Abstract
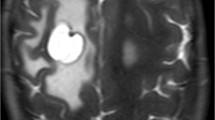
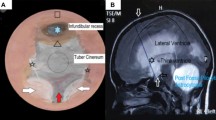
The authors present the case of a previously healthy 12-year-old male with intractable seizures localized to a right frontal area of encephalomalacia and porencephalic cyst who underwent resection of the seizure focus. The surgical resection cavity extended into the right lateral ventricle, and due to encountered hemorrhage, Gelfoam was used for optimal hemostasis. The patient did well following the procedure, but presented 5 months later with headaches and emesis and was discovered to have obstructive hydrocephalus on imaging studies. Endoscopic third ventriculostomy (ETV) was performed, where Gelfoam was encountered in the third ventricle, obstructing the cerebral aqueduct. After the completion of the ETV, the patient did well and continues to be asymptomatic 1 year following the procedure.


Similar content being viewed by others
Change history
26 April 2019
The original version of this article unfortunately contained an error. The authors apologize to have miss looked a typo of author name ���Joseph Diver���. The correct name is ���Joseph Driver���.
26 April 2019
The original version of this article unfortunately contained an error. The authors apologize to have miss looked a typo of author name ���Joseph Diver���. The correct name is ���Joseph Driver���.
26 April 2019
The original version of this article unfortunately contained an error. The authors apologize to have miss looked a typo of author name ���Joseph Diver���. The correct name is ���Joseph Driver���.
Reference
Edwards RJ, Dirks PB (2006) Gelfoam obstruction of endoscopic third ventriculostomy. J Neurosurg: Pediatrics 105:154–154. https://doi.org/10.3171/ped.2006.105.2.154
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors of this paper declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Hazama, A., Diver, J., Grannan, B. et al. Iatrogenic obstructive hydrocephalus resulting from Gelfoam accumulation within the cerebral aqueduct: a case report. Childs Nerv Syst 34, 2333–2335 (2018). https://doi.org/10.1007/s00381-018-3874-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-018-3874-y