure time compared to LPSR. Although no mesh-related complications have been reported by the included studies, no definitive conclusions can be made considering that the included studies were inadequately powered for such outcome. Future high-quality randomised studies with adequate sample size are required.



Similar content being viewed by others
References
Ahmad N, Stefan S, Adukia V, Naqvi S, Khan J (2018) Laparoscopic ventral mesh rectopexy: functional outcomes after surgery. Surg J 04(04):e205–e211
Felt-Bersma RJ, Cuesta MA (2001) Rectal prolapse, rectal intussusception, rectocele, and solitary rectal ulcer syndrome. Gastroenterol Clin N Am 30:199–222
Parks AG, Swash M, Urich H (1977) Sphincter denervation in anorectal incontinence and rectal prolapse. Gut 18:656–665
Azimuddin K, Khubchandani IT, Rosen L et al (2001) Rectal prolapse: a search for the best operation. Am Surg 67:622–627
Schiedeck TH, Schwandner O, Scheele J, Farke S, Bruch HP (2005) Rectal prolapse: which surgical option is appropriate? Langenbecks Arch Surg 390:8–14
Faucheron JL, Trilling B, Girard E, Sage PY, Barbois S, Reche F (2015) Anterior rectopexy for full-thickness rectal prolapse: technical and functional results. World J Gastroenterol 21:5049–5055
Brown RA, Ellis CN (2014) The role of synthetic and biologic materials in the treatment of pelvic organ prolapse. Clin Colon Rectal Surg. 27(4):182–190
Liberati A, Altman DG, Tetzlaff J et al (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ 339:b2700
Jorge JMN, Wexner SD (1993) (1993). Etiology and management of fecal incontinence. Dis Colon Rectum 36(1):77–97
Agachan F, Chen T, Pfeifer J, Reissman P, Wexner SD (1996) A constipation scoring system to simplify evaluation and management of constipated patients. Dis Colon Rectum 39(6):681–685
Higgins JP, Altman DG, editors Chapter 8 (2018) Assessing risk of bias in included studies. In: Higgins JP, Green S, editors. Cochrane handbook for systematic reviews of interventions. Version 5.0.4 Available at: http://hiv.cochrane.org/sites/hiv.cochrane.org/files/uploads/Ch08_Bias.pdf
Wells GA, Shea B, O’Connell D, Peterson J, Welch V, Losos M, Tugwell P. The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. Available at: http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. November 28, 2018
Hozo S, Djulbegovic B, Hozo I (2005) Estimating the mean and variance from the median, range, and the size of a sample. BMC Medical Research Methodology 5:13
Higgins JP, Altman DG, editors. Chapter 8: Assessing risk of bias in included studies. In: Higgins JP, Green S, editors. Cochrane handbook for systematic reviews of interventions. Version 5.0.1 [updated September 2008]. Available at: http://hiv.cochrane.org/sites/hiv. cochrane.org/files/uploads/Ch08_Bias.pdf. Accessed April 21, 2020
Sahoo MR, Thimmegowda AK, Gowda MS (2014) A single centre comparative study of laparoscopic mesh rectopexy versus suture rectopexy. J Minim Access Surg 10(1):18–22. https://doi.org/10.4103/0972-9941.124456.
Lundby L, Iversen LH, Buntzen S, Wara P, Høyer K, Laurberg S (2016) Bowel function after laparoscopic posterior sutured rectopexy versus ventral mesh rectopexy for rectal prolapse: a double-blind, randomised single-centre study. Lancet Gastroenterol Hepatol. 1(4):291–297
Luglio G, Tarquini R, Giglio MC, Sollazzo V, Peltrini R, Sacco M, Spiezio G, Amato B, De Palma GD, Bucci L (2017) Ventral mesh rectopexy versus conventional suture technique: a single-institutional experience. Aging Clin Exp Res. 29(Suppl 1):79–82
Hidaka J, Elfeki H, Duelund-Jakobsen J, Laurberg S, Lundby L (2019) Functional outcome after laparoscopic posterior sutured rectopexy versus ventral mesh rectopexy for rectal prolapse: six-year follow-up of a double-blind, randomized single-center study. EClinicalMedicine 16:18–22
Yehya A, Gamaan I, Abdelrazek M, Shahin M, Seddek A, Abdelhafez M (2020) Laparoscopic suture versus mesh rectopexy for the treatment of persistent complete rectal prolapse in children: a comparative randomized study. Minim Invasive Surg 2020:3057528. https://doi.org/10.1155/2020/3057528.
Emile SH, Elfeki HA, Youssef M, Farid M, Wexner SD (2017) Abdominal rectopexy for the treatment of internal rectal prolapse: a systematic review and meta-analysis. Colorectal Dis. 19(1):O13–O24
D’Hoore A, Cadoni R, Penninckx F (2004) Long-term outcome of laparoscopic ventral rectopexy for total rectal prolapse. Br J Surg. 91(11):1500–1505
Wong M, Meurette G, Abet E, Podevin J, Lehur PA (2011) Safety and efficacy of laparoscopic ventral mesh rectopexy for complex rectocele. Colorectal Dis 13(9):1019–1023
D’Hoore A, Penninckx F (2006) Laparoscopic ventral recto(colpo)pexy for rectal prolapse: surgical technique and outcome for 109 patients. Surg Endosc. 20(12):1919–1923
Ahmad M, Sileri P, Franceschilli L, Mercer-Jones M (2012) The role of biologics in pelvic floor surgery. Colorectal Dis. 14(3, Suppl 3):19–23
Emile SH, Elbanna H, Youssef M, Thabet W, Omar W, Elshobaky A et al (2017) Laparoscopic ventral mesh rectopexy vs Delorme's operation in management of complete rectal prolapse: a prospective randomized study. Colorectal Disease 19(1):50–57
De Oliveira O Jr, Stein SL, Trencheva KI, Sonoda T, Milsom JW, Lee SW (2010) Comparative outcomes of elderly patients undergoing Altemeier procedure versus laparoscopic rectopexy for rectal prolapse. Asian Journal of Endoscopic Surgery 3(1):28–32
Funding
There are no funding sources for this work and no conflicts of interest and financial disclosures for the authors
Author information
Authors and Affiliations
Contributions
Conception and design: Shahin H and Shahab H
Literature search and study selection: Shahin H and Shahab H
Data collection: Shahin H and Shahab H
Analysis and interpretation: Shahin H and Shahab H
Writing the article: Shahin H and Shahab H
Critical revision of the article: All authors
Final approval of the article: All authors
Statistical analysis: Shahin H and Shahab H
Corresponding author
Ethics declarations
Competing interests
The authors declare competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendix
Appendix
Search No | Search strategy* |
#1 | MeSH descriptor: [mesh rectopexy] explode all trees |
#2 | mesh rectopexy: TI,AB,KW |
#3 | MeSH descriptor: [sutured rectopexy] explode all trees |
#4 | sutured rectopexy: TI,AB,KW |
#5 | #1 OR #2 OR #3 OR #4 |
#6 | MeSH descriptor: [laparoscopic] explode all trees |
#7 | laparoscopic: TI,AB,KW |
#8 | MeSH descriptor: [abdominal rectopexy] explode all trees |
#9 | abdominal rectopexy: TI,AB,KW |
#10 | #6 OR #7 OR #8 OR #9 |
#11 | #5 AND #10 |
Rights and permissions
About this article
Cite this article
Hajibandeh, S., Hajibandeh, S., Arun, C. et al. Meta-analysis of laparoscopic mesh rectopexy versus posterior sutured rectopexy for management of complete rectal prolapse. Int J Colorectal Dis 36, 1357–1366 (2021). https://doi.org/10.1007/s00384-021-03883-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-021-03883-0