Abstract
Background
Extradural malignant rhabdoid tumors of the spine are highly malignant and invasive tumors (WHO grade IV) with poor prognosis, most frequently occurring in young children before 2 years of age. Pain and motor deficit are the most common presenting signs.
Case description
We report a case of a 2-year-old girl presenting with axial ataxia and paraparesis related to an extradural malignant rhabdoid tumor causing posterior thoracic spinal cord compression (D3–D6). She underwent two near-total removal of the tumor, adjuvant chemotherapy according to the Eu-Rhab protocol and proton beam therapy. She then developed multiple cranial nerve paresis (meningeal carcinomatosis) after 4 cycles of chemotherapy and died at 4.32 months of follow-up.
Discussion and conclusion
The role of the PET scan was essential to guide us to remove a residue, while two concomitant spinal MRIs were considered negative. We reviewed the 16 cases reported in the literature. Multiple surgeries and radiotherapy seem to be correlated with longer survival. No child younger than 2 years old had a documented survival higher than 4.32 months.






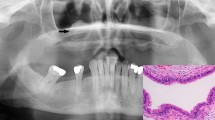
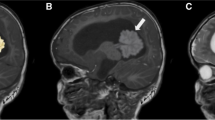
Similar content being viewed by others
Availability of data and material
All medical data are available and recorded in a secure computerized medical file.
Code availability
Not applicable.
References
Xie S, Yang J, Ma Y, Li K, Dong K, Yao W (2022) Analysis on diagnosis and treatments of 16 cases of extracranial malignant rhabdoid tumor in children. Transl Cancer Res 11(4):629–638
Uwineza A, Gill H, Buckley P, Owens C, Capra M, O’Sullivan C, McDermott M, Brett F, Farrell M, Pears J, O’Sullivan MJ (2014) Rhabdoid tumor: the Irish experience 1986–2013. Cancer Genet 207(9):398–402
Heuer GG, Kiefer H, Judkins AR, Belasco J, Biegel JA, Jackson EM et al (2010) Surgical treatment of a clival-C2 atypical teratoid/rhabdoid tumor. J Neurosurg Pediatr 5:75–79
Li D, Heiferman DM, Syed HR, Santos JG, Bowman RM, DiPatri AJ Jr, Tomita T, Wadhwani NR, Alden TD (2019) Pediatric primary spinal atypical teratoid rhabdoid tumor: a case series and review of the literature. J Neurosurg Pediatr 24(3):267–283
Lee RS, Stewart C, Carter SL, Ambrogio L, Cibulskis K, Sougnez C, Lawrence MS, Auclair D, Mora J, Golub TR et al (2012) A remarkably simple genome underlies highly malignant pediatric rhabdoid cancers. J Clin Investig 122:2983–2988
Hasselblatt M, Gesk S, Oyen F, Rossi S, Viscardi E, Giangaspero F, Giannini C, Judkins AR, Frühwald MC, Obser T, Schneppenheim R, Siebert R, Paulus W (2011) Nonsense mutation and inactivation of SMARCA4 (BRG1) in an atypical teratoid/rhabdoid tumor showing retained SMARCB1 (INI1) expression. Am J Surg Pathol 35(6):933–935
Schneppenheim R, Frühwald MC, Gesk S, Hasselblatt M, Jeibmann A, Kordes U, Kreuz M, Leuschner I, Subero JIM, Obser T et al (2010) Germline nonsense mutation and somatic inactivation of SMARCA4/BRG1 in a family with rhabdoid tumor predisposition syndrome. Am J Hum Genet 86:279–284
Kenny C, O’Meara E, Ulaş M, Hokamp K, O’Sullivan MJ (2021) Global chromatin changes resulting from single-gene inactivation-the role of SMARCB1 in malignant rhabdoid tumor. Cancers (Basel) 13(11):2561
Agrawal A, Bhake A, Cincu R (2009) Giant lumbar paraspinal atypical teratoid/rhabdoid tumor in a child. J Cancer Res Ther 5:318–320
Bourdeaut F, Fréneaux P, Thuille B, Bergeron C, Laurence V, Brugières L (2008) Extra-renal non-cerebral rhabdoid tumours. Pediatr Blood Cancer 51(3):363–368
Dobbs MD, Correa H, Schwartz HS, Kan JH (2011) Extrarenal rhabdoid tumor mimicking a sacral peripheral nerve sheath tumor. Skeletal Radiol 40:1363–1368
Horie H, Etoh T, Maie M (1992) Cytogenetic characteristics of a malignant rhabdoid tumor arising from the paravertebral region. A case report. Acta Pathol Jpn 42:460–465
Mahmood MN, Salama ME, Shah VV (2003) Pathologic quiz case: an 11-year-old boy with cervical lymphadenopathy. Metastatic malignant extrarenal rhabdoid tumor. Arch Pathol Lab Med 127:e361–e362
Nishimoto T, Nomura S, Fukano R, Kimura T, Ikeda E, Suzuki M (2018) A primary extradural malignant rhabdoid tumor at the craniovertebral junction in a 3-year-old boy. Childs Nerv Syst 34:367–371
Singla N, Kapoor A, Chatterjee D, Radotra BD (2016) Ultra early recurrence in giant congenital malignant rhabdoid tumor of spine. Childs Nerv Syst 32:2471–2474
Tamiya T, Nakashima H, Ono Y, Kawada S, Hamazaki S, Furuta T et al (2000) Spinal atypical teratoid/rhabdoid tumor in an infant. Pediatr Neurosurg 32:145–149
Tang Y, Li S, Qu J, Zhou Y, Xiao J (2015) Malignant rhabdoid tumor with cervical vertebra involvement in a teenage child: case report and review of the literature. Pediatr Neurosurg 50:173–178
Tsitsopoulos PP, Marinos K, Chochliourou E, Theologou M, Nikolaidou C, Sdougka M, Tsonidis CA (2020) Infantile atypical teratoid rhabdoid tumor of the spine presenting with acute hydrocephalus. Pediatr Neurosurg 55(5):313–318
Xin X, Zhu B, Shen J, Tian C, Fan X, Liu BR (2014) A primary spinal extradural atypical teratoid/rhabdoid tumor of the cervical spine with bony involvement. J Child Neurol 29(5):670–673
Bartelheim K, Nemes K, Seeringer A, Kerl K, Buechner J, Boos J, Graf N, Dürken M, Gerss J, Hasselblatt M, Kortmann RD, Teichert von Luettichau I, Nagel I, Nygaard R, Oyen F, Quiroga E, Schlegel PG, Schmid I, Schneppenheim R, Siebert R, Solano-Paez P, Timmermann B, Warmuth-Metz M, Frühwald MC (2016) Improved 6-year overall survival in AT/RT - results of the registry study Rhabdoid 2007. Cancer Med 5(8):1765–1775
Funding
No financial support was received for this work.
Author information
Authors and Affiliations
Contributions
EV: conception of the draft, conception of the figures and tables, clinical management of the patient. HR: substantial contributions to the conception of the work, clinical management of the patient. VJ: substantial contributions to the conception and design of the work, clinical management of the patient. LD: substantial contributions to the conception and design of the work, conception of the figures. AVD: conception of the draft, substantial contributions to the conception and design of the work, clinical management of the patient. CR: substantial contributions to the conception and design of the work.
Corresponding author
Ethics declarations
Ethics approval
The patient’s family has consented to the submission of the case report for submission to the journal.
Consent to participate
The patient’s family has consented to the submission of the case report for submission to the journal.
Consent for publication
The patient’s family has consented to the submission of the case report for submission to the journal.
Conflict of interest
The authors declare no competing interests.
Disclaimer
The manuscript is an original contribution, not submitted simultaneously in another journal or published elsewhere, partially or in full in any form or language. Results are presented clearly, honestly, and without fabrication, falsification or inappropriate data manipulation (including image based manipulation). Authors adhere to discipline-specific rules for acquiring, selecting and processing data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Vigneul, E., Rooijakkers, H., Joris, V. et al. Extradural malignant rhabdoid tumor of the spine in children: A case-based review. Childs Nerv Syst 40, 979–986 (2024). https://doi.org/10.1007/s00381-023-06224-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-023-06224-4