Abstract
Purpose
Carbon dioxide (CO2) insufflation reduces abdominal pain and discomfort after endoscopic procedures; however, there is no previous study focusing the safety of CO2 insufflation for patients with obstructive ventilatory disturbance. Here, we investigated the safety of CO2 insufflation during colorectal endoscopic submucosal dissection (ESD) for patients with obstructive disturbance.
Methods
Between January 2010 and January 2013, colorectal ESD was performed using CO2 insufflation for 385 consecutive patients. End-tidal CO2 (EtCO2) and transcutaneous oxygen saturation (SpO2) were consecutively measured from the time before insertion of the colonoscope to the end of ESD. Patients were monitored by two nurses during the procedure and controlled for clinical symptoms of hypercapnia such as apnea or a depressed level of consciousness. According to their respiratory function, patients were stratified into a normal group and an obstructive disturbance group. We retrospectively compared EtCO2 and SpO2 during the procedures and the incidence of symptoms related to CO2 retention between the two groups.
Results
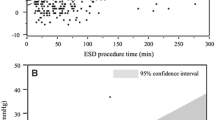
The obstructive disturbance group consisted of 77 patients. There were similar changes of EtCO2 in the obstructive disturbance group and normal group and no significant rise in EtCO2. The maximum EtCO2 level in any patient was <60 mmHg. In the obstructive disturbance group, there were no symptoms associated with CO2 retention. There were no significant differences in the median SpO2 between both groups and no prolonged drop of SpO2.
Conclusions
CO2 insufflation during colorectal ESD is safe for patients with obstructive ventilatory disturbance.



Similar content being viewed by others
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D (2011) Global cancer statistics. CA Cancer J Clin 61(2):69–90. doi:10.3322/caac.20107
Saito Y, Kawano H, Takeuchi Y, Ohata K, Oka S, Hotta K, Okamoto K, Homma K, Uraoka T, Hisabe T, Chang DK, Zhou PH (2012) Current status of colorectal endoscopic submucosal dissection in Japan and other Asian countries: progressing towards technical standardization. Dig Endosc 24(Suppl 1):67–72. doi:10.1111/j.1443-1661.2012.01282.x
Fujishiro M (2009) Endoscopic submucosal dissection for colorectal neoplasms. World J Gastrointest Endosc 1(1):32–38. doi:10.4253/wjge.v1.i1.32
Saito Y, Uraoka T, Yamaguchi Y, Hotta K, Sakamoto N, Ikematsu H, Fukuzawa M, Kobayashi N, Nasu J, Michida T, Yoshida S, Ikehara H, Otake Y, Nakajima T, Matsuda T, Saito D (2010) A prospective, multicenter study of 1111 colorectal endoscopic submucosal dissections (with video). Gastrointest Endosc 72(6):1217–1225. doi:10.1016/j.gie.2010.08.004
Hussein AM, Bartram CI, Williams CB (1984) Carbon dioxide insufflation for more comfortable colonoscopy. Gastrointest Endosc 30(2):68–70
Stevenson GW, Wilson JA, Wilkinson J, Norman G, Goodacre RL (1992) Pain following colonoscopy: elimination with carbon dioxide. Gastrointest Endosc 38(5):564–567
Church J, Delaney C (2003) Randomized, controlled trial of carbon dioxide insufflation during colonoscopy. Dis Colon Rectum 46(3):322–326. doi:10.1097/01.DCR.0000054700.26909.46
Sumanac K, Zealley I, Fox BM, Rawlinson J, Salena B, Marshall JK, Stevenson GW, Hunt RH (2002) Minimizing postcolonoscopy abdominal pain by using CO(2) insufflation: a prospective, randomized, double blind, controlled trial evaluating a new commercially available CO(2) delivery system. Gastrointest Endosc 56(2):190–194
Rogers BH (1974) The safety of carbon dioxide insufflation during colonoscopic electrosurgical polypectomy. Gastrointest Endosc 20(3):115–117
Bretthauer M, Lynge AB, Thiis-Evensen E, Hoff G, Fausa O, Aabakken L (2005) Carbon dioxide insufflation in colonoscopy: safe and effective in sedated patients. Endoscopy 37(8):706–709. doi:10.1055/s-2005-870154
Bretthauer M, Thiis-Evensen E, Huppertz-Hauss G, Gisselsson L, Grotmol T, Skovlund E, Hoff G (2002) NORCCAP (Norwegian Colorectal Cancer Prevention): a randomised trial to assess the safety and efficacy of carbon dioxide versus air insufflation in colonoscopy. Gut 50(5):604–607
Yamano HO, Yoshikawa K, Kimura T, Yamamoto E, Harada E, Kudou T, Katou R, Hayashi Y, Satou K (2010) Carbon dioxide insufflation for colonoscopy: evaluation of gas volume, abdominal pain, examination time and transcutaneous partial CO2 pressure. J Gastroenterol 45(12):1235–1240. doi:10.1007/s00535-010-0286-5
Saito Y, Uraoka T, Matsuda T, Emura F, Ikehara H, Mashimo Y, Kikuchi T, Kozu T, Saito D (2007) A pilot study to assess the safety and efficacy of carbon dioxide insufflation during colorectal endoscopic submucosal dissection with the patient under conscious sedation. Gastrointest Endosc 65(3):537–542. doi:10.1016/j.gie.2006.11.002
Nakajima K, Lee SW, Sonoda T, Milsom JW (2005) Intraoperative carbon dioxide colonoscopy: a safe insufflation alternative for locating colonic lesions during laparoscopic surgery. Surg Endosc 19(3):321–325. doi:10.1007/s00464-004-8915-9
Wu J, Hu B (2012) The role of carbon dioxide insufflation in colonoscopy: a systematic review and meta-analysis. Endoscopy 44(2):128–136. doi:10.1055/s-0031-1291487
Bretthauer M, Seip B, Aasen S, Kordal M, Hoff G, Aabakken L (2007) Carbon dioxide insufflation for more comfortable endoscopic retrograde cholangiopancreatography: a randomized, controlled, double-blind trial. Endoscopy 39(1):58–64. doi:10.1055/s-2006-945036
Uraoka T, Kato J, Kuriyama M, Hori K, Ishikawa S, Harada K, Takemoto K, Hiraoka S, Fujita H, Horii J, Saito Y, Yamamoto K (2009) CO(2) insufflation for potentially difficult colonoscopies: efficacy when used by less experienced colonoscopists. World J Gastroenterol 15(41):5186–5192
Kikuchi T, Fu KI, Saito Y, Uraoka T, Fukuzawa M, Fukunaga S, Sakamoto T, Nakajima T, Matsuda T (2010) Transcutaneous monitoring of partial pressure of carbon dioxide during endoscopic submucosal dissection of early colorectal neoplasia with carbon dioxide insufflation: a prospective study. Surg Endosc 24(9):2231–2235. doi:10.1007/s00464-010-0939-8
Suzuki T, Minami H, Komatsu T, Masusda R, Kobayashi Y, Sakamoto A, Sato Y, Inoue H, Serada K (2010) Prolonged carbon dioxide insufflation under general anesthesia for endoscopic submucosal dissection. Endoscopy 42(12):1021–1029. doi:10.1055/s-0030-1255969
Hotta K, Yamaguchi Y, Saito Y, Takao T, Ono H (2012) Current opinions for endoscopic submucosal dissection for colorectal tumors from our experiences: indications, technical aspects and complications. Dig Endosc 24(Suppl 1):110–116. doi:10.1111/j.1443-1661.2012.01262.x
Kakushima N (2011) Endoscopic submucosal dissection using the insulated-tip knife. Tech Gastrointest Endosc 13(1):63–69
Sessler CN, Gosnell MS, Grap MJ, Brophy GM, O’Neal PV, Keane KA, Tesoro EP, Elswick RK (2002) The Richmond Agitation-Sedation Scale: validity and reliability in adult intensive care unit patients. Am J Respir Crit Care Med 166(10):1338–1344. doi:10.1164/rccm.2107138
Goldman JM (1987) A simple, easy, and inexpensive method for monitoring ETCO2 through nasal cannulae. Anesthesiology 67(4):606
Kusunoki R, Amano Y, Yuki T, Oka A, Okada M, Tada Y, Uno G, Moriyama I, Ishimura N, Ishihara S, Kinoshita Y (2012) Capnographic monitoring for carbon dioxide insufflation during endoscopic submucosal dissection: comparison of transcutaneous and end-tidal capnometers [corrected]. Surg Endosc 26(2):501–506. doi:10.1007/s00464-011-1908-6
Engoren M, Plewa M, O’Hara D, Kline J (2005) Evaluation of capnography using a genetic algorithm to predict PaCO2. Chest 127(2):579–584
Lujan M, Canturri E, Moreno A, Arranz M, Vigil L, Domingo C (2008) Capnometry in spontaneously breathing patients: the influence of chronic obstructive pulmonary disease and expiration maneuvers. Med Sci Monit 14(9):CR485–CR492
Chuang M-L, Lin IF, Vintch JRE, Tien E-H (2012) Using statistical techniques to predict dynamic arterial P(CO(2)) in patients with COPD during maximum exercise. Respir Care 57(7):1106–1114
Price HL (1960) Effects of carbon dioxide on the cardiovascular system. Anesthesiology 21:652–663
Bond JH Jr, Levitt MD (1975) Factors affecting the concentration of combustible gases in the colon during colonoscopy. Gastroenterology 68(6):1445–1448
Fukuchi Y, Nishimura M, Ichinose M, Adachi M, Nagai A, Kuriyama T, Takahashi K, Nishimura K, Ishioka S, Aizawa H, Zaher C (2004) COPD in Japan: the Nippon COPD Epidemiology Study. Respirology 9(4):458–465. doi:10.1111/j.1440-1843.2004.00637.x
Rabe KF, Hurd S, Anzueto A, Barnes PJ, Buist SA, Calverley P, Fukuchi Y, Jenkins C, Rodriguez-Roisin R, van Weel C, Zielinski J, Global Initiative for Chronic Obstructive Lung D (2007) Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care Med 176(6):532–555. doi:10.1164/rccm.200703-456SO
Saltzman HA, Sieker HO (1968) Intestinal response to changing gaseous environments: normobaric and hyperbaric observations. Ann N Y Acad Sci 150(1):31–39
Forster RE (1968) Physiological basis of gas exchange in the gut. Ann N Y Acad Sci 150(1):4–12
Wagner PD, Dantzker DR, Dueck R, Clausen JL, West JB (1977) Ventilation–perfusion inequality in chronic obstructive pulmonary disease. J Clin Investig 59(2):203–216
Ozyuvaci E, Demircioglu O, Toprak N, Topacoglu H, Sitilci T, Akyol O (2012) Comparison of transcutaneous, arterial and end-tidal measurements of carbon dioxide during laparoscopic cholecystectomy in patients with chronic obstructive pulmonary disease. J Int Med Res 40(5):1982–1987
Hansen J, Ulubay G, Chow B, Sun X-G, Wasserman K (2007) Mixed-expired and end-tidal CO2 distinguish between ventilation and perfusion defects during exercise testing in patients with lung and heart diseases. Chest 132(3):977–983
Acknowledgments
A prototype of the IT knife nanoTM was provided by Olympus, Tokyo, Japan, as part of a cooperation.
Conflict of interest
The authors have declared that no competing interests exist.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yoshida, M., Imai, K., Hotta, K. et al. Carbon dioxide insufflation during colorectal endoscopic submucosal dissection for patients with obstructive ventilatory disturbance. Int J Colorectal Dis 29, 365–371 (2014). https://doi.org/10.1007/s00384-013-1806-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-013-1806-6