Abstract
Purpose
Posterior fossa surgeries for pediatric tumors pose challenges in achieving optimal dural repair and duraplasty is usually required. Autografts, allografts, xenografts, and synthetic substitutes can be used for duraplasty. Autologous cervical fascia can be a safe and reliable graft option for duraplasty after posterior fossa surgeries. This study aims to investigate the outcomes of duraplasty with autologous cervical fascial graft in children after posterior fossa surgery for pediatric brain tumors.
Methods
Pediatric patients with posterior fossa tumor who underwent surgery between March 2001 and August 2022 were retrospectively reviewed. Data on demographics, preoperative symptoms, diagnosis, tumor characteristics, hydrocephalus history, and postoperative complications, including cerebrospinal fluid (CSF) leakage, pseudomeningocele, and meningitis were collected. Logistic regression analysis was performed to explore risk factors for postoperative complications.
Results
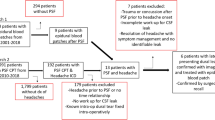
Patient cohort included 214 patients. Autologous cervical fascia was used in all patients for duraplasty. Mean age was 7.9 ± 5.3 years. Fifty-seven patients (26.6%) had preoperative hydrocephalus and 14 patients (6.5%) received VPS or EVD perioperatively. Postoperative hydrocephalus was present in 31 patients (14.5%). Rates of CSF leak, pseudomeningocele, and meningitis were 4.2%, 2.8%, and 4.2% respectively. Logistic regression analysis revealed that postoperative EVD and VPS placement were the factors associated with postoperative complications.
Conclusion
Autologous cervical fascia is a safe and reliable option for duraplasty with minimal risk of postoperative complications. The straightforward surgical technique and with no additional cost for harvesting the graft renders autologous cervical fascia a favorable alternative for resource-limited countries or surgical settings.

Similar content being viewed by others
Data Availability
The data that support the findings of this study are available on reasonable request from the corresponding author. The data are not publicly available due to privacy or ethical restrictions.
Abbreviations
- EVD:
-
External ventricular drain
- VPS:
-
Ventriculoperitoneal shunt
- CSF:
-
Cerebrospinal fluid
References
Eser MT, Hanalioglu S, Cetiner MZ, Dinc S, Peker HO, Sorar M et al (2019) Identification of risk factors for postoperative cerebrospinal fluid leakage and comparison of two alternative dural augmentation techniques in posterior fossa and spinal surgeries. Turk Neurosurg 29(3):377–385
Moskowitz SI, Liu J, Krishnaney AA. Postoperative complications associated with dural substitutes in suboccipital craniotomies. Neurosurgery. 2009;64(3 Suppl):ons28–33; discussion ons-4.
Mammadkhanli O, Elbir C, Hanalioglu S, Canbay S (2020) Subfascial drainage and clipping technique for treatment of cerebrospinal fluid leak following spinal surgery. Neurosciences (Riyadh) 25(1):50–54
Wang B, Shi W, Zhang Y, Wang Y, Yang C, Huang T, et al (2022) Duraplasty with autologous nuchal ligament fascia to reduce postoperative complications in pediatric patients undergoing neoplasia resection with a suboccipital midline approach. J Neurosurg Pediatr 1–9
Zhao Y, Chen L, Zhang J, You N, Liu Y, Yao A et al (2020) Duraplasty with cervical fascia autograft to reduce postoperative complications of posterior fossa tumor surgery with suboccipital midline approach. World Neurosurg 134:e1115–e1120
Martínez-Lage JF, Pérez-Espejo MA, Palazón JH, López Hernández F, Puerta P (2006) Autologous tissues for dural grafting in children: a report of 56 cases. Childs Nerv Syst 22(2):139–144
Lam FC, Kasper E. Augmented autologous pericranium duraplasty in 100 posterior fossa surgeries--a retrospective case series. Neurosurgery. 2012;71(2 Suppl Operative):ons302–7.
Wang J, Li P, Liang B, Ding X, Gao H, Feng E (2023) The comparison of the watertight and non-watertight dural closure in supratentorial craniotomy: a single-institute 10-year experience with 698 patients. Medicine 102(37)
Roth J, Benvenisti H, Constantini S (2018) Watertight dural closure in pediatric craniotomies-is it really necessary? World Neurosurg 114:e743–e746
Hale AT, Gannon SR, Zhao S et al (2019) Graft dural closure is associated with a reduction in CSF leak and hydrocephalus in pediatric patients undergoing posterior fossa brain tumor resection. J Neurosurg Pediatr 1–7
Malliti M, Page P, Gury C et al (2004) Comparison of deep wound infection rates using a synthetic dural substitute (neuro-patch) or pericranium graft for dural closure. a clinical review of 1 year. Neurosurgery 54(3):599–603
Dlouhy BJ, Menezes AH (2018) Autologous cervical fascia duraplasty in 123 children and adults with Chiari malformation type I: surgical technique and complications. Journal of Neurosurgery: Pediatrics PED 22(3):297–305
Djordjevic Z, Milosavlijevic B (1974) Postoperative cerebrospinal fluid fistulas and their treatment. J Neurosurg Sci 18(2):109–111
Abbe R (1895) Rubber tissue for meningeal adhesions. Trans Amer Surg Ass 13:490–491
Narotam PK, Qiao F, Nathoo N (2009) Collagen matrix duraplasty for posterior fossa surgery: evaluation of surgical technique in 52 adult patients. Clinical article J Neurosurg 111(2):380–386
Sabatino G, Della Pepa GM, Bianchi F, Capone G, Rigante L, Albanese A et al (2014) Autologous dural substitutes: a prospective study. Clin Neurol Neurosurg 116:20–23
Stevens EA, Powers AK, Sweasey TA, Tatter SB, Ojemann RG (2009) Simplified harvest of autologous pericranium for duraplasty in Chiari malformation Type I. Technical note J Neurosurg Spine 11(1):80–83
Author information
Authors and Affiliations
Contributions
Conceptualization: Sahin Hanalioglu, Burcak Bilginer, Ahmet Ilkay Isikay; methodology: Neslihan Nisa Gecici, Muhammet Enes Gurses; data analysis: Neslihan Nisa Gecici, Sahin Hanalioglu; writing—original draft preparation: Neslihan Nisa Gecici; writing—review and editing: Sahin Hanalioglu, Muhammet Enes Gurses; supervision: Sahin Hanalioglu, Burcak Bilginer, Ahmet Ilkay Isikay.
Corresponding author
Ethics declarations
Ethics approval
This study is approved by the ethics committee of the hospital where the research was conducted and informed consent is obtained from patients’ legal guardians.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (MP4 196073 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gecici, N.N., Gurses, M.E., Isikay, A. et al. Duraplasty with autologous cervical fascia in pediatric posterior fossa tumor surgery: a single-center experience with 214 cases. Childs Nerv Syst (2024). https://doi.org/10.1007/s00381-024-06351-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00381-024-06351-6