Abstract
Purpose
Paediatric spine trauma is uncommon and is managed differently from adults due to the anatomical differences of the paediatric spine. The paediatric spine is less ossified, with lax ligaments and a higher fulcrum in the c-spine which results in a different pattern of injuries. The aim of this study is to provide a contemporary audit of paediatric spinal trauma.
Methods
A retrospective review was conducted using the Trauma and Audit Research Network database at a major trauma centre (2011–2018). All patients < 18 years old with a spine injury underwent case note and radiology review.
Results
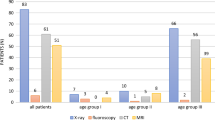
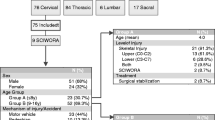
A total of 72 patients (37, 51.4% male with an average age of 13.3 (± 5.9) years old) were identified. The most common mechanism of injury was road traffic collisions (n = 39, 54.2%). The most common sporting cause was motocross accidents (n = 6, 8.3%), and a further 6 (8.3%) patients had a suspected inflicted injury. Eight patients (11.1%) sustained a spinal cord injury. Twenty-seven (37.5%) patients underwent surgical intervention to treat their spinal injury.
Conclusion
This series demonstrates the profile of injury mechanisms causing paediatric spinal injuries. Paediatric spine injuries continue to have the potential for lifelong disability and require careful, specialist management. This series also highlights certain causes such as motocross accidents and suspected inflicted injury which are more frequent than expected and raise potential public health concerns.






Similar content being viewed by others
References
Saul D, Dresing K (2018) Epidemiology of vertebral fractures in pediatric and adolescent patients. Pediatr Rep 10:17–23. https://doi.org/10.4081/pr.2018.7232
Kim C, Vassilyadi M, Forbes JK, Moroz NWP, Camacho A, Moroz PJ (2016) Traumatic spinal injuries in children at a single level 1 pediatric trauma centre: report of a 23-year experience. Can J Surg 59:205–212. https://doi.org/10.1503/cjs.014515
Zonfrillo MR, Zaniletti I, Hall M, Fieldston ES, Colvin JD, Bettenhausen JL, Macy ML, Alpern ER, Cutler GJ, Raphael JL, Morse RB, Sills MR, Shah SS (2016) Socioeconomic status and hospitalization costs for children with brain and spinal cord injury. J Pediatr 169:250–255. https://doi.org/10.1016/j.jpeds.2015.10.043
Cirak B, Ziegfeld S, Knight VM, Chang D, Avellino AM, Paidas CN (2004) Spinal injuries in children. J Pediatr Surg 39:607–612. https://doi.org/10.1016/j.jpedsurg.2003.12.011
Dickman CA, Rekate HL, Sonntag VKH, Zabramski JM (1989) Pediatric spinal trauma: vertebral column and spinal cord injuries in children. Pediatr Neurosurg 15:237–256. https://doi.org/10.1159/000120476
Resid Onen M, Naderi S (2015) J Spine Pediatr Spine Trauma:4. https://doi.org/10.4172/21657939.1000211
Bilston Lynne E, Brown Julie E (2007) Pediatric spinal injury type and severity are age and mechanism dependent. Spine (Phila Pa 1976) 32:2339–2347. https://doi.org/10.1097/BRS.0b013e3181558886
Barnes PD, Krasnokutsky MV, Monson KL, Ophoven J (2008) Traumatic spinal cord injury: accidental versus nonaccidental injury. Semin Pediatr Neurol 15:178–184. https://doi.org/10.1016/j.spen.2008.10.009
Dauleac C, Beuriat PA, Di Rocco F et al (2019) Surgical management of pediatric spine trauma: 12 years of experience. World Neurosurg 126:e1494–e1502. https://doi.org/10.1016/j.wneu.2019.03.134
Dogan S, Safavi-Abbasi S, Theodore N, Chang SW, Horn EM, Mariwalla NR, Rekate HL, Sonntag VKH (2007) Thoracolumbar and sacral spinal injuries in children and adolescents: a review of 89 cases. J Neurosurg Pediatr 106:426–433. https://doi.org/10.3171/ped.2007.106.6.426
Mortazavi M, Gore PA, Chang S, Tubbs RS, Theodore N (2011) Pediatric cervical spine injuries: a comprehensive review. Childs Nerv Syst 27:705–717. https://doi.org/10.1007/s00381-010-1342-4
Castranova V, Asgharian B, Sayre P et al (2016) Motor vehicle crash–related injury causation scenarios for spinal injuries in restrained children and adolescents MARK. 15:1922–2013. https://doi.org/10.1080/15389588.2014.934959.Motor
Vaccaro AR, Koerner JD, Radcliff KE, Oner FC, Reinhold M, Schnake KJ, Kandziora F, Fehlings MG, Dvorak MF, Aarabi B, Rajasekaran S, Schroeder GD, Kepler CK, Vialle LR (2016) AOSpine subaxial cervical spine injury classification system. Eur Spine J 25:2173–2184. https://doi.org/10.1007/s00586-015-3831-3
Vaccaro AR, Oner C, Kepler CK, Dvorak M, Schnake K, Bellabarba C, Reinhold M, Aarabi B, Kandziora F, Chapman J, Shanmuganathan R, Fehlings M, Vialle L, AOSpine Spinal Cord Injury & Trauma Knowledge Forum (2013) AOSpine thoracolumbar spine injury classification system: fracture description, neurological status, and key modifiers. Spine (Phila Pa 1976) 38:2028–2037. https://doi.org/10.1097/BRS.0b013e3182a8a381
Patel JC, Tepas JJ, Mollitt DL, Pieper P (2001) Pediatric cervical spine injuries: defining the disease. J Pediatr Surg 36:373–376. https://doi.org/10.1053/jpsu.2001.20720
Babcock L, Olsen CS, Jaffe DM, Leonard JC (2016) Cervical spine injuries in children associated with sports and recreational activities. Pediatr Emerg Care 00:1–10
Lee BB, Cripps RA, Fitzharris M, Wing PC (2014) The global map for traumatic spinal cord injury epidemiology: update 2011, global incidence rate. Spinal Cord 52:110–116. https://doi.org/10.1038/sc.2012.158
Freitag A, Kirkwood G, Scharer S, Ofori-Asenso R, Pollock AM (2015) Systematic review of rugby injuries in children and adolescents under 21 years. Br J Sports Med 49:511–519. https://doi.org/10.1136/bjsports-2014-093684
Knox J, Schneider J, Wimberly RL, Riccio AI (2014) Characteristics of spinal injuries secondary to nonaccidental trauma. J Pediatr Orthop 34:376–381. https://doi.org/10.1097/BPO.0000000000000111
Knox JB, Schneider JE, Cage JM, Wimberly RL, Riccio AI (2014) Spine trauma in very young children: a retrospective study of 206 patients presenting to a level 1 pediatric trauma center. J Pediatr Orthop 34:698–702
Sayama C, Chen T, Trost G, Jea A (2014) A review of pediatric lumbar spine trauma. Neurosurg Focus 37:1–9. https://doi.org/10.3171/2014.5.FOCUS1490
Pang D, Pollack IF (1989) Spinal cord injury without radiographic abnormality in children-the SCIWORA syndrome. J Trauma - Inj Infect Crit Care 29:654–664
Erfani MA, Pourabbas B, Nouraie H, Vadiee I, Vosoughi AR (2014) Results of fusion and instrumentation of thoracic and lumbar vertebral fractures in children: a prospective ten-year study. Musculoskelet Surg 98:107–114. https://doi.org/10.1007/s12306-014-0313-4
Magnus KK, Anders M, Ralph H, Jack B, Caroline K, Acke O (2003) A modeling capacity of vertebral fractures exists during growth - an up to 47-year follow-up. Spine (Phila Pa 1976) 28:2087–2092. https://doi.org/10.1097/01.BRS.0000084680.76654.B1
Author information
Authors and Affiliations
Contributions
The drafting of the manuscript was done by Booker J, Hall S, and Dando A. In addition, the analysis and interpretation of data were done by Booker J and Hall S. The remaining authors participated in the conception and design of the study as well as the review of the manuscript. Each author participated sufficiently to meet the criteria for authorship according to ICMJE.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study did not require ethics approval because the data was collected retrospectively and presented anonymously, and had no impact on the care received by each patient.
Consent for publication
Not applicable.
Conflict of interest
The authors report no conflict of interest.
Preliminary publication
None
Code availability
Not applicable.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Booker, J., Hall, S., Dando, A. et al. Paediatric spinal trauma presenting to a UK major trauma centre. Childs Nerv Syst 37, 1949–1956 (2021). https://doi.org/10.1007/s00381-021-05044-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-021-05044-8