Abstract
Purpose
Trauma is the most important etiology of morbidity and mortality among children. Penetrating injuries to the thorax and abdomen are extremely rare in children. In the present study, we compared the characteristics of patients, management, and outcomes of penetrating thoracic and abdominal trauma in children.
Materials and methods
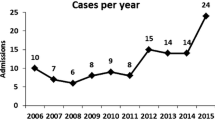
Data from children who were hospitalized for penetrating injuries of the thorax and abdomen from 2006 to 2012 were evaluated retrospectively. These injuries were evaluated with respect to patient details, clinical presentation, circumstances of trauma, management, and outcomes.
Results
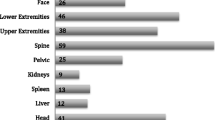
Eighty-four patients were hospitalized for penetrating injuries to the thorax and abdomen. The mean age was 10.3 ± 3.79 years. Patient injuries comprised 26 gunshots injuries and 58 stabbing injuries. Thirty-one patients were wounded in the thorax, 43 were wounded in the abdomen, and 10 were wounded in both the thorax and abdomen. Thirty-one patients had undergone surgical interventions, while the other 53 were managed conservatively. The mean hospital stay was 4.41 ± 6.84 days.
Conclusions
The incidences of penetrating abdominal and thoracic trauma did not differ significantly. Penetrating injuries may be successfully managed by conservative therapy.
Similar content being viewed by others
References
Wessen DE, Stylianos S, Pearl RH (2006) Thoracic injuries, abdominal trauma. In: Grosfeld JL, O’neill JA (eds) Pediatric surgery, 6th edn. Mosby Inc, Philadelpia, pp 275–316
Cotton BA, Nance ML (2004) Penetrating trauma in children. Semin Pediatr Surg 13(2):87–97
Sandler G, Leishman S, Branson H et al (2010) Body wall thickness in adults and children–relevance to penetrating trauma. Injury 41(5):506–509
Ottochian M, Salim A, DuBose J et al (2009) Does age matter? The relationship between age and mortality in penetrating trauma. Injury 40(4):354–357
Schecter SC, Betts J, Schecter WP et al (2012) Pediatric penetrating trauma: the epidemic continues. J Trauma Acute Care Surg 73(3):721–725
Adesanya AA, da Rocha-Afodu JT, Ekanem EE et al (2000) Factors affecting mortality and morbidity in patients with abdominal gunshot wounds. Injury 31(6):397–404
Melling L, Lansdale N, Mullassery D et al (2012) Penetrating assaults in children: often non-fatal near-miss events with opportunities for prevention in the UK. Injury 43(12):2088–2093
Adorisio O, Elia A, Pinzauti E et al (2008) The importance of a multidisciplinary approach in a child with major abdominal penetrating trauma. Pediatr Emerg Care 24(1):34–36
Moore K (2012) The knife and gun club just adjourned: managing penetrating injuries in the emergency department. J Emerg Nurs 38(1):102–103
Holland AJ, Kirby R, Browne GJ et al (2002) Penetrating injuries in children: is there a message? J Paediatr Child Health 38(5):487–491
Morrison JJ, Clasper JC, Gibb I et al (2011) Management of penetrating abdominal trauma in the conflict environment: the role of computed tomography scanning. World J Surg 35(1):27–33
Cobanoğlu U, Yalçinkaya I (2010) Thoracic injuries. Ulus Travma Acil Cerrahi Derg 16(1):77–83
Madiba TE, Thomson SR, Mdlalose N (2001) Penetrating chest injuries in the firearm era. Injury 32(1):13–16
Como JJ, Bokhari F, Chiu WC et al (2010) Practice management guidelines for selective nonoperative management of penetrating abdominal trauma. J Trauma 68(3):721–733
Salim A, Velmahos GC (2002) When to operate on abdominal gunshot wounds. Scand J Surg 91(1):62–66
Shaftan GW (1960) Indications for operation in abdominal trauma. Am J Surg 99:657–664
Cigdem MK, Onen A, Siga M et al (2009) Selective nonoperative management of penetrating abdominal injuries in children. J Trauma 67(6):1284–1286
Gaines BA, Rutkoski JD (2010) The role of laparoscopy in pediatric trauma. Semin Pediatr Surg 19(4):300–303
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Boleken, M.E., Cevik, M., Yagiz, B. et al. The characteristics and outcomes of penetrating thoracic and abdominal trauma among children. Pediatr Surg Int 29, 795–800 (2013). https://doi.org/10.1007/s00383-013-3339-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00383-013-3339-z