Abstract
Aim
Inflammatory bowel diseases (IBD) are associated with an increased risk for colorectal cancer (CRC). However and despite significant advances in the management of IBD and CRC, the prognosis of IBD-related CRC (IBD-CRC) remains controversial. The aim of the present case-control study was to compare the prognosis of IBD-CRC to sporadic CRC.
Methods
Consecutive patients operated for IBD-CRC from 2004 to 2014 were recruited and matched with sporadic CRC (ratio 3:1) from the same center. Matching was performed on gender, tumor stage, and location and period of surgery. Endpoints were postoperative morbidity (Dindo-Clavien III-V), quality of surgery, and long-term oncological outcomes.
Results
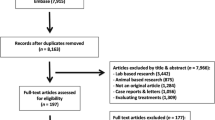
Among 1498 CRC patients operated during the study period, 21 patients were identified with IBD-CRC and matched to 63 patients with sporadic CRC (S-CRC). Patients with IBD-CRC were significantly younger (p < 0.001), had multifocal lesions more frequently (p = 0.04), and undergone abdominoperineal excision and coloproctectomy more often (p = 0.001). Postoperative morbidity was not significantly different between the two groups (25 vs. 14%; p = 0.309), as well as the rate of R0 resection (86 vs. 95%; p = 0.162). Five-year disease-free and overall survival were 71 and 81% in patients with IBD-CRC and 69% (p = 0.801) and 78% (p = 0.845) in those with S-CRC, respectively.
Conclusion
In a case-control study of patients operated for CRC within the last decade, the prognosis of cancer associated with IBD is similar to sporadic cancer.

Similar content being viewed by others
References
Eaden JA, Abrams KR, Mayberry JF (2001) The risk of colorectal cancer in ulcerative colitis: a meta-analysis. Gut 48(4):526–535
Beaugerie L, Svrcek M, Seksik P, Bouvier A, Simon T, Allez M et al (2013) Risk of colorectal high-grade dysplasia and cancer in a prospective observational cohort of patients with inflammatory bowel disease. Gastroenterology 145(1):166–75.e8
Bergeron V, Vienne A, Sokol H, Seksik P, Nion-Larmurier I, Ruskone-Fourmestraux A, Svrcek M, Beaugerie L, Cosnes J (2010) Risk factors for neoplasia in inflammatory bowel disease patients with pancolitis. Am J Gastroenterol 105(11):2405–2411
Delaunoit T, Limburg PJ, Goldberg RM, Lymp JF, Loftus EV Jr (2006) Colorectal cancer prognosis among patients with inflammatory bowel disease. Clin Gastroenterol Hepatol 4(3):335–342
Ording AG, Horváth-Puhó E, Erichsen R, Long MD, Baron JA, Lash TL, Sørensen HT (2013) Five-year mortality in colorectal cancer patients with ulcerative colitis or Crohn’s disease: a nationwide population-based cohort study. Inflamm Bowel Dis 19(4):800–805
Washington MK, Berlin J, Branton P, Burgart LJ, Carter DK, Fitzgibbons PL, Halling K, Frankel W, Jessup J, Kakar S, Minsky B, Nakhleh R, Compton CC, Members of the Cancer Committee, College of American Pathologists (2009) Protocol for the examination of specimens from patients with primary carcinoma of the colon and rectum. Arch Pathol Lab Med 133(10):1539–1551
Kiran RP, Nisar PJ, Goldblum JR, Fazio VW, Remzi FH, Shen B, Lavery IC (2012) Dysplasia associated with Crohn’s colitis: segmental colectomy or more extended resection? Ann Surg 256(2):221–226
Lindberg J, Stenling R, Palmqvist R, Rutegård J (2006) Surgery for neoplastic changes in ulcerative colitis--can limited resection be justified? Outcome for patients who underwent limited surgery. Color Dis 8(7):551–556
Øresland T, Bemelman WA, Sampietro GM, Spinelli A, Windsor A, Ferrante M, Marteau P, Zmora O, Kotze PG, Espin-Basany E, Tiret E, Sica G, Panis Y, Faerden AE, Biancone L, Angriman I, Serclova Z, de Buck van Overstraeten A, Gionchetti P, Stassen L, Warusavitarne J, Adamina M, Dignass A, Eliakim R, Magro F, D'Hoore A, European Crohn’s and Colitis Organisation (ECCO) (2015) European evidence based consensus on surgery for ulcerative colitis. J Crohns Colitis 9(1):4–25
Lavery IC, Chiulli RA, Jagelman DG, Fazio VW, Weakley FL (1982) Survival with carcinoma arising in mucosal ulcerative colitis. Ann Surg 195(4):508–512
Hrabe JE, Byrn JC, Button AM, Zamba GK, Kapadia MR, Mezhir JJ (2014) A matched case-control study of IBD-associated colorectal cancer: IBD portends worse outcome. J Surg Oncol 109(2):117–121
Watanabe T, Konishi T, Kishimoto J, Kotake K, Muto T, Sugihara K, Japanese Society for Cancer of the Colon and Rectum (2011) Ulcerative colitis-associated colorectal cancer shows a poorer survival than sporadic colorectal cancer: a nationwide Japanese study. Inflamm Bowel Dis 17(3):802–808
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Additional information
What does this paper add to the literature?
Most of retrospective cohort studies were based on historical data, collected before new trends on endoscopic surveillance, IBD treatments and CRC therapy.
The current study defined long-term outcomes in a recent cohort of patients with IBD-CRC in comparison to patients with S-CRC.
Rights and permissions
About this article
Cite this article
Thicoïpé, A., Laharie, D., Smith, D. et al. Oncological outcomes of IBD-associated versus sporadic colorectal cancer in modern era: a matched case-control study. Int J Colorectal Dis 33, 963–966 (2018). https://doi.org/10.1007/s00384-018-3049-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-018-3049-z