Abstract
Background
The incidence of rectal cancer has meaningfully increased in young patients. However, quantitative evaluation for the competing data of early-onset rectal cancer is lacking. So, we performed a competing risk analysis to calculate the cumulative incidence of death for patients with early-onset rectal cancer and developed a nomogram to predict the probability of cancer-specific mortality for these patients.
Methods
We abstracted data of patients with early-onset rectal cancer between 2004 and 2016 by using the Surveillance, Epidemiology, and End Results program database. The cumulative incidence function was used to calculate the crude cancer-specific mortality of early-onset rectal cancer. Fine and Gray’s proportional sub-distribution hazard model was adopted to explore the risk factors of cancer-specific death. Then, we establish a nomogram to predict their 3-, 5-, and 10-year probabilities.
Results
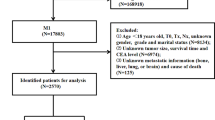
We identified 9917 patients with early-onset rectal cancer, and they were randomly divided into training (n = 6941) and validation (n = 2976) cohorts. In the training cohort, the 3-, 5-, and 10-year cumulative incidences of cancer-specific death after diagnosis for early-onset rectal cancer were 11.4%, 19.9%, and 28.8%, respectively. Fine and Gray’s model showed that sex, race, marital status, histology, T stage, N stage, M stage, examined lymph nodes, and pretreatment carcinoembryonic antigen were independently associated with cancer-specific mortality. Such factors were selected to develop a prognostic nomogram.
Conclusion
The competing risk nomogram has an ideal performance for predictive cancer-specific mortality in early-onset rectal cancer.




Similar content being viewed by others
Change history
24 March 2020
The original version of this article, unfortunately, contained errors.
References
Russell MC, You YN, Hu CY et al (2013) A novel risk-adjusted nomogram for rectal cancer surgery outcomes. JAMA Surg 8:769–777
Chong VH, Telisinghe PU, Bickle I et al (2015) Increasing incidence of colorectal cancer, starting at a younger age for rectal compared to colon cancer in Brunei Darussalam. Asian Pac J Cancer Prev 12:5063–5067
Murphy CC, Sanoff Hanna K, Stitzenberg Karyn B et al (2017) Patterns of sociodemographic and clinicopathologic characteristics of stages II and III colorectal cancer patients by age: examining potential mechanisms of young-onset disease. J Cancer Epidemiol 2017:4024580
Watson R, Liu TC, Ruzinova MB (2016) High frequency of KRAS mutation in early onset colorectal adenocarcinoma: implications for pathogenesis. Hum Pathol 56:163–170
Guthrie GJ, Charles KA, Roxburgh CS, Horgan PG, McMillan DC, Clarke SJ (2013) The systemic inflammation-based neutrophil-lymphocyte ratio: experience in patients with cancer. Crit Rev Oncol Hematol 88:218–230
Hussain N, Gahine R, Mourya J et al (2013) Colorectal cancer in young adults in a tertiary care hospital in Chhattisgarh, Raipur. Indian J Cancer 50:337–340
Manias E, Aitken R, Dunning T (2001) Colorectal adenocarcinoma in patients under 45 years of age: comparison with older patients in a well-defined French population. Dis Colon Rectum 44:380–387
Yeo SA, Chew MH, Koh PK, Tang CL (2013) Young colorectal carcinoma patients do not have a poorer prognosis: a comparative review of 2,426 cases. Tech Coloproctol 17(6):653–661
Bibbins-Domingo K, Grossman DC, Curry SJ et al (2008) Screening for colorectal cancer: US preventive services task force recommendation statement. Ann Intern Med 315:627–637
Zhang ZY, Luo QF, Yin XW et al (2016) Nomograms to predict survival after colorectal cancer resection without preoperative therapy. BMC Cancer 16:658–679
Balachandran VP, Gonen M, Smith JJ et al (2015) Nomograms in oncology: more than meets the eye. Lancet Oncol 16:173–180
Van GW, Van Stiphout RG, Van DVCJH et al (2015) Nomograms to predict survival and the risk for developing local or distant recurrence in patients with rectal cancer treated with optional short-term radiotherapy. Ann Oncol 26:928–935
Peng J, Ding Y, Tu S et al (2014) Prognostic nomograms for predicting survival and distant metastases in locally advanced rectal cancers. PLoS One 9:e106344
Valentini V, van Stiphout RG, Lammering G et al (2011) Nomograms for predicting local recurrence, distant metastases, and overall survival for patients with locally advanced rectal cancer on the basis of European randomized clinical trials. J Clin Oncol 29:3163
Van Stiphout RG, Valentini V, Buijsen J et al (2014) Nomogram predicting response after chemoradiotherapy in rectal cancer using sequential PETCT imaging: a multicentric prospective study with external validation. Radiother Oncol 113:215–222
Van Walraven C, McAlister FA (2016) Competing risk bias was common in Kaplan-Meier risk estimate published in prominent medical journals. J Clin Epidemiol 69:170–173
Li JQ, Li X, Gu GH, Ma XT et al (2018) A competing-risks nomogram for predicting probability of death from CRC in Chinese Han patients with stage I-III CRC. Jpn J Clin Oncol 48:1088–1095
Wolkewitz M, Cooper BS, Bonten MJ, Barnett AG, Schumacher M (2014) Interpreting and comparing risks in the presence of competing risks. BMJ 349:g5060
Latouche A, Aliqnol A, Beyersmann J, Labopin M, Fine JP (2013) A competing risks analysis should report results on all cause-specific hazards and cumulative incidence functions. J Clin Epidemiol 6:648–653
Parpia S, Thabane L, Julian JA, Whelan TJ, Levine MN (2013) Empirical comparison of methods for analyzing multiple time-to-event outcomes in a non-inferiority trial: a breast cancer study. BMC Med Res Methodol 13:44
Fang C, Wang W, Feng W et al (2017) Nomogram individually predicts the overall survival of patients with gastroenteropancreatic neuroendocrine neoplasms. Br J Cancer 117:1544–1550
Sun F, Ma K, Yang X, Li M, Shi Y, Zhan C, Jiang W, Wang Q (2017) A nomogram to predict prognosis after surgery in early stage non-small cell lung cancer in elderly patients. Int J Surg 42:11–16
Zhang J, Gong Z, Gong Y (2019) Development and validation of nomograms for prediction of overall survival and cancer-specific survival of patients with stage IV colorectal cancer. Jpn J Clin Oncol 49:438–446
Markl B (2015) Stage migration vs immunology: the lymph node count story in colon cancer. World J Gastroenterol 21:12218–12233
May M, Herrmann E, Bolenz C, Brookman-May S, Tiemann A, Moritz R, Fritsche HM, Burger M, Trojan L, Michel MS, Wülfing C, Müller SC, Ellinger J, Buchner A, Stief CG, Tilki D, Wieland WF, Gilfrich C, Höfner T, Hohenfellner M, Haferkamp A, Roigas J, Zacharias M, Bastian PJ (2011) Association between the number of dissected lymph nodes during pelvic lymphadenectomy and cancer-specific survival in patients with lymph node-negative urothelial carcinoma of the bladder undergoing radical cystectomy. Ann Surg Oncol 18:2018–2025
Xu C, Liu X, Chen YP et al (2017) Impact of marital status at diagnosis on survival and its change over time between 1973 and 2012 in patients with nasopharyngeal carcinoma: a propensity score-matched analysis. Cancer Med 6:3040–3051
Iwashyna TJ, Christakis NA (2004) Marriage, widowhood, and health-care use. Soc Sci Med 57:2137–2147
Carlsson S, Maschino A, Schröder F et al (2013) A novel risk-adjusted nomogram for rectal cancer surgery outcomes. JAMA Surg 148:769–777
Yao HH, Shao F, Huang Q, Wu Y, Qiang Zhu Z, Liang W (2014) Nomogram to predict anastomotic leakage after laparoscopic anterior resection with intracorporeal rectal transection and double-stapling technique anastomosis for rectal cancer. Hepato-gastroenterology 61:1257–1261
Jwa E, Kim JH, Han S, Park JH, Lim SB, Kim JC, Hong YS, Kim TW, Yu CS (2014) Nomogram to predict ypN status after chemoradiation in patients with locally advanced rectal cancer. Br J Cancer 111:249–254
Acknowledgments
The authors would like to thank SEER for open access to their database. The opinions expressed in this study are those of the authors and do not represent the opinions of the National Cancer Institute.
Funding
This project was funded by Natural Science Foundation of Guangdong (2015A030313827), Guangdong Province Medical Scientific Research Fund Project (No. A2019537), Competitive Project of Financial Special Funds for Science and Technology of Zhanjiang (2018A01026), Guangdong Medical University Scientific Research Fund Project (GDMUM201806), and The Affiliated Hospital of Guangdong Medical University Clinical Research Program (LCYJ2018C004).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
All procedures performed in studies involving human participants were following the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, Y., Wu, J., He, H. et al. Nomogram predicting cancer-specific mortality in early-onset rectal cancer: a competing risk analysis. Int J Colorectal Dis 35, 795–804 (2020). https://doi.org/10.1007/s00384-020-03527-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-020-03527-9