Abstract
Purpose
The treatment of intermediate risk (IR) neuroblastoma has evolved with the focus now on reducing the drugs, dosage, and duration of chemotherapy. The aim of this study is to present the outcomes of treatment and the complications of surgery in patients with IR neuroblastoma treated at a tertiary cancer center in India.
Methods
All eligible patients with IR neuroblastoma treated between April 2005 and August 2016 were identified. The presence and number of image-defined risk factors (IDRF) before and after neoadjuvant chemotherapy were retrospectively analyzed as were the extent of surgery, complications, and outcomes.
Results
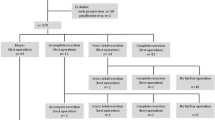
Of 282 neuroblastoma patients treated during the study period, 54 had IR neuroblastoma. Complete excision was achieved in 25 patients. There were 26 surgical complications in 22 patients with a similar incidence in patients with complete (n = 13) or incomplete (n = 13) resection (p = 0.78). After a median follow-up of 47 months, the 4-year overall and event-free survival was 91.5% and 75%, respectively. There was no difference in survival between patients who underwent complete resection versus those with incomplete resection (p = 0.9).
Conclusion
Outcomes of IR neuroblastoma are favorable. The extent of resection does not affect the survival and complications can occur even when the resection is incomplete.




Similar content being viewed by others
References
Gurney JG, Davis S, Severson RK, Fang JY, Ross JA, Robison LL (1996) Trends in cancer incidence among children in the US. Cancer 78:532–541
Magrath I, Steliarova-Foucher E, Epelman S, Ribeiro RC, Harif M, Li C-K et al (2013) Paediatric cancer in low-income and middle-income countries. Lancet Oncol 14:e104–e116
Maris JM, Hogarty MD, Bagatell R, Cohn SL (2007) Neuroblastoma. Lancet 369:2106–2120
Nickerson HJ, Matthay KK, Seeger RC et al (2000) Favourable biology and outcome of stage IV-S neuroblastoma with supportive care or minimal therapy: a Children’s Cancer Group study. J Clin Oncol 18:477–486
Schmidt ML, Lukens JN, Seeger RC et al (2000) Biologic factors determine prognosis in infants with stage IV neuroblastoma: a prospective Children’s Cancer Group Study. J Clin Oncol 18:1260–1268
Matthay KK, Perez C, Seeger RC et al (1998) Successful treatment of stage III neuroblastoma based on prospective biologic staging: a Children’s Cancer Group study. J Clin Oncol 16:1256–1264
Baker DL, Schmidt ML, Cohn SL, Maris JM, London WB, Buxton A et al (2010) Outcome after reduced chemotherapy for intermediate-risk neuroblastoma. N Engl J Med 363:1313–1323
Bagatell R, Rumcheva P, London WB, Cohn SL, Look AT, Brodeur GM et al (2005) Outcomes of children with intermediate-risk neuroblastoma after treatment stratified by MYCN status and tumor cell ploidy. J Clin Oncol 23:8819–8827
De Bernardi B, Gerrard M, Boni L, Rubie H, Canete A, Di Cataldo A et al (2009) Excellent outcome with reduced treatment for infants with disseminated neuroblastoma without MYCN gene amplification. J Clin Oncol 27:1034–1040
Rubie H, De Bernardi B, Gerrard M et al (2011) Excellent outcome with reduced treatment in infants with nonmetastatic and unresectable neuroblastoma without MYCN amplification: Results of the prospective INES 99.1. J Clin Oncol 29:449–455
Kohler JA, Rubie H, Castel V et al (2013) Treatment of children over the age of one year with unresectable localized neuroblastoma without MYCN amplification: results of the SIOPEN study. Eur J Cancer 49:3671–3679
Modak S, Kushner BH, LaQuaglia MP, Kramer K, Cheung N-KV (2009) Management and outcome of stage 3 neuroblastoma. Eur J Cancer 45:90–98
Brodeur GM, Pritchard J, Berthold F et al (1993) Revisions of the international criteria for neuroblastoma diagnosis, staging and response to treatment. J Clin Oncol 11:1466–1477
Cecchetto G, Mosseri V, De Bernardi B, Helardot P, Monclair T, Costa E et al (2005) Surgical risk factors in primary surgery for localized neuroblastoma: the LNESG1 study of the European International Society of Pediatric Oncology Neuroblastoma Group. J Clin Oncol 23:8483–8489
Yoneda A, Nishikawa M, Uehara S, Oue T, Usui N, Inoue M et al (2016) Can neoadjuvant chemotherapy reduce the surgical risks for localized neuroblastoma patients with image-defined risk factors at the time of diagnosis? Pediatr Surg Int 32:209–214
Irtan S, Brisse HJ, Minard-Colin V, Schleiermacher G, Galmiche-Rolland L, Le Cossec C et al (2015) Image-defined risk factor assessment of neurogenic tumors after neoadjuvant chemotherapy is useful for predicting intra-operative risk factors and the completeness of resection. Pediatr Blood Cancer 62:1543–1549
Qureshi SS, Rent EG, Bhagat M, Dsouza P, Kembhavi S, Vora T et al (2016) Chyle leak following surgery for abdominal neuroblastoma. J Pediatr Surg 51:1557–1560
Acknowledgements
We would like to thank Prof. Shakeel Modak for his valuable suggestions and review of the manuscript. We would also like to thank Mr. Mehboob Shah for meticulous data collection and compilation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Institutional review board approval and waiver of consent were taken since this was a retrospective study.
Rights and permissions
About this article
Cite this article
Qureshi, S.S., Bhagat, M., Harris, C. et al. Outcomes and complications of surgery in patients with intermediate-risk neuroblastoma: experience from an Indian tertiary Cancer Centre. Pediatr Surg Int 34, 435–442 (2018). https://doi.org/10.1007/s00383-018-4241-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-018-4241-5