Abstract
Introduction
Shunting for hydrocephalus can lead to improvement in the quality of life although the latter has been subdued by complications like shunt infection. Established protocols have contributed to the reduction of ventriculoperitoneal shunt (VPS) infections. Previously, we retrospectively demonstrated a low infection rate despite some of the protocol recommendations not being implemented. The aim of this study was to prospectively establish the incidence of shunt infection in the early post-shunt period following our protocol and elucidate on associated risk factors.
Patients and methods
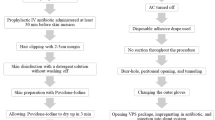
A multicenter prospective descriptive cohort study of consecutive 209 under-5 children requiring VPS for hydrocephalus was conducted between January 2013 and November 2018. An innovative protocol insisting on intermittent application of povidone-iodine on the skin during the operation was implemented. The patients were followed-up for 3 months post-surgery.
Results
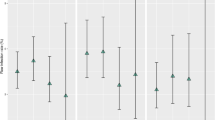
Included were 211 VPS procedures performed on 209 children. The median age was 9 months and 84 were males. Hydrocephalus was non-communicative in 72.0% and aqueductal stenosis was its most frequent cause (84.9%). Most surgeries were performed in the morning (90.5%), electively (95.3%), and for the first time (91%). The median duration of surgery was 65 min. Shunt infection rate was 1.9% (n = 4) (95% CI 0.7 to 5.0%) per procedure.
Conclusion
The observed infection rate was low. This suggests that the protocol followed captured the most critical components necessary to ensure low infection rates and that simple measures implemented in economically challenged environments may achieve internationally acceptable infection rates.



Similar content being viewed by others
Abbreviations
- CSF:
-
Cerebrospinal fluid
- VPS:
-
Ventriculoperitoneal shunt
- ETV:
-
Endoscopic third ventriculostomy
- EVD:
-
External ventricular drainage
- HCP:
-
Hydrocephalus
References
Akhaddar A (2015) Complications of extrathecal CSF shunts:infective complications. In: Di Rocco C, Turgut M, Jallo G, Martínez-Lage JF (eds) Complications of CSF shunting in hydrocephalus: prevention, identification, and management. Springer International Publishing, Cham, pp 141–149
Choux M, Genitori L, Lang D, Lena G (1992) Shunt implantation: reducing the incidence of shunt infection. J Neurosurg 77:875–880
Di Rocco C, Massimi L, Tamburrini G (2006) Shunts vs endoscopic third ventriculostomy in infants: are there different types and/or rates of complications? A review. Childs Nerv Syst 22:1573–1589
Dobson AJ (1984) Calculating sample size. Trans Menzies Foundation 7:75–79
Drake JM, Singhal A, Kulkarni AV, DeVeber G, Cochrane DD (2012) Consensus definitions of complications for accurate recording and comparisons of surgical outcomes in pediatric neurosurgery. J Neurosurg Pediatr 10:89–95
Esene IN, Ngu J, Elzoghby M, Solaroglu I, Sikod AM, Kotb A, Dechambenoit G, ElHusseiny H (2014) Case series and descriptive cohort studies in neurosurgery: the confusion and solution. Childs Nerv Syst 30:1321–1332
Gathura E, Poenaru D, Bransford R, Albright AL (2010) Outcomes of ventriculoperitoneal shunt insertion in Sub-Saharan Africa. J Neurosurg Pediatr 6:329–335
George R, Leibrock L, Epstein M (1979) Long-term analysis of cerebrospinal fluid shunt infections. A 25-year experience. J Neurosurg 51:804–811
Gutierrez-Murgas Y, Snowden JN (2014) Ventricular shunt infections: immunopathogenesis and clinical management. J Neuroimmunol 276:1–8
Kalangu KK (2000) Pediatric neurosurgery in Africa--present and future. Childs Nerv Syst 16:770–775
Kalangu KKN, Esene IN, Dzowa M, Musara A, Ntalaja J, Badra AK (2019) Towards zero infection for ventriculoperitoneal shunt insertion in resource-limited settings: a multicenter prospective cohort study. Childs Nerv Syst. https://doi.org/10.1007/s00381-019-04357-z
Kestle JR, Hoffman HJ, Soloniuk D, Humphreys RP, Drake JM, Hendrick EB (1993) A concerted effort to prevent shunt infection. Childs Nerv Syst 9:163–165
Kestle JR, Riva-Cambrin J, Wellons JC III, Kulkarni AV, Whitehead WE, Walker ML, Oakes WJ, Drake JM, Luerssen TG, Simon TD, Holubkov R (2011) A standardized protocol to reduce cerebrospinal fluid shunt infection: the Hydrocephalus Clinical Research Network Quality Improvement Initiative. J Neurosurg Pediatr 8:22–29
Komolafe EO, Adeolu AA, Komolafe MA (2008) Treatment of cerebrospinal fluid shunting complications in a Nigerian neurosurgery programme. Case illustrations and review. Pediatr Neurosurg 44:36–42
Limbrick DD Jr, Baird LC, Klimo P Jr, Riva-Cambrin J, Flannery AM (2014) Pediatric hydrocephalus: systematic literature review and evidence-based guidelines. Part 4: cerebrospinal fluid shunt or endoscopic third ventriculostomy for the treatment of hydrocephalus in children. J Neurosurg Pediatr 14(Suppl 1):30–34
Mangram AJ, Horan TC, Pearson ML, Silver LC, Jarvis WR (1999) Guideline for prevention of surgical site infection, 1999. Hospital Infection Control Practices Advisory Committee. Infect Control Hosp Epidemiol 20:250–278
Mark R.Lantosca , James M. Drak: Cerebrospinal fluid shunts, in A. Leland Albright, Ian F. Pollack (eds): Operative techniques in pediatric neurosurgery. New York, Thieme, 2001, pp 3–14
Greenberg MS (2016) Ch. 21:Skull, spine, and post-surgical infections: 21.1 shunt infection. In: Greenberg MS (ed) Handbook of neurosurgery. Thieme, New York, pp 339–342
McGirt MJ, Zaas A, Fuchs HE, George TM, Kaye K, Sexton DJ (2003) Risk factors for pediatric ventriculoperitoneal shunt infection and predictors of infectious pathogens. Clin Infect Dis 36:858–862
Mottolese C, Grando J, Convert J, Abdoulrahman M, Lelievre H, Vandenesch F, Bret P, Lapras C (2000) Zero rate of shunt infection in the first postoperative year in children--dream or reality? Childs Nerv Syst 16:210–212
Moussa WM, Mohamed MA (2016) Efficacy of postoperative antibiotic injection in and around ventriculoperitoneal shunt in reduction of shunt infection: a randomized controlled trial. Clin Neurol Neurosurg 143:144–149
Musara A, Kalangu K (2008) Ventriculperitoneal shunt infection in pediatric age group in Harare, Zimbabwe. Childs Nerv Syst 24:1280
Mwachaka PM, Obonyo NG, Mutiso BK, Ranketi S, Mwang’ombe N (2010) Ventriculoperitoneal shunt complications: a three-year retrospective study in a Kenyan national teaching and referral hospital. Pediatr Neurosurg 46:1–5
Nejat F, Tajik P, Ghodsi SM, Golestan B, Majdzadeh R, Yazdani S, Ansari S, Dadmehr M, Ganji S, Najafi M, Farahmand F, Moatamed F (2008) Breastfeeding: a potential protective factor against ventriculoperitoneal shunt infection in young infants. J Neurosurg Pediatr 1:138–141
Parker SL, McGirt MJ, Murphy JA, Megerian JT, Stout M, Engelhart L (2015) Comparative effectiveness of antibiotic-impregnated shunt catheters in the treatment of adult and pediatric hydrocephalus: analysis of 12,589 consecutive cases from 287 US hospital systems. J Neurosurg 122:443–448
Pirotte BJ, Lubansu A, Bruneau M, Loqa C, Van CN, Brotchi J (2007) Sterile surgical technique for shunt placement reduces the shunt infection rate in children: preliminary analysis of a prospective protocol in 115 consecutive procedures. Childs Nerv Syst 23:1251–1261
Rotim K, Miklic P, Paladino J, Melada A, Marcikic M, Scap M (1997) Reducing the incidence of infection in pediatric cerebrospinal fluid shunt operations. Childs Nerv Syst 13:584–587
Sarmey N, Kshettry VR, Shriver MF, Habboub G, Machado AG, Weil RJ (2015) Evidence-based interventions to reduce shunt infections: a systematic review. Childs Nerv Syst 31:541–549
Sciubba DM, Noggle JC, Carson BS, Jallo GI (2008) Antibiotic-impregnated shunt catheters for the treatment of infantile hydrocephalus. Pediatr Neurosurg 44:91–96
Sibanda EN, Levy LF, Makarawo S (1991) Infection after Harare valve V-P shunt operations: a review of 92 cases. Cent Afr J Med 37:397–403
Tarwa C, De Villiers FP (2007) The use of the road to health card in monitoring child health. S Afr Fam Pract 49:15–15d
Thompson DN, Hartley JC, Hayward RD (2007) Shunt infection: is there a near-miss scenario? J Neurosurg 106:15–19
Warf BC (2005) Comparison of 1-year outcomes for the Chhabra and Codman-Hakim Micro Precision shunt systems in Uganda: a prospective study in 195 children. J Neurosurg 102:358–362
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Patient consent
The patient or guardian has consented to this study by signing the consent form.
Conflict of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kalangu, K.K.N., Esene, I.N., Dzowa, M. et al. Towards zero infection for ventriculoperitoneal shunt insertion in resource-limited settings: a multicenter prospective cohort study. Childs Nerv Syst 36, 401–409 (2020). https://doi.org/10.1007/s00381-019-04357-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-019-04357-z