Abstract
Purpose
Minimally invasive surgery (MIS) has become widely accepted as a technique for abdominal neuroblastoma resection. However, the indications for MIS are still controversial. The aim of this study was to evaluate image-defined risk factors (IDRFs), complications, and oncologic outcomes in patients with abdominal neuroblastomas treated with MIS.
Methods
Between August 1998 and February 2016, MIS was planned for 20 children with abdominal neuroblastomas. Clinical data were retrospectively reviewed and compared between the IDRF-negative and IDRF-positive patients.
Results
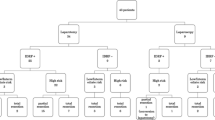
On the basis of the latest IDRF guidelines, five patients were classified as IDRF-positive and four of them had operative complications; namely, partial infarction of the ipsilateral kidney or open conversion. Concerning the two patients who needed open conversion, the primary reason for open conversion was difficulty in dissection of the tumor from the vena cava. Preoperative images of these cases showed either deformation or subtotal encasement of the vena cava. Relapse occurred in three high-risk patients and in none of the low/intermediate-risk patients. No complication occurred in the IDRF-negative cases.
Conclusions
IDRF-negative might be a good indication for MIS for abdominal neuroblastoma. However, deformation or subtotal encasement of the vena cava should be considered as IDRF-positive for MIS.



Similar content being viewed by others
References
Kadamba P, Habib Z, Rossi L (2004) Experience with laparoscopic adrenalectomy in children. J Pediatr Surg 39:764–767
Iwanaka T, Kawashima H, Uchida H (2007) The laparoscopic approach of neuroblastoma. Semin Pediatr Surg 16:259–265
Al-Shanafey S, Habib Z (2008) Feasibility and safety of laparoscopic adrenalectomy in children: special emphasis on neoplastic lesions. J Laparoendosc Adv Surg Tech A 18:306–309
Irtan S, Brisse HJ, Minard-Colin V, Schleiermacher G, Galmiche-Rolland L, Le Cossec C, Elie C, Canale S, Michon J, Valteau-Couanet D, Sarnacki S (2015) Image-defined risk factor assessment of neurogenic tumors after neoadjuvant chemotherapy is useful for predicting intra-operative risk factors and the completeness of resection. Pediatr Blood Cancer 62:1543–1549
de Lagausie P, Berrebi D, Michon J, Philippe-Chomette P, El Ghoneimi A, Garel C, Brisse H, Peuchmaur M, Aigrain Y (2003) Laparoscopic adrenal surgery for neuroblastomas in children. J Urol 170:932–935
International Pediatric Endosurgery Group (2010) IPEG guidelines for the surgical treatment of adrenal masses in children. J Laparoendosc Adv Surg Tech A 20:vii–ix
Monclair T, Brodeur GM, Ambros PF, Brisse HJ, Cecchetto G, Holmes K, Kaneko M, London WB, Matthay KK, Nuchtern JG, von Schweinitz D, Simon T, Cohn SL, Pearson AD (2009) The International Neuroblastoma Risk Group (INRG) staging system: an INRG Task Force report. J Clin Oncol 27:298–303
Brisse HJ, McCarville MB, Granata C, Krug KB, Wootton-Gorges SL, Kanegawa K, Giammarile F, Schmidt M, Shulkin BL, Matthay KK, Lewington VJ, Sarnacki S, Hero B, Kaneko M, London WB, Pearson AD, Cohn SL, Monclair T (2011) Guidelines for imaging and staging of neuroblastic tumors: consensus report from the International Neuroblastoma Risk Group Project. Radiology 261:243–257
Heloury Y, Muthucumaru M, Panabokke G, Cheng W, Kimber C, Leclair MD (2012) Minimally invasive adrenalectomy in children. J Pediatr Surg 47:415–421
Cecchetto G, Mosseri V, De Bernardi B, Helardot P, Monclair T, Costa E, Horcher E, Neuenschwander S, Toma P, Rizzo A, Michon J, Holmes K (2005) Surgical risk factors in primary surgery for localized neuroblastoma: the LNESG1 study of the European International Society of Pediatric Oncology Neuroblastoma Group. J Clin Oncol 23:8483–8489
Simon T, Hero B, Benz-Bohm G, von Schweinitz D, Berthold F (2008) Review of image defined risk factors in localized neuroblastoma patients: results of the GPOH NB97 trial. Pediatr Blood Cancer 50:965–969
Warmann SW, Seitz G, Schaefer JF, Scheel-Walter HG, Leuschner I, Fuchs J (2011) Vascular encasement as element of risk stratification in abdominal neuroblastoma. Surg Oncol 20:231–235
Fumino S, Kimura K, Iehara T, Nishimura M, Nakamura S, Souzaki R, Nishie A, Taguchi T, Hosoi H, Tajiri T (2015) Validity of image-defined risk factors in localized neuroblastoma: a report from two centers in Western Japan. J Pediatr Surg 50:2102–2106
Boutros J, Bond M, Beaudry P, Blair GK, Skarsgard ED (2008) Case selection in minimally invasive surgical treatment of neuroblastoma. Pediatr Surg Int 24:1177–1180
von Schweinitz D, Hero B, Berthold F (2002) The impact of surgical radicality on outcome in childhood neuroblastoma. Eur J Pediatr Surg 12:402–409
Leclair MD, de Lagausie P, Becmeur F, Varlet F, Thomas C, Valla JS, Petit T, Philippe-Chomette P, Mure PY, Sarnacki S, Michon J, Heloury Y (2008) Laparoscopic resection of abdominal neuroblastoma. Ann Surg Oncol 15:117–124
Fuchs J (2015) The role of minimally invasive surgery in pediatric solid tumors. Pediatr Surg Int 31:213–228
Simon T, Haberle B, Hero B, von Schweinitz D, Berthold F (2013) Role of surgery in the treatment of patients with stage 4 neuroblastoma age 18 months or older at diagnosis. J Clin Oncol 31:752–758
Kelleher CM, Smithson L, Nguyen LL, Casadiego G, Nasr A, Irwin MS, Gerstle JT (2013) Clinical outcomes in children with adrenal neuroblastoma undergoing open versus laparoscopic adrenalectomy. J Pediatr Surg 48:1727–1732
Metzelder M, Kuebler J, Shimotakahara A, Vieten G, von Wasielewski R, Ure BM (2008) CO(2) pneumoperitoneum increases systemic but not local tumor spread after intraperitoneal murine neuroblastoma spillage in mice. Surg Endosc 22:2648–2653
Iwanaka T, Arya G, Ziegler MM (1998) Mechanism and prevention of port-site tumor recurrence after laparoscopy in a murine model. J Pediatr Surg 33:457–461
Iwanaka T, Arai M, Yamamoto H, Fukuzawa M, Kubota A, Kouchi K, Nio M, Satomi A, Sasaki F, Yoneda A, Ohhama Y, Takehara H, Morikawa Y, Miyano T (2003) No incidence of port-site recurrence after endosurgical procedure for pediatric malignancies. Pediatr Surg Int 19:200–203
Pentek F, Schulte JH, Schweiger B, Metzelder M, Schundeln MM (2016) Development of Port-Site Metastases Following Thoracoscopic Resection of a Neuroblastoma. Pediatr Blood Cancer 63:149–151
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No competing financial interests exist.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Tanaka, Y., Kawashima, H., Mori, M. et al. Contraindications and image-defined risk factors in laparoscopic resection of abdominal neuroblastoma. Pediatr Surg Int 32, 845–850 (2016). https://doi.org/10.1007/s00383-016-3932-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-016-3932-z