Abstract
Purpose
Rectal cancer surgery is impaired by a high rate of postoperative sexual dysfunction cause of frequent nerve injuries. The aim of this study was to prospectively evaluate sexual function in a group of male patients after total mesorectal excision (TME) for rectal cancer, using an autonomic nerve sparing technique.
Methods
All patients underwent autonomic nerve preserving TME. Sexual function was assessed using the International Index of Erectile Function standardized questionnaire. All patients were studied preoperatively and at 3, 6, 12, 18, and 24 months after surgery.
Results
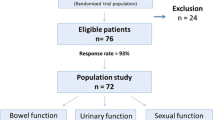
Fifty-one patients with adenocarcinoma of the rectum were enrolled; after excluding 16 patients not sexually active, nine with T4 stage disease and six with metastatic disease, 20 patients were prospectively evaluated. The preoperative erectile function (EF) domain score of the International Index of Erectile Function was 24.3 (±4.1). The score of the EF domain was 17.6 (±7.5), 19.l9 (±7.2), 20.3 (±7.4), 20.5 (±7.4), and 20.6 (±7.4) at 3, 6, 12, 18, and 24 months after surgery. In the group of patients in which there were no macroscopic damages to the nerves, only two out of 15 (13.3%) developed erectile dysfunction. All five patients in whom incomplete pelvic nerve preservation was necessary developed erectile dysfunction.
Conclusion
Our data show that nerve sparing technique can reduce the incidence of sexual dysfunction. Unfortunately, the technique is not applicable in every patient. Indications and techniques of autonomic nerve preservation are not standardized. Controlled trials with long-term follow-up seem to be necessary.

Similar content being viewed by others
References
Vironen JH, Kairaluoma M, Aalto AM, Kellokumpu IH (2006) Impact of functional results on quality of life after rectal cancer surgery. Dis Colon Rectum 49(5):568–578
Hendren SK, O’Connor BI, Liu M, Asano T, Cohen Z, Swallow CJ, Macrae HM, Gryfe R, McLeod RS (2005) Prevalence of male and female sexual dysfunction is high following surgery for rectal cancer. Ann Surg 242(2):212–223
Lindsey I, Mortensen NJ (2002) Iatrogenic impotence and rectal dissection. Br J Surg 89(12):1493–1494
Heald RJ, Husband EM, Ryall RD (1982) The mesorectal in rectal surgery—the clue to pelvic recurrence? Br J Surg 69:613–616
Heald RJ, Ryall RD (1986) Recurrence and survival after total mesorectal excision for rectal cancer..Lancet 28;1(8496):1479-82.
Walsh PC, Lepor H, Eggleston JC (1983) Radical prostatectomy with preservation of sexual function: anatomical and pathological considerations. Prostate 4(5):473–485
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A (1997) The International Index of Erectile Function (IIEF): a multidimensional scale for assessment of erectile dysfunction. Urology 49(6):822–830
Cappelleri JC, Rosen RC, Smith MD, Mishra A, Osterloh IH (1999) Diagnostic evaluation of the erectile function domain of the International Index of Erectile Function. Urology 54(2):346–351
Havenga K, DeRuiter MC, Enker WE, Welvaart K (1996) Anatomical basis of autonomic nerve-preserving total mesorectal excision for rectal cancer. Br J Surg 83(3):384–388
Junginger T, Kneist W, Heintz A (2003) Influence of identification and preservation of pelvic autonomic nerves in rectal cancer surgery on bladder dysfunction after total mesorectal excision. Dis Colon Rectum 46(5):621–628
Kourambas J, Angus DG, Hosking P, Chou ST (1998) A histological study of Denonvilliers’ fascia and its relationship to the neurovascular bundle. Br J Urol 82(3):408–410
Lindsey I, Guy RJ, Warren BF, Mortensen NJ (2000) Anatomy of Denonvilliers’ fascia and pelvic nerves, impotence, and implications for the colorectal surgeon. Br J Surg 87(10):1288–1299
da Silva GM, Zmora O, Börjesson L, Mizhari N, Daniel N, Khandwala F, Efron J, Weiss EG, Nogueras JJ, Vernava AM, Wexner SD (2005) The efficacy of a nerve stimulator (Cavermap) to enhance autonomic nerve identification and confirm nerve preservation during total mesorectal excision. Dis Colon Rectum 48(12):2354–2361
Kneist W, Junginger T (2007) Male urogenital function after confirmed nerve-sparing total mesorectal excision with dissection in front of Denonvilliers’ fascia. World J Surg 31(6):1321–1328
Lindsey I, Cunningham C, George BD, Mortensen NJ (2003) Nocturnal penile tumescence is diminished but not ablated in postproctectomy impotence. Dis Colon Rectum 46(1):14–19
Lindsey I, George B, Kettlewell M, Mortensen N (2002) Randomized, double-blind, placebo-controlled trial of sildenafil (Viagra) for erectile dysfunction after rectal excision for cancer and inflammatory bowel disease. Dis Colon Rectum 45(6):727–732
Asoglu O, Matlim T, Karanlik H, Atar M, Muslumanoglu M, Kapran Y, Igci A, Ozmen V, Kecer M, Parlak M (2009) Impact of laparoscopic surgery on bladder and sexual function after total mesorectal excision for rectal cancer. Surg Endosc 23(2):296–303
Jayne DG, Brown JM, Thorpe H, Walker J, Quirke P, Guillou PJ (2005) Bladder and sexual function following resection for rectal cancer in a randomized clinical trial of laparoscopic versus open technique. Br J Surg 92(9):1124–1132
Guillou PJ, Quirke P, Thorpe H, Walker J, Jayne DG, Smith A et al (2000) CLASICC: conventional versus Laparoscopic-assisted surgery in colorectal cancer. Colorectal Dis 2(Suppl 1):77
Lange MM, Marijnen CA, Maas CP, Putter H, Rutten HJ, Stiggelbout AM, Meershoek-Klein Kranenbarg E, van de Velde CJ, Cooperative Clinical Investigators of the Dutch (2009) Risk factors for sexual dysfunction after rectal cancer treatment. Eur J Cancer 45(9):1578–1588
Heriot AG, Tekkis PP, Fazio VW, Neary P, Lavery IC (2005) Adjuvant radiotherapy is associated with increased sexual dysfunction in male patients undergoing resection for rectal cancer: a predictive model. Ann Surg 242(4):502–510
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Celentano, V., Fabbrocile, G., Luglio, G. et al. Prospective study of sexual dysfunction in men with rectal cancer: feasibility and results of nerve sparing surgery. Int J Colorectal Dis 25, 1441–1445 (2010). https://doi.org/10.1007/s00384-010-0995-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-010-0995-5