Abstract
Background
The diagnosis of glioblastoma (GBM) in infants aged ≤ 1 year is extremely rare, and its comparability to the more common adult diagnosis is underexplored. Correspondingly, the objective of this study was to interrogate a national cancer database to elucidate the typical survival and clinical profile of this demographic.
Methods
All GBM patients aged ≤ 1 year in the U.S. National Cancer Database (NCDB) between 2005 and 2016 were retrospectively reviewed. Data were summarized, and overall survival (OS) was modeled using Kaplan–Meier and Cox regression analyses.
Results
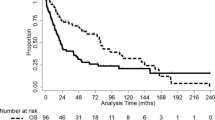
A total of 86 patients satisfied criteria for entry into study, making up 0.08% of all GBM diagnoses in the database. There were 32 (37%) females and 54 (63%) males. Irrespective of treatment, median OS was 67.3 months (95% CI, 46–91), which was distinct from all other ages and pediatric age groups. There were 74 (86%) treated by surgery, 51 (59%) treated by chemotherapy, and 17 (20%) treated by radiation therapy. Multivariable analysis demonstrated that Hispanic status (HR = 3.41, P = 0.02) and the presence of comorbidity (HR = 3.24, P = 0.01) independently predicted shorter OS, whereas treatment with chemotherapy (HR = 0.18, P < 0.01) independently predicted longer OS. Neither extent of surgery nor radiation therapy demonstrated independent statistical significance.
Conclusion
Infantile GBM should be viewed as a distinct GBM entity with a longer OS than other pediatric and adult patients. Chemotherapy is a statistically significant component in the treatment of this demographic, and the value of surgical treatment is likely universal. Future studies into understanding the biological and genetic profile of infantile GBM are needed to advance both pediatric and adult fields.


Similar content being viewed by others
References
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ, Belanger K, Brandes AA, Marosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer E, Mirimanoff RO (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352(10):987–996. https://doi.org/10.1056/NEJMoa043330
Ostrom QT, Gittleman H, Truitt G, Boscia A, Kruchko C, Barnholtz-Sloan JS (2018) CBTRUS statistical report: Primary brain and other central nervous system tumors diagnosed in the United States in 2011–2015. Neuro Oncol 20(suppl_4):iv1-iv86. https://doi.org/10.1093/neuonc/noy131
Brat DJ, Shehata BM, Castellano-Sanchez AA, Hawkins C, Yost RB, Greco C, Mazewski C, Janss A, Ohgaki H, Perry A (2007) Congenital glioblastoma: A clinicopathologic and genetic analysis. Brain Pathol 17(3):276–281. https://doi.org/10.1111/j.1750-3639.2007.00071.x
Davis T, Doyle H, Tobias V, Ellison DW, Ziegler DS (2016) Case report of spontaneous resolution of a congenital glioblastoma. Pediatrics 137(4):e20151241. https://doi.org/10.1542/peds.2015-1241
Kameda M, Otani Y, Ichikawa T, Shimada A, Ichimura K, Date I (2017) Congenital glioblastoma with distinct clinical and molecular characteristics: Case reports and a literature review. World Neurosurg 101:817.e815-817.e814. https://doi.org/10.1016/j.wneu.2017.02.026
Macy ME, Birks DK, Barton VN, Chan MH, Donson AM, Kleinschmidt-Demasters BK, Bemis LT, Handler MH, Foreman NK (2012) Clinical and molecular characteristics of congenital glioblastoma. Neuro Oncol 14(7):931–941. https://doi.org/10.1093/neuonc/nos125
Nomura Y, Yasumoto S, Yanai F, Akiyoshi H, Inoue T, Nibu K, Tsugu H, Fukushima T, Hirose S (2009) Survival and late effects on development of patients with infantile brain tumor. Pediatr Int 51(3):337–341. https://doi.org/10.1111/j.1442-200X.2008.02760.x
Winters JL, Wilson D, Davis DG (2001) Congenital glioblastoma multiforme: A report of three cases and a review of the literature. J Neurol Sci 188(1–2):13–19. https://doi.org/10.1016/s0022-510x(01)00538-x
Lu VM, O’Connor KP, Himes BT, Brown DA, Nesvick CL, Siada RG, Niazi TN, Schwartz J, Daniels DJ (2020) Effect of surgery and chemotherapy on long-term survival in infants with congenital glioblastoma: An integrated survival analysis. J Neurosurg Pediatr:1–9. https://doi.org/10.3171/2020.5.Peds20226
Lerro CC, Robbins AS, Phillips JL, Stewart AK (2013) Comparison of cases captured in the national cancer data base with those in population-based central cancer registries. Ann Surg Oncol 20(6):1759–1765. https://doi.org/10.1245/s10434-013-2901-1
Stupp R, Taillibert S, Kanner A, Read W, Steinberg D, Lhermitte B, Toms S, Idbaih A, Ahluwalia MS, Fink K, Di Meco F, Lieberman F, Zhu JJ, Stragliotto G, Tran D, Brem S, Hottinger A, Kirson ED, Lavy-Shahaf G, Weinberg U, Kim CY, Paek SH, Nicholas G, Bruna J, Hirte H, Weller M, Palti Y, Hegi ME, Ram Z (2017) Effect of tumor-treating fields plus maintenance temozolomide vs maintenance temozolomide alone on survival in patients with glioblastoma: A randomized clinical trial. JAMA 318(23):2306–2316. https://doi.org/10.1001/jama.2017.18718
Fabian D, Guillermo Prieto Eibl MDP, Alnahhas I, Sebastian N, Giglio P, Puduvalli V, Gonzalez J, Palmer JD (2019) Treatment of glioblastoma (GBM) with the addition of tumor-treating fields (TTF): A review. Cancers (Basel) 11(2):174. https://doi.org/10.3390/cancers11020174
Lu VM, O’Connor KP, Himes BT, Brown DA, Nesvick CL, Siada RG, Niazi TN, Schwartz J, Daniels DJ (2020) Surgery and chemotherapy confer long-term survival in infants with congenital glioblastoma: An integrated survival analysis. J Neurosurg Pediatrics In press.
Almeida JP, Chaichana KL, Rincon-Torroella J, Quinones-Hinojosa A (2015) The value of extent of resection of glioblastomas: clinical evidence and current approach. Curr Neurol Neurosci Rep 15(2):517. https://doi.org/10.1007/s11910-014-0517-x
Sanai N, Polley MY, McDermott MW, Parsa AT, Berger MS (2011) An extent of resection threshold for newly diagnosed glioblastomas. J Neurosurg 115(1):3–8. https://doi.org/10.3171/2011.2.jns10998
Kotecha RS, Burley K, Junckerstorff RC, Lee S, Phillips MB, Cole CH, Gottardo NG (2012) Chemotherapy increases amenability of surgical resection in congenital glioblastoma. Pediatr Hematol Oncol 29(6):538–544. https://doi.org/10.3109/08880018.2012.706867
Seker A, Ozek MM (2006) Congenital glioblastoma multiforme. Case report and review of the literature. J Neurosurg 105 (6 Suppl):473–479. https://doi.org/10.3171/ped.2006.105.6.473
Geyer JR, Sposto R, Jennings M, Boyett JM, Axtell RA, Breiger D, Broxson E, Donahue B, Finlay JL, Goldwein JW, Heier LA, Johnson D, Mazewski C, Miller DC, Packer R, Puccetti D, Radcliffe J, Tao ML, Shiminski-Maher T (2005) Multiagent chemotherapy and deferred radiotherapy in infants with malignant brain tumors: A report from the Children’s Cancer Group. J Clin Oncol 23(30):7621–7631. https://doi.org/10.1200/JCO.2005.09.095
Cohen BH, Packer RJ, Siegel KR, Rorke LB, D’Angio G, Sutton LN, Bruce DA, Schut L (1993) Brain tumors in children under 2 years: Treatment, survival and long-term prognosis. Pediatr Neurosurg 19(4):171–179
Kiltie AE, Lashford LS, Gattamaneni H (1997) Survival and late effects in medulloblastoma patients treated with craniospinal irradiation under three years old. Medical and Pediatric Oncology: The Official Journal of SIOP—International Society of Pediatric Oncology (Societé Internationale d’Oncologie Pédiatrique 28 (5):348–354
Walter AW, Mulhern RK, Gajjar A, Heideman RL, Reardon D, Sanford RA, Xiong X, Kun LE (1999) Survival and neurodevelopmental outcome of young children with medulloblastoma at St Jude Children’s Research Hospital. J Clin Oncol 17(12):3720–3728
Shimamura N, Asano K-I, Ogane K, Yagihashi A, Ohkuma H, Suzuki S (2003) A case of definitely congenital glioblastoma manifested by intratumoral hemorrhage. Childs Nerv Syst 19(10–11):778–781. https://doi.org/10.1007/s00381-003-0807-0
Patel NP, Lyon KA, Huang JH (2019) The effect of race on the prognosis of the glioblastoma patient: A brief review. Neurol Res 41(11):967–971. https://doi.org/10.1080/01616412.2019.1638018
Shabihkhani M, Telesca D, Movassaghi M, Naeini YB, Naeini KM, Hojat SA, Gupta D, Lucey GM, Ontiveros M, Wang MW, Hanna LS, Sanchez DE, Mareninov S, Khanlou N, Vinters HV, Bergsneider M, Nghiemphu PL, Lai A, Liau LM, Cloughesy TF, Yong WH (2017) Incidence, survival, pathology, and genetics of adult Latino Americans with glioblastoma. J Neurooncol 132(2):351–358. https://doi.org/10.1007/s11060-017-2377-0
Brown DA, Himes BT, Kerezoudis P, Chilinda-Salter YM, Grewal SS, Spear JA, Bydon M, Burns TC, Parney IF (2018) Insurance correlates with improved access to care and outcome among glioblastoma patients. Neuro Oncol 20(10):1374–1382. https://doi.org/10.1093/neuonc/noy102
Dressler EV, Liu M, Garcia CR, Dolecek TA, Pittman T, Huang B, Villano JL (2019) Patterns and disparities of care in glioblastoma. Neurooncol Pract 6(1):37–46. https://doi.org/10.1093/nop/npy014
Lu VM, Shah AH, Eichberg DG, Quinones-Hinojosa A, Esquenazi Y, Komotar RJ, Ivan ME (2020) Geographic disparities in access to glioblastoma treatment based on Hispanic ethnicity in the United States: Insights from a national database. J Neurooncol 147(3):711–720. https://doi.org/10.1007/s11060-020-03480-1
Gilani A, Donson A, Davies KD, Whiteway SL, Lake J, DeSisto J, Hoffman L, Foreman NK, Kleinschmidt-DeMasters BK, Green AL (2020) Targetable molecular alterations in congenital glioblastoma. J Neurooncol 146(2):247–252. https://doi.org/10.1007/s11060-019-03377-8
Guerreiro Stucklin AS, Ryall S, Fukuoka K, Zapotocky M, Lassaletta A, Li C, Bridge T, Kim B, Arnoldo A, Kowalski PE, Zhong Y, Johnson M, Li C, Ramani AK, Siddaway R, Nobre LF, de Antonellis P, Dunham C, Cheng S, Boué DR, Finlay JL, Coven SL, de Prada I, Perez-Somarriba M, Faria CC, Grotzer MA, Rushing E, Sumerauer D, Zamecnik J, Krskova L, Garcia Ariza M, Cruz O, Morales La Madrid A, Solano P, Terashima K, Nakano Y, Ichimura K, Nagane M, Sakamoto H, Gil-da-Costa MJ, Silva R, Johnston DL, Michaud J, Wilson B, van Landeghem FKH, Oviedo A, McNeely PD, Crooks B, Fried I, Zhukova N, Hansford JR, Nageswararao A, Garzia L, Shago M, Brudno M, Irwin MS, Bartels U, Ramaswamy V, Bouffet E, Taylor MD, Tabori U, Hawkins C (2019) Alterations in ALK/ROS1/NTRK/MET drive a group of infantile hemispheric gliomas. Nat Commun 10(1):4343. https://doi.org/10.1038/s41467-019-12187-5
Whiteway SL, Betts AM, O’Neil ER, Green AL, Gilani A, Orr BA, Mathis DA (2020) Oncogenic GOPC-ROS1 fusion identified in a congenital glioblastoma case. J Pediatr Hematol Oncol. https://doi.org/10.1097/MPH.0000000000001711.10.1097/MPH.0000000000001711
Thirant C, Bessette B, Varlet P, Puget S, Cadusseau J, Tavares Sdos R, Studler JM, Silvestre DC, Susini A, Villa C, Miquel C, Bogeas A, Surena AL, Dias-Morais A, Leonard N, Pflumio F, Bieche I, Boussin FD, Sainte-Rose C, Grill J, Daumas-Duport C, Chneiweiss H, Junier MP (2011) Clinical relevance of tumor cells with stem-like properties in pediatric brain tumors. PLoS One 6(1):e16375. https://doi.org/10.1371/journal.pone.0016375
Epstein NE, Sundrani SL, Rosenthal AD, Decker RE (1987) Extensive surgical excision of large hemispheric “malignant” astrocytoma in a 6-week-old infant. Childs Nerv Syst 3(4):248–250. https://doi.org/10.1007/bf00274061
Perry A (2021) Preview of the WHO 2021 CNS Tumor Classification Scheme. https://www.youtube.com/watch?v=CEY9OqSrLUA&t=436s&ab_channel=UCSFNeurosurgeryUCSFNeurosurgery. University of California San Francisco
Kalani MY, Kalani MA, Gwinn R, Keogh B, Tse VC (2009) Embryological development of the human insula and its implications for the spread and resection of insular gliomas. Neurosurg Focus 27(2):E2. https://doi.org/10.3171/2009.5.Focus0997
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors report no funding sources or conflict of interest concerning the materials or methods used in this study or the findings specified in this paper.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lu, V.M., Eichberg, D.G., Luther, E.M. et al. Distinct survival and clinical profile of infantile glioblastoma: insights from a national database. Childs Nerv Syst 38, 85–94 (2022). https://doi.org/10.1007/s00381-021-05386-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-021-05386-3