Abstract
Purpose
Vascular anomalies are classified as either vascular tumors or vascular malformations. Vascular malformations can be difficult to diagnose and treat in the pediatric population and can masquerade as malignant processes. Understanding the genetics behind vascular malformations can lead to identification of specific mutations which can be treated with targeted immunotherapy.
Methods
Our case presents a pediatric patient with progressively enlarging vascular malformation despite multiple surgical resections and systemic medical treatments who underwent genetic evaluation and was found to have PIK3CA mutation.
Results
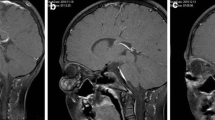
After identification of PIK3CA mutation, our patient was successfully treated with the p110ɑ-specific inhibitor, alpelisib, with both shrinkage of malformation on follow-up imaging as well as gains in her developmental milestones.
Conclusion
Progressive vascular malformations in the pediatric population can be hard to diagnose and treat and are thought to arise from somatic mutations. Our case highlights a patient with progressive malformation despite multiple surgical resections who was successfully treated with targeted immunotherapy after proper identification of genetic mutation.


Similar content being viewed by others
References
Flucke U, Karanian M, Broek RW, Thway K (2020) Soft Tissue Special Issue: Perivascular and vascular tumors of the head and neck. Head Neck Pathol 14(1):21–32. https://doi.org/10.1007/s12105-020-01129-z
Kunimoto K, Yamamoto Y, Jinnin M (2022) ISSVA classification of vascular anomalies and molecular biology. Int J Mol Sci 23(4):2358. https://doi.org/10.3390/ijms23042358. PMID: 35216474; PMCID: PMC8876303
Sadick M, Müller-Wille R, Wildgruber M, Wohlgemuth WA (2018) Vascular anomalies (part I): classification and diagnostics of vascular anomalies. Rofo 90(9):825–835. English. https://doi.org/10.1055/a-0620-8925. Epub 2018 Jun 6. PMID: 29874693
Mahady K, Thust S, Berkeley R, Stuart S, Barnacle A, Robertson F, Mankad K (2015) Vascular anomalies of the head and neck in children. Quant Imaging Med Surg 5(6):886–897. https://doi.org/10.3978/j.issn.2223-4292.2015.04.06
Vikkula M, Boon LM, Mulliken JB (2001) Molecular genetics of vascular malformations. Matrix Biol 20(5–6):327–335. https://doi.org/10.1016/s0945-053x(01)00150-0
Wassef M, Blei F, Adams D, Alomari A, Baselga E, Berenstein A et al (2015) Vascular Anomalies Classification: Recommendations From the International Society for the Study of Vascular Anomalies. Pediatrics 136(1):e203–e214. https://doi.org/10.1542/peds.2014-3673
Watson KD, Kim KR, Blatt J (2022) How we approach complex vascular anomalies and overgrowth syndromes. Pediatr Blood Cancer 69(S3). https://doi.org/10.1002/pbc.29273
Kalish JM, Biesecker LG, Brioude F, Deardorff MA, Di Cesare-Merlone A, Druley T, Ferrero GB, Lapunzina P, Larizza L, Maas S, Macchiaiolo M, Maher ER, Maitz S, Martinez-Agosto JA, Mussa A, Robinson P, Russo S, Selicorni A, Hennekam RC (2017) Nomenclature and definition in asymmetric regional body overgrowth. Am J Med Genet A 173(7):1735–1738. https://doi.org/10.1002/ajmg.a.38266
Jarrett DY, Ali M, Chaudry G (2013) Imaging of vascular anomalies. Dermatol Clin 31(2):251–266. https://doi.org/10.1016/j.det.2012.12.004
Frieden IJ, Rogers M, Garzon MC (2009) Conditions masquerading as infantile haemangioma: part 1. Australas J Dermatol 50(2):77–97. https://doi.org/10.1111/j.1440-0960.2009.00514_1.x
Borst AJ, Nakano TA, Blei F, Adams DM, Duis J (2020) A primer on a comprehensive genetic approach to vascular anomalies. Front Pedia 8. https://doi.org/10.3389/fped.2020.579591
Limaye N, Kangas J, Mendola A, Godfraind C, Schlögel MJ, Helaers R, Eklund L, Boon LM, Vikkula M (2015) Somatic activating PIK3CA mutations cause venous malformation. Am J Hum Genet 97(6):914–921. https://doi.org/10.1016/j.ajhg.2015.11.011
Nguyen H-L, Boon LM, Vikkula M (2014) Genetics of vascular malformations. Semin Pediatr Surg 23:2216. https://doi.org/10.1053/j.sempedsurg.2014.06.014
Keppler-Noreuil KM, Rios JJ, Parker VER, Semple RK, Lindhurst MJ, Sapp JC, Alomari A, Ezaki M, Dobyns W, Biesecker LG (2014) pik3ca -related overgrowth spectrum (PROS): Diagnostic and testing eligibility criteria, differential diagnosis, and evaluation. Am J Med Genet A 167(2):287–295. https://doi.org/10.1002/ajmg.a.36836
Tsujioka Y, Nozaki T, Niimi Y, Starkey J, Hasegawa D, Kondo M, Enokizono M, Makidono A, Kono T, Jinzaki M (2022) Syndromic vascular malformations related to the PIK3CA and RAS pathways: A clinical and imaging review. Clin Imaging 89:162–173. https://doi.org/10.1016/j.clinimag.2022.06.017. Epub 2022 Jul 2 PMID: 35849880
Castel P, Carmona FJ, Grego-Bessa J, Berger MF, Viale A, Anderson KV, Bague S, Scaltriti M, Antonescu CR, Baselga E, Baselga J (2016) Somatic pik3ca mutations as a driver of sporadic venous malformations. Sci Trans Med 8(332). https://doi.org/10.1126/scitranslmed.aaf1164
Castillo SD, Tzouanacou E, Zaw-Thin M, Berenjeno IM, Parker VE, Chivite I, Milà-Guasch M, Pearce W, Solomon I, Angulo-Urarte A, Figueiredo AM et al (2016) Somatic activating mutations in pik3ca cause sporadic venous malformations in mice and humans. Sci Trans Med 8(332). https://doi.org/10.1126/scitranslmed.aad9982
Chung HY, Chung JY, Lee DG, Yang JD, Baik BS, Hwang SG, Cho BC (2004) Surgical treatment of ossified cephalhematoma. J Craniofac Surg 15(5):774–779. https://doi.org/10.1097/00001665-200409000-00015
Heckl S, Aschoff A, Kunze S (2002) Cavernomas of the skull: review of the literature 1975–2000. Neurosurg Rev 25(1–2):56–62; discussion 66–7. https://doi.org/10.1007/s101430100180
Canaud G, López Gutiérrez JC, Irvine A, Ankrah N, Papadimitriou A, Ridolfi A, Adams DM (2021) LBA23 Epik-P1: Retrospective Chart Review Study of patients (PTS) with PIK3CA-related overgrowth spectrum (PROS) who have received alpelisib (ALP) as part of a compassionate use programme. Annal Oncol 32. https://doi.org/10.1016/j.annonc.2021.08.2097
Author information
Authors and Affiliations
Contributions
A.M. wrote the main manuscript text. L.Z. assisted with writing of the main manuscript text. A.A. assisted with the diagnosis of the patient. N.M. assisted with the diagnosis of the patient. M.B. assisted with tissue diagnosis of the patient. E.B. assisted with radiographic diagnosis and preparing figures. D.S. assisted with surgical resection and diagnosis. M.G. assisted with surgical resection. M.S. was the primary surgeon and assisted with diagnosis and treatment of the patient. He is the most senior author of the paper. All authors reviewed the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Medina, A., Zima, L., Atkinson, A. et al. Progressive vascular tumor in infant: A case report and literature review of PIK3CA vascular malformation. Childs Nerv Syst 40, 1005–1010 (2024). https://doi.org/10.1007/s00381-024-06290-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-024-06290-2