Abstract
Purpose
To determine the outcomes of resection of satellite lesions in PRE-treatment Tumor EXTension (PRETEXT) II and III multifocal hepatoblastoma irrespective of their disappearance after chemotherapy. To compare the overall outcomes of multifocal and unifocal hepatoblastoma.
Methods
Fourteen patients with PRETEXT II (n = 7) and III (n = 7) multifocal hepatoblastoma treated between April 2006 and July 2014 were analyzed and their outcomes were compared with PRETEXT II and III unifocal hepatoblastoma treated in the similar period.
Results
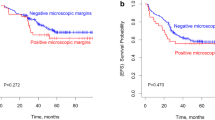
Satellite lesion or the affected segments with disappeared satellite lesions were resected in 11 patients. Amongst them, all relapses were distant except one in the liver. In contrast, two of three patients developed liver relapse when the affected segments were not resected. None of the patients receiving intensive chemotherapy based on SIOPEL-3 guidelines developed a relapse. The 3-year event-free and overall survival were 38.6 and 42.9 % in multifocal hepatoblastoma and 86.4 and 92.4 % in unifocal hepatoblastoma (p = 0.001). Multifocality (p = 0.002) and AFP >10,000 after induction chemotherapy significantly affected event-free survival (p = 0.01).
Conclusion
Multifocal hepatoblastoma is associated with poor outcomes as compared to unifocal hepatoblastoma. These preliminary observations of relapse and the role of chemotherapy intensification deserve further study in a multicenter controlled trial setting.



Similar content being viewed by others
References
Semeraro M, Branchereau S, Maibach R et al (2013) Relapses in hepatoblastoma patients: clinical characteristics and outcome–experience of the International Childhood Liver Tumour Strategy Group (SIOPEL). Eur J Cancer 49:915–922
Saettini F, Conter V, Provenzi M et al (2014) Is multifocality a prognostic factor in childhood hepatoblastoma? Pediatr Blood Cancer 61:1593–1597
Qiao GL, Li L, Cheng W, Ge J, Zhang Z, Wei Y (2014) Predictors of survival after resection of children with hepatoblastoma: a single Asian center experience. Eur J Surg Oncol 40:1533–1539
Ismail H, Broniszczak D, Kaliciński P et al (2012) Changing treatment and outcome of children with hepatoblastoma: analysis of a single center experience over the last 20 years. J Pediatr Surg 47:1331–1339
Otte JB, Pritchard J, Aronson DC et al (2004) Liver transplantation for hepatoblastoma: results from the International Society of Pediatric Oncology (SIOP) Study SIOPEL-1 and Review of the World Experience. Pediatr Blood Cancer 42:74–83
DallIgna P, Cecchetto G, Toffolutti T et al (2013) Multifocal hepatoblastoma: is there a place for partial hepatectomy? Med Pediatr Oncol 40:113–116
Roebuck DJ, Aronson D, Clapuyt P et al (2007) 2005 PRETEXT: a revised staging system for primary malignant liver tumours of childhood developed by the SIOPEL group. Pediatr Radiol 37:123–132
Zsıros J, Maibach R, Shafford E et al (2010) Successful treatment of childhood high-risk hepatoblastoma with dose-intensive multiagent chemotherapy and surgery: final results of the SIOPEL-3HR study. J Clin Oncol 28:2584–2590
Perilongo G, Maibach R, Shafford E et al (2009) Cisplatin versus cisplatin plus doxorubicin for standard-risk hepatoblastoma. N Engl J Med 361:1662–1670
Maibach R, Roebuck D, Brugieres L et al (2012) Prognostic stratification for children with hepatoblastoma: the SIOPEL experience. Eur J Cancer 48:1543–1549
Hishiki T, Matsunaga T, Sasaki F et al (2011) Outcome of hepatoblastomas treated using the Japanese Study Group for Pediatric Tumor (JPLT) protocol 2: report from the JPLT. Pediatr Surg Int 27:1–8
Fuchs J, Rydzynski J, Von Schweinitz D et al (2002) Pretreatment prognostic factors and treatment results in children with hepatoblastoma: a report from the German Cooperative Pediatric Liver Tumor Study HB 94. Cancer 95:172–182
Czauderna P, Otte JB, Aronson DC et al (2005) Guidelines for surgical treatment of hepatoblastoma in the modern era–recommendations from the Childhood Liver Tumour Strategy Group of the International Society of Paediatric Oncology (SIOPEL). Eur J Cancer 41:1031–1036
Otte JB, de Goyet JDV, Reding R (2005) Liver transplantation for hepatoblastoma: indications and contraindications in the modern era. Pediatr Transplant 9:557–656
Srinivasan P, McCall J, Pritchard J et al (2002) Orthotopic liver transplantation for unresectable hepatoblastoma. Transplantation 74:652–655
Stringer MD (2007) The role of liver transplantation in the management of paediatric liver tumours. Ann R Coll Surg Engl 89:12–21
Baertschiger RM, Ozsahin H, Rougemont AL et al (2010) Cure of multifocal panhepatic hepatoblastoma: is liver transplantation always necessary? J Pediatr Surg 45:1030–1036
Rana AN, Qidwai A, Pritchard J, Ashraf MS (2006) Successful treatment of multifocal unresectable hepatoblastoma with chemotherapy only. Pediatr Hematol Oncol 23:153–158
Lautz TB, Ben-Ami T, Tantemsapya N, Gosiengfiao Y, Superina RA et al (2011) Successful nontransplant resection of POST-TEXT III and IV hepatoblastoma. Cancer 117:1976–1983
Schnater JM, Aronson DC, Plaschkes J et al (2002) Surgical view of the treatment of patients with hepatoblastoma: results from the first prospective trial of the International Society of Pediatric Oncology Liver Tumor Study Group. Cancer 94:1111–1120
Acknowledgments
We would like to thank Mr. Mehboob Shah for meticulous data collection and compilation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Qureshi, S.S., Bhagat, M., Kembhavi, S. et al. PRETEXT II–III multifocal hepatoblastoma: significance of resection of satellite lesions irrespective of their disappearance after chemotherapy. Pediatr Surg Int 31, 573–579 (2015). https://doi.org/10.1007/s00383-015-3713-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-015-3713-0