Abstract
Purpose
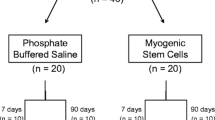
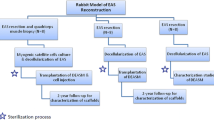
Reliable animal models are essential to evaluate future therapeutic options like cell-based therapies for external anal sphincter insufficiency. The goal of our study was to describe the most reliable model for external sphincter muscle insufficiency by comparing three different methods to create sphincter muscle damage.
Methods
In an experimental animal study, female Lewis rats (200–250 g) were randomly assigned to three treatment groups (n = 5, each group). The external sphincter muscle was weakened in the left dorsal quadrant by microsurgical excision, cryosurgery, or electrocoagulation by diathermy. Functional evaluation included in vivo measurements of resting pressure, spontaneous muscle contraction, and contraction in response to electrical stimulation of the afferent nerve at baseline and at 2, 4, and 6 weeks after sphincter injury. Masson’s trichrome staining and immunofluorescence for skeletal muscle markers was performed for morphological analysis.
Results
Peak contraction after electrical stimulation was significantly decreased after sphincter injury in all groups. Contraction forces recovered partially after cryosurgery and electrocoagulation but not after microsurgical excision. Morphological analysis revealed an incomplete destruction of the external sphincter muscle in the cryosurgery and electrocoagulation groups compared to the microsurgery group.
Conclusions
For the first time, three different models of external sphincter muscle insufficiency were directly compared. The animal model using microsurgical sphincter destruction offers the highest level of consistency regarding tissue damage and sphincter insufficiency, and therefore represents the most reliable model to evaluate future therapeutic options. In addition, this study represents a novel model to specifically test the external sphincter muscle function.






Similar content being viewed by others
References
Miner PB Jr (2004) Economic and personal impact of fecal and urinary incontinence. Gastroenterology 126(1 Suppl 1):S8–13
Perry S, Shaw C, McGrother C, Matthews RJ, Assassa RP, Dallosso H, Williams K, Brittain KR, Azam U, Clarke M, Jagger C, Mayne C, Castleden CM (2002) Prevalence of faecal incontinence in adults aged 40 years or more living in the community. Gut 50(4):480–484
Nelson R, Norton N, Cautley E, Furner S (1995) Community-based prevalence of anal incontinence. JAMA 274(7):559–561
Whitehead WE, Borrud L, Goode PS, Meikle S, Mueller ER, Tuteja A, Weidner A, Weinstein M, Ye W (2009) Fecal incontinence in US adults: epidemiology and risk factors. Gastroenterology 137(2):512–517. doi:10.1053/j.gastro.2009.04.054
Hetzer FH, Bieler A, Hahnloser D, Lohlein F, Clavien PA, Demartines N (2006) Outcome and cost analysis of sacral nerve stimulation for faecal incontinence. Br J Surg 93(11):1411–1417. doi:10.1002/bjs.5491
Belyaev O, Muller C, Uhl W (2006) Neosphincter surgery for fecal incontinence: a critical and unbiased review of the relevant literature. Surg Today 36(4):295–303. doi:10.1007/s00595-005-3159-4
Chapman AE, Geerdes B, Hewett P, Young J, Eyers T, Kiroff G, Maddern GJ (2002) Systematic review of dynamic graciloplasty in the treatment of faecal incontinence. BrJ Surg 89(2):138–153
Mundy L, Merlin TL, Maddern GJ, Hiller JE (2004) Systematic review of safety and effectiveness of an artificial bowel sphincter for faecal incontinence. BrJ Surg 91(6):665–672
Dudding TC, Vaizey CJ, Kamm MA (2008) Obstetric anal sphincter injury: incidence, risk factors, and management. Ann Surg 247(2):224–237. doi:10.1097/SLA.0b013e318142cdf4
Wheeler TL 2nd, Richter HE (2007) Delivery method, anal sphincter tears and fecal incontinence: new information on a persistent problem. Curr Opin Obstet Gynecol 19(5):474–479. doi:10.1097/GCO.0b013e3282ef4142
Lewicky-Gaupp C, Hamilton Q, Ashton-Miller J, Huebner M, DeLancey JO, Fenner DE (2009) Anal sphincter structure and function relationships in aging and fecal incontinence. Am J Obstet Gynecol 200(5):559–e551. doi:10.1016/j.ajog.2008.11.009
Rao SS (2004) Pathophysiology of adult fecal incontinence. Gastroenterology 126(1 Suppl 1):S14–22
Rasmussen OO (2003) Fecal incontinence. Studies on physiology, pathophysiology and surgical treatment. DanMed Bull 50(3):262–282
Lorenzi B, Pessina F, Lorenzoni P, Urbani S, Vernillo R, Sgaragli G, Gerli R, Mazzanti B, Bosi A, Saccardi R, Lorenzi M (2008) Treatment of experimental injury of anal sphincters with primary surgical repair and injection of bone marrow-derived mesenchymal stem cells. Dis Colon Rectum 51(4):411–420
Zutshi M, Salcedo LB, Zaszczurynski PJ, Hull TL, Butler RS, Damaser MS (2009) Effects of sphincterotomy and pudendal nerve transection on the anal sphincter in a rat model. Dis Colon Rectum 52(7):1321–1329. doi:10.1007/DCR.0b013e31819f746d
Yamaguchi I, Fujita F, Yamanouchi K, Mishima T, Kawahara D, Sakai Y, Ito S, Kanetaka K, Takatsuki M, Kuroki T, Eguchi S (2013) A novel animal model of long-term sustainable anal sphincter dysfunction. J Surg Res. doi:10.1016/j.jss.2013.04.010
Yiou R, Yoo JJ, Atala A (2003) Restoration of functional motor units in a rat model of sphincter injury by muscle precursor cell autografts. Transplantation 76(7):1053–1060
Kang SB, Lee HN, Lee JY, Park JS, Lee HS (2008) Sphincter contractility after muscle-derived stem cells autograft into the cryoinjured anal sphincters of rats. Dis Colon Rectum 51(9):1367–1373. doi:10.1007/s10350-008-9360-y
Vinograd I, Hanani M, Hadary A, Merguerian P, Nissan S (1985) Animal model for the study of internal anal sphincter activity. Eur Surg Res 17(4):259–263
Yablonka-Reuveni Z (2011) The skeletal muscle satellite cell: still young and fascinating at 50. J Histochem Cytochem 59(12):1041–1059. doi:10.1369/0022155411426780
Shafik A (1995) Inferior rectal nerve stimulation for anal sphincteric control: experimental study. J Surg Res 59(4):441–445. doi:10.1006/jsre.1995.1188
Kajbafzadeh AM, Elmi A, Talab SS, Esfahani SA, Tourchi A (2010) Functional external anal sphincter reconstruction for treatment of anal incontinence using muscle progenitor cell auto grafting. Dis Colon Rectum 53(10):1415–1421. doi:10.1007/DCR.0b013e3181e53088
Raghavan S, Gilmont RR, Miyasaka EA, Somara S, Srinivasan S, Teitelbaum DH, Bitar KN (2011) Successful implantation of bioengineered, intrinsically innervated, human internal anal sphincter. Gastroenterology 141(1):310–319. doi:10.1053/j.gastro.2011.03.056
Maeda Y, Laurberg S, Norton C (2010) Perianal injectable bulking agents as treatment for faecal incontinence in adults. Cochrane Database Syst Rev 5, CD007959. doi:10.1002/14651858.CD007959.pub2
Acknowledgments
The authors thank Meline Stoelting, Souzan Salemi, and Fatma Kivrak for the introduction in analyzing techniques and for technical assistance. This research project was financially supported by grants from the EMDO foundation and the Insula Foundation, Switzerland.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Brügger, L., Inglin, R., Candinas, D. et al. A novel animal model for external anal sphincter insufficiency. Int J Colorectal Dis 29, 1385–1392 (2014). https://doi.org/10.1007/s00384-014-2006-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-014-2006-8