Abstract
Background
Traumatic retroclival hematomas (RCHs) are infrequent occurrences among the pediatric population. The existing body of research pertaining to these hematomas primarily consists of case reports or small case series, which do not provide adequate guidance for managing this condition.
Objective
This study aims to present a report on four cases of RCHs. Additionally, we aim to conduct a systematic review to consolidate the existing literature on pediatric RCHs.
Methods
The authors conducted a systematic review in accordance with the PRISMA and CARE guidelines. A multivariate logistic regression model was developed to evaluate the potential impact of various clinical variables on clinical outcomes. The study also documented four of our cases, one of which was a rare occurrence of spontaneous subdural RCH.
Results
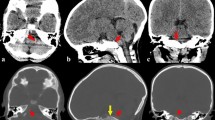
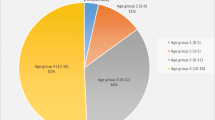
A total of 62 traumatic RCHs have been documented in the literature. We documented three cases of traumatic RCHs and one case of spontaneous RCH. A systematic analysis of 65 traumatic RCHs was performed. Of trauma cases, 64.6% demonstrated craniocervical junction instability with 83.3% ligamentous involvement. Thirty-five patients were males. 50.7% were aged between 5 and 9 years. Cranial nerve palsies occurred in 29 patients (27 had abducent palsy), 26 of which resolved within 6 months of trauma. 23.5% underwent surgery, and 76.5% were conservatively managed. Surgeries targeted hematomas, hydrocephalus, or craniocervical instability. Approaches to hematomas included transclival and far/extreme lateral suboccipital approaches. Clinical outcome was good in 75.4% and intermediate or poor in 24.6%. Logistic regression suggested an association between craniocervical junction injuries and poor or intermediate outcomes (OR 4.88, 95% CI (1.17, 27.19), p = 0.04).
Conclusion
Pediatric RCHs are mostly traumatic and extradural. Children between 5 and 9 years old are most vulnerable. Craniocervical junction injuries, mainly ligamentous, are common in RCHs and are associated with intermediate or poor outcomes. Cervical MRI could be important in cases of trauma to rule out ligamentous injuries of the craniocervical junction. The small size of RCHs should not exempt the careful assessment of craniocervical junction instability. Cranial nerve palsies are common and usually resolve within 6 months. Conservative treatment is typical unless brainstem compression, hydrocephalus, or craniocervical junction instability exists.






Similar content being viewed by others
Availability of data and material
The data and material are available on contact with Y. H. K., email yakhormi@jazanu.edu.sa.
Abbreviations
- CARE:
-
CaSe reports checklist guidelines
- CVJI:
-
Craniocervical junction injury
- CSF:
-
Cerebrospinal fluid
- CT:
-
Computed tomography
- ER:
-
Emergency room
- EVD:
-
External ventricular drain
- ICU:
-
Intensive care unit
- MVA:
-
Motor vehicle accident
- SDH:
-
Subdural hematoma
- PRISMA:
-
Preferred reporting items for systematic reviews and meta-analyses
- RCH:
-
Retroclival hematoma
References
Agrawal D, Cochrane DD (2006) Traumatic retroclival epidural hematoma - a pediatric entity? Childs Nerv Syst 22(7):670–673. https://doi.org/10.1007/s00381-006-0059-x
Mizushima H, Kobayashi N, Sawabe Y et al (1998) Epidural hematoma of the clivus. Case report J Neurosurg 88(3):590–593. https://doi.org/10.3171/jns.1998.88.3.0590
Myers DJ, Moossy JJ, Ragni MV (1995) Fatal clival subdural hematoma in a hemophiliac. Ann Emerg Med 25(2):249–252. https://doi.org/10.1016/s0196-0644(95)70333-0
Sahlu A, Getachew K, Mekonnen A (2020) Traumatic retroclival subdural hematoma in a child with hemophilia. World Neurosurg 133:112–120. https://doi.org/10.1016/j.wneu.2019.09.059
Kurosu A, Amano K, Kubo O et al (1990) Clivus epidural hematoma. Case report J Neurosurg 72(4):660–662. https://doi.org/10.3171/jns.1990.72.4.0660
Marks SM, Paramaraswaren RN, Johnston RA (1997) Transoral evacuation of a clivus extradural haematoma with good recovery: a case report. Br J Neurosurg 11(3):245–247. https://doi.org/10.1080/02688699746339
Dal Bo S, Cenni P, Marchetti F (2015) Retroclival hematoma. J Pediatr 166(3):773. https://doi.org/10.1016/j.jpeds.2014.12.034
Ahn ES, Smith ER (2005) Acute clival and spinal subdural hematoma with spontaneous resolution: clinical and radiographic correlation in support of a proposed pathophysiological mechanism. Case report J Neurosurg 103(2 Suppl):175–179. https://doi.org/10.3171/ped.2005.103.2.0175
Becco de Souza R, Brasileiro de Aguiar G, Sette Dos Santos ME, Acioly MA (2011) Retroclival epidural hematoma in a child affected by whiplash cervical injury: a typical case of a rare condition. Pediatr Neurosurg 47(4):288–291. https://doi.org/10.1159/000335446
Calisaneller T, Ozdemir O, Altinors N (2006) Posttraumatic acute bilateral abducens nerve palsy in a child. Childs Nerv Syst 22(7):726–728. https://doi.org/10.1007/s00381-005-0036-9
Catalá-Antúnez I, de Quintana-Schmidt C, Clavel-Laria P, Montes-Graciano G, Molet-Teixidó J (2011) Paresia VI par craneal por hematoma subdural retroclival y espinal postraumatico: presentacin de un caso y revision de la literatura [Abducens nerve palsy due to postraumatic retroclival and spinal subdural hematoma: case report and literature review]. Neurocirugia (Astur) 22(4):337–341
Dayaratne S, Rajapakse D, Jayaweera N, Wadanamby S, Rajapakse T (2015) A case of post-traumatic retroclival subdural haematoma. Ceylon Med J 60(4):159–160. https://doi.org/10.4038/cmj.v60i4.8225
Diaz R, Zouros A, Stewart GM (2010) Atlanto-occipital dislocation with retroclival hematoma in a pediatric patient presenting to the emergency department. Pediatr Emerg Care 26(11):843–847. https://doi.org/10.1097/PEC.0b013e3181fb0e4c
Fiester P, Rao D, Andreou S, Soule E, Patel J (2021) Pediatric retroclival epidural hematoma in the acute trauma setting: a sign of tectorial membrane stripping injury. AJR Am J Roentgenol 216(6):1641–1648. https://doi.org/10.2214/AJR.20.22957
Garton HJ, Gebarski SS, Ahmad O, Trobe JD (2010) Clival epidural hematoma in traumatic sixth cranial nerve palsies combined with cervical injuries. J Neuroophthalmol 30(1):18–25. https://doi.org/10.1097/WNO.0b013e3181ce14ae
Itshayek E, Goldman J, Rosenthal G, Chikoya L, Gomori M, Segal R (2006) Extradural hematoma of the clivus, not limited to the severely injured patient: case report and review of the literature. J Trauma 60(2):417–420. https://doi.org/10.1097/01.ta.0000204617.70599.c4
Goodman JM, Kuzma B, Britt P (1997) Retroclival hematoma secondary to pituitary apoplexy. Surg Neurol 47(1):79–80. https://doi.org/10.1016/s0090-3019(96)00384-9
Kwon TH, Joy H, Park YK, Chung HS (2008) Traumatic retroclival epidural hematoma in a child: case report. Neurol Med Chir (Tokyo) 48(8):347–350. https://doi.org/10.2176/nmc.48.347
Lee IL, Vasquez LF, Tyroch AH, Trier TT (2017) Association of atlanto-occipital dislocation, retroclival hematoma, and hydrocephalus: management and survival in a pediatric patient. J Neurol Surg Rep 78(1):e53–e58. https://doi.org/10.1055/s-0037-1600914
McDougall CM, Sankar T, Mehta V, Pugh JA (2011) Pediatric traumatic retroclival epidural hematoma. Can J Neurol Sci 38(2):338–340. https://doi.org/10.1017/s0317167100011550
Nguyen HS, Shabani S, Lew S (2016) Isolated traumatic retroclival hematoma: case report and review of literature. Childs Nerv Syst 32(9):1749–1755. https://doi.org/10.1007/s00381-016-3098-y
Paterakis KN, Karantanas AH, Hadjigeorgiou GM, Anagnostopoulos V, Karavelis A (2005) Retroclival epidural hematoma secondary to a longitudinal clivus fracture. Clin Neurol Neurosurg 108(1):67–72. https://doi.org/10.1016/j.clineuro.2004.11.010
Samanci Y, Baskurt I, Celik SE (2019) Traumatic retroclival epidural hematoma. Pediatr Emerg Care 35(10):e184–e187. https://doi.org/10.1097/PEC.0000000000001756
Sridhar K, Venkateswara PG, Ramakrishnaiah S, Iyer V (2010) Posttraumatic retroclival acute subdural hematoma: report of two cases and review of literature. Neurol India 58(6):945–948. https://doi.org/10.4103/0028-3886.73756
Zabalo G, Ortega R, Díaz J et al (2017) Retroclival epidural haematoma: a diagnosis to suspect. Report of three cases and review of the literature. Acta Neurochir (Wien) 159(8):1571–1576. https://doi.org/10.1007/s00701-017-3214-0
Papadopoulos SM, Dickman CA, Sonntag VK, Rekate HL, Spetzler RF (1991) Traumatic atlantooccipital dislocation with survival. Neurosurgery 28(4):574–579. https://doi.org/10.1097/00006123-199104000-00015
Orrison WW, Rogde S, Kinard RE et al (1986) Clivus epidural hematoma: a case report. Neurosurgery 18(2):194–196. https://doi.org/10.1227/00006123-198602000-00014
Yama N, Kano H, Nara S et al (2007) The value of multidetector row computed tomography in the diagnosis of traumatic clivus epidural hematoma in children: a three-year experience. J Trauma 62(4):898–901. https://doi.org/10.1097/01.ta.0000221058.72995.c9
Fiester P, Soule E, Natter P, Rao D (2019) Tectorial membrane injury in adult and pediatric trauma patients: a retrospective review and proposed classification scheme. Emerg Radiol 26(6):615–622. https://doi.org/10.1007/s10140-019-01710-2
Shojima H, Hayashi Y, Tamase A, Takata S, Iizuka H (2022) Traumatic retroclival epidural hematoma associated with reversible ipsilateral internal carotid artery stenosis. Childs Nerv Syst 38(2):485–489. https://doi.org/10.1007/s00381-021-05276-8
Desimpel J, Parizel PM, Dekeyzer S (2020) Posttraumatic retroclival hematoma: a case report. Acta Neurol Belg 120(1):177–178. https://doi.org/10.1007/s13760-019-01117-3
Author information
Authors and Affiliations
Contributions
Study concept and design (Y. H. K. and M. M. E. A.) data acquisition and analysis (M. M. E. A. and A. I. H.), evaluation and re-classification of all published radiographs (H.H., M. M. E. A., and A. I. H.), writing of manuscript, figure design, table design, critically revising manuscript, and review of submitted manuscript: (all authors), study supervision (M. M. E. A.).
Corresponding author
Ethics declarations
Ethical approval and consent to participate
This systematic review was not registered in PROSPERO or other review databases. No IRB/ethics committee approval was needed for this case presentation and systematic review. We conducted our study following the principles outlined in the Declaration of Helsinki.
Consent for publication
Written consent was obtained in our four cases from the parents or the legal guardians.
Conflict of interest
The authors declare no conflict of interests.
Disclaimer
The topic was presented as a poster presentation in the 48th Annual Meeting of the International Society for Pediatric Neurosurgery (ISPN), 06–10 December 2022, Singapore. Part of this work was accepted and presented as an oral presentation in 16th Annual Meeting of the Saudi Association of Neurological Surgery (SANS), Riyadh, KSA, 25–27 March 2022.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Khormi, Y.H., Aly, M.M., Hamda, H.K. et al. Pediatric retroclival hematomas. Childs Nerv Syst 40, 1389–1404 (2024). https://doi.org/10.1007/s00381-023-06233-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-023-06233-3