Abstract
Purpose
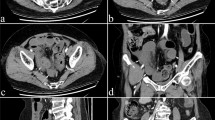
The aim of this study was to investigate the diagnostic accuracy of MR enterography (MRE) for detection of distal ileal and colorectal inflammatory bowel disease (IBD) and to evaluate whether 3 T MRI can provide a higher diagnostic performance compared to 1.5 T.
Methods
A retrospective review of patients with known or suspected IBD who underwent MRE and colonoscopy within 3 months was performed. For analysis, the bowel was divided into six segments. Compared with colonoscopy, the accuracy values for MRI diagnosis of overall and each magnetic field strength were calculated, and the differences between 1.5 T and 3.0 T were compared. The image quality was scored separately for both field strengths and compared.
Results
Eighty-eight patients were included in the study. On a patient basis, MRE had an overall sensitivity of 92.1 % and specificity of 72.0 %. On a segment basis, the sensitivity and specificity were 79.1 % and 93.6 %, respectively. Concerning severely inflamed segments, per-segment sensitivity increased from 79.1 to 94.7 %. The comparison of accuracy values between the two field strengths showed no statistically significant difference. B1 homogeneity and overall artifacts were not significantly different between 3.0 T and 1.5 T imaging. Compared to colonoscopy, MRI found four more fistulas confirmed at subsequent surgery.
Conclusions
MRI has a high diagnostic accuracy for detection of distal ileal and colorectal IBD. 3 T MRI can be considered equivalent but not superior compared to 1.5 T imaging in this context. In addition, our findings suggest MRE to be a valuable tool in detecting surgically relevant pathologies (fistulas) with higher accuracy than colonoscopy.




Similar content being viewed by others
References
Carter MJ, Lobo AJ, Travis SP (2004) Guidelines for the management of inflammatory bowel disease in adults. Gut 53:v1–v16
Anderson ML, Pasha TM, Leighton JA (2000) Endoscopic perforation of the colon: lessons from a 10-year study. Am J Gastroenterol 95:3418–3422
Cappell MS, Friedel D (2002) The role of sigmoidoscopy and colonoscopy in the diagnosis and management of lower gastrointestinal disorders: endoscopic findings, therapy, and complications. Med Clin N Am 86:1253–1288
Fletcher JG, Fidler JL, Bruining DH, Huprich JE (2011) New concepts in intestinal imaging for inflammatory bowel diseases. Gastroenterology 140:1795–1806, e1797
Tielbeek JA, Makanyanga JC, Bipat S et al (2013) Grading Crohn disease activity with MRI: interobserver variability of MRI features, MRI scoring of severity, and correlation with Crohn disease endoscopic index of severity. Am J Roentgenol 201:1220–1228
Rimola J, Ordas I, Rodriguez S et al (2011) Magnetic resonance imaging for evaluation of Crohn’s disease: validation of parameters of severity and quantitative index of activity. Inflamm Bowel Dis 17:1759–1768
Punwani S, Rodriguez-Justo M, Bainbridge A et al (2009) Mural inflammation in Crohn disease: location-matched histologic validation of MR imaging features 1. Radiology 252:712–720
Baumgart DC, Sandborn WJ (2007) Inflammatory bowel disease: clinical aspects and established and evolving therapies. Lancet 369:1641–1657
Erturk SM, Alberich-Bayarri A, Herrmann KA, Marti-Bonmati L, Ros PR (2009) Use of 3.0-T MR imaging for evaluation of the abdomen. Radiographics 29:1547–1563
Patak MA, von Weymarn C, Froehlich JM (2007) Small bowel MR imaging: 1.5T versus 3T. Magn Reson Imaging Clin N Am 15:383–393, vii
van Gemert‐Horsthuis K, Florie J, Hommes DW et al (2006) Feasibility of evaluating Crohn’s disease activity at 3.0 Tesla. J Magn Reson Imaging 24:340–348
Rimola J, Rodríguez S, García-Bosch O et al (2009) Magnetic resonance for assessment of disease activity and severity in ileocolonic Crohn’s disease. Gut 58:1113–1120
Adamek HE, Schantzen W, Rinas U, Goyen M, Ajaj W, Esser C (2012) Ultra-high-field magnetic resonance enterography in the diagnosis of ileitis (neo-)terminalis: a prospective study. J Clin Gastroenterol 46:311–316
Fiorino G, Bonifacio C, Padrenostro M et al (2013) Comparison between 1.5 and 3.0 Tesla magnetic resonance enterography for the assessment of disease activity and complications in ileo-colonic Crohn’s disease. Dig Dis Sci 58:3246–3255
Herrmann KA, Paspulati RM, Lauenstein T, Reiser MF (2010) Benefits and challenges in bowel MR imaging at 3.0 T. Top Magn Reson Imaging 21:165–175
Chang KJ, Kamel IR, Macura KJ, Bluemke DA (2008) 3.0-T MR imaging of the abdomen: comparison with 1.5 T. Radiographics 28:1983–1998
Dagia C, Ditchfield M, Kean M, Catto‐Smith T (2008) Imaging for Crohn disease: use of 3‐T MRI in a paediatric setting. J Med Imaging Radiat Oncol 52:480–488
Franklin KM, Dale BM, Merkle EM (2008) Improvement in B1-inhomogeneity artifacts in the abdomen at 3T MR imaging using a radiofrequency cushion. J Magn Reson Imaging 27:1443–1447
Katscher U, Börnert P (2006) Parallel RF transmission in MRI. NMR Biomed 19:393–400
Koh D, Miao Y, Chinn R et al (2001) MR imaging evaluation of the activity of Crohn’s disease. Am J Roentgenol 177:1325–1332
Schreyer AG, Gölder S, Scheibl K et al (2005) Dark lumen magnetic resonance enteroclysis in combination with MRI colonography for whole bowel assessment in patients with Crohn’s disease: first clinical experience. Inflamm Bowel Dis 11:388–394
Hyun SB, Kitazume Y, Nagahori M et al (2011) Magnetic resonance enterocolonography is useful for simultaneous evaluation of small and large intestinal lesions in Crohn’s disease. Inflamm Bowel Dis 17:1063–1072
Al-Hawary MM, Zimmermann EM, Hussain HK (2014) MR imaging of the small bowel in Crohn disease. Magn Reson Imaging Clin N Am 22:13–22
Negaard A, Paulsen V, Sandvik L et al (2007) A prospective randomized comparison between two MRI studies of the small bowel in Crohn’s disease, the oral contrast method and MR enteroclysis. Eur Radiol 17:2294–2301
Florie J, Birnie E, van Gelder RE et al (2007) MR colonography with limited bowel preparation: patient acceptance compared with that of full-preparation colonoscopy 1. Radiology 245:150–159
Papadia C, Maffei E, Del Rio P et al (2013) Sensitivity and specificity of magnetic resonance enterography in the clinical management of fistulizing Crohn’s disease. Inflamm Bowel Dis 19:1896–1903
Lichtenstein GR, Hanauer SB, Sandborn WJ (2009) Management of Crohn’s disease in adults. Am J Gastroenterol 104:465–483
Schreyer A, Rath H, Kikinis R et al (2005) Comparison of magnetic resonance imaging colonography with conventional colonoscopy for the assessment of intestinal inflammation in patients with inflammatory bowel disease: a feasibility study. Gut 54:250–256
Horsthuis K, Bipat S, Stokkers PC, Stoker J (2009) Magnetic resonance imaging for evaluation of disease activity in Crohn’s disease: a systematic review. Eur Radiol 19:1450–1460
Ajaj WM, Lauenstein TC, Pelster G et al (2005) Magnetic resonance colonography for the detection of inflammatory diseases of the large bowel: quantifying the inflammatory activity. Gut 54:257–263
Dignass A, Van Assche G, Lindsay JO et al (2010) The second European evidence-based consensus on the diagnosis and management of Crohn’s disease: current management. J Crohn's Colitis 4:28–62
Dignass A, Lindsay JO, Sturm A et al (2012) Second European evidence-based consensus on the diagnosis and management of ulcerative colitis part 2: current management. J Crohn's Colitis 6:991–1030
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jiang, X., Asbach, P., Hamm, B. et al. MR imaging of distal ileal and colorectal chronic inflammatory bowel disease—diagnostic accuracy of 1.5 T and 3 T MRI compared to colonoscopy. Int J Colorectal Dis 29, 1541–1550 (2014). https://doi.org/10.1007/s00384-014-2037-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-014-2037-1