Abstract
Background
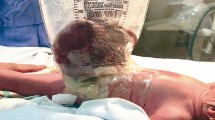
Gastroschisis is the most common congenital abdominal wall defect. Due to the exposure of midgut to amniotic fluid, the recovery of bowel function is often delayed. This study aimed to identify the factors associated with the successful early enteral feeding in gastroschisis and to develop further guidelines of treatment.
Methods
A retrospective cohort study of gastroschisis babies from January 2006 to December 2015 was done. Exclusion criteria were incomplete data and death. Successful early enteral feeding was defined when full feeding was achieved within 21 days of life.
Results
One hundred and five gastroschisis patients were divided into a successful early-feeding group (n = 56, 53%) and a non-successful early-feeding group (n = 49, 46%). In multivariable analysis, significant factors for successful feeding clustered by primary treatment were female (RR = 1.38, P value < 0.001), gestational age > 36 weeks (RR = 1.23, P value < 0.001), age at surgery less than 10 h (RR = 1.15, P value < 0.001), postoperative extubation time < 4 days (RR = 1.39, P value < 0.001), and age when feeding started less than 10 days (RR = 35.69, P value < 0.001).
Conclusion
Several factors were found to be associated with successful early enteral feeding. The modifiable factors found in this study were surgery within 10 h, early postoperative extubation within 4 days, and feeding started before 10 days of life. These will guide the management of gastroschisis to achieve successful early enteral feeding.

Similar content being viewed by others
References
Holland AJ, Walker K, Badawi N (2010) Gastroschisis: an update. Pediatr Surg Int 26(9):871–878
Aljahdali A, Mohajerani N, Skarsgard ED, Canadian Pediatric Surgery Network (2013) Effect of timing of enteral feeding on outcome in gastroschisis. J Pediatr Surg 48(5):971–976
Langer JC (1996) Gastroschisis and omphalocele. Semin Pediatr Surg 5(2):124–128
Marinovic VM, Lukac ML, Mikovic Z, Grujic B, Stojanovic A, Sabbagh D, Samardzija G (2016) Gastroschisis with gastric perforation and jejunal stenosis. A rare association of anomalies. Ann Ital Chir 87:263–267
Skarsgard ED (2016) Management of gastroschisis. Curr Opin Pediatr 28(3):363–369
Singh SJ, Fraser A, Leditschke JF et al (2003) Gastroschisis: determinants of neonatal outcome. Pediatr Surg Int 19(4):260–265
Allotey J, Davenport M, Njere I et al (2007) Benefit of preformed silos in the management of gastroschisis. Pediatr Surg Int 23(11):1065–1069
Lobo JD, Kim AC, Davis RP et al (2010) No free ride? The hidden costs of delayed operative management using a spring-loaded silo for gastroschisis. J Pediatr Surg 45(7):1426–1432
Alali JS, Tander B, Malleis J, Klein MD (2011) Factors affecting the outcome in patients with gastroschisis: how important is immediate repair? Eur J Pediatr Surg 21(2):99–102. https://doi.org/10.1055/s-0030-1267977
Novotny DA, Klein RL, Boeckman CR (1993) Gastroschisis: an 18-year review. J Pediatr Surg 28(5):650–652
Schlatter M, Norris K, Uitvlugt N, DeCou J, Connors R (2003) Improved outcomes in the treatment of gastroschisis using a preformed silo and delayed repair approach. J Pediatr Surg 38(3):459–464 (discussion 459–464)
Kunz SN, Tieder JS, Whitlock K, Jackson JC, Avansino JR (2013) Primary fascial closure versus staged closure with silo in patients with gastroschisis: a meta-analysis. J Pediatr Surg 48(4):845–857
Schmidt AF, Gonçalves A, Bustorff-Silva JM, Oliveira Filho AG, Marba ST, Sbragia L (2011) Does staged closure have a worse prognosis in gastroschisis? Clinics 66(4):563–566
Jager LC, Heij HA (2007) Factors determining outcome in gastroschisis: clinical experience over 18 years. Pediatr Surg Int 23(8):731–736
Snyder CW, Biggio JR, Bartle DT, Georgeson KE, Muensterer OJ (2011) Early severe hypoalbuminemia is an independent risk factor for intestinal failure in gastroschisis. Pediatr Surg Int 27(11):1155–1158
Miranda da Silva Alves F, Miranda ME, de Aguiar MJ, Bouzada Viana MC (2016) Nutritional management and postoperative prognosis of newborns submitted to primary surgical repair of gastroschisis. J Pediatr 92(3):268–275
Maramreddy H, Fisher J, Slim M, Lagamma EF, Parvez B (2009) Delivery of gastroschisis patients before 37 weeks of gestation is associated with increased morbidities. J Pediatr Surg 44(7):1360–1366
Ergun O, Barksdale E, Ergun FS et al (2005) The timing of delivery of infants with gastroschisis influences outcome. J Pediatr Surg 40(2):424–428
Vilela PC, Ramos De Amorim MM, Falbo GH, Santos LC (2001) Risk factors for adverse outcome of newborns with gastroschisis in a Brazilian hospital. J Pediatr Surg 36(4):559–564
Berseth MCL (1992) Effect of early feeding on maturation of the preterm infant’s intestine. J Pediatr 120(6):947–953
Elizabeth Walter-Nicolet VR, Francois, Kieffer et al (2009) Neonatal outcome of gastroschisis is mainly influenced by nutritional management. J Pediatr Gastroenterol Nutr 48:612–617
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We report no conflicts of interest in this work.
Rights and permissions
About this article
Cite this article
Pratheeppanyapat, T., Tepmalai, K., Singhavejsakul, J. et al. The factors associated with successful early enteral feeding in gastroschisis. Pediatr Surg Int 34, 743–748 (2018). https://doi.org/10.1007/s00383-018-4282-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-018-4282-9