Abstract
Aim
Granulomatosis with polyangiitis (GPA), extremely rare in children, is a disease characterized by granulomatous inflammation and necrotizing vasculitis that involves medium and small vessels. Central nervous system (CNS) involvement in GPA is not common and often appears at a later stage of the disease. The CNS manifestation of pediatric GPA was fragmentally discussed. Herein, we reported a case of relapsing-remitting pediatric GPA with prominent CNS involvement as initial symptoms.
Method
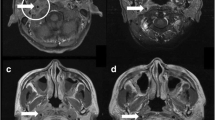
The patient was a 9-year-old female. The first episode manifested as uroclepsia and bilateral lower extremity weakness, resulting from diffused dot-enhanced large lesions within bilateral anterior cerebral artery territory on magnetic resonance (MR). This was followed by three recurring episodes of visual impairment as a result of optic neuritis. MR in the last episode indicated bilateral sphenoid sinus inflammation adjacent to the left optical nerve. All four episodes were combined with upper respiratory tract symptoms and slight urine abnormality. She responded well to large doses of corticosteroids and immunoglobulins. However, the patient had long been suspected of having multiple sclerosis and had not received appropriate maintenance treatment.
Result
After being diagnosed with GPA, the patient received small doses of glucocorticoids and mycophenolate mofetil for maintenance, which generated a favorable outcome.
Conclusion
CNS involvement in pediatric GPA is rare. Single large or multifocal insults involving one or more lobes consistent with the distribution of cerebral arteries could be a typical feature on MR. Early diagnosis and proper treatments help to improve the prognosis.


Similar content being viewed by others
References
Grisaru S, Yuen GW, Miettunen PM, Hamiwka LA (2010) Incidence of Wegener’s granulomatosis in children. J Rheumatol 37:440–442
Bohm M, Gonzalez Fernandez MI, Ozen S, Pistorio A, Dolezalova P, Brogan P, Barbano G, Sengler C, Klein-Gitelman M, Quartier P, Fasth A, Herlin T, Terreri MT, Nielsen S, van Rossum MA, Avcin T, Castell ER, Foeldvari I, Foell D, Kondi A, Kone-Paut I, Kuester RM, Michels H, Wulffraat N, Amer HB, Malattia C, Martini A, Ruperto N (2014) Clinical features of childhood granulomatosis with polyangiitis (Wegener’s granulomatosis). Pediatr Rheumatol Online J 12:18
Tahghighi F, Moradinejad MH, Aghighi Y, Shiari R, Raeeskarami SR, Salehzadeh F, Javadi V, Ziaee V (2013) Evaluation of 10-year experience of Wegener’s granulomatosis in Iranian children. ISRN Rheumatol 2013:694928
Leavitt RY, Fauci AS, Bloch DA, Michel BA, Hunder GG, Arend WP, Calabrese LH, Fries JF, Lie JT, Lightfoot RW Jr, et al. (1990) The American College of Rheumatology 1990 criteria for the classification of Wegener’s granulomatosis. Arthritis Rheum 33:1101–1107
Twilt M, Benseler S, Cabral D (2012) Granulomatosis with polyangiitis in childhood. Curr Rheumatol Rep 14:107–115
De Luna G, Terrier B, Kaminsky P, Le Quellec A, Maurier F, Solans R, Godmer P, Costedoat-Chalumeau N, Seror R, Charles P, Cohen P, Puechal X, Mouthon L, Guillevin L, French Vasculitis Study G (2015) Central nervous system involvement of granulomatosis with polyangiitis: clinical-radiological presentation distinguishes different outcomes. Rheumatology (Oxford) 54:424–432
Holle JU, Gross WL (2011) Neurological involvement in Wegener’s granulomatosis. Curr Opin Rheumatol 23:7–11
Cabral DA, Uribe AG, Benseler S, O’Neil KM, Hashkes PJ, Higgins G, Zeft AS, Lovell DJ, Kingsbury DJ, Stevens A, McCurdy D, Chira P, Abramson L, Arkachaisri T, Campillo S, Eberhard A, Hersh AO, Huber AM, Kim S, Klein-Gitelman M, Levy DM, Li SC, Mason T, Dewitt EM, Muscal E, Nassi L, Reiff A, Schikler K, Singer NG, Wahezi D, Woodward A, Network ARI (2009) Classification, presentation, and initial treatment of Wegener’s granulomatosis in childhood. Arthritis Rheum 60:3413–3424
Belostotsky VM, Shah V, Dillon MJ (2002) Clinical features in 17 paediatric patients with Wegener granulomatosis. Pediatr Nephrol 17:754–761
von Scheven E, Lee C, Berg BO (1998) Pediatric Wegener’s granulomatosis complicated by central nervous system vasculitis. Pediatr Neurol 19:317–319
Ohta T, Sakano T, Shiotsu M, Furue T, Ohtani H, Kinoshita Y, Mizoue T, Kiya K, Tanaka I (2004) Reversible posterior leukoencephalopathy in a patient with Wegener granulomatosis. Pediatr Nephrol 19:442–444
Ulinski T, Martin H, Mac Gregor B, Dardelin R, Cochat P (2005) Fatal neurologic involvement in pediatric Wegener’s granulomatosis. Pediatr Neurol 32:278–281
Moore BM, Rothman SM, Clark HB, Vehe RK, Laguna TA (2010) Epilepsy: an anticipatory presentation of pediatric Wegener’s granulomatosis. Pediatr Neurol 43:49–52
Nagaoka T, Ikeda K, Hirayama T, Yamamoto T, Iwasaki Y (2012) Wegener granulomatosis-associated optic perineural hypertrophy and optic neuropathy. Intern Med 51:227–228
O’Neil KM (2009) Progress in pediatric vasculitis. Curr Opin Rheumatol 21:538–546
Hiemstra TF, Walsh M, Mahr A, Savage CO, de Groot K, Harper L, Hauser T, Neumann I, Tesar V, Wissing KM, Pagnoux C, Schmitt W, Jayne DR, European Vasculitis Study G (2010) Mycophenolate mofetil vs azathioprine for remission maintenance in antineutrophil cytoplasmic antibody-associated vasculitis: a randomized controlled trial. JAMA 304:2381–2388
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Funding
The authors received no financial support for this article.
Rights and permissions
About this article
Cite this article
Lu, T., Bao, J., Lin, D. et al. Pediatric granulomatosis with polyangiitis exhibiting prominent central nervous system symptoms. Childs Nerv Syst 32, 1517–1521 (2016). https://doi.org/10.1007/s00381-016-3080-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-016-3080-8