Abstract
Background
Controversial data exists in the current literature in regard to the use of neoadjuvant chemoradiation (nCRT) in patients with clinical T3N0 (cT3N0) rectal cancers, specifically based on location and relation to peritoneal reflection. We aimed to analyze the impact of nCRT on oncologic outcomes among cT3N0 rectal cancers, depending on the tumor height from anal verge (AV).
Methods
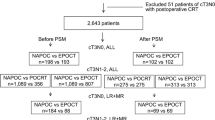
A retrospective analysis of patients with cT3N0 rectal cancers was included from a query of a prospectively maintained rectal cancer database from 1980 to 2016. Patients were divided into 3 groups based on the tumor height: low (1–5 cm from AV), mid (6–10 cm from AV), and upper (11–15 cm from AV). Patients were stratified by use of nCRT. Main outcomes: 5-year overall survival (OS), disease-free survival (DFS), cancer-specific survival (CSS), and local recurrence (LR) using Kaplan-Meier curves.
Results
Five hundred ninety-two patients were included. Overall, 364 (61.4%) patients received nCRT and 228 (38.6%) patients did not. There were 251 (43%) patients with low, 302 (51%) with mid, and 39 (7%) with upper rectal cancer. Patients with low and mid rectal cancers received nCRT more frequently than those with upper rectal cancers (68.5% and 61.2% vs 43.6%, p = 0.007). The 5-year OS was 78% and 63%, DFS—88% and 73%, LR—1% and 8% in nCRT followed by resection vs. surgery alone (p < 0.001). In regard to cancer location after nCRT compared with surgery alone, low and mid cancers had better OS, DFS, and CSS, compared with upper ones.
Conclusion
nCRT prolongs survival among patients with rectal cancer below 10 cm from AV; however, it has no effect on 5-year oncologic survival of patients with upper rectal cancer located below peritoneal reflection.


Similar content being viewed by others
References
Tural D, Yildiz O, Elcin O, Erdamar S, Guney S, Demireli F, Buyukunal E, Serdengecti S (2014) What is the optimal treatment in clinical stage T3N0M0 rectal cancer? JBUON 19(1):97–102
Heald RJ, Husband M, Ryall RD (1982) The mesorectum in rectal cancer surgery–the clue to pelvic recurrence? Br J Surg 69:613–616
Morino M, Risio M, Bach S, Beets-Tan R, Bujko K, Panis Y, Quirke P, Rembacken B, Rullier E, Saito Y, Young-Fadok T, Allaix ME, European Association for Endoscopic Surgery, European Society of Coloproctology, European Association for Endoscopic Surgery; European Society of Coloproctology (2015) Early rectal cancer: the European Association for Endoscopic Surgery (EAES) clinical consensus conference. Surg Endosc 29(4):755–773
Stitzenberg KB, Sanoff HK, Penn DC, Meyers MO, Tepper JE (2013) Practice patterns and long-term survival for early-stage rectal cancer. J Clin Oncol 31(34):4276–4282
Bergquist J, Thiels C, Shubert C, Habermann EB, Hayman AV, Zielinski MD, Mathis KL (2016) Is chemotherapy or radiation therapy in addition to surgery beneficial for locally advanced rectal cancer in the elderly? A national cancer data base (NCBD study). World J Surg 40:447–455
Kim N, Baik S, Seong J et al (2006) Oncologic outcomes after neoadjuvant chemoradiation followed by curative resection with tumor-specific mesorectal excision for fixed locally advanced rectal cancer. Ann Surg 244(6):1024–1029
Lombardi R, Cuicchi D, Pinto C et al (2010) Clinically-staged T3N0 rectal cancer: is preoperative chemoradiotherapy the optimal treatment? Ann Surg Onc 17:838–845
Park I, Kim J, Yu C, Lee JS, Lim SB, Lee JL, Yoon YS, Kim CW, Kim JC (2016) Preoperative chemotherapy for clinically diagnosed T3N0 rectal cancer. Surg Today 46:90–96
Balyasnikova S, Brown G (2016) Optimal imaging strategies for rectal cancer staging and ongoing management. Curr Treat Options in Oncol 17(6):32
Videhult P, Smedh K, Lundin P, Kraaz W (2007) Magnetic resonance imaging for preoperative staging of rectal cancer in clinical practice: high accuracy in predicting circumferential margin with clinical benefit. Color Dis 9(5):412–419
Guillem J, Diaz-Gonzalez J, Minsky B et al (2008) cT3N0 rectal cancer: potential overtreatment with preoperative chemoradiotherpay is warranted. J Clin Oncol 26:368–373
Akeel N, Lan N, Stocchi L, Costedio MM, Dietz DW, Gorgun E, Kalady MF, Karagkounis G, Kessler H, Remzi FH (2017) Clinically node negative, pathologically node positive rectal cancer patients who did not receive neoadjuvant therapy. J Gastrointest Surg 21:49–55
Delitto D, George T, Loftus T et al (2018) Prognostic value of clinical vs pathological stage in rectal cancer patietns receiving neoadjuvamt therapy. JNCI J Natl Cancer Inst 110(5):460–465
Gourtsoyianni S, Papanikolaou N (2016) Role of magnetic resonance imaging in primary rectal cancer-standard protocol and beyond. Semin Ultrasound CT MR 37(4):323–330
Beets-Tan RGH, Lambregts DMJ, Maas M, Bipat S, Barbaro B, Curvo-Semedo L, Fenlon HM, Gollub MJ, Gourtsoyianni S, Halligan S, Hoeffel C, Kim SH, Laghi A, Maier A, Rafaelsen SR, Stoker J, Taylor SA, Torkzad MR, Blomqvist L (2018) Magnetic resonance imaging for clinical management of rectal cancer: updated recommendations from the 2016 European Society of Gastrointestinal and Abdominal Radiology (ESGAR) consensus meeting. Eur Radiol 28(4):1465–1475
Hwang MR, Park JW, Kim DY et al (2010) Prognostic impact of peritonealisation in rectal cancer treated with preoperative chemoradiotherapy: extraperitoneal versus intraperitoneal rectal cancer. Radiother Oncol 94(3):353–358
Delaney CP, Lavery IC, Brenner A, Hammel J, Senagore AJ, Noone RB, Fazio VW (2002) Preoperative radiotherapy improves survival for patients undergoing total mesorectal excision for stage T3 low rectal cancers. Ann Surg 236(2):203–207
Huang M, Lee H, Tsai H et al (2018) Comparison of efficacy and safety of preoperative chemoradiotherapy in locally advanced upper and middle/lower rectal cancer. Radiat Oncol 13:53
Marinello FG, Frasson M, Baguena G et al (2015) Selective approach for upper rectal cancer treatment: total mesorectal excision and preoperative chemoradiation are seldom necessary. Dis Col Rectum 58:556–565
Rosenberg R, Maak M, Schuster S et al (2010) Does a rectal cancer of the upper third behave more like a colon or a rectal cancer? Dis Colon Rectum 53(5):761–770
Gietelink L, Wouters M, Marijnen C, van Groningen J, van Leersum N, Beets-Tan RGH, Tollenaar RAEM, Tanis PJ, Dutch Surgical Colorectal Cancer Audit Group (2017) Changes in nationwide use of preoperative radiotherapy for rectal cancer after revision of the national colorectal cancer guideline. EJSO 43:1297–1303
Bondeven P, Laurberg S, Hagemann-Madsen RH et al (2015) Suboptimal surgery and omission of neoadjuvant therapy for upper rectal cancer is associated with a high risk of local recurrence. Color Dis 17(3):216–224
Lopez-Kostner F, Lavery IC, Hool GR et al (1998) Total mesorectal excision is not necessary for cancers of the upper rectum. Surgery. 124(4):612–618
Park JS, Sakai Y, Simon NS et al (2016) Long-term survival and local relapse following surgery without radiotherapy for locally advanced upper rectal cancer: an international multi-institutional study. Medicine (Baltimore) 95(22):2990
Lichliter WE (2015) Techniques in total mesorectal excision surgery. Clin Colon Rectal Surg 28(1):21–27
Khan MA, Ang CW, Hakeem AR (2017) The impact of tumour distance from the anal verge on clinical management and outcomes in patients having a curative resection for rectal cancer. J Gastrointest Surg 21:2056–2065
Lim SB, Yu CS, Hong YS, Kim TW, Kim JH, Kim JC (2012) Long-term outcomes in patients with locally advanced rectal cancer treated with preoperative chemoradiation followed by curative surgical resection. J Surg Oncol 106:659–666
Peng LC, Milsom J, Garrett K et al (2014) Surveillance, epidemiology, and end results-based analysis of the impact of preoperative or postoperative radiotherapy on survival outcomes for T3N0 rectal cancer. Cancer Epidemiol 38:73–78
Ihn MH, Kim YH, Oh HK, Lee SY et al (2015) Effects of preoperative chemoradiotherapy on the likelihood of sphincter preservation surgery in locally advanced distal rectal cancer: a longitudinal study based on pelvic magnetic resonance imaging. Ann Surg Oncol 22:2159–2167
Sauer R, Becker H, Hohenberger W (2004) Preoerative versus postoeprative CRT for rectal cancer. The German rectal cancer study group. N Engl J Med 351:1731–1740
Augestad K, Keller D, Bakaki P, Rose J, Koroukian SM, Øresland T, Delaney CP (2018) The impact of rectal cancer tumor height on recurrence rates and metastatic location: a competing risk analysis of a national database. Cancer Epidemiol 53:56–64
Author information
Authors and Affiliations
Contributions
All authors participated in the conception and design of the study, acquisition of data, analysis and interpretation of data, drafting and revising the manuscript, and approval of the published version.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This manuscript was presented as a poster presentation at the ASCRS meeting May 19–23, 2018, Nashville, Tennessee
Rights and permissions
About this article
Cite this article
Lavryk, O.A., Manilich, E., Valente, M.A. et al. Neoadjuvant chemoradiation improves oncologic outcomes in low and mid clinical T3N0 rectal cancers. Int J Colorectal Dis 35, 77–84 (2020). https://doi.org/10.1007/s00384-019-03452-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-019-03452-6